Abstract
Purpose of Review
Chicago Classification has standardized clinical approach to primary esophageal motility disorders. With new clinical data and advancing treatments, Chicago Classification has undergone multiple revisions to reflect updated findings and enhance diagnostic accuracy. This review will describe the recently published Chicago Classification version 4.0 (CCv4.0), which aimed to enhance diagnostic characterization and limit overdiagnosis of inconclusive esophageal motility diagnoses.
Recent Findings
Key revisions outlined in CCv4.0 include (1) a modified standardized HRM study protocol performed in supine and upright positions, (2) recommended ancillary testing and manometric provocation for inconclusive manometric diagnoses (3) the required presence of obstructive symptoms for conclusive diagnoses of esophagogastric junction outflow obstruction, distal esophageal spasm and hypercontractile esophagus, and (4) requirement of confirmatory testing for esophagogastric junction outflow obstruction.
Summary
These key modifications aim to improve diagnostic accuracy and consistency of clinically relevant esophageal motility disorders, and subsequently clinical outcomes.


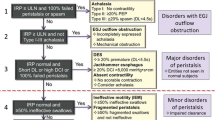
Adapted from the Chicago Classification version 4.0 ©. Hypercontractile Esophagus is defined by a normal median IRP and at least 20% or more swallows as hypercontractile (DCI ≥ 8000 mmHg-s-cm). In the Chicago Classification update hypercontractile esophagus is no longer synonymous with Jackhammer esophagus but rather may indicate one of three phenotypes: A) single peak hypercontractile swallow (the most common), B) jackhammer esophagus with repetitive prolonged contractions, or a new entity defined by a C) hypercontractile lower esophageal sphincter

Similar content being viewed by others
Abbreviations
- HRM:
-
High-resolution manometry
- CCv4.0:
-
Chicago Classification version 4.0
- EPT:
-
Esophageal pressure topography
- CCv1.0:
-
Chicago Classification version 1.0
- CCv2.0:
-
Chicago Classification version 2.0
- CCv3.0:
-
Chicago Classification version 3.0
- EGJ:
-
Esophagogastric junction
- EGJOO:
-
Esophagogastric junction outflow obstruction
- DCI:
-
Distal contractile integral
- IEM:
-
Ineffective esophageal motility
- IRP:
-
Integrated relaxation pressure
- LES:
-
Lower esophageal sphincter
- MRS:
-
Multiple rapid swallow
- RDC:
-
Rapid drink challenge
- TBE:
-
Timed barium esophagram
- FLIP:
-
Functional lumen imaging probe
- OIED:
-
Opioid-induced esophageal dysfunction
- DL:
-
Distal latency
- DES:
-
Distal esophageal spasm
- GERD:
-
Gastroesophageal reflux disease
References
Kahrilas PJ, Ghosh SK, Pandolfino JE. Esophageal motility disorders in terms of pressure topography: the Chicago Classification. J Clin Gastroenterol. 2008;42(5):627–35.
Pandolfino JE, et al. High-resolution manometry in clinical practice: utilizing pressure topography to classify oesophageal motility abnormalities. Neurogastroenterol Motil. 2009;21(8):796–806.
Yadlapati, R., et al., What is new in Chicago Classification version 4.0? Neurogastroenterol Motil, 2021. 33(1): p. e14053.
This article summarizes key modifications outlined in the recently published Chicago Classification version 4.0. The authors highlight updated criteria for disorders of esophageal motility in this concise review by outlining revised categorization, recommended ancillary tests, and future research implications.
Kahrilas, P.J., et al., The Chicago Classification of esophageal motility disorders, v3.0. Neurogastroenterol Motil, 2015. 27(2): p. 160–74.
Bredenoord AJ, et al. Chicago classification criteria of esophageal motility disorders defined in high resolution esophageal pressure topography. Neurogastroenterol Motil. 2012;24(Suppl 1):57–65.
Pandolfino JE, et al. Achalasia: a new clinically relevant classification by high-resolution manometry. Gastroenterology. 2008;135(5):1526–33.
Pratap N, et al. Achalasia cardia subtyping by high-resolution manometry predicts the therapeutic outcome of pneumatic balloon dilatation. J Neurogastroenterol Motil. 2011;17(1):48–53.
