Abstract
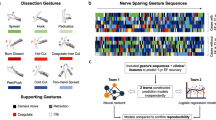
Our group previously defined a dissection gesture classification system that deconstructs robotic tissue dissection into its most elemental yet meaningful movements. The purpose of this study was to expand upon this framework by adding an assessment of gesture efficacy (ineffective, effective, or erroneous) and analyze dissection patterns between groups of surgeons of varying experience. We defined three possible gesture efficacies as ineffective (no meaningful effect on the tissue), effective (intended effect on the tissue), and erroneous (unintended disruption of the tissue). Novices (0 prior robotic cases), intermediates (1–99 cases), and experts (≥ 100 cases) completed a robotic dissection task in a dry-lab training environment. Video recordings were reviewed to classify each gesture and determine its efficacy, then dissection patterns between groups were analyzed. 23 participants completed the task, with 9 novices, 8 intermediates with median caseload 60 (IQR 41–80), and 6 experts with median caseload 525 (IQR 413–900). For gesture selection, we found increasing experience associated with increasing proportion of overall dissection gestures (p = 0.009) and decreasing proportion of retraction gestures (p = 0.009). For gesture efficacy, novices performed the greatest proportion of ineffective gestures (9.8%, p < 0.001), intermediates commit the greatest proportion of erroneous gestures (26.8%, p < 0.001), and the three groups performed similar proportions of overall effective gestures, though experts performed the greatest proportion of effective retraction gestures (85.6%, p < 0.001). Between groups of experience, we found significant differences in gesture selection and gesture efficacy. These relationships may provide insight into further improving surgical training.


Similar content being viewed by others
References
Birkmeyer JD, Finks JF, O’Reilly A et al (2013) Surgical skill and complication rates after bariatric surgery. N Engl J Med 369:1434–1442. https://doi.org/10.1056/NEJMsa1300625
Fecso AB, Szasz P, Kerezov G, Grantcharov TP (2017) The Effect of Technical Performance on Patient Outcomes in Surgery: A Systematic Review. Ann Surg 265:492–501. https://doi.org/10.1097/SLA.0000000000001959
Hung AJ, Chen J, Ghodoussipour S et al (2019) Deep learning on automated performance metrics and clinical features to predict urinary continence recovery after robot-assisted radical prostatectomy. BJU Int 124:487–495. https://doi.org/10.1111/bju.14735
Sridhar AN, Briggs TP, Kelly JD, Nathan S (2017) Training in robotic surgery—an overview. Curr Urol Rep 18:58. https://doi.org/10.1007/s11934-017-0710-y
Gabrysz-Forget F, Young M, Zahabi S et al (2020) Surgical errors happen, but are learners trained to recover from them? a survey of North American surgical residents and fellows. J Surg Educ 77:1552–1561. https://doi.org/10.1016/j.jsurg.2020.05.031
Vanlander AE, Mazzone E, Collins JW et al (2020) Orsi Consensus Meeting on European Robotic Training (OCERT): results from the first multispecialty consensus meeting on training in robot-assisted surgery. Eur Urol 78(5):713–716. https://doi.org/10.1016/j.eururo.2020.02.003
Gallagher AG, De Groote R, Paciotti M, Mottrie A (2022) Proficiency-based progression training: a scientific approach to learning surgical skills. Eur Urol 81(4):394–395. https://doi.org/10.1016/j.eururo.2022.01.004
Chen J, Cheng N, Cacciamani G et al (2019) Objective assessment of robotic surgical technical skill: a systematic review. J Urol 201:461–469. https://doi.org/10.1016/j.juro.2018.06.078
Hung AJ, Ma R, Cen S et al (2021) Surgeon Automated Performance Metrics as Predictors of Early Urinary Continence Recovery After Robotic Radical Prostatectomy—A Prospective Bi-institutional Study. Eur Urol Open Sci 27:65–72. https://doi.org/10.1016/j.euros.2021.03.005
