Abstract
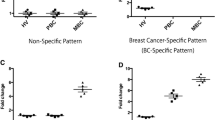
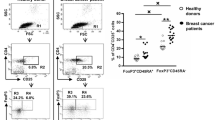
Generation of Regulatory T cells (Tregs) is known to play a major role in progression and modulation of the immune escape mechanisms in cancer. These cells express Forkhead/winged helix transcription factor (FOXP3) and also Cytotoxic T-lymphocyte antigen-4 (CTLA-4), as a negative regulatory molecule which, is a potential target for immunotherapy. We, therefore, evaluated FOXP3 and CTLA-4 transcripts in the peripheral blood mononuclear cells from 55 women with histologically-confirmed infiltrating ductal carcinoma of the breast. Blood samples from 40 healthy volunteer women without a history of malignancies or autoimmune disorders were also obtained as a control. The abundance of FOXP3 and CTLA-4 gene transcripts was determined by quantitative real-time PCR (qRT-PCR). Compared to healthy individuals, significantly higher amounts of these transcripts were found in the mononuclear cells from breast cancer patients. Also, a significant correlation was found between CTLA-4 and FOXP3 expressions in a group of patients. Among patients with early stage, nonmetastatic or low-grade disease, the relative expression of CTLA-4 was about 10-fold as much as in the control group. These patients also showed a significant increase, more than 10 fold, in mean relative FOXP3 expression. The results of this investigation point to functional activity of Treg cells in early stages of breast cancer, a finding which emphasizes the significance of Tregs as an imminent target for breast cancer immunotherapy.



Similar content being viewed by others
Abbreviations
- CTLA-4:
-
Cytotoxic T-lymphocyte antigen-4
- GITR:
-
Glucocorticoid-induced tumor necrosis factor receptor
- TGF-β:
-
Τransforming growth factor- betta
- FoxP3:
-
Forkhead/winged helix transcription factor
- qRT-PCR:
-
quantitative real-time PCR
References
Kaklamanis L, Townsend A, Doussis-Anagnostopoulou IA et al (1994) Loss of major histocompatibility complex-encoded transporter associated with antigen presentation (TAP) in colorectal cancer. Am J Pathol 145:505–509
Elgert KD, Alleva DG, Mullins DW (1998) Tumor-induced immune dysfunction: the macrophage connection. J Leukoc Biol 64:275–290
Staveley-O’Carroll K, Sotomayor E, Montgomery J et al (1998) Induction of antigen-specific T cell anergy: an early event in the course of tumor progression. Proc Natl Acad Sci USA 95:1178–1183
Roncarolo MG, Gregori S, Levings M (2003) Type 1 T regulatory cells and their relationship with CD4+CD25+ T regulatory cells. Novartis Found Symp 252:115–127
Caras I, Grigorescu A, Stavaru C et al (2004) Evidence for immune defects in breast and lung cancer patients. Cancer Immunol Immunother 53:1146–1152
Wolf AM, Wolf D, Steurer M et al (2003) Increase of regulatory T cells in the peripheral blood of cancer patients. Clin Cancer Res 9:606–612
O’Garra A, Vieira P (2004) Regulatory T cells and mechanisms of immune system control. Nat Med 10:801–805
Sakaguchi S (2000) Regulatory T cells: key controllers of immunologic self-tolerance. Cell 101:455–458
Sakaguchi S (2005) Naturally arising Foxp3-expressing CD25+CD4+ regulatory T cells in immunological tolerance to self and non-self. Nat Immunol 6:345–352
Hori S, Nomura T, Sakaguchi S (2003) Control of regulatory T cell development by the transcription factor Foxp3. Science 299:1057–1061
Fontenot JD, Rasmussen JP, Williams LM et al (2005) Regulatory T cell lineage specification by the forkhead transcription factor foxp3. Immunity 22:329–341
Woo EY, Chu CS, Goletz TJ et al (2001) Regulatory CD4(+)CD25(+) T cells in tumors from patients with early-stage non-small cell lung cancer and late-stage ovarian cancer. Cancer Res 61:4766–4772
Liyanage UK, Moore TT, Joo HG et al (2002) Prevalence of regulatory T cells is increased in peripheral blood and tumor microenvironment of patients with pancreas or breast adenocarcinoma. J Immunol 169:2756–2761
Viguier M, Lemaitre F, Verola O et al (2004) Foxp3 expressing CD4+CD25(high) regulatory T cells are overrepresented in human metastatic melanoma lymph nodes and inhibit the function of infiltrating T cells. J Immunol 173:1444–1453
