Abstract
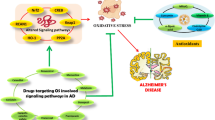
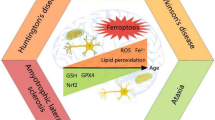
Neurodegeneration may be defined as a clinical condition wherein neurons gradually lose their structural integrity, viability, and functional abilities and the damage inflicted upon the neurons is often irreversible. The various mechanisms that have been observed to contribute to neurodegeneration include aggregation and accumulation of misfolded proteins, impaired autophagy, oxidative damage, neuroinflammation, mitochondrial defects, increased SUMOylation of proteins, impaired unfolded protein response (UPR) pathways, and disruption of axonal transport. Melatonin, a neurohormone, is involved in a variety of functions including scavenging free radicals, synchronizing the circadian rhythm, and mitigating immune response. Melatonin has shown to modulate the UPR pathway, antioxidant pathway through Nrf2 and inflammatory pathway through NFκB. The study aims to determine the efficacy of melatonin on neurodegeneration mediated by endoplasmic reticulum (ER) stress, inflammation, and oxidative damage through in silico approaches. The molecular targets chosen were ATF6, XBP1, PERK, Nrf2, and NFκB and they were docked against melatonin. Melatonin showed to have binding energy with ATF6 as − 4.8 kJ, with PERK as − 3.2 kJ, with XBP1 as − 4.8 kJ, with Nrf2 as − 4.5 kJ, and with that of NFκB as − 4.2 kJ, which implies it interacts well with them. Additionally various physiochemical analyses such as absorption, distribution, metabolism, excretion (ADME) were also carried out. Those analyses revealed that it has an optimal log P of about 1.98, optimal log S of − 2.34, is BBB permeant, has high GI absorption, is not a P-Gp substrate, has a TPSA of 54.12, has a molecular weight of 232.28, and has about 4 rotatable bonds. Also, it showed a bioactivity score of 0.06 for GPCR which implies that it is most likely to exert its function by binding GPCR. The findings imply that melatonin not only shows excellent interactions with the targets but also possesses drug-like physicochemical properties that makes it a valuable choice for the treatment of neurodegenerative disorders.





Similar content being viewed by others
Availability of Data and Material
Data will be available on request.
Code Availability
Not applicable.
References
Przedborski, S. (2008). Neurodegeneration. Neuroimmune. Pharmacology, 1918, 229–237. https://doi.org/10.1007/978-0-387-72573-4_17
World Health Organization. (2017). Global action plan on the public health response to dementia 2017 - 2025. Geneva: World Health Organization, 52. http://www.who.int/mental_health/neurology/dementia/action_plan_2017_2025/en/. Accessed 15 Sept 2021
Yacoubian, T. A. (2017). Neurodegenerative disorders: Why do we need new therapies? Alzheimer’s disease. Elsevier Inc. https://doi.org/10.1016/B978-0-12-802810-0.00001-5
Przedborski, S., Vila, M., & Jackson-Lewis, V. (2003). Neurodegeneration: What is it and where are we? Journal of Clinical Investigation, 111(1), 3–10. https://doi.org/10.1172/JCI200317522
Jellinger, K. A. (2010). Basic mechanisms of neurodegeneration: A critical update. Journal of Cellular and Molecular Medicine, 14(3), 457–487. https://doi.org/10.1111/j.1582-4934.2010.01010.x
Basha, F. H., Waseem, M., & Srinivasan, H. (2021). Cellular and molecular mechanism in neurodegeneration: Possible role of neuroprotectants. Cell Biochemistry and Function, 39(5), 613–622. https://doi.org/10.1002/cbf.3630
Alghamdi, B. S. (2018). The neuroprotective role of melatonin in neurological disorders. Journal of Neuroscience Research, 96(7), 1136–1149. https://doi.org/10.1002/jnr.24220
Fernández, A., Ordõñez, R., Reiter, R. J., González-Gallego, J., & Mauriz, J. L. (2015). Melatonin and endoplasmic reticulum stress: Relation to autophagy and apoptosis. Journal of Pineal Research, 59(3), 292–307. https://doi.org/10.1111/jpi.12264
