Abstract
Objectives
To compare the change in serum vitamin D levels and to compare the changes in serum levels of calcium, phosphate, alkaline phosphatase and parathyroid hormone in vitamin D supplemented and unsupplemented groups after 3 mo.
Methods
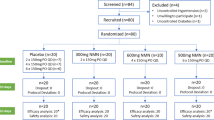
In this randomized, parallel group, nonblinded, controlled trial, 40 children, 2–12 y of age with newly diagnosed epilepsy, and vitamin D sufficient status, and started on valproate monotherapy, were randomized into the intervention group (n = 20), which was given daily oral 600 IU vitamin D supplementation, and the control group (n = 20), which was not given any supplementation. Changes in the biochemical parameters was measured in the two groups after 3 mo.
Results
There was a significant reduction in the median (IQR) vitamin D levels in the control group as compared to an increase seen in the intervention group [−6.64 (−8.4, −2.65) vs. 5.66 (1.81, 7.12); p < 0.001]. In the control group, 37.5% children developed vitamin D insufficiency and 12.5% developed deficiency whereas only 5% of the intervention group developed vitamin D insufficiency (p = 0.005). There was a significant decrease in ionized calcium (p = 0.02), increase in serum phosphate (p = 0.02), and alkaline phosphatase level (p = 0.003) in the unsupplemented group as compared to the supplemented group.
Conclusion
Vitamin D supplementation can reduce the valproate-associated decline in vitamin D levels and the negative impact on other markers of bone mineral metabolism.
Trial Registration
TCTR20200621002, 19.06.2020, retrospectively registered.


Similar content being viewed by others
References
Egunsola O, Choonara I, Sammons HM. Antiepileptic drug utilisation in paediatrics: a systematic review. BMJ Paediatr Open. 2017;1:e000088.
Vestergaard P. Effects of antiepileptic drugs on bone health and growth potential in children with epilepsy. Paediatr Drugs. 2015;17:141–50.
Zhang Y, Zheng YX, Zhu JM, Zhang JM, Zheng Z. Effects of antiepileptic drugs on bone mineral density and bone metabolism in children: a meta-analysis. J Zhejiang Univ Sci B. 2015;16:611–21.
Lee Y-J, Park KM, Kim YM, Yeon GM, Nam SO. Longitudinal change in vitamin status in children with epilepsy on anti-epileptic drugs: prevalence and risk factors. Pediatr Neurol. 2015;52:153–9.
Oner N, Kaya M, Karasalihoğlu S, Karaca H, Celtik C, Tütüncüler F. Bone mineral metabolism changes in epileptic children receiving valproic acid. J Paediatr Child Health. 2004;40:470–3.
Kapil U, Pandey RM, Goswami R, et al. Prevalence of vitamin D deficiency and associated risk factors among children residing at high altitude in Shimla district, Himachal Pradesh. India Indian J Endocr Metab. 2017;21:178–83.
Marwaha RK, Tandon N, Reddy DR, et al. Vitamin D and bone mineral density status of healthy school children in Northern India. Am J Clin Nutr. 2005;82:477–82.
Mandlik R, Kajale N, Ekbote V, et al. Determinants of vitamin D status in Indian school children. Indian J Endocr Metab. 2018;22:244–8.
Munns CF, Shaw N, Kiely M, et al. Global consensus recommendations on prevention and management of nutritional rickets. J Clin Endocrinol Metab. 2016;101:394–415.
Seth A, Aneja S, Singh R, Majumdar R, Sharma N, Gopinath M. Effect of impaired ambulation and anti-epileptic drug intake in vitamin D status of children with cerebral palsy. Pediatr Int Child Health. 2017;37:193–8.
Aggarwal V, Seth A, Aneja S, et al. Role of calcium deficiency in development of nutritional rickets in Indian children: a case control study. J Clin Endocrinol Metab. 2012;97:3461–6.
WHO Multicentre Growth Reference Study Group. WHO child growth standards based on length/height, weight and age. Acta paediatr Suppl. 2006;450:76–85.
Indian Academy of Pediatrics Growth Charts Committee, Khadilkar V, Yadav S, Agrawal KK, et al. Revised IAP growth charts for height, weight and body mass index for 5-to 18-year-old Indian children. Indian Pediatr. 2015;52:47–55.
