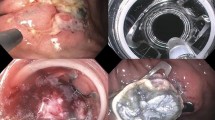
Abstract
Purpose of Review
Endoscopic submucosal dissection (ESD) is recognized as a minimally invasive treatment for colorectal cancer. However, colorectal ESD has not been internationally accepted as a first-line therapeutic option due to technical difficulties and high complication rates. Non-lifting tumors present a further limitation of ESD. Colorectal endoscopic full-thickness resection (eFTR) with over-the-scope clips (OTSCs) shows great potential in patients for whom ESD is not possible and also for those who might have ESD-related complications. The present manuscript aims to discuss the complementary role of eFTR using OTSCs and the future development of eFTR with a novel suturing device.
Recent Findings
Colorectal eFTR is feasible and has acceptable en bloc and R0 resection rates and procedure-related adverse events. This technique is primarily used for non-lifting and recurrent adenomas, especially in lesions ≤ 2 cm. This approach offers the potential to decrease the postoperative morbidity and mortality associated with segmental colectomy while enhancing the diagnostic yield compared to that of current endoscopic techniques.
Summary
eFTR using OTSCs is a safe and effective procedure for treating colorectal non-lifting and recurrent adenoma. The indications may be expanded to include subepithelial tumors, carcinoid tumors, and neuromuscular GI disorders. eFTR using OTSCs is not recommended for large lesions (> 30 mm), but innovative methods and new devices for eFTR and suturing will overcome the limitations by allowing minimally invasive surgery for colorectal cancer in the near future.

Similar content being viewed by others
Abbreviations
- EMR:
-
Endoscopic mucosal resection
- ESD:
-
Endoscopic submucosal dissection
- GI:
-
Gastrointestinal
- OTS:
-
Over-the-scope
- OTSC:
-
Over-the-scope clip
- FTRD:
-
Full-thickness resection device
- eFTR:
-
Endoscopic full-thickness resection
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Saito Y, Sakamoto T, Nakajima T, Matsuda T. Colorectal ESD: current indications and latest technical advances. Gastrointest Endosc Clin N Am. 2014;24(2):245–55. https://doi.org/10.1016/j.giec.2013.11.005.
Saito Y, Yamada M, So E, Abe S, Sakamoto T, Nakajima T, et al. Colorectal endoscopic submucosal dissection: technical advantages compared to endoscopic mucosal resection and minimally invasive surgery. Dig Endosc. 2014;26(Suppl 1):52–61. https://doi.org/10.1111/den.12196.
Oda I, Suzuki H, Nonaka S, Yoshinaga S. Complications of gastric endoscopic submucosal dissection. Dig Endosc. 2013;25(Suppl 1):71–8. https://doi.org/10.1111/j.1443-1661.2012.01376.x.
• Mönkemüller K, Peter S, Toshniwal J, Popa D, Zabielski M, Stahl RD, et al. Multipurpose use of the ‘bear claw’ (over-the-scope-clip system) to treat endoluminal gastrointestinal disorders. Dig Endosc. 2014;26(3):350–7. https://doi.org/10.1111/den.12145. This is an observational, open-label, retrospective, single-arm case series conducted at two hospitals with tertiary care endoscopy. The OTSC system is a useful device in a variety of clinical scenarios including the management of larger GI leaks and fistulas, GI bleeding, and full-thickness resection of tumors, even in very old and frail patients.
• Sarker S, Gutierrez JP, Council L, Brazelton JD, Kyanam Kabir Baig KR, Mönkemüller K. Over-the-scope clip-assisted method for resection of full-thickness submucosal lesions of the gastrointestinal tract. Endoscopy. 2014;46(09):758–61. https://doi.org/10.1055/s-0034-1365513. This was a retrospective, observational cohort study of patients undergoing endoscopic resection of submucosal lesions. This case series suggests that the OTSC system may be a valuable tool for the resection of submucosal lesions.
•• Fähndrich M, Sandmann M. Endoscopic full-thickness resection for gastrointestinal lesions using the over-the-scope clip system: a case series. Endoscopy. 2015;47(01):76–9. https://doi.org/10.1055/s-0034-1377975. This is retrospective, observational, open-label case study, a total of 17 patients underwent eFTR using OTSCs. The indications were carcinoids, incompletely resected colon cancers, recurrent fibrosed adenoma, and submucosal lesions. The technical success was 94 % (16 /17). The complete resection (R0) rate was 100 %. There were no complications.