Chen, D., Zhang, T., & Lee, T. H. (2020). Cellular mechanisms of melatonin: Insight from neurodegenerative diseases. Biomolecules, 10(8), 1–26. https://doi.org/10.3390/biom10081158
Rink, C., & Khanna, S. (2011). Significance of brain tissue oxygenation and the arachidonic acid cascade in stroke. Antioxidants and Redox Signaling, 14(10), 1889–1903. https://doi.org/10.1089/ars.2010.3474
Davinelli, S., Maes, M., Corbi, G., Zarrelli, A., Willcox, D. C., & Scapagnini, G. (2016). Dietary phytochemicals and neuro-inflammaging: From mechanistic insights to translational challenges. Immunity and Ageing, 13(1), 1–17. https://doi.org/10.1186/s12979-016-0070-3
Ahmadi, Z., & Ashrafizadeh, M. (2020). Melatonin as a potential modulator of Nrf2. Fundamental and Clinical Pharmacology, 34(1), 11–19. https://doi.org/10.1111/fcp.12498
Fan, C., Feng, J., Tang, C., Zhang, Z., Feng, Y., Duan, W., … Luo, E. (2020). Melatonin suppresses ER stress-dependent proapoptotic effects via AMPK in bone mesenchymal stem cells during mitochondrial oxidative damage. Stem Cell Research and Therapy, 11(1), 1–22https://doi.org/10.1186/s13287-020-01948-5
Marsh, A. P. (2019). Molecular mechanisms of proteinopathies across neurodegenerative disease: A review. Neurological Research and Practice, 1(1), 1–7. https://doi.org/10.1186/s42466-019-0039-8
Chauhan, N. B., & Mehla, J. (2015). Ameliorative effects of nutraceuticals in neurological disorders. Bioactive nutraceuticals and dietary supplements in neurological and brain disease: Prevention and therapy. Elsevier Inc. https://doi.org/10.1016/B978-0-12-411462-3.00027-8
Xiang, C., Wang, Y., Zhang, H., & Han, F. (2017). The role of endoplasmic reticulum stress in neurodegenerative disease. Apoptosis, 22(1), 1–26. https://doi.org/10.1007/s10495-016-1296-4
Lou, G., Palikaras, K., Lautrup, S., Scheibye-Knudsen, M., Tavernarakis, N., & Fang, E. F. (2020). Mitophagy and neuroprotection. Trends in Molecular Medicine, 26(1), 8–20. https://doi.org/10.1016/j.molmed.2019.07.002
Hetz, C., & Saxena, S. (2017). ER stress and the unfolded protein response in neurodegeneration. Nature Reviews Neurology, 13(8), 477–491. https://doi.org/10.1038/nrneurol.2017.99
Adams, C. J., Kopp, M. C., Larburu, N., Nowak, P. R., & Ali, M. M. U. (2019). Structure and molecular mechanism of ER stress signaling by the unfolded protein response signal activator IRE1. Frontiers in Molecular Biosciences, 6(MAR), 1–12. https://doi.org/10.3389/fmolb.2019.00011
Scheper, W., & Hoozemans, J. J. M. (2015). The unfolded protein response in neurodegenerative diseases: A neuropathological perspective. Acta Neuropathologica, 130(3), 315–331. https://doi.org/10.1007/s00401-015-1462-8
Yeganeh, B., Jäger, R., Gorman, A. M., Samali, A., & Ghavami, S. (2015). Induction of autophagy: Role of endoplasmic reticulum stress and unfolded protein response. Autophagy: Cancer, other pathologies, inflammation, immunity, infection, and aging, 7, 91–101. https://doi.org/10.1016/B978-0-12-801043-3.00005-4
Markouli, M., Strepkos, D., Papavassiliou, A. G., & Piperi, C. (2020). Targeting of endoplasmic reticulum (ER) stress in gliomas. Pharmacological Research, 157(March), 104823. https://doi.org/10.1016/j.phrs.2020.104823
da Silva, D. C., Valentão, P., Andrade, P. B., & Pereira, D. M. (2020). Endoplasmic reticulum stress signaling in cancer and neurodegenerative disorders: Tools and strategies to understand its complexity. Pharmacological Research, 155(February), 104702. https://doi.org/10.1016/j.phrs.2020.104702
Luo, F., Sandhu, A. F., Rungratanawanich, W., Williams, G. E., Akbar, M., Zhou, S., … Wang, X. (2020). Melatonin and autophagy in aging-related neurodegenerative diseases. International Journal of Molecular Sciences, 21(19), 1–31https://doi.org/10.3390/ijms21197174
Srinivasan, V., Pandi-Perumal, S. R., Maestroni, G. J. M., Esquifino, A. I., Hardeland, R., & Cardinali, D. P. (2005). Role of melatonin in neurodegenerative diseases. Neurotoxicity Research, 7(4), 293–318. https://doi.org/10.1007/BF03033887
