Abstract
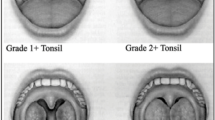
Adenotonsillar hypertrophy is one of the commonest causes of upper airway obstruction in children. It can cause hypoxic state by impairing pulmonary functions. Peak expiratory flow rate is a basic, convenient and reliable indicator of pulmonary function in children. To study the improvement in pulmonary functions by assessing Peak expiratory flow rate, before and after adenotonsillectomy in children. Design: Cross sectional, prospective, observational study. Setting: Department of otorhinolaryngology in tertiary care centre. Subjects: Included 40 children aged between 5 and 15 years, who had adenotonsillar hypertrophy and underwent adenotonsillectomy. Method: Diagnostic nasal endoscopy and X-ray, nasopharynx, was done to assess the grade of adenoid hypertrophy endoscopically and radiologically respectively. Peak expiratory flow rate was assessed using Mini Wright peak expiratory flow meter pre-operatively and 1 month post-operatively and both the readings were compared. Subjective improvement was also compared pre-operatively and post-operatively using visual analogue score. This study included 40 patients with male to female ratio of 1.6:1, 92.5% presented with mouth breathing. 92.5% presented with grade III tonsillar hypertrophy and 70% with grade III adenoid hypertrophy endoscopically. After adenotonsillectomy, improvement in Peak expiratory flow rate ranged from 16 to 25.3% which was statistically significant. Patients with grade III tonsillar and grade IV adenoid hypertrophy showed 25.3% improvement. Subjective improvement was 98.8% in the complaint of snoring. Adenotonsillectomy significantly improves pulmonary functions. This may help to improve physical and cognitive development in children and decrease chances of getting cardiopulmonary problems in later life.

Similar content being viewed by others
References
Niedzielska G, Kotowski M, Niedzielski A (2008) Assessment of pulmonary function and nasal flow in children with adenoid hypertrophy. Int J Pediatr Otorhinolaryngol 72:333–335
Wiatrak BJ, Woolley AL (1998) Pharyngitis and Adenotonsillar disease. In: Cummings CW, Fredrickson JM, Harker LA, Krause CT, Richardson MA, Schuller DE (eds) Pediatric otolaryngology-head and neck surgery, 3rd edn. Mosby Year Book, St Louis, pp 188–215
American Academy of Otolaryngology-Head and Neck Surgery; Clinical Indicators: Adenoidectomy. http://www.entnet.org/Practice/upload/Adenoidectomy-CI_Final-May-2012.pdf. Accessed 14 Aug 2013
Ali NJ, Pitson D, Stradling JR (1996) Effects of adenotonsillectomy on behavior and psychological functioning. Eur J Pediatr 155:56–62
Shirley WP, Woolley AL, Wiatrak BJ (2010) Pharyngitis and adenotonsillar disease. Otolaryngology: head and neck surgery, 5th edn. Mosby, Philadelphia, pp 2782–2802
Mead J, Turner JM, Macklem PT et al (1967) Significance of the relationship between lung recoil and maximum expiratory flow. J Appl Physiol 22:95–108
Wille and Svensson, 1989; Perks, Tams, Thompson, 1979; deHamel, 1982; Burns, 1979; Perks, Cole, Steventon, 1981.
Milner AD, Ingram D (1970) Peak expiratory flow rates in children under 5 years of age. Arch Dis Child 45(244):780–782
Rogha M, Amini J, Raisi M (2016) Pulmonary function after adenotonsillectomy. Iran J Otorhinolaryngol 28(89):383
Crepeau J, Patriquin HB, Poliquin JF, Tetreault L (1982) Radiographic evaluation of the symptom-producing adenoid. Otolaryngol Head Neck Surg 90(5):548–554
Hubballi RK, Nayaka GSSS, Koujalagi SM (2020) Clinical correlation between tonsillar hypertrophy and tonsillitis. Int J Otorhinolaryngol Head Neck Surg 6:132–136
Sarwar SM, Rahman M, Ali MI, Alam MM, Hossain MA, Sanyal NP (2015) Correlation of enlarged adenoids with conductive hearing impairment in children under twelve. Bangladesh J Otorhinolaryngol 21(2):62–68
Ren DD, Wang WQ (2012) Assessment of middle ear effusion and audiological characteristics in young children with adenoid hypertrophy. Chin Med J 125(7):1276–1281
Hamza SB, Ranjith VT (2019) Assessment of size of adenoid-comparison of adenoidal nasopharyngeal ratio and nasal endoscopy in children with chronic adenoiditis. Int J Res Med Sci 7:776–781
Koc S, Aytekin M, Kalay N, Ozcetin M, Burucu T, Ozbek K, Celik A, Kadi H, Gulturk S, Koc F (2012) The effect of adenotonsillectomy on right ventricle function and pulmonary artery pressure in children with adenotonsillar hypertrophy. Int J Pediatr Otorhinolaryngol 76(1):45–48
Cassano P, Gelardi M, Cassano M, Fiorella ML, Fiorella R (2003) Adenoid tissue rhinopharyngeal obstruction grading based on fiberendoscopic findings: a novel approach to therapeutic management. Int J Pediatr Otorhinolaryngol 67(12):1303–1309
Lourenço EA, Lopes KD, Pontes Á Jr, Oliveira MH, Umemura A, Vargas AL (2005) Comparison between radiological and nasopharyngolaryngoscopic assessment of adenoid tissue volume in mouth breathing children. Revista Brasileira de Otorrinolaringologia 71(1):23–28
Yaseen ET, Khammas AH, Al-Anbaky F (2012) Adenoid enlargement assessment by plain X-ray & nasoendoscopy. Iraqi J Commun Med 25(1):88–91
Yadav J, Gathwala G, Sood S, Maharjan M, Singh I (2005) Effect of adenotonsillitis on peak exploratory flow rate in children. JNMA J Nepal Med Assoc 44(160):135–137
Ahmed M, Gavhane J, Goel S (2017) Age specific peak expiratory flow nomogram in children. Indian J Pediatr 84(4):271–275
Fekri MS, Mianroodi AA, Shakeri H, Khanjani N (2016) Effects of tonsil size on pulmonary function test results after tonsillectomy in children. Iran J Otorhinolaryngol 28(84):61
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
Clearance obtained from Ethical committee of Institute- wide letter no. SRHU/HIMS/RC/2021/42.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Singhal, A., Kumar, L., Agarwal, V.K. et al. Effect of Adenotonsillectomy on Peak Expiratory Flow Rate Among Children. Indian J Otolaryngol Head Neck Surg 74 (Suppl 3), 6491–6496 (2022). https://doi.org/10.1007/s12070-021-02748-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-021-02748-w