Abstract
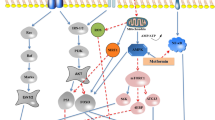
Osteoporosis (OP) is a common age-related disease. OP is mainly a decrease in bone density and mass caused by the destruction of bone microstructure, which leads to an increase in bone fragility. SIRT3 is a mitochondrial deacetylase that plays critical roles in mitochondrial homeostasis, metabolic regulation, gene transcription, stress response, and gene stability. Studies have shown that the higher expression levels of SIRT3 are associated with decreased levels of oxidative stress in the body and may play important roles in the prevention of age-related diseases. SIRTs can enhance the osteogenic potential and osteoblastic activity of bone marrow mesenchymal stromal cells not only by enhancing PGC-1α, FOXO3, SOD2, and oxidative phosphorylation, but also by anti-aging and reducing mitochondrial autophagy. SIRT3 is able to upregulate antioxidant enzymes to exert an inhibitory effect on osteoclasts, however, it has been shown that the inflammatory cascade response can in turn increase SIRT3 and inhibit osteoclast differentiation through the AMPK-PGC-1β pathway. SIRT3 plays an important role in different types of osteoporosis by affecting osteoblasts, osteoclasts, and bone marrow mesenchymal cells. In this review, we discuss the classification and physiological functions of SIRTs, the effects of SIRT3 on OCs osteoblasts, and BMSCs, and the roles and mechanisms of SIRT3 in different types of OP, such as diabetic OP, glucocorticoid-induced OP, postmenopausal OP, and senile OP.


Similar content being viewed by others
References
Słupski, W., Jawień, P., & Nowak, B. (2021). Botanicals in postmenopausal osteoporosis. Nutrients, 13(5), 1609. https://doi.org/10.3390/nu13051609.
Johnston, C. B., & Dagar, M. (2020). Osteoporosis in older adults. The Medical Clinics of North America, 104(5), 873–884. https://doi.org/10.1016/j.mcna.2020.06.004.
He, J., Xu, S., Zhang, B., Xiao, C., Chen, Z., Si, F., Fu, J., Lin, X., Zheng, G., Yu, G., & Chen, J. (2020). Gut microbiota and metabolite alterations associated with reduced bone mineral density or bone metabolic indexes in postmenopausal osteoporosis. Aging, 12(9), 8583–8604. https://doi.org/10.18632/aging.103168.
Noh, J. Y., Yang, Y., & Jung, H. (2020). Molecular mechanisms and emerging therapeutics for osteoporosis. International Journal of Molecular Sciences, 21(20), 7623. https://doi.org/10.3390/ijms21207623.
Anam, A. K., & Insogna, K. (2021). Update on osteoporosis screening and management. The Medical Clinics of North America, 105(6), 1117–1134. https://doi.org/10.1016/j.mcna.2021.05.016.
Sun, K., Jing, X., Guo, J., Yao, X., & Guo, F. (2021). Mitophagy in degenerative joint diseases. Autophagy, 17(9), 2082–2092. https://doi.org/10.1080/15548627.2020.1822097.
Singh, C. K., Chhabra, G., Ndiaye, M. A., Garcia-Peterson, L. M., Mack, N. J., & Ahmad, N. (2018). The role of sirtuins in antioxidant and redox signaling. Antioxidants & Redox Signaling, 28(8), 643–661. https://doi.org/10.1089/ars.2017.7290.
Jin, W., Li, C., Yang, S., Song, S., Hou, W., Song, Y., & Du, Q. (2023). Hypolipidemic effect and molecular mechanism of ginsenosides: A review based on oxidative stress. Frontiers in Pharmacology, 14, 1166898. https://doi.org/10.3389/fphar.2023.1166898.
Golob, A. L., & Laya, M. B. (2015). Osteoporosis: Screening, prevention, and management. The Medical Clinics of North America, 99(3), 587–606. https://doi.org/10.1016/j.mcna.2015.01.010.
Awasthi, H., Mani, D., Singh, D., & Gupta, A. (2018). The underlying pathophysiology and therapeutic approaches for osteoporosis. Medicinal Research Reviews, 38(6), 2024–2057. https://doi.org/10.1002/med.21504.
