Abstract
Purpose
Thyroid-associated ophthalmopathy (TAO) may result in increased metabolism and abnormalities in microcirculation. The fractal dimension (Df) of retinal vessels has been shown to be related to the pathology of a number of ophthalmic disorders, but it hasn’t been investigated in TAO.
Methods
We analyzed 1078 participants aged 18 to 72 (548 healthy volunteers and 530 TAO). Images were captured using a non-mydriatic 45-degree fundus camera. Baseline retinal characteristics, such as vessel width, tortuosity, and Df were measured using semiautomated software from fundus images. The average retinal parameters were compared between the two groups. The receiver operation curve (ROC) was used to assess the diagnostic efficacy of various retinal vascular parameters for TAO.
Results
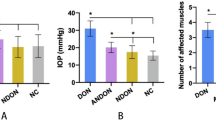
Despite controlling for potential confounding variables, Df, vessel width, and tortuosity significantly increased in TAO compared to healthy volunteers. Compared to active TAO, patients in the inactive phase had a larger retinal venous caliber (p < 0.05), but there was no difference in Df or arterial caliber. Moderate and severe cases had a higher Df compared with mild cases (EUGOGO guidelines). The area under the ROC for Df, tortuosity, and vascular caliber in the diagnosis of TAO was 0.904 (95% CI: 0.884–0.924), 0.638 (95% CI: 0.598–0.679), and 0.617 (95% CI: 0.576–0.658), respectively.
Conclusions
Due to its accessibility, affordability, and non-invasive nature, retinal vascular Df may serve as a surrogate marker for TAO and might be used to identify severe cases. With relatively high diagnostic performance, the Df is of some utility for the detection of TAO.




Similar content being viewed by others
References
T.J. Smith, J.A.M.J.L. Janssen, Insulin-like growth Factor-I receptor and thyroid-associated ophthalmopathy. Endocr. Rev. 40(1), 236–267 (2019). https://doi.org/10.1210/er.2018-00066
P.N. Taylor, L. Zhang, R.W.J. Lee et al. New insights into the pathogenesis and nonsurgical management of Graves orbitopathy. Nat. Rev. Endocrinol. 16(2), 104–116 (2020). https://doi.org/10.1038/s41574-019-0305-4
Y. Wu, Q. Yang, L. Ding et al. Peripapillary structural and microvascular alterations in early dysthyroid optic neuropathy. Eye Vis. Lond. Engl. 9(1), 30 (2022). https://doi.org/10.1186/s40662-022-00301-6
T.J. Smith, L. Hegedüs, Graves’ disease. N. Engl. J. Med 375(16), 1552–1565 (2016). https://doi.org/10.1056/NEJMra1510030
L. Ye, S.S. Zhou, W.L. Yang et al. Retinal microvasculature alteration in active thyroid-associated ophthalmopathy. Endocr. Pr. 24(7), 658–667 (2018). https://doi.org/10.4158/EP-2017-0229
T. Zhang, W. Xiao, H. Ye, R. Chen, Y. Mao, H. Yang, Peripapillary and macular vessel density in dysthyroid optic neuropathy: an optical coherence tomography angiography study. Invest Ophthalmol. Vis. Sci. 60(6), 1863–1869 (2019). https://doi.org/10.1167/iovs.18-25941
J. Ye, W. Liu, X. Hu et al. Elevated pulse pressure correlated with reduced retinal peripapillary capillary in thyroid-associated ophthalmology with visual field defect. Front Endocrinol. 13, 941051 (2022). https://doi.org/10.3389/fendo.2022.941051
M. Jamshidian Tehrani, Z. Mahdizad, A. Kasaei, M.A. Fard, Early macular and peripapillary vasculature dropout in active thyroid eye disease. Graefes Arch. Clin. Exp. Ophthalmol. Albrecht Von. Graefes Arch. Klin. Exp. Ophthalmol. 257(11), 2533–2540 (2019). https://doi.org/10.1007/s00417-019-04442-8