Haze, K., Yoshida, H., Yanagi, H., Yura, T., & Mori, K. (1999). Mammalian transcription factor ATF6 is synthesized as a transmembrane protein and activated by proteolysis in response to endoplasmic reticulum stress. Molecular Biology of the Cell, 10(11), 3787–3799. https://doi.org/10.1091/mbc.10.11.3787
Wang, P., Li, J., Tao, J., & Sha, B. (2018). The luminal domain of the ER stress sensor protein PERK binds misfolded proteins and thereby triggers PERK oligomerization. Journal of Biological Chemistry, 293(11), 4110–4121. https://doi.org/10.1074/jbc.RA117.001294
Yoshida, H., Oku, M., Suzuki, M., & Mori, K. (2006). pXBP1(U) encoded in XBP1 pre-mRNA negatively regulates unfolded protein response activator pXBP1(S) in mammalian ER stress response. Journal of Cell Biology, 172(4), 565–575. https://doi.org/10.1083/jcb.200508145
Furukawa, M., & Xiong, Y. (2005). BTB protein Keap1 targets antioxidant transcription factor Nrf2 for ubiquitination by the Cullin 3-Roc1 ligase. Molecular and Cellular Biology, 25(1), 162–171. https://doi.org/10.1128/mcb.25.1.162-171.2005
Hansen, S. K., Nerlov, C., Zabel, U., Verde, P., Johnsen, M., Baeuerle, P. A., & Blasi, F. (1992). A novel complex between the p65 subunit of NF-κB and c-Rel binds to a DNA element involved in the phorbol ester induction of the human urokinase gene. EMBO Journal, 11(1), 205–213. https://doi.org/10.1002/j.1460-2075.1992.tb05043.x
Elkington, P., Tebruegge, M., Mansour, S., & Respiratory, S. (2017). Sciences, E., & Unit, A. Tuberculosis. An infection-initiated autoimmune disease ?, 37(12), 815–818. https://doi.org/10.1016/j.it.2016.09.007.Tuberculosis
Cockman, M. E., Lancaster, D. E., Stolze, I. P., Hewitson, K. S., McDonough, M. A., Coleman, M. L., … Ratcliffe, P. J. (2006). Posttranslational hydroxylation of ankyrin repeats in IκB proteins by the hypoxia-inducible factor (HIF) asparaginyl hydroxylase, factor inhibiting HIF (FIH). Proceedings of the National Academy of Sciences of the United States of America, 103(40), 14767–14772https://doi.org/10.1073/pnas.0606877103
Li, Z., Zhang, J., Chen, D., & Shu, H. B. (2003). Casper/c-FLIP is physically and functionally associated with NF-κB1 p105. Biochemical and Biophysical Research Communications, 309(4), 980–985. https://doi.org/10.1016/j.bbrc.2003.08.104
Liu, T., Zhang, L., Joo, D., & Sun, S. C. (2017). NF-κB signaling in inflammation. Signal Transduction and Targeted Therapy, 2(March). https://doi.org/10.1038/sigtrans.2017.23
Ahmed, S. M. U., Luo, L., Namani, A., Wang, X. J., & Tang, X. (2017). Nrf2 signaling pathway: Pivotal roles in inflammation. Biochimica et Biophysica Acta - Molecular Basis of Disease, 1863(2), 585–597. https://doi.org/10.1016/j.bbadis.2016.11.005
Sekar, A., Soundhararajan, R., & Srinivasan, H. (2021). In silico analysis of quercetin and its analogues against targeted proteins. Biointerface Research in Applied Chemistry, 11(5), 13695–13705. https://doi.org/10.33263/BRIAC115.1369513705
Meng, X. Y., Zhang, H. X., Mezei, M., & Cui, M. (2011). Molecular docking: A powerful approach for structure-based drug discovery. Current computer-aided drug design. Current Computer Aided Drug Design, 7(2), 146–157. Retrieved from https://www.ingentaconnect.com/content/ben/cad/2011/00000007/00000002/art00008%0Ahttps://www.ncbi.nlm.nih.gov/pmc/articles/PMC3624763/pdf/nihms412728.pdf
Lindholm, D., Wootz, H., & Korhonen, L. (2006). ER stress and neurodegenerative diseases. Cell Death and Differentiation, 13(3), 385–392. https://doi.org/10.1038/sj.cdd.4401778
Salentin, S., Schreiber, S., Haupt, V. J., Adasme, M. F., & Schroeder, M. (2015). PLIP: Fully automated protein-ligand interaction profiler. Nucleic Acids Research, 43(W1), W443–W447. https://doi.org/10.1093/nar/gkv315
Ã, C. A. L. (2004). Lead profiling lead- and drug-like compounds : The rule-of-five revolution, 337–341. https://doi.org/10.1016/j.ddtec.2004.11.007
Ditri, E. L. Z., & J. W. (2017). 乳鼠心肌提取 HHS Public Access. Physiology & behavior, 176(1), 139–148. https://doi.org/10.1016/j.addr.2016.05.007.BDDCS