Arceo-Mendoza, R. M., & Camacho, P. M. (2021). Postmenopausal osteoporosis: Latest guidelines. Endocrinology and Metabolism Clinics of North America, 50(2), 167–178. https://doi.org/10.1016/j.ecl.2021.03.009.
Li, J., Chen, X., Lu, L., & Yu, X. (2020). The relationship between bone marrow adipose tissue and bone metabolism in postmenopausal osteoporosis. Cytokine & Growth Factor Reviews, 52, 88–98. https://doi.org/10.1016/j.cytogfr.2020.02.003.
Cheng, C. H., Chen, L. R., & Chen, K. H. (2022). Osteoporosis due to hormone imbalance: An overview of the effects of estrogen deficiency and glucocorticoid overuse on bone turnover. International Journal of Molecular Sciences, 23(3), 1376. https://doi.org/10.3390/ijms23031376.
Manolagas, S. C. (2010). From estrogen-centric to aging and oxidative stress: A revised perspective of the pathogenesis of osteoporosis. Endocrine Reviews, 31(3), 266–300. https://doi.org/10.1210/er.2009-0024.
Li, Y., Wu, Q., Wang, Y., Li, L., Bu, H., & Bao, J. (2017). Senescence of mesenchymal stem cells (review). International Journal of Molecular Medicine, 39(4), 775–782. https://doi.org/10.3892/ijmm.2017.2912.
Zou, Z., Liu, W., Cao, L., Liu, Y., He, T., Peng, S., & Shuai, C. (2020). Advances in the occurrence and biotherapy of osteoporosis. Biochemical Society Transactions, 48(4), 1623–1636. https://doi.org/10.1042/BST20200005.
Herath, M., Langdahl, B., Ebeling, P. R., & Milat, F. (2022). Challenges in the diagnosis and management of glucocorticoid-induced osteoporosis in younger and older adults. Clinical Endocrinology, 96(4), 460–474. https://doi.org/10.1111/cen.14637.
Honaker, K., Tanabe, M., Kawate, H., Nawata, H., & Takayanagi, R. (2005). Glucocorticoid suppresses the canonical Wnt signal in cultured human osteoblasts. Biochemical and Biophysical Research Communications, 329(1), 177–181. https://doi.org/10.1016/j.bbrc.2005.01.117.
Cipriani, C., Colangelo, L., Santori, R., Renella, M., Mastrantonio, M., Minisola, S., & Pepe, J. (2020). The interplay between bone and glucose metabolism. Frontiers in Endocrinology, 11, 122. https://doi.org/10.3389/fendo.2020.00122.
Tanaka, K., Yamaguchi, T., Kanazawa, I., & Sugimoto, T. (2015). Effects of high glucose and advanced glycation end products on the expressions of sclerostin and RANKL as well as apoptosis in osteocyte-like MLO-Y4-A2 cells. Biochemical and Biophysical Research Communications, 461(2), 193–199. https://doi.org/10.1016/j.bbrc.2015.02.091.
Yi, S. J., & Kim, K. (2020). New insights into the role of histone changes in aging. International Journal of Molecular Sciences, 21(21), 8241. https://doi.org/10.3390/ijms21218241.
García-Giménez, J. L., Garcés, C., Romá-Mateo, C., & Pallardó, F. V. (2021). Oxidative stress-mediated alterations in histone post-translational modifications. Free Radical Biology & Medicine, 170, 6–18. https://doi.org/10.1016/j.freeradbiomed.2021.02.027.
Zhang, T., Cooper, S., & Brockdorff, N. (2015). The interplay of histone modifications—writers that read. EMBO Reports, 16(11), 1467–1481. https://doi.org/10.15252/embr.201540945.
Shen, Y., Wei, W., & Zhou, D. X. (2015). Histone acetylation enzymes coordinate metabolism and gene expression. Trends in Plant Science, 20(10), 614–621. https://doi.org/10.1016/j.tplants.2015.07.005.
Yang, K., Pei, L., Zhou, S., Tao, L., & Zhu, Y. (2021). Metformin attenuates H2O2-induced osteoblast apoptosis by regulating SIRT3 via the PI3K/AKT pathway. Experimental and Therapeutic Medicine, 22(5), 1316. https://doi.org/10.3892/etm.2021.10751.
