Abstract
Much clinical experience has led us to assume that the administration of a β-blocker, regardless of dose or frequency, would produce similar mortality benefits in patients with heart failure. The results from the recently published Carvedilol or Metoprolol European Trial (COMET), which found greater benefit of carvedilol than immediate-release metoprolol on mortality, clearly demonstrated this is not true. In heart failure, the COMET results strongly support the use of β-blockers that have proven effective in largescale clinical trials. The primary disagreement regarding COMET concerns the explanation of the efficacy difference between the two β-blockers tested. Pharmacodynamic considerations and hemodynamic data from the COMET trial itself suggest there were unequal degrees of e 67-001-blockade between patients receiving carvedilol and immediaterelease metoprolol. Failure to achieve a similar degree of i,e 67-001-receptor blockade in the two groups prevents conclusions regarding the potential incremental benefits of selective versus nonselective adrenergic blockade. Further studies are needed to determine whether there are additional clinical benefits from the inhibition of adrenergic receptors beyond the proven benefits of i,e 67-001-blockade.
Similar content being viewed by others
References and Recommended Reading
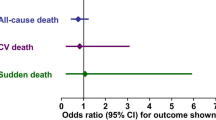
Poole-Wilson PA, Swedberg K, Cleland JG, et al.: Comparison of carvedilol and metoprolol on clinical outcomes in patients with chronic heart failure in the Carvedilol Or Metoprolol European Trial (COMET): randomized controlled trial. Lancet 2003, 362:7–13. This is an attempt to study the relative clinical efficacy of a β1-selective versus a nonselective β-blocker with β-blocking properties in patients with heart failure. The study supports the notion that adequate doses of β-blockade are important for the extent of clinical efficacy achieved. The primary controversy related to the study concerns the origin of the differential mortality effect of the two agents. This review argues that the difference is related to disimilar degrees of i,e 67-001-receptor blockade.
MERIT-HF Study Group: Effect of metoprolol CR/XL in chronic heart failure: Metoprolol CR/XL Randomised Intervention Trial in Congestive Heart Failure (MERIT-HF). Lancet 1999, 353:2001–2007.
Hjalmarson A, Goldstein S, Fagerberg B, et al.: Effects of controlled-release metoprolol on total mortality, hospitalizations, and well-being in patients with heart failure. The Metoprolol CR/XL Randomized Intervention Trial in Congestive Heart Failure (MERIT-HF). JAMA 2000, 283:1295–1302.
Waagstein F, Bristow MR, Swedberg K, et al.: Beneficial effects of metoprolol in idiopathic dilated cardiomyopathy. Metoprolol in Dilated Cardiomyopathy (MDC) Trial Study Group. Lancet 1993, 342:1441–1446.
Gattis WA: Metoprolol CR/XL in the treatment of chronic heart failure. Pharmacotherapy 2001, 21:604–613.
Sandberg A, Blomqvist I, Jonsson UE, Lundborg P: Pharmacokinetic and pharmacodynamic properties of a new controlledrelease formulation of metoprolol: a comparison with conventional tablets. Eur J Clin Pharmacol 1988, 33(Suppl): S9-S14.
Wikstrand J: Achieving optimal beta1-blockade with metoprolol CR/Zok. Basic Res Cardiol 2000, 95(Suppl 1):I46-I51.
Lechat P, Packer M, Chalon S, et al.: Clinical effects of betaadrenergic blockade in chronic heart failure: a meta-analysis of double-blind, placebo-controlled, randomized trials. Circulation 1998, 98:1184–1191.
Darmansjah I, Wong E, Setiawati D, et al.: Pharmacokinetic and pharmacodynamic properties of controlled release (CR/ZOK) metoprolol and atenolol. J Clin Pharmacol 1990, 30:S39-S45. This article provides information regarding the effects of different β-receptor blockers on exercise heart failure. It illustrates the pharmacodynamic differences between these compounds that translate pharmacokinetics into actual physiologic effects.
