Abstract
Objectives
To summarize the experience of mitral valve (MV) repair with artificial chordae replacement in children, and analyze early and intermediate outcomes.
Methods
From January 2011 to May 2019, all patients (< 18 years) who received MV repair with artificial chordae replacement were retrospectively reviewed. Freedom from MV reoperation, MV dysfunction, moderate or severe MR were estimated by the Kaplan–Meier curve and log-rank test.
Results
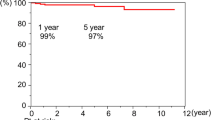
A total of 30 patients were included in this study. According to our definition, 15 patients had simple lesions and 15 patients had complex lesions. During 36 months’ follow-up (range 3–97 months), two patients received MV reoperation and seven patients developed MV dysfunction, including six patients with moderate or severe MR and one patient with mitral stenosis. Freedom from MV reoperation at 1, 5 and 8 years were 100%, 91.3% and 91.3%, respectively. And freedom from MV dysfunction at 1, 3 and 5 year were 96.0%, 77.1% and 61.8%, respectively. Five-year freedom from MV dysfunction showed significant differences between patients with simple lesions and patients with complex lesions (100% vs 32.7%, log-rank P = 0.008), and between patients aged less than 12 years and patients aged more than 12 year (33.5% vs 90.0%, log-rank P = 0.025).
Conclusion
The early and intermediate outcomes of mitral valve repair with artificial chordae replacement were acceptable in children, and the outcomes were optimal in patients with simple lesions, and patients aged more than 12 years.




Similar content being viewed by others

References
Beierlein W, Becker V, Yates R, et al. Long-term follow-up after mitral valve replacement in childhood: poor event-free survival in the young child. Eur J Cardiothorac Surg. 2007;31:860–5. https://doi.org/10.1016/j.ejcts.2007.02.006.
Selamet Tierney ES, Pigula FA, Berul CI, et al. Mitral valve replacement in infants and children 5 years of age or younger: evolution in practice and outcome over three decades with a focus on supra-annular prosthesis implantation. J Thorac Cardiovasc Surg. 2008;136(954–61):961. https://doi.org/10.1016/j.jtcvs.2007.12.076.
Caldarone CA, Raghuveer G, Hills CB, et al. Long-term survival after mitral valve replacement in children aged < 5 years: a multi-institutional study. Circulation. 2001;104:I143–7. https://doi.org/10.1161/hc37t1.094840.
Brown JW, Fiore AC, Ruzmetov M, et al. Evolution of mitral valve replacement in children: a 40-year experience. Ann Thorac Surg. 2012;93:626–33. https://doi.org/10.1016/j.athoracsur.2011.08.085.
David TE. Replacement of chordae tendineae with expanded polytetrafluoroethylene sutures. J Card Surg. 1989;4:286–90. https://doi.org/10.1111/j.1540-8191.1989.tb00291.x.
David TE, Armstrong S, Ivanov J. Chordal replacement with polytetrafluoroethylene sutures for mitral valve repair: a 25-year experience. J Thorac Cardiovasc Surg. 2013;145:1563–9. https://doi.org/10.1016/j.jtcvs.2012.05.030.
Salvador L, Mirone S, Bianchini R, et al. A 20-year experience with mitral valve repair with artificial chordae in 608 patients. J Thorac Cardiovasc Surg. 2008;135:1280–7. https://doi.org/10.1016/j.jtcvs.2007.12.026.
Oda S, Nakano T, Tatewaki H, et al. A 17-year experience with mitral valve repair with artificial chordae in infants and children. Eur J Cardiothorac Surg. 2013;44:e40–5. https://doi.org/10.1093/ejcts/ezt183.
Kluin J, Sojak V, Koolbergen DR, et al. Fifteen years’ experience with the use of artificial chords for valve reconstruction in children. Eur J Cardiothorac Surg. 2017;52:1155–60. https://doi.org/10.1093/ejcts/ezx146.
Murashita T, Hoashi T, Kagisaki K, et al. Long-term results of mitral valve repair for severe mitral regurgitation in infants: fate of artificial chordae. Ann Thorac Surg. 2012;94:581–6. https://doi.org/10.1016/j.athoracsur.2012.03.064.
Sai S, Konishi A, Sato M, et al. Efficacy of artificial chordal reconstruction for idiopathic severe mitral regurgitation due to chordal rupture in infancy. Semin Thorac Cardiovasc Surg. 2015;27:321–5. https://doi.org/10.1053/j.semtcvs.2015.08.004.