Fujihara S, Mori H, Kobara H, Nishiyama N, Matsunaga T, Ayaki M, et al. Current innovations in endoscopic therapy for the management of colorectal cancer: from endoscopic submucosal dissection to endoscopic full-thickness resection. Biomed Res Int. 2014;2014:1–12. https://doi.org/10.1155/2014/925058.
Mori H, Kobara H, Nishiyama N, Fujihara S, Masaki T. Review of pure endoscopic full-thickness resection of the upper gastrointestinal tract. Gut Liver. 2015;9(5):590–600. https://doi.org/10.5009/gnl14380.
Schmidt A, Meier B, Caca K. Endoscopic full-thickness resection: current status. World J Gastroenterol. 2015;21(31):9273–85. https://doi.org/10.3748/wjg.v21.i31.9273.
•• Schmidt A, Bauerfeind P, Gubler C, Damm M, Bauder M, Caca K. Endoscopic full-thickness resection in the colorectum with a novel over-the-scope device: first experience. Endoscopy. 2015;47(8):719–25. This is retrospective, observational study at two tertiary referral centers. All resections were performed using the FTRD (full-thickness resection device). Indications for eFTR were recurrent or incompletely resected adenoma, untreated adenoma and nonlifting sign, adenoma involving the appendix, etc. The R0 resection rate was 75.0 % (18/24), and full-thickness resectionwas histologically confirmed in 87.5 %. There were no complications. https://doi.org/10.1055/s-0034-1391781.
Meier B, Caca K, Schmidt A. Hybrid endoscopic mucosal resection and full-thickness resection: a new approach for resection of large non-lifting colorectal adenomas (with video). Surg Endosc. 2017;31(10):4268–74. https://doi.org/10.1007/s00464-017-5461-9.
• Andrisani G, Pizzicannella M, Martino M, Rea R, Pandolfi M, Taffon C, et al. Endoscopic full-thickness resection of superficial colorectal neoplasms using a new over-the-scope clip system: a single-centre study. Dig Liver Dis. 2017;49:1–5. This is retrospective, observational, open-label case study, a total of 20 patients with superficial colorectalneoplasms, underwent EFTR using FTRD. The technical success rate was 100% (20/20). Mean size of the resected lesions was 26mm, ranging from 10 to 42mm.
•• Backes Y, Kappelle WF, Berk L, Koch AD, Groen JN, tot Nederveen WH, et al. Colorectal endoscopic full-thickness resection using a novel, flat-base over-the-scope clip: a prospective study. Endoscopy. 2017;49:1–2. This is a prospective study. Endoscopic full-thickness resection (eFTR) was performed using the Padlock clip. Indications for eFTR were mainly recurrent or incompletely resected adenoma, and nonlifting sign. Technical success rate and full-thickness resectionrate were 100 % (26/26) and 92 % (24/26). No complications occurred during the procedure.
• Valli PV, Mertens J, Bauerfeind P. Safe and successful resection of difficult GI lesions using a novel single-step full-thickness resection device (FTRD®). Surg Endosc. 2017; https://doi.org/10.1007/s00464-017-5676-9. This is retrospective, observational case study, a total of 60 patients underwent EFTR using FTRD. The technical success rate was 97% (58/60). The R0 resection rate was 88% (51/58) on histologically examination.
Sato K, Ito S, Kitagawa T, Kato M, Tominaga K, Suzuki T, et al. Factors affecting the technical difficulty and clinical outcome of endoscopic submucosal dissection for colorectal tumors. Surg Endosc. 2014;28(10):2959–65. https://doi.org/10.1007/s00464-014-3558-y.
Hayashi N, Tanaka S, Nishiyama S, Terasaki M, Nakadoi K, Oka S, et al. Predictors of incomplete resection and perforation associated with endoscopic submucosal dissection for colorectal tumors. Gastrointest Endosc. 2014;79(3):427–35. https://doi.org/10.1016/j.gie.2013.09.014.
Toyonaga T, Tanaka S, Man-I M, East J, Ono W, Nishino E, et al. Clinical significance of the muscle-retracting sign during colorectal endoscopic submucosal dissection. Endosc Int Open. 2015;3(03):E246–51. https://doi.org/10.1055/s-0034-1391665.
Oka S, Tanaka S, Saito Y, Iishi H, Kudo SE, Ikematsu H, et al. Local recurrence after endoscopic resection for large colorectal neoplasia: a multicenter prospective study in Japan. Am J Gastroenterol. 2015;110(5):697–707. https://doi.org/10.1038/ajg.2015.96.
