Abstract
Purpose
Pediatric patients who undergo hematopoietic cell transplant (HCT) are at risk for neurocognitive impairments, which can impact quality of life. Given limited long-term studies, we aimed to characterize the late neurocognitive outcomes in a cohort of pediatric HCT survivors.
Methods
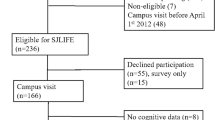
Eligible survivors (HCT at age < 21 year and ≥ 1 year post-HCT) completed a 60-question survey of neurocognitive function and quality of life, which included the Childhood Cancer Survivor Study Neurocognitive Questionnaire (CCSS-NCQ) and the Neuro-Quality of Life Cognitive Function Short Form (Neuro-QoL). Analyses of risk factors included univariate comparisons and multivariable logistic regression.
Results
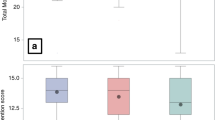
Participants (n = 199, 50.3% female, 53.3% acute leukemia, 87.9% allogeneic transplants) were surveyed at median age of 37.8 years (interquartile range [IQR] 28.5–48.8) at survey and median 27.6 years (IQR 17.0–34.0) from transplant. On the CCSS-NCQ, 18.9–32.5% of survivors reported impairments (Z score > 1.28) in task efficiency, memory, emotional regulation, or organization, compared with expected 10% in the general population (all p < 0.01). In contrast, survivors reported average Neuro-QoL (T score 49.6±0.7) compared with population normative value of 50 (p = 0.52). In multivariable regression, impaired Neuro-QoL (T score < 40) was independently associated with hearing issues (OR 4.97, 95% CI 1.96-12.6), history of stroke or seizure (OR 4.46, 95% CI 1.44-13.8), and sleep disturbances (OR 6.95, 95% CI 2.53–19.1).
Conclusions
Although long-term survivors of pediatric HCT reported higher rates of impairment in specific neurocognitive domains, cognitive quality of life was perceived as similar to the general population. Subsets of survivors with certain co-morbidities had substantially worse neurocognitive outcomes.
Implications for Cancer Survivors
While the long-term impact of pediatric HCT can include neurocognitive deficits, survivors report average cognitive quality of life.

Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Chow EJ, Anderson L, Baker KS, Bhatia S, Guilcher GM, Huang JT, et al. Late effects surveillance recommendations among survivors of childhood hematopoietic cell transplantation: a Children's Oncology Group report. Biology of Blood and Marrow Transplantation. 2016;22(5):782–95.
Yen H-J, Eissa H, Bhatt NS, Huang S, Ehrhardt M, Bhakta N et al. Patient-reported outcomes in survivors of childhood hematologic malignancies with hematopoietic stem cell transplant. Blood Journal. 2020:blood. 2019003858.
Buchbinder D, Kelly DL, Duarte RF, Auletta JJ, Bhatt N, Byrne M, et al. Neurocognitive dysfunction in hematopoietic cell transplant recipients: expert review from the late effects and Quality of Life Working Committee of the CIBMTR and complications and Quality of Life Working Party of the EBMT. Bone Marrow Transplant. 2018;53(5):535–55.
Kadan-Lottick NS, Zeltzer LK, Liu Q, Yasui Y, Ellenberg L, Gioia G, et al. Neurocognitive functioning in adult survivors of childhood non-central nervous system cancers. JNCI: Journal of the National Cancer Institute. 2010;102(12):881–93.
Ellenberg L, Liu Q, Gioia G, Yasui Y, Packer RJ, Mertens A, et al. Neurocognitive status in long-term survivors of childhood CNS malignancies: a report from the Childhood Cancer Survivor Study. Neuropsychology. 2009;23(6):705–17.
Krull KR, Hardy KK, Kahalley LS, Schuitema I, Kesler SR. Neurocognitive outcomes and interventions in long-term survivors of childhood cancer. J Clin Oncol. 2018;36(21):2181–9.
Iyer NS, Balsamo LM, Bracken MB, Kadan-Lottick NS. Chemotherapy-only treatment effects on long-term neurocognitive functioning in childhood ALL survivors: a review and meta-analysis. Blood. 2015;126(3):346–53.
Brinkman TM, Krasin MJ, Liu W, Armstrong GT, Ojha RP, Sadighi ZS, et al. Long-term neurocognitive functioning and social attainment in adult survivors of pediatric CNS tumors: results from the St Jude Lifetime Cohort Study. J Clin Oncol. 2016;34(12):1358–67.