Diao, Z., Ji, Q., & Wu, Z., et al. (2021). SIRT3 consolidates heterochromatin and counteracts senescence. Nucleic Acids Research, 49(8), 4203–4219. https://doi.org/10.1093/nar/gkab161.
Kim, H. S., Patel, K., & Muldoon-Jacobs, K., et al. (2010). SIRT3 is a mitochondria-localized tumor suppressor required for maintenance of mitochondrial integrity and metabolism during stress. Cancer Cell, 17(1), 41–52. https://doi.org/10.1016/j.ccr.2009.11.023.
Zhang, J., Xiang, H., Liu, J., Chen, Y., He, R. R., & Liu, B. (2020). Mitochondrial sirtuin 3: New emerging biological function and therapeutic target. Theranostics, 10(18), 8315–8342. https://doi.org/10.7150/thno.45922.
Cheng, Y., Ren, X., & Gowda, A. S., et al. (2013). Interaction of Sirt3 with OGG1 contributes to repair of mitochondrial DNA and protects from apoptotic cell death under oxidative stress. Cell Death & Disease, 4(7), e731. https://doi.org/10.1038/cddis.2013.254.
Liu, J., Li, D., Zhang, T., Tong, Q., Ye, R. D., & Lin, L. (2017). SIRT3 protects hepatocytes from oxidative injury by enhancing ROS scavenging and mitochondrial integrity. Cell Death & Disease, 8(10), e3158. https://doi.org/10.1038/cddis.2017.564.
Gao, J. M., Li, R., Zhang, L., Jia, L. L., Ying, X. X., Dou, D. Q., Li, J. C., & Li, H. B. (2013). Cuscuta chinensis seeds water extraction protecting murine osteoblastic MC3T3-E1 cells against tertiary butyl hydroperoxide induced injury. Journal of Ethnopharmacology, 148(2), 587–595. https://doi.org/10.1016/j.jep.2013.05.005.
Guo, Y., Jia, X., Cui, Y., Song, Y., Wang, S., Geng, Y., Li, R., Gao, W., & Fu, D. (2021). Sirt3-mediated mitophagy regulates AGEs-induced BMSCs senescence and senile osteoporosis. Redox Biology, 41, 101915. https://doi.org/10.1016/j.redox.2021.101915.
Kim, T. S., Jin, Y. B., & Kim, Y. S., et al. (2019). SIRT3 promotes antimycobacterial defenses by coordinating mitochondrial and autophagic functions. Autophagy, 15(8), 1356–1375. https://doi.org/10.1080/15548627.2019.1582743.
Li, R., Xin, T., Li, D., Wang, C., Zhu, H., & Zhou, H. (2018). Therapeutic effect of sirtuin 3 on ameliorating nonalcoholic fatty liver disease: The role of the ERK-CREB pathway and Bnip3-mediated mitophagy. Redox Biology, 18, 229–243. https://doi.org/10.1016/j.redox.2018.07.011.
Wang, T., Zhang, F., Peng, W., Wang, L., Zhang, J., Dong, W., Tian, X., Ye, C., Li, Y., & Gong, Y. (2022). Overexpression of NMNAT3 improves mitochondrial function and enhances antioxidative stress capacity of bone marrow mesenchymal stem cells via the NAD+-Sirt3 pathway. Bioscience Reports, 42(1), BSR20211005. https://doi.org/10.1042/BSR20211005.
Bugga, P., Alam, M. J., Kumar, R., Pal, S., Chattopadyay, N., & Banerjee, S. K. (2022). Sirt3 ameliorates mitochondrial dysfunction and oxidative stress through regulating mitochondrial biogenesis and dynamics in cardiomyoblast. Cellular Signalling, 94, 110309. https://doi.org/10.1016/j.cellsig.2022.110309.
Giralt, A., & Villarroya, F. (2012). SIRT3, a pivotal actor in mitochondrial functions: Metabolism, cell death and aging. The Biochemical Journal, 444(1), 1–10. https://doi.org/10.1042/BJ20120030.
