Abstract
Background
Soft tissue sarcomas (STS) have a high risk of relapse in spite of the use of (neo)adjuvant chemotherapy. In this context, looking for new prognostic biomarkers is an interesting field of research. Our aim is to analyze the prognostic impact of neutrophil-to-lymphocyte ratio (NLR) and other serum markers in patients with STS who received chemotherapy with curative intent.
Materials and methods
This is a retrospective observational study. We included all patients with STS (primary tumor, local recurrence or resected metastatic disease) treated with high-dose ifosfamide and epirubicin with curative intent from January 2007 to December 2018. The pretreatment NLR and other serum markers were calculated, selecting the median as the cut-off value for the survival and multivariate analysis.
Results
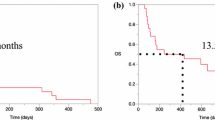
Seventy-nine patients were included. Median NLR, platelet-to-lymphocyte ratio (PLR) and lymphocyte-to-monocyte ratio (LMR) were 2.83, 174.05 and 3.25, respectively. Median progression-free survival (PFS) was significantly longer in patients with low NLR [not reached (NR) vs 21, 92 months, P < 0.01]. No significant differences were found for PFS regarding PLR or LMR. For overall survival (OS), a significant survival advantage was also found for patients with low NLR (NR vs 65.45 months, P = 0.01), without differences for PLR or LMR. In multivariate analysis, NLR remains an independent prognostic factor for PFS.
Conclusion
In our cohort, low NLR was significantly associated with a longer PFS and OS, and is consolidated as an independent prognostic factor.


Similar content being viewed by others
References
Stiller CA, Trama A, Serraino D, et al. Descriptive epidemiology of sarcomas in Europe: report from the RARECARE project. Eur J Cancer. 2013;49:684–95.
Casali PG, Abecassis N, Aro HT, et al. Soft tissue and visceral sarcomas: ESMO-EURACAN Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2018;29(Suppl 4):iv268–iv269. https://doi.org/10.1093/annonc/mdy321.
Gronchi A, Ferrari S, Quagliuolo V, et al. Histotype-tailored neoadjuvant chemotherapy versus standard chemotherapy in patients with high-risk soft-tissue sarcomas (ISG-STS 1001): an international, open-label, randomised, controlled, phase 3, multicentre trial. Lancet Oncol. 2017;18(6):812–22. https://doi.org/10.1016/S1470-2045(17)30334-0(Epub 2017 May 9).
Pasquali S, Colombo C, Pizzamiglio S, et al. High-risk soft tissue sarcomas treated with perioperative chemotherapy: improving prognostic classification in a randomised clinical trial. Eur J Cancer. 2018;93:28–36. https://doi.org/10.1016/j.ejca.2018.01.071(Epub 2018 Feb 21).
Grivennikov SI, Greten FR, Karin M. Immunity, inflammation, and cancer. Cell. 2010;140(6):883–99. https://doi.org/10.1016/j.cell.2010.01.025.
Liu G, Ke LC, Sun SR. Prognostic value of pretreatment neutrophil-to-lymphocyte ratio in patients with soft tissue sarcoma: a meta-analysis. Medicine (Baltimore). 2018;97(36):e12176. https://doi.org/10.1097/MD.0000000000012176.
Mirili C, Paydaş S, Guney IB. Assessment of potential predictive value of peripheral blood inflammatory indexes in 26 cases with soft tissue sarcoma treated by pazopanib: a retrospective study. Cancer Manag Res. 2019;11:3445–533. https://doi.org/10.2147/CMAR.S191199(eCollection 2019).
Aggerholm-Pedersen N, Maretty-Kongstad K, Keller J, et al. Serum biomarkers as prognostic factors for metastatic sarcoma. Clin Oncol (R Coll Radiol). 2019;31(4):242–9. https://doi.org/10.1016/j.clon.2019.01.011(Epub 2019 Feb 7).
Kobayashi H, Okuma T, Oka H, et al. Neutrophil-to-lymphocyte ratio after pazopanib treatment predicts response in patients with advanced soft-tissue sarcoma. Int J Clin Oncol. 2018;23(2):368–74. https://doi.org/10.1007/s10147-017-1199-6(Epub 2017 Oct 31).
Jiang L, Jiang S, Situ D, et al. Prognostic value of monocyte and neutrophils to lymphocytes ratio in patients with metastatic soft tissue sarcoma. Oncotarget. 2015;6(11):9542–50.
Park G, Song SY, Ahn JH, et al. The pretreatment erythrocyte sedimentation rate predicts survival outcomes after surgery and adjuvant radiotherapy for extremity soft tissue sarcoma. Radiat Oncol. 2019;14(1):116. https://doi.org/10.1186/s13014-019-1331-z.
Liang Y, Hou T, Que Y, et al. Elevated Controlling Nutritional Status (CONUT) score is associated with poor long-term survival in patients with low-grade soft-tissue sarcomas treated with surgical resection. Clin Orthop Relat Res. 2019. https://doi.org/10.1097/CORR.0000000000000767.
Yanagisawa M, Gingrich AA, Judge S, et al. Serum C-reactive protein and neutrophil/lymphocyte ratio after neoadjuvant radiotherapy in soft tissue sarcoma. Anticancer Res. 2018;38(3):1491–7.
Liang Y, Xiao W, Guan YX, et al. Prognostic value of the C-reactive protein/Albumin Ratio (CAR) in patients with operable soft tissue sarcoma. Oncotarget. 2017;8(58):98135–47. https://doi.org/10.18632/oncotarget.20990(eCollection 2017 Nov 17).