Li, A. P. (2001). Screening for human ADME/Tox drug properties in drug discovery. Drug Discovery Today, 6(7), 357–366. https://doi.org/10.1016/S1359-6446(01)01712-3
Daina, A., Michielin, O., & Zoete, V. (2017). SwissADME: A free web tool to evaluate pharmacokinetics, drug-likeness and medicinal chemistry friendliness of small molecules. Scientific Reports, 7, 1–13. https://doi.org/10.1038/srep42717
Arnott, J. A., & Planey, S. L. (2012). The influence of lipophilicity in drug discovery and design. Expert Opinion on Drug Discovery, 7(10), 863–875. https://doi.org/10.1517/17460441.2012.714363
Savjani, K. T., Gajjar, A. K., & Savjani, J. K. (2012). Drug solubility: Importance and enhancement techniques. ISRN Pharmaceutics, 2012(100 mL), 1–10. https://doi.org/10.5402/2012/195727
Finch, A., & Pillans, P. (2014). P-glycoprotein and its role in drug-drug interactions. Australian Prescriber, 37(4), 137–139. https://doi.org/10.18773/austprescr.2014.050
Leeson, P. D., & Springthorpe, B. (2007). The influence of drug-like concepts on decision-making in medicinal chemistry. Nature Reviews Drug Discovery, 6(11), 881–890. https://doi.org/10.1038/nrd2445
Lipinski, C. A. (2003). Compound properties and drug quality. The practice of medicinal chemistry: Second edition (Second Edi.). Elsevier Inc. https://doi.org/10.1016/B978-012744481-9/50025-8
Veber, D. F., Johnson, S. R., Cheng, H. Y., Smith, B. R., Ward, K. W., & Kopple, K. D. (2002). Molecular properties that influence the oral bioavailability of drug candidates. Journal of Medicinal Chemistry, 45(12), 2615–2623. https://doi.org/10.1021/jm020017n
Pajouhesh, H., & Lenz, G. R. (2005). Medicinal chemical properties of successful central nervous system drugs. NeuroRx, 2(4), 541–553. https://doi.org/10.1602/neurorx.2.4.541
Husain, A., Ahmad, A., Khan, S. A., Asif, M., Bhutani, R., & Al-Abbasi, F. A. (2016). Synthesis, molecular properties, toxicity and biological evaluation of some new substituted imidazolidine derivatives in search of potent anti-inflammatory agents. Saudi Pharmaceutical Journal, 24(1), 104–114. https://doi.org/10.1016/j.jsps.2015.02.008
Rajasekaran, S., Prasad, P., & Rao, G. K. (2020). iMedPub Journals Molecular Properties and Bio-Activity Score of 2 {[ 2- ( 4-chlorophenyl ) -4- oxoquinazolin-3 ( 4H ) -yl ] amino } -N- ( substitutedphenyl ) acetamides Molinspiration software, 3, 12–14. https://doi.org/10.36648/0975-9344.12.1.153
Lutfiya, A. S., Priya, S., Manzoor, M. A. P., & Hemalatha, S. (2019). Molecular docking and interactions between vascular endothelial growth factor (VEGF) receptors and phytochemicals: An in-silico study. Biocatalysis and Agricultural Biotechnology, 22(October), 101424. https://doi.org/10.1016/j.bcab.2019.101424
Rosenbaum, D. M., Rasmussen, S. G. F., & Kobilka, B. K. (2009). The structure and function of G-protein-coupled receptors. Nature, 459(7245), 356–363. https://doi.org/10.1038/nature08144
Acknowledgements
The authors are thankful to B.S. Abdur Rahman Institute of Science & Technology, Chennai, for providing research facilities in school of life sciences. The authors also gratefully acknowledge ASEAN University network (AUN)/Southeast Asia Engineering Education Development Network (SEED)/Japan International Cooperation Agency (JICA) SPRAC (SN042/MI.KU/2020).
Author information
Authors and Affiliations
Contributions
SH conceived and designed research. FHB performed software analyses. All authors wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
All authors read and approved for publication.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Basha, F.H., S.Hemalatha Screening the Efficacy of Melatonin on Neurodegeneration Mediated by Endoplasmic Reticulum Stress, Inflammation, and Oxidative Damage. Appl Biochem Biotechnol 194, 1105–1119 (2022). https://doi.org/10.1007/s12010-022-03814-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12010-022-03814-x