Abstract
Purpose
To explore the relationship between miR-145 and ADP ribosylation factor 6 (Arf6) in regulating macrophage-mediated inflammation.
Methods
THP-1 cells were induced by 160 nM of phorbol 12−myristate 13-acetate (PMA) for 48 h to differentiate to macrophages and then were treated with LPS (100 ng/ml) for 8 h to simulate chronic metabolic inflammation in vitro. Dual-luciferase reporter assay was performed. MiR-145 siRNA and LV-ARF6-RNAi were used to up or down regulate miR-145 and Arf6 expression in THP-1 cells, respectively. Omental adipose tissue from patients in surgical ward were collected to detect the expression of miR-145, Arf6 and production of proinflammatory cytokines. Patients were divided into three groups according to their body mass index and history of diabetes.
Results
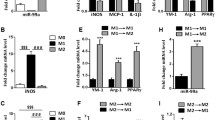
Dual-luciferase reporter assays showed the direct down-regulation of Arf6 by miR-145. Forty-eight-hour-transfection of miR-145 inhibitor resulted in significant increase of Arf6, IL-1beta, TNF-alpha and IL-6 as well as phosphorylation of p65 in NF-kappaB pathway in THP-1 cells, which, inversely, were reversed by overexpressing miR-145. In addition, down-regulation of Arf6 in macrophages reduced expression and secretion of cytokines. Expression of miR-145 was found to be attenuated in the omental adipose tissue of obese patients and diabetics with greater Arf6 expression, confirming the role of miR-145 in regulating macrophage-mediated inflammation targeting Arf6.
Conclusions
By means of reducing the expression of Arf6 and subsequent signal transduction via NF-kappaB, miR-145 plays a role in inhibiting the secretion of inflammatory factors and then improving the inflammatory status. MiR-145 might be one of the candidates for anti-inflammatory treatment for metabolic diseases.





Similar content being viewed by others
References
International Diabetes Federation (IDF), Diabetes Atlas. 7th edn. Canada, (2015). www.diabetesatlas.org
J.C. Pickup, M.B. Mattock, G.D. Chusney, D. Burt, NIDDM as a disease of the innate immune systemassociation of acute-phase reactants and interleukin-6 with metabolicsyndromeX. Diabetologia 40, 1286–1292 (1997)
M. Rodriguez-Moran, F. Guerrero-Romero, Increased levels of C-reactive protein in noncontrolled type II diabetic subjects. J. Diabetes Complicat. 13(4), 211–215 (1999)
P.D. Cani, R. Bibiloni, C. Knauf, A. Waget, A.M. Neyrinck, N.M. Delzenne, R. Burcelin, Changes in gut microbiota control metabolic endotoxemia-induced inflammation in high-fat diet-induced obesity and diabetes in mice. Diabetes 57, 1470–1481 (2008)
A.D. Pradhan, J.E. Manson, N. Rifai, J.E. Buring, P.M. Ridker, C-reactive protein, interleukin 6, and riskof developing type 2 diabetes mellitus. JAMA 286, 327–334 (2001)
A. Chawla, K.D. Nguyen, Y.P. Goh, Macrophage-mediated inflammation in metabolic disease. Nat. Rev. Immunol. 11(11), 738–749 (2011)
G.S. Hotamisligil, Inflammation, metaflammation and immunometabolic disorders. Nature 542(7640), 177–185 (2017)
S.L. Ameres, P.D. Zamore, Diversifying microRNA sequence and function. Nat. Rev. Mol. Cell Biol. 14(8), 475–488 (2013)
Y. Cheng, X. Liu, J. Yang, Y. Lin, D.Z. Xu, Q. Lu, E.A. Deitch, Y. Huo, E.S. Delphin, C. Zhang, MicroRNA-145, a novel smooth muscle cell phenotypic marker and modulator, controls vascular neointimal lesion formation. Circ. Res. 105(2), 158–166 (2009)