Ding, Y., Yang, H., Wang, Y., Chen, J., Ji, Z., & Sun, H. (2017). Sirtuin 3 is required for osteogenic differentiation through maintenance of PGC-1ɑ-SOD2-mediated regulation of mitochondrial function. International Journal of Biological Sciences, 13(2), 254–264. https://doi.org/10.7150/ijbs.17053.
Wang, F. S., Wu, R. W., Chen, Y. S., Ko, J. Y., Jahr, H., & Lian, W. S. (2021). Biophysical modulation of the mitochondrial metabolism and redox in bone homeostasis and osteoporosis: How biophysics converts into bioenergetics. Antioxidants, 10(9), 1394. https://doi.org/10.3390/antiox10091394.
Gao, J., Feng, Z., & Wang, X., et al. (2018). SIRT3/SOD2 maintains osteoblast differentiation and bone formation by regulating mitochondrial stress. Cell Death and Differentiation, 25(2), 229–240. https://doi.org/10.1038/cdd.2017.144.
Zheng, K., Bai, J., & Li, N., et al. (2021). Protective effects of sirtuin 3 on titanium particle-induced osteogenic inhibition by regulating the NLRP3 inflammasome via the GSK-3β/β-catenin signalling pathway. Bioactive Materials, 6(10), 3343–3357. https://doi.org/10.1016/j.bioactmat.2021.02.039.
Zhou, W., Liu, Y., & Shen, J., et al. (2019). Melatonin increases bone mass around the prostheses of OVX rats by ameliorating mitochondrial oxidative stress via the SIRT3/SOD2 signaling pathway. Oxidative Medicine and Cellular Longevity, 2019, 4019619. https://doi.org/10.1155/2019/4019619.
Xiao, L., Lin, J., Chen, R., Huang, Y., Liu, Y., Bai, J., Ge, G., Shi, X., Chen, Y., Shi, J., Aiqing, L., Yang, H., Geng, D., & Wang, Z. (2020). Sustained release of melatonin from GelMA liposomes reduced osteoblast apoptosis and improved implant osseointegration in osteoporosis. Oxidative Medicine and Cellular Longevity, 2020, 6797154. https://doi.org/10.1155/2020/6797154.
Li, Y., Yu, C., Shen, G., Li, G., Shen, J., Xu, Y., & Gong, J. (2015). Sirt3-MnSOD axis represses nicotine-induced mitochondrial oxidative stress and mtDNA damage in osteoblasts. Acta Biochimica et Biophysica Sinica, 47(4), 306–312. https://doi.org/10.1093/abbs/gmv013.
Wang, S., Yang, J., Lin, T., Huang, S., Ma, J., & Xu, X. (2020). Excessive production of mitochondrion‑derived reactive oxygen species induced by titanium ions leads to autophagic cell death of osteoblasts via the SIRT3/SOD2 pathway. Molecular Medicine Reports, 22(1), 257–264. https://doi.org/10.3892/mmr.2020.11094.
Kim, H., Lee, Y. D., Kim, H. J., Lee, Z. H., & Kim, H. H. (2017). SOD2 and Sirt3 control osteoclastogenesis by regulating mitochondrial ROS. Journal of Bone and Mineral Research, 32(2), 397–406. https://doi.org/10.1002/jbmr.2974.
Ling, W., Krager, K., Richardson, K. K., Warren, A. D., Ponte, F., Aykin-Burns, N., Manolagas, S. C., Almeida, M., & Kim, H. N. (2021). Mitochondrial Sirt3 contributes to the bone loss caused by aging or estrogen deficiency. JCI Insight, 6(10), e146728. https://doi.org/10.1172/jci.insight.146728.
Li, Q., Wang, H., Zhang, J., Kong, A. P., Li, G., Lam, T. P., Cheng, J. C., & Lee, W. Y. (2021). Deletion of SIRT3 inhibits osteoclastogenesis and alleviates aging or estrogen deficiency-induced bone loss in female mice. Bone, 144, 115827. https://doi.org/10.1016/j.bone.2020.115827.