Andersson B, Aberg J, Lindelow B, et al.: Dose-related effects of metoprolol on heart rate and pharmacokinetics in heart failure. J Card Fail 2001, 7:311–317.
Wikstrand J, Hjalmarson A, Waagstein F, et al.: MERIT-HF Study Group. Dose of metoprolol CR/XL and clinical outcomes in patients with heart failure: analysis of the experience in metoprolol CR/XL randomized intervention trial in chronic heart failure (MERIT-HF). J Am Coll Cardiol 2002, 40:491–498. Although retrospective, this study appears to make an important contribution to our understanding of dose-response relationships related to ER metoprolol. The study indicates similar reductions in mortality, despite marked differences in dose, when similar reductions in resting HR are obtained. The study finding must be interpreted with caution, given the potential variable relationship between resting HR and degree of i,e 67-001-receptor blockade. However, the findings suggest that heart response during selective i,e 67-001-blockade may be predictive of clinical efficacy.
Packer M, Fowler MB, Roecker EB, et al.: Effect of carvedilol on the morbidity of patients with severe chronic heart failure: results of the Carvedilol Prospective Randomized Cumulative Survival (COPERNICUS) Study. Circulation 2002, 106:2194–2199.
Bristow MR, Gilbert EM, Abraham WT, et al.: Carvedilol produces dose-related improvements in left ventricular function and survival in subjects with chronic heart failure. MOCHA Investigators. Circulation 1996, 94:2807–2816.
Packer M, Coats AJ, Fowler MB, et al.: Effect of carvedilol on survival in severe chronic heart failure. N Engl J Med 2001, 344:1651–1658.
Neaton JD, Wentworth D: Serum cholesterol, blood pressure cigarette smoking, and death from coronary heart disease: overall findings and differences of age for 316,099 white men. Arch Intern Med 1992, 152:56–64.
Franklin SS, Larson MG, Kahn SA, et al.: Does the relation of blood pressure to coronary heart disease risk change with aging? Circulation 2001, 103:1245–1249.
Stamler J, Stamler R, Neaton JD. Blood pressure, systolic and diastolic, and cardiovascular risks: US population data. Arch Intern Med 1993, 153:598–615.
Izzo JL, Levy D, Black HR: Importance of systolic blood pressure in older Americans. Hypertension 2000, 35:1021–1024.
Brophy JM, Joseph L, Rouleau JL: Beta-blockers in congestive heart failure. A Bayesian meta-analysis. Ann Intern Med 2001, 134:550–560.
Adams KF: Which beta-blocker for heart failure? Am Heart J 2001, 141:884–888. This article provides an overview of the clinical and pharmacologic aspects of current β-blockers. It focuses on the basic mechanisms of action of these drugs and how they may differ. It integrates a clinical perspective into the overall assessment of the practical utility of one type of β-blocker over another.
Lowes BD, Gilbert EM, Abraham WT, et al.: Myocardial gene expression in dilated cardiomyopathy treated with beta-blocking agents. N Engl J Med 2002, 346:1357–1365. This is an important paper describing the effect of β-blockade on the molecular make-up of the failing human heart. It illustrates the apparent reversal by blockade of the fetal gene program induced by heart failure state.
American Heart Association: Heart Disease and Stroke Statistics-2003 Update. Dallas, TX: American Heart Association; 2002.
Heart Failure Society of America (HFSA) practice guidelines. HFSA guidelines for management of patients with heart failure caused by left ventricular systolic dysfunction-pharmacological approaches. J Card Fail 1999, 5:357–382.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Adams, K.F. How should COMET influence heart failure practice?. Curr Heart Fail Rep 1, 67–71 (2004). https://doi.org/10.1007/s11897-004-0028-1
Issue Date:
DOI: https://doi.org/10.1007/s11897-004-0028-1