S. Albinsson, W.C. Sessa, Can microRNAs control vascular smooth muscle phenotypic modulation and the response to injury? Physiol. Genom. 43(10), 529–533 (2011)
F. Sala, J.F. Aranda, N. Rotllan, C.M. Ramirez, B. Aryal, L. Elia, G. Condorelli, A.L. Catapano, C. Fernandez-Hernando, G.D. Norata, MiR-143/145 deficiency attenuates the progression of atherosclerosis in Ldlr-/-mice. Thromb. Haemost. 112(4), 796–802 (2014)
M. Boufraqech, L. Zhang, M. Jain, D. Patel, R. Ellis, Y. Xiong, M. He, N. Nilubol, M.J. Merino, E. Kebebew, miR-145 suppresses thyroid cancer growth and metastasis and targets AKT3. Endocr. Relat. Cancer 21(4), 517–531 (2014)
G. Eades, B. Wolfson, Y. Zhang, Q. Li, Y. Yao, Q. Zhou, lincRNA-RoR and miR-145 regulate invasion in triple-negative breast cancer via targeting ARF6. Mol. Cancer Res. 13(2), 330–338 (2015)
S. Li, X. Wu, Y. Xu, S. Wu, Z. Li, R. Chen, N. Huang, Z. Zhu, X. Xu, miR-145 suppresses colorectal cancer cell migration and invasion by targeting an ETS-related gene. Oncol. Rep. 36(4), 1917–1926 (2016)
Y. Teng, R. Zhang, C. Liu, L. Zhou, H. Wang, W. Zhuang, Y. Huang, Z. Hong, miR-143 inhibits interleukin-13-induced inflammatory cytokine and mucus production in nasal epithelial cells from allergic rhinitis patients by targeting IL13Ralpha1. Biochem. Biophys. Res. Commun. 457(1), 58–64 (2015)
F. Lovren, Y. Pan, A. Quan, K.K. Singh, P.C. Shukla, N. Gupta, B.M. Steer, A.J. Ingram, M. Gupta, M. Al-Omran, H. Teoh, P.A. Marsden, S. Verma, MicroRNA-145 targeted therapy reduces atherosclerosis. Circulation 126(11Suppl 1), S81–S90 (2012)
M. Yuan, L. Zhang, F. You, J. Zhou, Y. Ma, F. Yang, L. Tao, MiR-145-5p regulates hypoxia-induced inflammatory response and apoptosis in cardiomyocytes by targeting CD40. Mol. Cell Biochem. 431(1-2), 123–131 (2017)
Y. Zhang, Q. Lin, MicroRNA-145 inhibits migration and invasion by down-regulating FSCN1 in lung cancer. Int. J. Clin. Exp. Med 8(6), 8794–8802 (2015)
S. Lorente-Cebrian, N. Mejhert, A. Kulyte, J. Laurencikiene, G. Astrom, P. Heden, M. Ryden, P. Arner, MicroRNAs regulate human adipocyte lipolysis: effects of miR-145 are linked to TNF-alpha. PLoS One 9(1), e86800 (2014)
F. Wen, Y. Yang, D. Jin, J. Sun, X. Yu, Z. Yang, MiRNA-145 is involved in the development of resistin-induced insulin resistance in HepG2 cells. Biochem. Biophys. Res. Commun. 445(2), 517–523 (2014)
Y. Egami, M. Fujii, K. Kawai, Y. Ishikawa, M. Fukuda, N. Araki, Activation-inactivation cycling of Rab35 and ARF6 is required for phagocytosis of zymosan in RAW264 macrophages. J. Immunol. Res 2015, 429439 (2015)
T. Hongu, Y. Kanaho, Activation machinery of the small GTPase Arf6. Adv. Biol. Regul. 54, 59–66 (2014)
J.C. Kagan, R. Medzhitov, Phosphoinositide-mediated adaptor recruitment controls Toll-like receptor signaling. Cell 125(5), 943–955 (2006)
T. Van Acker, S. Eyckerman, L. Vande Walle, S. Gerlo, M. Goethals, M. Lamkanfi, C. Bovijn, J. Tavernier, F. Peelman, The small GTPase Arf6 is essential for the Tram/Trif pathway in TLR4 signaling. J. Biol. Chem. 289(3), 1364–1376 (2014)
P.D. Cani, J. Amar, M.A. Iglesias, M. Poggi, C. Knauf, D. Bastelica, A.M. Neyrinck, R. Burelin, Metabolic Endotoxemia Initiates Obesity and Insulin Resistance. Diabetes 56(7), 1761–1772 (2007)