Ho, L., Wang, L., Roth, T. M., Pan, Y., Verdin, E. M., Hsiao, E. C., & Nissenson, R. A. (2017). Sirtuin-3 promotes adipogenesis, osteoclastogenesis, and bone loss in aging male mice. Endocrinology, 158(9), 2741–2753. https://doi.org/10.1210/en.2016-1739.
Li, N., Li, X., Zheng, K., Bai, J., Zhang, W., Sun, H., Ge, G., Wang, W., Wang, Z., Gu, Y., Xue, Y., Xu, Y., Geng, D., & Zhou, J. (2021). Inhibition of Sirtuin 3 prevents titanium particle-induced bone resorption and osteoclastsogenesis via suppressing ERK and JNK signaling. International Journal of Biological Sciences, 17(5), 1382–1394. https://doi.org/10.7150/ijbs.53992.
Richardson, K. K., Ling, W., Krager, K., Fu, Q., Byrum, S. D., Pathak, R., Aykin-Burns, N., & Kim, H. N. (2022). Ionizing radiation activates mitochondrial function in osteoclasts and causes bone loss in young adult male mice. International Journal of Molecular Sciences, 23(2), 675. https://doi.org/10.3390/ijms23020675.
Huh, J. E., Shin, J. H., Jang, E. S., Park, S. J., Park, D. R., Ko, R., Seo, D. H., Kim, H. S., Lee, S. H., Choi, Y., Kim, H. S., & Lee, S. Y. (2016). Sirtuin 3 (SIRT3) maintains bone homeostasis by regulating AMPK-PGC-1β axis in mice. Scientific Reports, 6, 22511. https://doi.org/10.1038/srep22511.
Hu, S., & Wang, S. (2022). The role of SIRT3 in the osteoporosis. Frontiers in Endocrinology, 13, 893678. https://doi.org/10.3389/fendo.2022.893678.
Mazzotti, E., Teti, G., Falconi, M., Chiarini, F., Barboni, B., Mazzotti, A., & Muttini, A. (2019). Age-related alterations affecting the chondrogenic differentiation of synovial fluid mesenchymal stromal cells in an equine model. Cells, 8(10), 1116. https://doi.org/10.3390/cells8101116.
Ballard, A., Zeng, R., Zarei, A., Shao, C., Cox, L., Yan, H., Franco, A., Dorn, 2nd, G. W., Facci, R., & Deborah, J. V. (2020). The tethering function of mitofusin2 controls osteoclast differentiation by modulating the Ca2+-NFATc1 axis. The Journal of Biological Chemistry, 295(19), 6629–6640. https://doi.org/10.1074/jbc.RA119.012023.
Walters, H. E., & Cox, L. S. (2018). mTORC inhibitors as broad-spectrum therapeutics for age-related diseases. International Journal of Molecular Sciences, 19(8), 2325. https://doi.org/10.3390/ijms19082325.
Minhas, P. S., Liu, L., & Moon, P. K., et al. (2019). Macrophage de novo NAD+ synthesis specifies immune function in aging and inflammation. Nature Immunology, 20(1), 50–63. https://doi.org/10.1038/s41590-018-0255-3.
Bordag, N., Klie, S., Jürchott, K., Vierheller, J., Schiewe, H., Albrecht, V., Tonn, J. C., Schwartz, C., Schichor, C., & Selbig, J. (2015). Glucocorticoid (dexamethasone)-induced metabolome changes in healthy males suggest prediction of response and side effects. Scientific Reports, 5, 15954. https://doi.org/10.1038/srep15954.
Wang, L., Li, Q., Yan, H., Jiao, G., Wang, H., Chi, H., Zhou, H., Chen, L., Shan, Y., & Chen, Y. (2020). Resveratrol protects osteoblasts against dexamethasone-induced cytotoxicity through activation of AMP-activated protein kinase. Drug Design, Development and Therapy, 14, 4451–4463. https://doi.org/10.2147/DDDT.S266502.
Chen, L., Wang, B. Z., Xie, J., Zhang, R. Y., Jin, C., Chen, W. K., Fang, K. H., Hong, C. X., Xu, T. H., Huang, C. B., Yang, L. & & Weng, S. J. (2021). Therapeutic effect of SIRT3 on glucocorticoid-induced osteonecrosis of the femoral head via intracellular oxidative suppression. Free Radical Biology & Medicine, 176, 228–240. https://doi.org/10.1016/j.freeradbiomed.2021.07.016.