Scheffer IE, Berkovic S, Capovilla G, et al. ILAE classification of the epilepsies: position paper of the ILAE commission for classification and terminology. Epilepsia. 2017;58:512–21.
Fisher RS, Cross JH, D'souza C, et al. Instruction manual for the ILAE 2017 operational classification of seizure types. Epilepsia. 2017;58:531–42.
Durá-Travé T, Gallinas-Victoriano F, Malumbres-Chacón M, Moreno-Gónzalez P, Aguilera-Albesa S, Yoldi-Petri ME. Vitamin D deficiency in children with epilepsy taking valproate and levetiracetam as monotherapy. Epilepsy Res. 2018;139:80–4.
Vijaykumar M, BK A, George B, Bhatia V. Vitamin D status in children on anticonvulsant therapy. Indian J Pediatr. 2021. https://doi.org/10.1007/s12098-021-03853-y.
Krishnamoorthy G, Nair R, Sundar U, Kini P, Shrivastava M. Early predisposition to osteomalacia in Indian adults on phenytoin or valproate monotherapy and effective prophylaxis by simultaneous supplementation with calcium and 25-hydroxy vitamin D at recommended daily allowance dosage: a prospective study. Neurol India. 2010;58:213–9.
Papassava M, Siomou E, Nakou I, Cholevas V, Challa A, Tzoufi M. Effects of long-term antiepileptic polytherapy on bone biochemical markers in ambulatory children and adolescents and possible benefits of vitamin D supplementation: a prospective interventional study. Epilepsy Behav. 2021;115:107708.
Mikati MA, Dib L, Yamout B, Sawaya R, Rahi AC, Fuleihan Gel-H. Two randomized vitamin D trials in ambulatory patients on anticonvulsants: impact on bone. Neurology. 2006;67:2005–14.
Babayigit A, Dirik E, Bober E, Cakmakci H. Adverse effects of anti-epileptic drugs on bone mineral density. Pediatr Neurol. 2006;35:177–81.
Albaghdadi O, Alhalabi MS, Alourfi Z, Youssef LA. Bone health and vitamin D status in young epilepsy patients on valproate monotherapy. Clin Neurol Neurosurg. 2016;146:52–6.
Offermann G, Pinto V, Kruse R. Antiepileptic drugs and vitamin D supplementation. Epilepsia. 1979;20:3–15.
Chaudhuri JR, Mridula KR, Rathnakishore C, Balaraju B, Bandaru VS. Association of 25-hydroxyvitamin D deficiency in pediatric epileptic patients. Iran J Child Neurol. 2017;11:48–56.
Christiansen C, Rodbro P, Lund M. Effect of vitamin D on bone mineral mass in normal subjects and in epileptic patients on anticonvulsants: a controlled therapeutic trail. Br Med J. 1973;2:208–9.
Gauci Z, Rizzo C, Mifsud S, Cachia MJ. Paradoxical deterioration in seizure control due to anticonvulsant-induced hypocalcemia. BMJ Case Rep. 2019;12:e232429
Funding
None.
Author information
Authors and Affiliations
Contributions
DM conceptualized and planned the study, supervised the conduct of the study, and assisted in the statistical analysis and finalization of the manuscript; SM assisted in planning the study and statistical analysis, evaluated and enrolled the patients and carried out sample collection, carried out follow-up and assessed the outcomes, and prepared the initial draft of the manuscript; MM provided important intellectual inputs in planning and conduct of the study, and assisted in manuscript preparation; BM provided important intellectual inputs in planning and conduct of the study, and supervised the sample storage and analysis; AMK provided important intellectual inputs in planning and conduct of the study, and the data analysis. All authors approved the final manuscript. DM will act as the guarantor for this paper.
Corresponding author
Ethics declarations
Ethics Approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Maulana Azad Medical College, University of Delhi (F.No./17/IEC/MAMC/2018/09).
Consent to Participate
Informed consent was taken from parents and assent was taken from all participants 7 to 12 y of age.
Conflict of Interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mishra, S., Mishra, D., Mahajan, B. et al. Effect of Daily Vitamin D Supplementation on Serum Vitamin D Levels in Children with Epilepsy Receiving Sodium Valproate Monotherapy: A Randomized, Controlled Trial. Indian J Pediatr 90, 450–456 (2023). https://doi.org/10.1007/s12098-022-04225-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-022-04225-w