Que Y, Qiu H, Li Y, et al. Preoperative platelet-lymphocyte ratio is superior to neutrophil-lymphocyte ratio as a prognostic factor for soft-tissue sarcoma. BMC Cancer. 2015;2(15):648. https://doi.org/10.1186/s12885-015-1654-6.
Szkandera J, Gerger A, Liegl-Atzwanger B, et al. The derived neutrophil/lymphocyte ratio predicts poor clinical outcome in soft tissue sarcoma patients. Am J Surg. 2015;210(1):111–6. https://doi.org/10.1016/j.amjsurg.2014.10.021(Epub 2014 Dec 18).
García-Ortega DY, Álvarez-Cano A, Sánchez-Llamas LA, et al. Neutrophil/lymphocyte ratio is associated with survival in synovial sarcoma. Surg Oncol. 2018;27(3):551–5. https://doi.org/10.1016/j.suronc.2018.07.012(Epub 2018 Jul 18).
Maretty-Kongstad K, Aggerholm-Pedersen N, Keller J. A validated prognostic biomarker score for adult patients with nonmetastatic soft tissue sarcomas of the trunk and extremities. Transl Oncol. 2017;10(6):942–8. https://doi.org/10.1016/j.tranon.2017.09.002(Epub 2017 Oct 11).
Li Y, Liu X, Zhang J, et al. Prognostic role of elevated preoperative systemic inflammatory markers in localized soft tissue sarcoma. Cancer Biomark. 2016;16(3):333–42. https://doi.org/10.3233/CBM-160571.
Choi ES, Kim HS, Han I, et al. Elevated preoperative systemic inflammatory markers predict poor outcome in localized soft tissue sarcoma. Ann Surg Oncol. 2014;21(3):778–85. https://doi.org/10.1245/s10434-013-3418-3(Epub 2013 Dec 4).
Szkandera J, Absenger G, Liegl-Atzwanger B, et al. Elevated preoperative neutrophil/lymphocyte ratio is associated with poor prognosis in soft-tissue sarcoma patients. Br J Cancer. 2013;108(8):1677–83. https://doi.org/10.1038/bjc.2013.135(Epub 2013 Apr 4).
Idowu OK, Ding Q, Taktak AF, et al. Clinical implication of pretreatment neutrophil to lymphocyte ratio in soft tissue sarcoma. Biomarkers. 2012;17(6):539–44. https://doi.org/10.3109/1354750X.2012.699554(Epub 2012 Jul 16).
Liang Y, Wang W, Li J, et al. Combined use of the neutrophil-lymphocyte and platelet-lymphocyte ratios as a prognostic predictor in patients with operable soft tissue sarcoma. J Cancer. 2018;9(12):2132–9. https://doi.org/10.7150/jca.24871(eCollection 2018).
Nakamura T, Matsumine A, Matsubara T, et al. The combined use of the neutrophil-lymphocyte ratio and C-reactive protein level as prognostic predictors in adult patients with soft tissue sarcoma. J Surg Oncol. 2013;108(7):481–5. https://doi.org/10.1002/jso.23424(Epub 2013 Sep 9).
Pisters PW, Leung DH, Woodruff J, et al. Analysis of prognostic factors in 1,041 patients with localized soft tissue sarcomas of the extremities. J Clin Oncol. 1996;14(5):1679–89.
Kattan MW, Leung DH, Brennan MF. Postoperative nomogram for 12-year sarcoma-specific death. J Clin Oncol. 2002;20(3):791.
Dalal KM, Kattan MW, Antonescu CR, et al. Subtype specific prognostic nomogram for patients with primary liposarcoma of the retroperitoneum, extremity, or trunk. Ann Surg. 2006;244(3):381.
Sampo M, Tarkkanen M, Tukiainen E, et al. A web-based prognostic tool for extremity and trunk wall soft tissue sarcomas and its external validation. Br J Cancer. 2012;106(6):1076–82 (Epub 2012 Feb 2).
Callegaro D, Miceli R, Mariani L, et al. Soft tissue sarcoma nomograms and their incorporation into practice. Cancer. 2017;123(15):2802–20. https://doi.org/10.1002/cncr.30721(Epub 2017 May 10).
Callegaro D, Miceli R, Bonvalot S, et al. Development and external validation of two nomograms to predict overall survival and occurrence of distant metastases in adults after surgical resection of localised soft-tissue sarcomas of the extremities: a retrospective analysis. Lancet Oncol. 2016;17(5):671–80. https://doi.org/10.1016/S1470-2045(16)00010-3(Epub 2016 Apr 5).
Funding
This work has not been supported by public grants or financial support. No sources of funding were used to assist in the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization: Andres Redondo, David Viñal; data collection: David Viñal, Daniel Martinez, Jose Angel Garcia-Cuesta, Laura Gutierrez-Sainz, Sergio Martinez-Recio, Julia Villamayor; data analysis: David Viñal, Daniel Martinez, Laura Gutierrez, Sergio Martinez-Recio. writing—original draft preparation: David Viñal, Daniel Martinez, Andres Redondo; writing—review and editing: Virginia Martinez-Marin, Alejandro Gallego, Eduardo Ortiz-Cruz, Marta Mendiola, Jose Juan Pozo-Kreilinger, Alberto Berjon, Belen Belinchon, Daniel Bernabeu, Enrique Espinosa, Jaime Feliu, Andres Redondo; supervision: Andres Redondo, Jaime Feliu.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the Ethics Committee of the La Paz University Hospital. This article does not contain any studies with animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Viñal, D., Martinez, D., Garcia-Cuesta, J.A. et al. Prognostic value of neutrophil-to-lymphocyte ratio and other inflammatory markers in patients with high-risk soft tissue sarcomas. Clin Transl Oncol 22, 1849–1856 (2020). https://doi.org/10.1007/s12094-020-02324-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-020-02324-8