Suwanjang, W., Sirisuwat, C., Srisung, S., Isarankura-Na-Ayudhya, C., Pannengpetch, S., & Prachayasittikul, S. (2022). Protective efficacy of Spilanthes acmella murr. extracts and bioactive constituents in neuronal cell death. Rejuvenation Research, 25(1), 2–15. https://doi.org/10.1089/rej.2021.0002.
Huang, X., Shu, H., Ren, C., & Zhu, J. (2022). SIRT3 improves bone regeneration and rescues diabetic fracture healing by regulating oxidative stress. Biochemical and Biophysical Research Communications, 604, 109–115. https://doi.org/10.1016/j.bbrc.2022.03.001.
Kitada, M., Ogura, Y., Monno, I., & Koya, D. (2019). Sirtuins and type 2 diabetes: Role in inflammation, oxidative stress, and mitochondrial function. Frontiers in Endocrinology, 10, 187. https://doi.org/10.3389/fendo.2019.00187.
An, Y., Zhang, H., Wang, C., Jiao, F., Xu, H., Wang, X., Luan, W., Ma, F., Ni, L., Tang, X., Liu, M., Guo, W., & Yu, L. (2019). Activation of ROS/MAPKs/NF-κB/NLRP3 and inhibition of efferocytosis in osteoclast-mediated diabetic osteoporosis. FASEB Journal, 33(11), 12515–12527. https://doi.org/10.1096/fj.201802805RR.
Chen, J., Zhang, Y., Gao, J., Li, T., Gan, X., & Yu, H. (2021). Sirtuin 3 deficiency exacerbates age-related periodontal disease. Journal of Periodontal Research, 56(6), 1163–1173. https://doi.org/10.1111/jre.12930.
Qadir, A., Liang, S., Wu, Z., Chen, Z., Hu, L., & Qian, A. (2020). Senile osteoporosis: The involvement of differentiation and senescence of bone marrow stromal cells. International Journal of Molecular Sciences, 21(1), 349. https://doi.org/10.3390/ijms21010349.
Cheng, Y. Z., Yang, S. L., Wang, J. Y., Ye, M., Zhuo, X. Y., Wang, L. T., Chen, H., Zhang, H., & Yang, L. (2018). Irbesartan attenuates advanced glycation end products-mediated damage in diabetes-associated osteoporosis through the AGEs/RAGE pathway. Life Sciences, 205, 184–192. https://doi.org/10.1016/j.lfs.2018.04.042.
Cao, L., Zhou, S., Qiu, X., & Qiu, S. (2022). Trehalose improves palmitic acid-induced apoptosis of osteoblasts by regulating SIRT3-medicated autophagy via the AMPK/mTOR/ULK1 pathway. FASEB Journal, 36(9), e22491. https://doi.org/10.1096/fj.202200608RR.
Li, H., Zhang, M., & Wang, Y., et al. (2022). Daidzein alleviates doxorubicin-induced heart failure via the SIRT3/FOXO3a signaling pathway. Food & Function, 13(18), 9576–9588. https://doi.org/10.1039/d2fo00772j.
Jin, Z. H., Wang, S. F., & Liao, W. (2020). Zoledronic acid accelerates osteogenesis of bone marrow mesenchymal stem cells by attenuating oxidative stress via the SIRT3/SOD2 pathway and thus alleviates osteoporosis. European Review for Medical and Pharmacological Sciences, 24(4), 2095–2101. https://doi.org/10.26355/eurrev_202002_20389.
Funding
This study was funded by National Natural Science Foundation of China (No. 81960155) and The First Hospital of Lanzhou University Fund (ldyyyn2020-01).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Binjing Pan wrote the main manuscript text and figures. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pan, B., Chen, C., Zhao, Y. et al. SIRT3: A Potential Target of Different Types of Osteoporosis. Cell Biochem Biophys (2024). https://doi.org/10.1007/s12013-024-01254-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12013-024-01254-4