Abstract
Background & aims
Few studies have investigated the prognosis of patients with non-severe alcoholic hepatitis (Non-SAH). The study aimed to develop a new prognostic model for patients with especially Non-SAH.
Methods
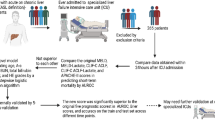
We extracted 316 hospitalized patients with alcoholic cirrhosis without severe alcoholic hepatitis, defined as Maddrey’s discriminant function score lower than 32, from the retrospective Korean Acute-on-Chronic Liver Failure (KACLiF) cohort to develop a new prognostic model (training set), and validated it in 419 patients from the prospective KACLiF cohort (validation set). Prognostic factors for death and liver transplantation were analyzed to construct a prognostic model.
Results
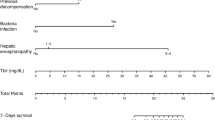
Twenty-one and 24 patients died within 6 months in both sets, respectively. In the training set, the highest area under the curve (AUC) of conventional prognostic models was 0.765, 0.732, and 0.684 for 1-, 3-, and 6-month mortality, respectively. Refractory ascites, vasopressor use, and hyponatremia were independently associated with mortality of cirrhotic patients with Non-SAH. The new model consisted of four variables: past deterioration, neutrophil proportion > 70%, Na < 128 mmol/L, and vasopressor use. It showed the highest accuracy for short-term mortality in the training and validation sets (0.803 and 0.786; 0.797 and 0.776; and 0.789 and 0.721 for 1-, 3-, and 6-month mortality, respectively).
Conclusion
There is a group of patients with high risk among those classified as Non-SAH. The new model will help stratifying cirrhotic patients with Non-SAH more accurately in terms of prognosis. The patients with high Non-SAH score need to monitor closely and might be considered for preemptive liver transplantation.
Trial regestration
ClinicalTrials.gov identifier: NCT02650011.


Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the current study are not publicly available due personal medical records, but are available from the corresponding author on reasonable request and approval of IRB.
References
Wong RJ, Singal AK. Trends in lliver ddisease eetiology aamong aadults aawaiting lliver ttransplantationliver disease etiology among adults awaiting liver transplantation in the United States, 2014–2019. JAMA Netw Open. 2020;3(2): e1920294
European Association for the Study of the Liver (EASL). EASL clinical practice guidelines: management of alcohol-related liver disease. J Hepatol. 2018;69(1):154–181
Bennett K, Enki DG, Thursz M, Cramp ME, Dhanda AD. Systematic review with meta-analysis: high mortality in patients with non-severe alcoholic hepatitis. Aliment Pharmacol Ther. 2019;50:249–257
Louvet A, Labreuche J, Artru F, et al. Main drivers of outcome differ between short term and long term in severe alcoholic hepatitis: a prospective study. Hepatol. 2017;66:1464–1473
Shin J, Yu JH, Jin Y-J, et al. Acute-on-chronic liver failure as a major predictive factor for mortality in patients with variceal bleeding. Clin Mol Hepatol. 2020;26:540–553
Kim JH, Kim SE, Song DS, et al. Platelet-to-white blood cell ratio is associated with adverse outcomes in cirrhotic patients with acute deterioration. J Clin Med. 2022;11:2463
Yoon EL, Kim TY, Song DS, et al. The impact of previous acute decompensation on the long-term prognosis of alcoholic hepatitis in cirrhotic patients. J Clin Med. 2019;8:1600
Kim TH, Um SH, Lee YS, et al. Determinants of re-compensation in patients with hepatitis B virus-related decompensated cirrhosis starting antiviral therapy. Aliment Pharmacol Ther. 2022;55:83–96
Korean Association for the Study of the Liver (KASL). KASL clinical practice guidelines: management of alcoholic liver disease. Clin Mol Hepatol. 2013;19:216–254
Bone RC, Balk RA, Cerra FB, et al. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest. 1992;101:1644–1655
Sarin SK, Choudhury A, Sharma MK, et al. Acute-on-chronic liver failure: consensus recommendations of the Asian Pacific association for the study of the liver (APASL): an update. Hepatol Int. 2019;13:353–390
Tornai D, Szabo G. Emerging medical therapies for severe alcoholic hepatitis. Clin Mol Hepatol. 2020;26:686–696