X. Yang, D. Huang, S. Ai, X. Liang, J. Zhao, L. Fang, Retinal vessel oxygen saturation and vessel diameter in inactive graves ophthalmopathy. Ophthal Plast. Reconstr. Surg. 33(6), 459–465 (2017). https://doi.org/10.1097/IOP.0000000000000826
A. Sadeghi-Tari, M. Jamshidian-Tehrani, A. Nabavi et al. Effect of smoking on retrobulbar blood flow in thyroid eye disease. Eye Lond. Engl. 30(12), 1573–1578 (2016). https://doi.org/10.1038/eye.2016.184
C. Del Noce, M. Roda, N. Valsecchi et al. Evaluation of peripapillary vascular flow in patients with Thyroid-Associated Ophthalmopathy (TAO) by OCT angiography. Graefes Arch. Clin. Exp. Ophthalmol. Albrecht Von. Graefes Arch. Klin. Exp. Ophthalmol. 260(8), 2711–2716 (2022). https://doi.org/10.1007/s00417-022-05551-7
Fractal analysis of the vascular tree in the human retina - PubMed. Accessed January 3, 2023. https://pubmed.ncbi.nlm.nih.gov/15255776/
M.A. Mainster, The fractal properties of retinal vessels: embryological and clinical implications. Eye Lond. Engl. 4(Pt 1), 235–241 (1990). https://doi.org/10.1038/eye.1990.33
S.W. Lim, N. Cheung, J.J. Wang et al. Retinal vascular fractal dimension and risk of early diabetic retinopathy: A prospective study of children and adolescents with type 1 diabetes. Diabetes Care 32(11), 2081–2083 (2009). https://doi.org/10.2337/dc09-0719
G. Liew, J.J. Wang, N. Cheung et al. The retinal vasculature as a fractal: methodology, reliability, and relationship to blood pressure. Ophthalmology 115(11), 1951–1956 (2008). https://doi.org/10.1016/j.ophtha.2008.05.029
B. Laviña, Brain Vascular Imaging Techniques. Int J. Mol. Sci. 18(1), 70 (2016). https://doi.org/10.3390/ijms18010070
F. Rb, G. Es, S. Aj, et al. Retinal venular tortuosity and fractal dimension predict incident retinopathy in adults with type 2 diabetes: the Edinburgh Type 2 Diabetes Study. Diabetologia. 2021;64(5). https://doi.org/10.1007/s00125-021-05388-5
C.Y. Cheung, G.N. Thomas, W. Tay et al. Retinal vascular fractal dimension and its relationship with cardiovascular and ocular risk factors. Am. J. Ophthalmol. 154(4), 663–674.e1 (2012). https://doi.org/10.1016/j.ajo.2012.04.016
X. Huang, Y. Zhong, M. Cai, X. Huang, Y. Zhong, M. Cai, Retinal vascular features and diagnostic values in patients with liver cirrhosis. J. NEW Med 52(4), 255 (2021). https://doi.org/10.3969/j.issn.0253-9802.2021.04.006
L. Shao, Q.L. Zhang, T.F. Long et al. Quantitative assessment of fundus tessellated density and associated factors in fundus images using artificial intelligence. Transl. Vis. Sci. Technol. 10(9), 23 (2021). https://doi.org/10.1167/tvst.10.9.23
X. Lyu, P. Jajal, M.Z. Tahir, S. Zhang, Fractal dimension of retinal vasculature as an image quality metric for automated fundus image analysis systems. Sci. Rep. 12(1), 11868 (2022). https://doi.org/10.1038/s41598-022-16089-3
Y. Wu, Y. Tu, L. Bao et al. Reduced retinal microvascular density related to activity status and serum antibodies in patients with graves’ ophthalmopathy. Curr. Eye Res. 45(5), 576–584 (2020). https://doi.org/10.1080/02713683.2019.1675177
T.V. Dave, S. Laghmisetty, G. Krishnamurthy et al. Retinal vascularity, nerve fiber, and ganglion cell layer thickness in thyroid eye disease on optical coherence tomography angiography. Orbit Amst. Neth. 41(2), 170–177 (2022). https://doi.org/10.1080/01676830.2020.1846761
M. Salvi, D. Dazzi, I. Pellistri, F. Neri, J.R. Wall. Classification and prediction of the progression of thyroid-associated ophthalmopathy by an artificial neural network. Ophthalmology. 2002;109(9). https://doi.org/10.1016/s0161-6420(02)01127-2