Ormandy LA, Hillemann T, Wedemeyer H et al (2005) Increased populations of regulatory T cells in peripheral blood of patients with hepatocellular carcinoma. Cancer Res 65:2457–2464
Clarke SL, Betts GJ, Plant A et al (2006) CD4+CD25+FOXP3+ regulatory T cells suppress anti-tumor immune responses in patients with colorectal cancer. PLoSONE 1:e129
Gallimore A, Godkin A (2008) Regulatory T cells and tumour immunity—observations in mice and men. Immunology 123:157–163
Strauss L, Bergmann C, Gooding W et al (2007) The frequency and suppressor function of CD4+CD25highFoxp3+ T cells in the circulation of patients with squamous cell carcinoma of the head and neck. Clin Cancer Res 13:6301–6311
Bi Y, Wei L, Mao HT, Zhang L, Zuo WS (2008) Expressions of Fas, CTLA-4 and RhoBTB2 genes in breast carcinoma and their relationship with clinicopathological factors. Zhonghua ZhongLiu Za Zhi 30:749–753, Article in Chinease
Ohara M, Yamaguchi Y, Matsuura K et al (2009) Possible involvement of regulatory T cells in tumor onset and progression in primary breast cancer. Cancer Immunol Immunother 58:441–447
Mansfield AS, Heikkila PS, Vaara AT et al (2009) Simultaneous Foxp3 and IDO expression is associated with sentinel lymph node metastases in breast cancer. BMC Cancer 9:231
Merlo A, Casalini P, Carcangiu ML et al (2009) FOXP3 expression and overall survival in breast cancer. J Clin Oncol 27:1746–1752
Gupta S, Joshi K, Wig JD, Arora SK (2007) Intratumoral FOXP3 expression in infiltrating breast carcinoma: its association with clinicopathologic parameters and angiogenesis. Acta Oncol 46:792–797
Pfaffl MW (2001) A new mathematical model for relative quantification in real-time RT-PCR. Nucleic Acids Res 29:e45
Shevach EM, McHugh RS, Piccirillo CA et al (2001) Control of T-cell activation by CD4+ CD25+ suppressor T cells. Immunol Rev 182:58–67
Hilchey SP, Bernstein SH (2007) Use of CFSE to monitor ex vivo regulatory T-cell suppression of CD4+ and CD8+ T-cell proliferation within unseparated mononuclear cells from malignant and non-malignant human lymph node biopsies. Immunol Invest 36:629–648
Brusko TM, Hulme MA, Myhr CB et al (2007) Assessing the in vitro suppressive capacity of regulatory T cells. Immunol Invest 36:607–628
Capriotti E, Vonderheid EC, Thoburn CJ et al (2008) Expression of T-plastin, FoxP3 and other tumor-associated markers by leukemic T-cells of cutaneous T-cell lymphoma. Leuk Lymphoma 49:1190–1201
Tuve S, Chen BM, Liu Y et al (2007) Combination of tumor site-located CTL-associated antigen-4 blockade and systemic regulatory T-cell depletion induces tumor-destructive immune responses. Cancer Res 67:5929–5939
Matsuura K, Yamaguchi Y, Ueno H et al (2006) Maturation of dendritic cells and T-cell responses in sentinel lymph nodes from patients with breast carcinoma. Cancer 106:1227–1236
Bates GJ, Fox SB, Han C et al (2006) Quantification of regulatory T cells enables the identification of high-risk breast cancer patients and those at risk of late relapse. J Clin Oncol 24:5373–5380
Hodi FS, Mihm MC, Soiffer RJ et al (2003) Biologic activity of cytotoxic T lymphocyte-associated antigen 4 antibody blockade in previously vaccinated metastatic melanoma and ovarian carcinoma patients. Proc Natl Acad Sci USA 100:4712–4717
Phan GQ, Yang JC, Sherry RM et al (2003) Cancer regression and autoimmunity induced by cytotoxic T lymphocyte-associated antigen 4 blockade in patients with metastatic melanoma. Proc Natl Acad Sci USA 100:8372–8377
Acknowledgements
This work was funded by grant no. 87-4330 from Shiraz University of Medical Sciences and by Iranian Cancer Network and Shiraz Institute for Cancer Research (ICR-87-505). We also are grateful to the women with and without breast cancer who participated in this project.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jaberipour, M., Habibagahi, M., Hosseini, A. et al. Increased CTLA-4 and FOXP3 Transcripts in Peripheral Blood Mononuclear Cells of Patients with Breast Cancer. Pathol. Oncol. Res. 16, 547–551 (2010). https://doi.org/10.1007/s12253-010-9256-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12253-010-9256-8