A. Muniategui, J. Pey, F.J. Planes, A. Rubio, Joint analysis of miRNA and mRNA expression data. Brief. Bioinform. 14(3), 263–278 (2013)
G.S. Hotamisligil, Inflammation and metabolic disorders. Nature 444(7121), 860–867 (2006)
J.C. McNelis, J.M. Olefsky, Macrophages, immunity, and metabolic disease. Immunity 41(1), 36–48 (2014)
J. Sloan-Lancaster, E. Abu-Raddad, J. Polzer, J.W. Miller, J.C. Scherer, A. De Gaetano, J.K. Berg, W.H. Landschulz, Double-blind, randomized study evaluating the glycemic and anti-inflammatory effects of subcutaneous LY2189102, a neutralizing IL-1beta antibody, in patients with type 2 diabetes. Diabetes Care 36(8), 2239–2246 (2013)
P.C. van Poppel, E.J. van Asseldonk, J.J. Holst, T. Vilsboll, M.G. Netea, C.J. Tack, The interleukin-1 receptor antagonist anakinra improves first-phase insulin secretion and insulinogenic index in subjects with impaired glucose tolerance. Diabetes Obes. Metab. 16(12), 1269–1273 (2014)
I. Stagakis, G. Bertsias, S. Karvounaris, M. Kavousanaki, D. Virla, A. Raptopoulou, D. Kardassis, D.T. Boumpas, P.I. Sidiropoulos, Anti-tumor necrosis factor therapy improves insulin resistance, beta cell function and insulin signaling in active rheumatoid arthritis patients with high insulin resistance. Arthritis Res. Ther. 14(3), R141 (2012)
T.L. Stanley, M.V. Zanni, S. Johnsen, S. Rasheed, H. Makimura, H. Lee, V.K. Khor, R.S. Ahima, S.K. Grinspoon, TNF-alpha antagonism with etanercept decreases glucose and increases the proportion of high molecular weight adiponectin in obese subjects with features of the metabolic syndrome. J. Clin. Endocrinol. Metab. 96(1), E146–E150 (2011)
J.C. Davies, S. Tamaddon-Jahromi, R. Jannoo, V. Kanamarlapudi, Cytohesin 2/ARF6 regulates preadipocyte migration through the activation of ERK1/2. Biochem. Pharmacol. 92(4), 651–660 (2014)
T. Torii, Y. Miyamoto, A. Sanbe, K. Nishimura, J. Yamauchi, A. Tanoue, Cytohesin-2/ARNO, through its interaction with focal adhesion adaptor protein paxillin, regulates preadipocyte migration via the downstream activation of Arf6. J. Biol. Chem. 285(31), 24270–24281 (2010)
J.C. Davies, S.C. Bain, V. Kanamarlapudi, ADP-ribosylation factor 6 regulates endothelin-1-induced lipolysis in adipocytes. Biochem. Pharmacol. 90(4), 406–413 (2014)
Y. Liu, D. Zhou, N.A. Abumrad, X. Su, ADP-ribosylation factor 6 modulates adrenergic stimulated lipolysis in adipocytes. Am. J. Physiol. Cell Physiol. 298(4), C921–C928 (2010)
J. Li, A.W. Malaby, M. Famulok, H. Sabe, D.G. Lambright, V.W. Hsu, Grp1 plays a key role in linking insulin signaling to glut4 recycling. Dev. Cell 22(6), 1286–1298 (2012)
J. Li, P.J. Peters, M. Bai, J. Dai, E. Bos, T. Kirchhausen, K.V. Kandror, V.W. Hsu, An ACAP1-containing clathrin coat complex for endocytic recycling. J. Cell Biol. 178(3), 453–464 (2007)
Acknowledgements
This research was supported by the National Natural Science Foundation of China (No.81471057,81270902).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Li, R., Shen, Q., Wu, N. et al. MiR-145 improves macrophage-mediated inflammation through targeting Arf6. Endocrine 60, 73–82 (2018). https://doi.org/10.1007/s12020-018-1521-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-018-1521-8