Collins JW, Levy J, Stefanidis D et al (2019) Utilising the delphi process to develop a proficiency-based progression train-the-trainer course for robotic surgery training. Eur Urol 75:775–785. https://doi.org/10.1016/j.eururo.2018.12.044
Goh AC, Goldfarb DW, Sander JC et al (2012) Global evaluative assessment of robotic skills: validation of a clinical assessment tool to measure robotic surgical skills. J Urol 187:247–252. https://doi.org/10.1016/j.juro.2011.09.032
Hussein AA, Ghani KR, Peabody J et al (2017) Development and validation of an objective scoring tool for robot-assisted radical prostatectomy: prostatectomy assessment and competency evaluation. J Urol 197:1237–1244. https://doi.org/10.1016/j.juro.2016.11.100
Vanstrum EB, Ma R, Maya-Silva J et al (2021) Development and Validation of an objective scoring tool to evaluate surgical dissection: Dissection Assessment for Robotic Technique (DART). Urology Practice 8:596–604. https://doi.org/10.1097/UPJ.0000000000000246
Chen J, Oh PJ, Cheng N et al (2018) Use of automated performance metrics to measure surgeon performance during robotic Vesicourethral anastomosis and methodical development of a training tutorial. J Urol 200:895–902. https://doi.org/10.1016/j.juro.2018.05.080
Collins JW, Dell’Oglio P, Hung AJ, Brook NR (2018) The importance of technical and non-technical skills in Robotic surgery training. Eur Urol Focus 4:674–676. https://doi.org/10.1016/j.euf.2018.08.018
Ma R, Vanstrum EB, Nguyen JH et al (2021) A novel dissection gesture classification to characterize robotic dissection technique for renal hilar dissection. J Urol 205:271–275. https://doi.org/10.1097/JU.0000000000001328
Hung AJ, Chen J, Jarc A et al (2018) Development and validation of objective performance metrics for robot-assisted radical prostatectomy: a Pilot Study. J Urol 199:296–304. https://doi.org/10.1016/j.juro.2017.07.081
Abboudi H, Khan MS, Guru KA et al (2014) Learning curves for urological procedures: a systematic review. BJU Int 114:617–629. https://doi.org/10.1111/bju.12315
Nguyen JH, Chen J, Marshall SP et al (2020) Using objective robotic automated performance metrics and task-evoked pupillary response to distinguish surgeon expertise. World J Urol 38:1599–1605. https://doi.org/10.1007/s00345-019-02881-w
Roberts SI, Cen SY, Nguyen J et al (2021) The relationship of technical skills and cognitive workload to errors during robotic surgical exercises. J Endourol 36:712–720. https://doi.org/10.1089/end.2021.0790
Luongo F, Hakim R, Nguyen JH et al (2021) Deep learning-based computer vision to recognize and classify suturing gestures in robot-assisted surgery. Surgery 169:1240–1244. https://doi.org/10.1016/j.surg.2020.08.016
Acknowledgements
None
Funding
The authors declare that no support, financial or otherwise, were received for the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
D Inouye: project development, data collection and management, data analysis, manuscript writing and editing. R Ma: project development, data management, data analysis, manuscript writing and editing. J Nguyen: project development, data analysis, manuscript writing and editing. J Laca: project development, data analysis. R Kocielnik: project development, data analysis. A Anandkumar: project development. A Hung: project development, data analysis, manuscript writing and editing.
Corresponding author
Ethics declarations
Conflict of interest
Andrew J. Hung has financial disclosures with Intuitive Surgical, Inc.
Ethics approval
This study was approved by the University of Southern California’s Institutional Review Board (protocol HS-16–00,318).
Consent to participate
Informed consent was obtained per Institutional Review Board protocol.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Inouye, D.A., Ma, R., Nguyen, J.H. et al. Assessing the efficacy of dissection gestures in robotic surgery. J Robotic Surg 17, 597–603 (2023). https://doi.org/10.1007/s11701-022-01458-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-022-01458-x