Degré D, Stauber RE, Englebert G, et al. Long-term outcomes in patients with decompensated alcohol-related liver disease, steatohepatitis and Maddrey’s discriminant function <32. J Hepatol. 2020;72:636–642
Moreau R. Acute-on-chronic liver failure: a new syndrome in cirrhosis. Clin Mol Hepatol. 2016;22:1–6
Korean Association for the Study of the Liver (KASL). KASL clinical practice guidelines for liver cirrhosis: ascites and related complications. Clin Mol Hepatol. 2018;24:230–277
Kim TH, Ku DH, Um SH, et al. How can we improve the performance of model for end-stage liver disease sodium score in patients with hepatitis B virus-related decompensated liver cirrhosis commencing antiviral treatment? J Gastroenterol Hepatol. 2018;33:1641–1648
Kim WR, Mannalithara A, Heimbach JK, et al. MELD 3.0: the model for end-stage liver disease updated for the Modern Era. Gastroenterology. 2021;161:1887–1895
Cárdenas A, Solà E, Rodríguez E, et al. Hyponatremia influences the outcome of patients with acute-on-chronic liver failure: an analysis of the CANonIC study. Crit Care. 2014;18:700
Ginès P, Krag A, Abraldes JG, Solà E, Fabrellas N, Kamath PS. Liver cirrhosis. Lancet. 2021;398:1359–1376
Clària J, Stauber RE, Coenraad MJ, et al. Systemic inflammation in decompensated cirrhosis: characterization and role in acute-on-chronic liver failure. Hepatol. 2016;64:1249–1264
Forrest EH, Storey N, Sinha R, et al. Baseline neutrophil-to-lymphocyte ratio predicts response to corticosteroids and is associated with infection and renal dysfunction in alcoholic hepatitis. Aliment Pharmacol Ther. 2019;50:442–453
Chen L, Lou Y, Chen Y, Yang J. Prognostic value of the neutrophil-to-lymphocyte ratio in patients with acute-on-chronic liver failure. Int J Clin Pract. 2014;68:1034–1040
Cai YJ, Dong JJ, Dong JZ, et al. A nomogram for predicting prognostic value of inflammatory response biomarkers in decompensated cirrhotic patients without acute-on-chronic liver failure. Aliment Pharmacol Ther. 2017;45:1413–1426
Sun J, Guo H, Yu X, et al. A neutrophil-to-lymphocyte ratio-based prognostic model to predict mortality in patients with HBV-related acute-on-chronic liver failure. BMC Gastroenterol. 2021;21:422
Trebicka J, Fernandez J, Papp M, et al. The PREDICT study uncovers three clinical courses of acutely decompensated cirrhosis that have distinct pathophysiology. J Hepatol. 2020;73:842–854
Acknowledgments
We thank the Collaborators of the Korean Acute-on-Chronic Liver Failure (KACLiF) study group, and Editage (www.editage.co.kr) for English language editing.
Funding
This work was supported partly by Korea University Research Grants (No. K2119231) and partly by Basic Science Research Program (National Research Foundation of Korea), No. 2020R1A6A1A03043026.
Author information
Authors and Affiliations
Consortia
Contributions
Study conception and design: Yim HJ, Kim DJ; Acquisition of data: Yoon EL, Kang SH, Kim HY, Chang Y, Lee SW, Yoo JJ, Baek GJ, Park JK, Kim TY, Song DS, Park JW, Kim SE, Jeong SW, Suk KT, Jung YK, Kim MY, Kim SG, Jang JY, Kim W and Yang JM.; Data analysis and interpretation: Kim TH and Yim HJ.; Draft writing: Kim TH.; Review and final approval of the submission of the manuscript: Yim HJ, Jang JY and Kim DJ.
Corresponding authors
Ethics declarations
Conflict of interest
The authors Tae Hyung Kim, Hyung Joon Yim, Young Kul Jung, Do Seon Song, Eileen L. Yoon, Hee Yeon Kim, Seong Hee Kang, Young Chang, Jeong-Ju Yoo, Baek Gyu Jun, Sung Won Lee, Jung Gil Park, Ji Won Park, Sung-Eun Kim, Tae Yeob Kim, Soung Won Jeong, Ki Tae Suk, Moon Young Kim, Sang Gyune Kim, Won Kim, Jae Young Jang, Jin Mo Yang, Dong Joon Kim have no relevant financial or non-financial interests to disclose.
Ethical approval
The present study was approved by the institutional review board of each participating center (approval nos. 2014AS0123 and 2015AS0090 from the center of the corresponding author). All authors had access to the study data and had reviewed and approved the final manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kim, T.H., Yim, H.J., Jung, Y.K. et al. New prognostic model for hospitalized patients with alcoholic cirrhosis and Maddrey’s discriminant function <32. Hepatol Int 18, 500–508 (2024). https://doi.org/10.1007/s12072-023-10582-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-023-10582-1