Abstract
Purpose of Review
To understand the current literature on age-related neural and detrusor changes associated with overactive bladder symptoms.
Recent Findings
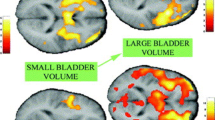
Recent functional magnetic resonance imaging (fMRI) studies have unveiled an age-related decrease in the neural control of continence, represented in the insula, anterior cingulate cortex (ACC), and prefrontal cortex (PFC). Older individuals with overactive bladder symptoms also demonstrate heightened activation of the ACC with low volumes, representing increased bladder sensitivity or sense of urgency. At the level of the bladder, age-related changes in the urothelium, neurotransmitters/receptors (both muscarinic and purinergic), and inflammation (including nerve growth factor (NGF), monocyte chemoattractant protein-1 (MCP-1), and oxidative stress) are also associated with overactive bladder.
Summary
Overactive bladder among older adults is a complex condition incorporating physiologic age-related changes from the brain to the bladder and beyond.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Milsom I, Stewart W, Thuroff J. The prevalence of overactive bladder. Am J Manag Care. 2000;6(11 Suppl):S565–73.
Abrams P, Cardozo L, Fall M, et al. The standardisation of terminology in lower urinary tract function: report from the standardisation sub-committee of the International Continence Society. Urology. 2003;61(1):37–49.
Wolff GF, Kuchel GA, Smith PP. Overactive bladder in the vulnerable elderly. Res Rep Urol. 2014;6:131–8.
Hald T, Horn T. The human urinary bladder in ageing. Br J Urol. 1998;82 Suppl 1:59–64.
Homma Y, Imajo C, Takahashi S, Kawabe K, Aso Y. Urinary symptoms and urodynamics in a normal elderly population. Scand J Urol Nephrol Suppl. 1994;157:27–30.
Tadic SD, Griffiths D, Schaefer W, Murrin A, Clarkson B, Resnick NM. Brain activity underlying impaired continence control in older women with overactive bladder. Neurourol Urodyn. 2012;31(5):652–8.
•• de Groat WC, Griffiths D, Yoshimura N. Neural control of the lower urinary tract. Compr Physiol. 2015;5(1):327–96. Excellent up-to-date review of insights into neural activity controlling the lower urinary tract.
•• Smith PP, Kuchel GA, Griffiths D. Functional brain imaging and the neural basis for voiding dysfunction in older adults. Clin Geriatr Med. 2015;31(4):549–65. In-depth review of recent advances in brain imaging, particularly studies using fMRI, and contributions to our understanding o neural control of the lower urinary tract.
Griffiths D, Derbyshire S, Stenger A, Resnick N. Brain control of normal and overactive bladder. J Urol. 2005;174(5):1862–7.
Kuhtz-Buschbeck JP, Gilster R, van der Horst C, Hamann M, Wolff S, Jansen O. Control of bladder sensations: an fMRI study of brain activity and effective connectivity. NeuroImage. 2009;47(1):18–27.
Fowler CJ, Griffiths D, de Groat WC. The neural control of micturition. Nat Rev Neurosci. 2008;9(6):453–66.
Griffiths DJ, Tadic SD, Schaefer W, Resnick NM. Cerebral control of the lower urinary tract: how age-related changes might predispose to urge incontinence. NeuroImage. 2009;47(3):981–6.
Griffiths D, Tadic SD, Schaefer W, Resnick NM. Cerebral control of the bladder in normal and urge-incontinent women. NeuroImage. 2007;37(1):1–7.
Sakakibara R, Panicker J, Fowler CJ, et al. Is overactive bladder a brain disease? The pathophysiological role of cerebral white matter in the elderly. Int J Urol: Off J Jpn Urol Assoc. 2014;21(1):33–8.
Sakakibara R, Hattori T, Uchiyama T, Yamanishi T. Urinary function in elderly people with and without leukoaraiosis: relation to cognitive and gait function. J Neurol Neurosurg Psychiatry. 1999;67(5):658–60.
Baloh RW, Vinters HV. White matter lesions and disequilibrium in older people. II. Clinicopathologic correlation. Arch Neurol. 1995;52(10):975–81.
Yamanouchi H, Nagura H. Neurological signs and frontal white matter lesions in vascular parkinsonism. A clinicopathologic study. Stroke; J Cereb Circ. 1997;28(5):965–9.
Mok VC, Wong A, Wong K, et al. Executive dysfunction and left frontal white matter hyperintensities are correlated with neuropsychiatric symptoms in stroke patients with confluent white matter hyperintensities. Dement Geriatr Cogn Disord. 2010;30(3):254–60.
Tadic SD, Griffiths D, Murrin A, Schaefer W, Aizenstein HJ, Resnick NM. Brain activity during bladder filling is related to white matter structural changes in older women with urinary incontinence. NeuroImage. 2010;51(4):1294–302.
Araki I, Kitahara M, Oida T, Kuno S. Voiding dysfunction and Parkinson’s disease: urodynamic abnormalities and urinary symptoms. J Urol. 2000;164(5):1640–3.
Kitta T, Kakizaki H, Furuno T, et al. Brain activation during detrusor overactivity in patients with Parkinson’s disease: a positron emission tomography study. J Urol. 2006;175(3 Pt 1):994–8.
