Abstract
Purpose
Obesity and its metabolic impairments are discussed as major risk factors for sarcopenia leading to sarcopenic obesity. Cushing’s syndrome is known to be associated with obesity and muscle atrophy. We compared Cushing’s syndrome with matched obese controls regarding body composition, physical performance, and biochemical markers to test the hypothesis that Cushing’s syndrome could be a model for sarcopenic obesity.
Methods
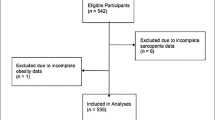
By propensity score matching, 47 controls were selected by body mass index and gender as obese controls. Fat mass and muscle mass were measured by bioelectrical impedance analysis. Muscle function was assessed by chair rising test and hand grip strength. Biochemical markers of glucose and lipid metabolism and inflammation (hsCRP) were measured in peripheral blood.
Results
Muscle mass did not differ between Cushing’s syndrome and obese controls. However, Cushing’s syndrome patients showed significantly greater chair rising time (9.5 s vs. 7.3 s, p = 0.008) and significantly lower hand grip strength (32.1 kg vs. 36.8 kg, p = 0.003). Cushing’s syndrome patients with impaired fasting glucose have shown the highest limitations in hand grip strength and chair rising time.
Conclusions
Similar to published data in ageing medicine, Cushing’s syndrome patients show loss of muscle function that cannot be explained by loss of muscle mass. Impaired muscle quality due to fat infiltration may be the reason. This is supported by the observation that Cushing’s syndrome patients with impaired glucose metabolism show strongest deterioration of muscle function. Research in sarcopenic obesity in elderly is hampered by confounding comorbidities and polypharmacy. As Cushing’s syndrome patients are frequently free of comorbidities and as Cushing’s syndrome is potentially curable we suggest Cushing’s syndrome as a clinical model for further research in sarcopenic obesity.

Similar content being viewed by others
References
D.R. Thomas, Sarcopenia. Clin. Geriatr. Med. 26, 331–46 (2010). doi:10.1016/j.cger.2010.02.012
F. Landi, R. Liperoti, D. Fusco et al., Sarcopenia and mortality among older nursing home residents. J. Am. Med. Dir. Assoc. 13, 121–126 (2012). doi:10.1016/j.jamda.2011.07.004
C. Beaudart, M. Zaaria, F. Pasleau et al., Health outcomes of sarcopenia: a systematic review and meta-analysis. PLoS ONE 12, e0169548 (2017). doi:10.1371/journal.pone.0169548
K. Kohara, Sarcopenic obesity in aging population: current status and future directions for research. Endocrine 45, 15–25 (2014). doi:10.1007/s12020-013-9992-0
T.S. Han, E. Correa, M.E.J. Lean et al., Changes in prevalence of obesity and high waist circumference over four years across European regions: the European male ageing study (EMAS). Endocrine 55, 456–469 (2017). doi:10.1007/s12020-016-1135-y
Y. Rolland, V. Lauwers-Cances, C. Cristini et al., Difficulties with physical function associated with obesity, sarcopenia, and sarcopenic-obesity in community-dwelling elderly women: the EPIDOS (EPIDemiologie de l’OSteoporose) study. Am. J. Clin. Nutr. 89, 1895–900 (2009). doi:10.3945/ajcn.2008.26950
P.M. Peeke, G.P. Chrousos, PDFlib PLOP: PDF linearization, optimization, protection page inserted by evaluation version hypercortisolism and obesity. Ann. N. Y. Acad. Sci. 771, 665–676 (1995)
T.C. Friedman, G. Mastorakos, T.D. Newman et al., Carbohydrate and lipid metabolism in endogenous hypercortisolism: shared features with metabolic syndrome X and NIDDM. Endocr. J. 43, 645–55 (1996). doi:10.1507/endocrj.43.645
C. Tsigos, C. Stefanaki, G.I. Lambrou et al., Stress and inflammatory biomarkers and symptoms are associated with bioimpedance measures. Eur. J. Clin. Invest. 45, 126–34 (2015). doi:10.1111/eci.12388