Kobara H, Mori H, Chei L, Fujihara S, Nishiyama N, Masaki T. The advantage of an endoscopic submucosal tunneling technique for rectal carcinoid tumors. Gut Liver. 2017;11(5):735–7. https://doi.org/10.5009/gnl16580.
Fähndrich M, Heike M, Sandmann M. The Dortmund endoscopic full-thickness resection method: combination of the over-the-scope clip system and the Inoue cap. Endoscopy. 2014;46(Suppl 1 UCTN):E466. https://doi.org/10.1055/s-0034-1377548.
Di Mitri ML. One-session “2-step” technique for endoscopic full-thickness resection of a large rectal adenocarcinoma: when it is possible, overcome the lesion’s size. YMGE. American Society for Gastrointestinal Endoscopy; 2017.
Chen T, Yao LQ, Xu MD, Zhang YQ, Chen WF, Shi Q, et al. Efficacy and safety of endoscopic submucosal dissection for colorectal carcinoids. Clin Gastroenterol Hepatol. 2016;14(4):575–81. https://doi.org/10.1016/j.cgh.2015.07.048.
Kaneko H, Hirasawa K, Koh R, Kobayashi R, Kokawa A, Tanaka K, et al. Treatment outcomes of endoscopic resection for rectal carcinoid tumors: an analysis of the resectability and long-term results from 46 consecutive cases. Scand J Gastroenterol. 2016;51(12):1489–94. https://doi.org/10.1080/00365521.2016.1216591.
Al-Bawardy B, Rajan E, Wong Kee Song LM. Over-the-scope clip-assisted endoscopic full-thickness resection of epithelial and subepithelial GIlesions. Gastrointest Endosc. 2017;85(5):1087–92. https://doi.org/10.1016/j.gie.2016.08.019.
Grauer M, Gschwendtner A, Schäfer C, Neumann H. Resection of rectal carcinoids with the newly introduced endoscopic full-thickness resectiondevice. Endoscopy. 2016;48(Suppl 1):E123–4. https://doi.org/10.1055/s-0042-104651.
Klare P, Burlefinger R, Neu B, Bajbouj M, Specht K, Schmid RM, et al. Over-the-scope clip-assisted endoscopic full-thickness resection after incomplete resection of a rectal neuroendocrine tumor. Endoscopy. 2015;47(Suppl 1 UCTN):E47–8. https://doi.org/10.1055/s-0034-1391301.
Probst A, Schaller T, Messmann H. Gastrointestinal stromal tumor of the colon - endoscopic treatment by full-thickness resection. Endoscopy. 2015;47(Suppl 1 UCTN):E460–1. https://doi.org/10.1055/s-0034-1392862.
Salerno R, Gherardi G, Paternò E, Ardizzone S. Endoscopic full-thickness resection of a submucosal right colon lesion. Endoscopy. 2016;48(S 01):E376–E7. https://doi.org/10.1055/s-0042-120338.
Khater S, Rahmi G, Perrod G, Samaha E, Benosman H, Abbes L, et al. Over-the-scope clip (OTSC) reduces surgery rate in the management of iatrogenic gastrointestinal perforations. Endosc Int Open. 2017;5(05):E389–E94. https://doi.org/10.1055/s-0043-104862.
Brandler J, Baruah A, Zeb M, Mehfooz A, Pophali P, Wong Kee Song L, et al. Efficacy of over-the-scope clips in management of high-risk gastrointestinal bleeding. Clin Gastroenterol Hepatol. 2017; https://doi.org/10.1016/j.cgh.2017.07.020.
Wedi E, von Renteln D, Gonzalez S, Tkachenko O, Jung C, Orkut S, et al. Use of the over-the-scope-clip (OTSC) in non-variceal upper gastrointestinal bleeding in patients with severe cardiovascular comorbidities: a retrospective study. Endosc Int Open. 2017;5(09):E875–E82. https://doi.org/10.1055/s-0043-105496.
•• Haito-Chavez Y, Law JK, Kratt T, Arezzo A, Verra M, Morino M, et al. International multicenter experience with an over-the-scope clipping device for endoscopic management of GI defects (with video). Gastrointest Endosc. 2014;80(4):610–22. https://doi.org/10.1016/j.gie.2014.03.049. This is international multicenter study. A total of 188 patients (108 GI fistulae, 48 GI perforations, 32 GI leaks) were included. Long-term success of OTSC treatment was achieved in 60.2% of patients during a median follow-up of 146 days.