Krull KR, Annett RD, Pan Z, Ness KK, Nathan PC, Srivastava DK, et al. Neurocognitive functioning and health-related behaviours in adult survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. Eur J Cancer. 2011;47(9):1380–8.
Clanton NR, Klosky JL, Li C, Jain N, Srivastava DK, Mulrooney D, et al. Fatigue, vitality, sleep, and neurocognitive functioning in adult survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. Cancer. 2011;117(11):2559–68.
Mulrooney DA, Ness KK, Neglia JP, Whitton JA, Green DM, Zeltzer LK, et al. Fatigue and sleep disturbance in adult survivors of childhood cancer: a report from the childhood cancer survivor study (CCSS). Sleep. 2008;31(2):271–81.
Cheung YT, Brinkman TM, Li C, Mzayek Y, Srivastava D, Ness KK, et al. Chronic health conditions and neurocognitive function in aging survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. JNCI: Journal of the National Cancer Institute. 2018;110(4):411–9.
Barrera M, Atenafu E. Cognitive, educational, psychosocial adjustment and quality of life of children who survive hematopoietic SCT and their siblings. Bone Marrow Transplant. 2008;42(1):15–21.
Harder H, Cornelissen JJ, Van Gool AR, Duivenvoorden HJ, Eijkenboom WM, van den Bent MJ. Cognitive functioning and quality of life in long-term adult survivors of bone marrow transplantation. Cancer. 2002;95(1):183–92.
Phipps S, Rai SN, Leung W-H, Lensing S, Dunavant M. Cognitive and academic consequences of stem-cell transplantation in children. J Clin Oncol. 2008;26(12):2027–33.
Syrjala KL, Artherholt SB, Kurland BF, Langer SL, Roth-Roemer S, Elrod JB, et al. Prospective neurocognitive function over 5 years after allogeneic hematopoietic cell transplantation for cancer survivors compared with matched controls at 5 years. J Clin Oncol. 2011;29(17):2397–404.
Parsons SK, Phipps S, Sung L, Baker KS, Pulsipher MA, Ness KK. NCI, NHLBI/PBMTC first international conference on late effects after pediatric hematopoietic cell transplantation: health-related quality of life, functional, and neurocognitive outcomes. Biology of Blood and Marrow Transplantation. 2012;18(2):162–71.
Kelly DL, Buchbinder D, Duarte RF, Auletta JJ, Bhatt N, Byrne M, et al. Neurocognitive dysfunction in hematopoietic cell transplant recipients: expert review from the Late Effects and Quality of Life Working Committee of the Center for International Blood and Marrow Transplant Research and Complications and Quality of Life Working Party of the European Society for Blood and Marrow Transplantation. Biology of Blood and Marrow Transplantation. 2018;24(2):228–41.
Baker KS, Bhatia S, Bunin N, Nieder M, Dvorak CC, Sung L, et al. NCI, NHLBI first international consensus conference on late effects after pediatric hematopoietic cell transplantation: state of the science, future directions. Biology of Blood and Marrow Transplantation. 2011;17(10):1424–7.
Lee SJ, Onstad L, Chow EJ, Shaw BE, Jim HS, Syrjala KL, et al. Patient-reported outcomes and health status associated with chronic graft-versus-host disease. Haematologica. 2018;103(9):1535–41.
Khera N, Chow EJ, Leisenring WM, Syrjala KL, Baker KS, Flowers ME, et al. Factors associated with adherence to preventive care practices among hematopoietic cell transplantation survivors. Biology of Blood and Marrow Transplantation. 2011;17(7):995–1003.
Kenzik KM, Huang I, Brinkman TM, Baughman B, Ness KK, Shenkman EA, et al. The Childhood Cancer Survivor Study–Neurocognitive Questionnaire (CCSS-NCQ) revised: item response analysis and concurrent validity. Neuropsychology. 2015;29(1):31–44.
Krull KR, Gioia G, Ness KK, Ellenberg L, Recklitis C, Leisenring W, et al. Reliability and validity of the childhood cancer survivor study neurocognitive questionnaire. Cancer. 2008;113(8):2188–97.
National Institute of Neurological Disorders and Stroke (NINDS). User Manual for the Quality of Life in Neurological Disorders (Neuro-QoL) Measures, Version 2.02015.
Gershon RC, Lai JS, Bode R, Choi S, Moy C, Bleck T, et al. Neuro-QOL: quality of life item banks for adults with neurological disorders: item development and calibrations based upon clinical and general population testing. Qual Life Res. 2012;21(3):475–86.
Yu L, Buysse DJ, Germain A, Moul DE, Stover A, Dodds NE, et al. Development of short forms from the PROMIS™ sleep disturbance and sleep-related impairment item banks. Behav Sleep Med. 2012;10(1):6–24.