M. Jiang, X. Song, H. Zhang et al. The combination of T2-mapping value of lacrimal gland and clinical indicators can improve the stage prediction of Graves’ ophthalmopathy compared to clinical activity scores. Endocrine 78(2), 321–328 (2022). https://doi.org/10.1007/s12020-022-03167-9
Q. Ge, X. Zhang, L. Wang et al. Quantitative evaluation of activity of thyroid-associated Ophthalmopathy using short-tau inversion recovery (STIR) sequence. BMC Endocr. Disord. 21(1), 226 (2021). https://doi.org/10.1186/s12902-021-00895-3
B. Mandelbrot, How long is the coast of britain? Statistical self-similarity and fractional dimension. Science 156(3775), 636–638 (1967). https://doi.org/10.1126/science.156.3775.636
Z. Feng, G. Wang, H. Xia et al. Macular vascular geometry changes with sex and age in healthy subjects: a fundus photography study. Front. Med. 2021;8. https://doi.org/10.3389/fmed.2021.778346
J. Grauslund, A. Green, R. Kawasaki, L. Hodgson, A.K. Sjølie, T.Y. Wong, Retinal vascular fractals and microvascular and macrovascular complications in Type 1 diabetes. Ophthalmology 117(7), 1400–1405 (2010). https://doi.org/10.1016/j.ophtha.2009.10.047
Fractal analysis of the retinal vasculature and chronic kidney disease - PubMed. Accessed January 4, 2023. https://pubmed.ncbi.nlm.nih.gov/20124213/
Cheung N., Liew G., Lindley R.I. et al. Retinal fractals and acute lacunar stroke. Ann Neurol. 2010;68(1). https://doi.org/10.1002/ana.22011
G. Liew, P. Mitchell, E. Rochtchina et al. Fractal analysis of retinal microvasculature and coronary heart disease mortality. Eur. Heart J. 32(4), 422–429 (2011). https://doi.org/10.1093/eurheartj/ehq431
K. Fazil, G. Ozturk Karabulut, Z. Alkin, Evaluation of choroidal thickness and retinal vessel density in patients with inactive Graves’ orbitopathy. Photodiagnosis Photodyn. Ther. 32, 101898 (2020). https://doi.org/10.1016/j.pdpdt.2020.101898
Evaluation of retinal and choroidal variations in thyroid-associated ophthalmopathy using optical coherence tomography angiography - PubMed. Accessed January 4, 2023. https://pubmed.ncbi.nlm.nih.gov/33081749/
Funding
This work was supported by the National Natural Science Foundation of China (82071005); and the Special Fund of the Pediatric Medical Coordinated Development Center of Beijing Hospitals Authority, China (No. XTCX201824).
Author information
Authors and Affiliations
Contributions
X.J.: Funding acquisition, methodology, supervision, data curation, formal analysis, visualization and original draft writing. L.L., S.L. and D.Z.: Investigation, sample analysis, data curation, resources and review and editing of manuscript. D.L.: Conceptualization, funding acquisition, methodology, supervision, visualization and intellectual editing of manuscript. L.D.: original draft writing, manuscript preparation and final revisions. All authors contributed to the article and approved the submitted version.
Corresponding author
Ethics declarations
Ethics
This study is based on the latest version of the Declaration of Helsinki. All participants obtained written informed consent, and the study was approved by the Ethics Committee of Beijing Tongren Hospital
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jiang, X., Dong, L., Luo, L. et al. Artificial Intelligence-based quantitative evaluation of retinal vascular parameters in thyroid-associated ophthalmopathy. Endocrine (2024). https://doi.org/10.1007/s12020-023-03561-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12020-023-03561-x