Sakakibara R, Fowler CJ, Hattori T. Voiding and MRI analysis of the brain. Int Urogynecol J Pelvic Floor Dysfunct. 1999;10(3):192–9.
Griffiths D. Clinical studies of cerebral and urinary tract function in elderly people with urinary incontinence. Behav Brain Res. 1998;92(2):151–5.
Ishiura Y. Experimental study of voiding dysfunction induced by cerebral infarction in rats. Nihon Hinyokika Gakkai zasshi Jpn J Urol. 1996;87(11):1221–30.
Suzuki M, Ohtake A, Yoshino T, et al. Effects of solifenacin succinate (YM905) on detrusor overactivity in conscious cerebral infarcted rats. Eur J Pharmacol. 2005;512(1):61–6.
Maruyama S, Kurosawa S, Takagi Y, et al. Urodynamics and bladder muscarinic receptors in rats with cerebral infarction and bladder outlet obstruction. Neurosci Lett. 2007;414(1):80–4.
Siroky MB. The aging bladder. Rev Urol. 2004;6 Suppl 1:S3–7.
Lepor H, Sunaryadi I, Hartanto V, Shapiro E. Quantitative morphometry of the adult human bladder. J Urol. 1992;148(2 Pt 1):414–7.
Ameda K, Sullivan MP, Bae RJ, Yalla SV. Urodynamic characterization of nonobstructive voiding dysfunction in symptomatic elderly men. J Urol. 1999;162(1):142–6.
Azadzoi KM, Tarcan T, Kozlowski R, Krane RJ, Siroky MB. Overactivity and structural changes in the chronically ischemic bladder. J Urol. 1999;162(5):1768–78.
• Birder L, Andersson KE. Urothelial signaling. Physiol Rev. 2013;93(2):653–80. Thorough review of the complexities of urothelial signalling incorporating current research studies/advances.
Mulvey MA, Schilling JD, Martinez JJ, Hultgren SJ. Bad bugs and beleaguered bladders: interplay between uropathogenic Escherichia coli and innate host defenses. Proc Natl Acad Sci U S A. 2000;97(16):8829–35.
Gibson W, Wagg A. New horizons: urinary incontinence in older people. Age Ageing. 2014;43(2):157–63.
Yoshida M, Homma Y, Inadome A, et al. Age-related changes in cholinergic and purinergic neurotransmission in human isolated bladder smooth muscles. Exp Gerontol. 2001;36(1):99–109.
Mansfield KJ, Liu L, Mitchelson FJ, Moore KH, Millard RJ, Burcher E. Muscarinic receptor subtypes in human bladder detrusor and mucosa, studied by radioligand binding and quantitative competitive RT-PCR: changes in ageing. Br J Pharmacol. 2005;144(8):1089–99.
O’Reilly BA, Kosaka AH, Knight GF, et al. P2X receptors and their role in female idiopathic detrusor instability. J Urol. 2002;167(1):157–64.
Santos ML, Gomes WF, Pereira DS, et al. Muscle strength, muscle balance, physical function and plasma interleukin-6 (IL-6) levels in elderly women with knee osteoarthritis (OA). Arch Gerontol Geriatr. 2011;52(3):322–6.
Blain H, Jaussent A, Beziat S, et al. Low serum IL-6 is associated with high 6-minute walking performance in asymptomatic women aged 20 to 70 years. Exp Gerontol. 2012;47(2):143–8.
•• Tyagi P, Tyagi V, Qu X, et al. Association of inflammaging (inflammation + aging) with higher prevalence of OAB in elderly population. Int Urol Nephrol. 2014;46(5):871–7. Recent study describing age-related biochemical changes associated with inflammation and overactive bladder, particularly NGF and MCP-1.
Kashyap M, Kawamorita N, Tyagi V, et al. Down-regulation o f nerve growth factor expression in the bladder by antisense oligonucleotides as new treatment for overactive bladder. J Urol. 2013;190(2):757–64.
Taylor 3rd JA, Kuchel GA. Detrusor underactivity: clinical features and pathogenesis of an underdiagnosed geriatric condition. J Am Geriatr Soc. 2006;54(12):1920–32.
Liu HT, Chancellor MB, Kuo HC. Decrease of urinary nerve growth factor levels after antimuscarinic therapy in patients with overactive bladder. BJU Int. 2009;103(12):1668–72.
Semirale AA, Zhang XW, Wiren KM. Body composition changes and inhibition of fat development in vivo implicates androgen in regulation of stem cell lineage allocation. J Cell Biochem. 2011;112(7):1773–86.
Tajar A, O’Connell MD, Mitnitski AB, et al. Frailty in relation to variations in hormone levels of the hypothalamic-pituitary-testicular axis in older men: results from the European male aging study. J Am Geriatr Soc. 2011;59(5):814–21.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Dr. Suskind has no conflicts of interests to declare.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Funding
This paper was supported and funded by NIDDK K12 DK83021-09.
Additional information
This article is part of the Topical Collection on Overactive Bladder
Rights and permissions
About this article
Cite this article
Suskind, A.M. The Aging Overactive Bladder: a Review of Aging-Related Changes from the Brain to the Bladder. Curr Bladder Dysfunct Rep 12, 42–47 (2017). https://doi.org/10.1007/s11884-017-0406-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11884-017-0406-7