National Health and Nutrition Examination Survey. Audiometry. 2011. https://wwwn.cdc.gov/nchs/data/nhanes/2011-2012/questionnaires/auq.pdf. Accessed 06/01/2020.
Childhood Cancer Survivor Study. Questionnaires. 2020. https://ccss.stjude.org/tools-and-documents/questionnaires.html. Accessed Oct 15 2020.
Gabel N, Altshuler DB, Brezzell A, Briceño EM, Boileau NR, Miklja Z, et al. Health related quality of life in adult low and high-grade glioma patients using the national institutes of health patient reported outcomes measurement information system (PROMIS) and neuro-QOL assessments. Front Neurol. 2019;10:212.
Seaman SR, White IR. Review of inverse probability weighting for dealing with missing data. Stat Methods Med Res. 2013;22(3):278–95.
Parris KR, Russell KM, Triplett BM, Phipps S. Neurocognitive functioning in long-term survivors of pediatric hematopoietic cell transplantation. Bone Marrow Transplant. 2020:1–10.
Baker KS, Bresters D, Sande JE. The burden of cure: long-term side effects following hematopoietic stem cell transplantation (HSCT) in children. Pediatr Clin. 2010;57(1):323–42.
Willard VW, Leung W, Huang Q, Zhang H, Phipps S. Cognitive outcome after pediatric stem-cell transplantation: impact of age and total-body irradiation. J Clin Oncol. 2014;32(35):3982–8.
Armstrong GT, Jain N, Liu W, Merchant TE, Stovall M, Srivastava DK, et al. Region-specific radiotherapy and neuropsychological outcomes in adult survivors of childhood CNS malignancies. Neuro-oncology. 2010;12(11):1173–86.
Armstrong GT, Liu Q, Yasui Y, Huang S, Ness KK, Leisenring W, et al. Long-term outcomes among adult survivors of childhood central nervous system malignancies in the Childhood Cancer Survivor Study. JNCI: Journal of the National Cancer Institute. 2009;101(13):946–58.
Krull KR, Zhang N, Santucci A, Srivastava DK, Krasin MJ, Kun LE, et al. Long-term decline in intelligence among adult survivors of childhood acute lymphoblastic leukemia treated with cranial radiation. Blood, The Journal of the American Society of Hematology. 2013;122(4):550–3.
Mueller S, Kline CN, Buerki RA, Chen Y, Yasui Y, Howell R, et al. Stroke impact on mortality and psychologic morbidity within the Childhood Cancer Survivor Study. Cancer. 2020;126(5):1051–9.
Children's Oncology Group. Long-term follow-up guidelines for survivors of childhood, adolescent and young adult cancers. : Children’s Oncology Group2018.
Phipps S, Dunavant M, Srivastava DK, Bowman L, Mulhern RK. Cognitive and academic functioning in survivors of pediatric bone marrow transplantation. J Clin Oncol. 2000;18(5):1004.
Willasch AM, Peters C, Sedláček P, Dalle J-H, Kitra-Roussou V, Yesilipek A, et al. Myeloablative conditioning for allo-HSCT in pediatric ALL: FTBI or chemotherapy?—A multicenter EBMT-PDWP study. Bone Marrow Transplant. 2020;55(8):1540–51.
Bunin N, Aplenc R, Kamani N, Shaw K, Cnaan A, Simms S. Randomized trial of busulfan vs total body irradiation containing conditioning regimens for children with acute lymphoblastic leukemia: a Pediatric Blood and Marrow Transplant Consortium study. Bone Marrow Transplant. 2003;32(6):543–8.
Code availability
The code generated during the current study is available from the corresponding author on reasonable request.
Funding
This study was funded in part by the National Institute of Health (NIH) grants CA15704 and CA18029.
Author information
Authors and Affiliations
Contributions
Kevin R. Krull, Nicole J. Ullrich, Nina S. Kadan-Lottick, Stephanie J. Lee, and Eric J. Chow contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Natalie L. Wu, Kara L. Cushing-Haugen, and Eric J. Chow. The first draft of the manuscript was written by Natalie L. Wu and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Fred Hutchinson Institutional Review Board on March 16, 2018.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wu, N.L., Krull, K.R., Cushing-Haugen, K.L. et al. Long-term neurocognitive and quality of life outcomes in survivors of pediatric hematopoietic cell transplant. J Cancer Surviv 16, 696–704 (2022). https://doi.org/10.1007/s11764-021-01063-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-021-01063-1