Kobara H, Mori H, Fujihara S, Nishiyama N, Chiyo T, Yamada T, et al. Outcomes of gastrointestinal defect closure with an over-the-scope clip system in a multicenter experience: an analysis of a successful suction method. World J Gastroenterol. 2017;23(9):1645–56. https://doi.org/10.3748/wjg.v23.i9.1645.
Nishiyama N, Mori H, Kobara H, Rafiq K, Fujihara S, Kobayashi M, et al. Efficacy and safety of over-the-scope clip: including complications after endoscopic submucosal dissection. World J Gastroenterol. 2013;19(18):2752–60. https://doi.org/10.3748/wjg.v19.i18.2752.
Valli PV, Pohl D, Fried M, Caduff R, Bauerfeind P. Diagnostic use of endoscopic full-thickness wall resection (eFTR)-a novel minimally invasive technique for colonic tissue sampling in patients with severe gastrointestinal motility disorders. Neurogastroenterol Motil. 2017;2017(59):e13153–6. https://doi.org/10.1111/nmo.13153.
Nishiyama N, Mori H, Kobara H, Fujihara S, Ayaki M, Miyai Y, et al. Minimal incision-assisted full-thickness sampling with over-the-scope clip targeting intestinalneuronal malformation. Endoscopy. 2017;49(S 01):E103–E4. https://doi.org/10.1055/s-0043-100626.
Dinelli M, Omazzi B, Andreozzi P, Zucchini N, Redaelli A, Manes G. First clinical experiences with a novel endoscopic over-the-scope clip system. Endosc Int Open. 2017;5(03):E151–E6. https://doi.org/10.1055/s-0043-101692.
Schmidt A, Riecken B, Damm M, Cahyadi O, Bauder M, Caca K. Endoscopic removal of over-the-scope clips using a novel cutting device: a retrospective case series. Endoscopy. 2014;46(09):762–6. https://doi.org/10.1055/s-0034-1365493.
•• Schmidt A, Beyna T, Schumacher B, Meining A, Richter-Schrag HJ, Messmann H, et al. Colonoscopic full-thickness resection using an over-the-scope device: a prospective multicentre study in various indications. Gut. 2017:gutjnl-2016-313677. https://doi.org/10.1136/gutjnl-2016-313677. This is a non-randomized, prospective multicenter study. All resections were performed using the FTRD. Indications for eFTR were difficult adenomas (non-lifting and/or at difficult locations), early cancers and subepithelial tumours. R0 resection rate was 77.7%. In general, R0 resection rate was higher with lesions ≤2 cm vs >2 cm (81.2% vs 58.1%, p=0.0038). Adverse event rate was 9.9% with a 2.2% rate of emergency surgery.
Tanaka S, Terasaki M, Hayashi N, Oka S, Chayama K. Warning for unprincipled colorectal endoscopic submucosal dissection: accurate diagnosis and reasonable treatment strategy. Dig Endosc. 2013;25(2):107–16. https://doi.org/10.1111/den.12016.
Rahmi G, Hotayt B, Chaussade S, Lepilliez V, Giovannini M, Coumaros D, et al. Endoscopic submucosal dissection for superficial rectal tumors: prospective evaluation in France. Endoscopy. 2014;46(08):670–6. https://doi.org/10.1055/s-0034-1365810.
Kiriyama S, Saito Y, Yamamoto S, Soetikno R, Matsuda T, Nakajima T, et al. Comparison of endoscopic submucosal dissection with laparoscopic-assisted colorectal surgery for early-stage colorectal cancer: a retrospective analysis. Endoscopy. 2012;44(11):1024–30. https://doi.org/10.1055/s-0032-1310259.
Nakamura F, Saito Y, Sakamoto T, Otake Y, Nakajima T, Yamamoto S, et al. Potential perioperative advantage of colorectal endoscopic submucosal dissection versus laparoscopy-assisted colectomy. Surg Endosc. 2015;29(3):596–606. https://doi.org/10.1007/s00464-014-3705-5.
Silva GL, de Moura EG, Bernardo WM, Leite de Castro V, Morais C, Baba ER, et al. Endoscopic versus surgical resection for early colorectal cancer-a systematic review and meta-analysis. J Gastrointest Oncol. 2016;7(3):326–35. https://doi.org/10.21037/jgo.2015.10.02.
Fischer A, Knoop RF, Walker C, Thimme R, Richter-Schrag HJ. Resection of a large rectal polyp with the simultaneous combination of snare polypectomy and full-thickness resection device resection. Endoscopy. 2015;47(Suppl 1):E607–E8. https://doi.org/10.1055/s-0035-1569658.