C. Stefanaki, M. Peppa, D. Boschiero, G.P. Chrousos, Healthy overweight/obese youth: early osteosarcopenic obesity features. Eur. J. Clin. Invest. 46, 767–78 (2016). doi:10.1111/eci.12659
A.D. Pradhan, J.E. Manson, N. Rifai et al., C-reactive protein, interleukin 6, and risk of developing type 2 diabetes mellitus. JAMA 286, 327–334 (2001)
C.M. Berr, M.R. Stieg, T. Deutschbein et al., Persistence of myopathy in Cushing’s syndrome: evaluation of the German cushing’s registry. Eur. J. Endocrinol. 176, 737–746 (2017). doi:10.1530/EJE-16-0689
A. Oßwald, E. Plomer, C. Dimopoulou et al., Favorable long-term outcomes of bilateral adrenalectomy in Cushing’s disease. Eur. J. Endocrinol. 171, 209–215 (2014). doi:10.1530/EJE-14-0214
G. Arnaldi, A. Angeli, A.B. Atkinson et al., Diagnosis and complications of Cushing’s syndrome: a consensus statement. J. Clin. Endocrinol. Metab. 88, 5593–5602 (2003). doi:10.1210/jc.2003-030871
L.K. Nieman, B.M.K. Biller, J.W. Findling et al., The diagnosis of cushing’s syndrome: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 93, 1526–1540 (2008). doi:10.1210/jc.2008-0125
I. Janssen, S.B. Heymsfield, R.N. Baumgartner, R. Ross, Estimation of skeletal muscle mass by bioelectrical impedance analysis. J. Appl. Physiol. 89, 465–471 (2000)
R. Kob, L.C. Bollheimer, T. Bertsch et al., Sarcopenic obesity: molecular clues to a better understanding of its pathogenesis? Biogerontology 16, 15–29 (2015). doi:10.1007/s10522-014-9539-7
J.Z. Ilich, O.J. Kelly, J.E. Inglis et al., Interrelationship among muscle, fat, and bone: connecting the dots on cellular, hormonal, and whole body levels. Ageing Res. Rev. 15, 51–60 (2014). doi:10.1016/j.arr.2014.02.007
M. Cesari, Y. Rolland, G. Abellan Van Kan et al., Sarcopenia-related parameters and incident disability in older persons: results from the “invecchiare in Chianti” study. J. Gerontol. A Biol. Sci. Med. Sci. 70, 457–463 (2015). doi:10.1093/gerona/glu181
P.M. Cawthon, K.M. Fox, S.R. Gandra et al., Clustering of strength, physical function, muscle, and adiposity characteristics and risk of disability in older adults. J. Am. Geriatr. Soc. 59, 781–787 (2011). doi:10.1111/j.1532-5415.2011.03389.x
A.W. Frank-Wilson, J.P.Farthing, P.D.Chilibeck et al., Lower leg muscle density is independently associated with fall status in community-dwelling older adults. Osteoporos Int. 27(7), 2231–2240 (2016). doi:10.1007/s00198-016-3514-x
B.K. Koo, E. Roh, Y.S. Yang, M.K. Moon, Difference between old and young adults in contribution of β-cell function and sarcopenia in developing diabetes mellitus. J. Diabetes Investig. 7, 233–240 (2016). doi:10.1111/jdi.12392
D.J. Cuthbertson, J.A. Bell, S.Y. Ng, et al. Dynapenic obesity and the risk of incident type 2 diabetes: the English longitudinal study of ageing. Diabet Med. 33(8), 1052–1059 (2016). doi: 10.1111/dme.12991
E. Poggiogalle, S. Migliaccio, A. Lenzi, L.M. Donini, Treatment of body composition changes in obese and overweight older adults: insight into the phenotype of sarcopenic obesity. Endocrine 47, 699–716 (2014). doi:10.1007/s12020-014-0315-x
Acknowledgements
The authors want to thank the volunteer participants and John Hoppe for providing language help.
Funding
This work is part of the German Cushing registry CUSTODES and has been supported by grants from the Else Kröner-Fresenius Stiftung to MR (2012 A103 and 2015 A228).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Drey, M., Berr, C.M., Reincke, M. et al. Cushing’s syndrome: a model for sarcopenic obesity. Endocrine 57, 481–485 (2017). https://doi.org/10.1007/s12020-017-1370-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-017-1370-x