Rohof, W.O., et al., Outcomes of treatment for achalasia depend on manometric subtype. Gastroenterology, 2013. 144(4): p. 718–25; quiz e13–4.
Richter JE. High-resolution manometry in diagnosis and treatment of achalasia: help or hype. Curr Gastroenterol Rep. 2014;16(12):420.
Laing, P., et al., Trends in diagnoses after implementation of the Chicago classification for esophageal motility disorders (V3.0) for high-resolution manometry studies. Dis Esophagus, 2017. 30(12): p. 1–6.
Patel, A., et al., Comparison of motor diagnoses by Chicago Classification versions 2.0 and 3.0 on esophageal high-resolution manometry. Neurogastroenterol Motil, 2017. 29(7).
Yadlapati, R., et al., Esophageal motility disorders on high-resolution manometry: Chicago classification version 4.0((c)). Neurogastroenterol Motil, 2021. 33(1): p. e14058.
The authors provide an updated classification scheme for diagnosis of esophageal motility disorders that includes an expanded protocol. The updated diagnostic scheme aims to limit diagnostic ambiguity and improve diagnostic accuracy using newly developed data and therapies as well as supportive diagnostic testing.
Fox MR, et al. Inter-observer agreement for diagnostic classification of esophageal motility disorders defined in high-resolution manometry. Dis Esophagus. 2015;28(8):711–9.
Myers, J.C. and C. Cock, Achalasia subtypes are front and center of the Chicago classification—strategies to overcome limitations in clinical application. Annals of Esophagus, 2020. 3.
This article outlines achalasia subtypes and technical limitations in their diagnoses using Chicago Classification version 3.0 protocol. The authors describe diagnostic ambiguity and ancillary testing in the setting of inconclusive disorders of EGJ outflow. Overall, this article outlines key diagnostic limitations of Chicago Classification version 3.0 protocol that were at the forefront of the Chicago Classification version 4.0 modified protocol.
Ratuapli SK, et al. Opioid-Induced Esophageal Dysfunction (OIED) in Patients on Chronic Opioids. Am J Gastroenterol. 2015;110(7):979–84.
Myers JC, Cock C. Achalasia subtypes are front and center of the Chicago classification—strategies to overcome limitations in clinical application. Annals of Esophagus. 2020;3:24–24.
Samo S, Qayed E. Esophagogastric junction outflow obstruction: Where are we now in diagnosis and management? World J Gastroenterol. 2019;25(4):411–7.
Ihara E, et al. Diagnosis and Treatment Strategy of Achalasia Subtypes and Esophagogastric Junction Outflow Obstruction Based on High-Resolution Manometry. Digestion. 2017;95(1):29–35.
de Bortoli, N., et al., Hypercontractile Esophagus From Pathophysiology to Management: Proceedings of the Pisa Symposium. Am J Gastroenterol, 2021. 116(2): p. 263–273.
Achem SR, Vazquez-Elizondo G, Fass R. Jackhammer Esophagus: Current Concepts and Dilemmas. J Clin Gastroenterol. 2021;55(5):369–79.
Al-Qaisi MT, et al. The clinical significance of hypercontractile peristalsis: comparison of high-resolution manometric features, demographics, symptom presentation, and response to therapy in patients with Jackhammer esophagus versus Nutcracker esophagus. Dis Esophagus. 2017;30(12):1–7.
Funding
RY is supported by NIH K23 DK125266 (PI: Yadlapati).
Author information
Authors and Affiliations
Contributions
PS and RY: Literature review, drafting of manuscript, critical revision of manuscript, final approval of manuscript to be published.
Corresponding author
Ethics declarations
Conflicts of Interest
Rena Yadlapati: Institutional Consulting Agreement: Medtronic, Ironwood Pharmaceuticals, Diversatek; Consultant: Phathom Pharmaceuticals; Research support: Ironwood Pharmaceuticals; Advisory Board with Stock Options: RJS Mediagnostix; Priya Sharma: None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Neurogastroenterology and Motility Disorders of the Gastrointestinal Tract
Rights and permissions
About this article
Cite this article
Sharma, P., Yadlapati, R. Evaluation of Esophageal Motility and Lessons from Chicago Classification version 4.0. Curr Gastroenterol Rep 24, 10–17 (2022). https://doi.org/10.1007/s11894-022-00836-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11894-022-00836-7