Fattouch K, Bianco G, Sbraga F, et al. Simple, safe and easy technique to ensure the correct length of artificial chordae in mitral valve repair. Ann Thorac Surg. 2007;83:1902–3. https://doi.org/10.1016/j.athoracsur.2006.06.012.
Zoghbi WA, Adams D, Bonow RO, et al. Recommendations for noninvasive evaluation of native valvular regurgitation: a report from the American Society of Echocardiography Developed in Collaboration with the Society for Cardiovascular Magnetic Resonance. J Am Soc Echocardiogr. 2017;30:303–71. https://doi.org/10.1016/j.echo.2017.01.007.
Carpentier A, Branchini B, Cour JC, et al. Congenital malformations of the mitral valve in children. Pathology and surgical treatment. J Thorac Cardiovasc Surg. 1976;72:854–66.
Minami K, Kado H, Sai S, et al. Midterm results of mitral valve repair with artificial chordae in children. J Thorac Cardiovasc Surg. 2005;129:336–42. https://doi.org/10.1016/j.jtcvs.2004.10.016.
Matsumoto T, Kado H, Masuda M, et al. Clinical results of mitral valve repair by reconstructing artificial chordae tendineae in children. J Thorac Cardiovasc Surg. 1999;118:94–8. https://doi.org/10.1016/S0022-5223(99)70147-9.
Vida VL, Zanotto L, Carrozzini M, et al. Repair techniques for mitral valve insufficiency in children. Seminars in thoracic and cardiovascular surgery. Pediatric Cardiac Surg Ann. 2018. https://doi.org/10.1053/j.pcsu.2017.11.004.
Eishi K, Kawazoe K, Nakano K, et al. Long-term results of artificial chordae implantation in patients with mitral valve prolapse. J Heart Valve Dis. 1997;6:594–8.
Eishi K, Kawazoe K, Sasako Y, et al. Comparison of repair techniques for mitral valve prolapse. J Heart Valve Dis. 1994;3:432–8.
Chauvaud S, Fuzellier JF, Houel R, et al. Reconstructive surgery in congenital mitral valve insufficiency (Carpentier’s techniques): long-term results. J Thorac Cardiovasc Surg. 1998;115:84–92. https://doi.org/10.1016/s0022-5223(98)99001-8.
Kalfa D, Vergnat M, Ly M, et al. A standardized repair-oriented strategy for mitral insufficiency in infants and children: midterm functional outcomes and predictors of adverse events. J Thorac Cardiovasc Surg. 2014. https://doi.org/10.1016/j.jtcvs.2014.02.057.
Hetzer R, Delmo WEB, Hübler M, et al. Modified surgical techniques and long-term outcome of mitral valve reconstruction in 111 children. Ann Thorac Surg. 2008. https://doi.org/10.1016/j.athoracsur.2008.03.026.
Oppido G, Davies B, McMullan DM, et al. Surgical treatment of congenital mitral valve disease: midterm results of a repair-oriented policy. J Thorac Cardiovasc Surg. 2008. https://doi.org/10.1016/j.jtcvs.2007.09.071.
Alfieri O, Maisano F, de Bonis M, et al. The double-orifice technique in mitral valve repair: a simple solution for complex problems. J Thorac Cardiovasc Surg. 2001;122:674–81. https://doi.org/10.1067/mtc.2001.117277.
Vricella La, Ravekes WA, Arbustini E, et al. Simplified mitral valve repair in pediatric patients with connective tissue disorders. J Thorac Cardiovasc Surg. 2017. https://doi.org/10.1016/j.jtcvs.2016.09.039.
Anyanwu AC, Itagaki S, Chikwe J, et al. A complexity scoring system for degenerative mitral valve repair. J Thorac Cardiovasc Surg. 2016. https://doi.org/10.1016/j.jtcvs.2016.01.033.
Qi L, Ma K, Zhang B, et al. Pediatric mitral regurgitation: standardized repair-oriented strategy with leaflet plication. Semin Thorac Cardiovasc Surg. 2020. https://doi.org/10.1053/j.semtcvs.2020.05.029.
Funding
No.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Yaojun Dun, Jiayi Xing, Dong Zhao, Wenjun Su, Guohua Luo, and Keming Yang have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dun, Y., Xing, J., Zhao, D. et al. Mitral valve repair with artificial chordae replacement in children: a single-center experience. Gen Thorac Cardiovasc Surg 69, 1383–1391 (2021). https://doi.org/10.1007/s11748-021-01597-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-021-01597-2