Jacob H, Toyonaga T, Ohara Y, Tsubouchi E, Takihara H, Baba S, et al. Endoscopic submucosal dissection of cecal lesions in proximity to the appendiceal orifice. Endoscopy. 2016;48(09):829–36. https://doi.org/10.1055/s-0042-110396.
Loske G, Schorsch T, Daseking E, Martens E, Müller CT. Small intestine grasped by over-the-scope-clip during attempt to close an iatrogenic colonicperforation. Endoscopy. 2016;48(Suppl 1 UCTN):E26–7. https://doi.org/10.1055/s-0041-110594.
Stavropoulos SN, Modayil R, Friedel D. Current applications of endoscopic suturing. World J Gastrointest Endosc. 2015;7(8):777–89. https://doi.org/10.4253/wjge.v7.i8.777.
Sharaiha RZ, Kumta NA, DeFilippis EM, Dimaio CJ, Gonzalez S, Gonda T, et al. A large multicenter experience with endoscopic suturing for management of gastrointestinal defects and stent anchorage in 122 patients: a retrospective review. J Clin Gastroenterol. 2016;50:388–92. https://doi.org/10.1097/MCG.0000000000000336.
Azzolini F, Cecinato P, Iori V, De Marco L, Sassatelli R. Endoscopic full-thickness resection for suspected residual rectal neuroendocrine tumor and closure of the defect with a new suturing system. Endoscopy. 2015;47(Suppl 1):E556–7. https://doi.org/10.1055/s-0034-1393384.
Kantsevoy SV, Bitner M, Mitrakov AA, Thuluvath PJ. Endoscopic suturing closure of large mucosal defects after endoscopic submucosal dissection is technically feasible, fast, and eliminates the need for hospitalization (with videos). Gastrointest Endosc. 2014;79(3):503–7. https://doi.org/10.1016/j.gie.2013.10.051.
Mori H, Kobara H, Fujihara S, Nishiyama N, Rafiq K, Oryu M, et al. Feasibility of pure EFTR using an innovative new endoscopic suturing device: the double-arm-bar suturing system (with video). Surg Endosc. 2014;28(2):683–90. https://doi.org/10.1007/s00464-013-3266-z.
Mori H, Rafiq K, Kobara H, Fujihara S, Nishiyama N, Oryuu M, et al. Innovative noninsufflation EFTR: sufficient endoscopic operative field by mechanical counter traction device. Surg Endosc. 2013;27(8):3028–34. https://doi.org/10.1007/s00464-013-2846-2.
Mori H, Kobara H, Tsushimi T, Fujihara S, Nishiyama N, Matsunaga T, et al. Reduction effect of bacterial counts by preoperative saline lavage of the stomach in performing laparoscopic and endoscopic cooperative surgery. World J Gastroenterol. 2014;20(42):15763–70. https://doi.org/10.3748/wjg.v20.i42.15763.
Goto O, Shimoda M, Sasaki M, Kiguchi Y, Mitsunaga Y, Akimoto T, et al. Potential for peritoneal cancer cell seeding in endoscopic full-thickness resection for early gastric cancer. Gastrointest Endosc. 2017; https://doi.org/10.1016/j.gie.2017.08.036.
Mori H, Kobara H, Fujihara S, Nishiyama N, Ayaki M, Chiyo T, et al. Innovative pure non-exposed endoscopic full-thickness resection using an endoscopic suturing device. Gastrointest Endosc. 2016;84(1):178–9. https://doi.org/10.1016/j.gie.2016.02.001.
Mori H, Rahman A, Kobara H, Fujihara S, Nishiyama N, Ayaki M, et al. Current status of exposed endoscopic full-thickness resection and further development of non-exposed endoscopic full-thickness resection. Digestion. 2017;95(1):6–15. https://doi.org/10.1159/000452352.
Acknowledgements
This article is dedicated to the memory of Dr. Hirohito Mori, Dr. Hideki Kobara, and Dr. Noriko Nishiyama who were our teachers and role models. They were always the first to try innovative ideas and inspired those around them to never stop challenging themselves.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Surgery and Surgical Innovations in Colorectal Cancer
Rights and permissions
About this article
Cite this article
Fujihara, S., Mori, H., Kobara, H. et al. Endoscopic Full-Thickness Resection for Colorectal Neoplasm: Current Status and Future Directions. Curr Colorectal Cancer Rep 14, 22–30 (2018). https://doi.org/10.1007/s11888-018-0399-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11888-018-0399-4