Abstract
Objective
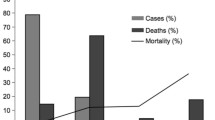
Pulmonary complications in patients with obesity carry a high morbidity and mortality. An analysis of the MBSAQIP database was performed to determine the effect of post-operative pulmonary complications on patients undergoing elective bariatric surgery, with the primary outcome of 30-day mortality.
Methods
We extracted data from the MBSAQIP database from 2015 to 2019 on patients who underwent elective Roux-en-Y gastric bypass or sleeve gastrectomy. Pulmonary complications were defined as prolonged ventilation, pneumonia, unplanned intubation, pulmonary embolism, and coma past 24 h (with the assumption of this being due to hypercapnia). Data on post-operative complications and 30-day mortality was extracted. To determine the effect of pulmonary complications on 30-day mortality, a multivariable logistic regression model was developed.
Results
Pulmonary complications were associated with a near 50-fold increased odds of 30-day mortality (OR 47.1; 95%, 38.6–57.5; p < 0.0001). Pulmonary complications were also associated with higher rates of anastomotic leaks (9.5% vs. 0.3%; p < 0.0001), post-operative bleeding (13.7% vs. 0.9%; p < 0.0001), cardiac complications (6.6% vs. 0.0%; p < 0.0001), post-operative AKIs (9.6% vs. 0.1%; p < 0.0001), incidence of deep SSI (9.4% vs. 0.2%; p < 0.0001), incidence of post-operative sepsis (6.2% vs. 0.1%; p < 0.0001), and incidence of Clostridioides difficile (2.0% vs. 0.1%; p < 0.0001).
Conclusion
Pulmonary complications after elective bariatric surgery are a strong predictor of 30-day mortality. Patients who experience pulmonary complications have a higher incidence of co-morbidities and unfavorable baseline patient characteristics, and thus, likely form a unique subset of the bariatric patient population.
Graphical abstract

Similar content being viewed by others
References
Collaboration NCDRF. Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: a pooled analysis of 2416 population-based measurement studies in 128.9 million children, adolescents, and adults. Lancet 2017;390(10113):2627–42.
Inoue Y, Qin B, Poti J, et al. Epidemiology of obesity in adults: latest trends. Curr Obes Rep. 2018;7(4):276–88.
Piziak VK. Medical management of obesity. Compr Ther. 1991;17(3):54–9.
Salminen P, Helmio M, Ovaska J, et al. Effect of laparoscopic sleeve gastrectomy vs laparoscopic Roux-en-Y gastric bypass on weight loss at 5 years among patients with morbid obesity: the SLEEVEPASS randomized clinical trial. JAMA. 2018;319(3):241–54.
Littleton SW, Tulaimat A. The effects of obesity on lung volumes and oxygenation. Respir Med. 2017;124:15–20.
Gupta PK, Gupta H, Kaushik M, et al. Predictors of pulmonary complications after bariatric surgery. Surg Obes Relat Dis. 2012;8(5):574–81.
Miskovic A, Lumb AB. Postoperative pulmonary complications. Br J Anaesth. 2017;118(3):317–34.
Yang CK, Teng A, Lee DY, et al. Pulmonary complications after major abdominal surgery: National Surgical Quality Improvement Program analysis. J Surg Res. 2015;198(2):441–9.
Koenig SM. Pulmonary complications of obesity. Am J Med Sci. 2001;321(4):249–79.
Ortega FB, Lavie CJ, Blair SN. Obesity and Cardiovascular Disease. Circ Res. 2016;118(11):1752–70.
Zewari S, Vos P, van den Elshout F, et al. Obesity in COPD: Revealed and Unrevealed Issues. COPD. 2017;14(6):663–73.
Peters U, Dixon AE, Forno E. Obesity and asthma. J Allergy Clin Immunol. 2018;141(4):1169–79.
Hubbard RE, Lang IA, Llewellyn DJ, et al. Frailty, body mass index, and abdominal obesity in older people. J Gerontol A Biol Sci Med Sci. 2010;65(4):377–81.
Choi KM. Sarcopenia and sarcopenic obesity. Korean J Intern Med. 2016;31(6):1054–60.
Mosli RH, Mosli HH. Obesity and morbid obesity associated with higher odds of hypoalbuminemia in adults without liver disease or renal failure. Diabetes Metab Syndr Obes. 2017;10:467–72.
Novello M, Mandarino FV, Di Saverio S, et al. Post-operative outcomes and predictors of mortality after colorectal cancer surgery in the very elderly patients. Heliyon. 2019;5(8):e02363.
Emile SH, Elgamal M, Elshobaky A, et al. Identifying patients at high risk of having pulmonary dysfunction before laparoscopic bariatric surgery and its impact on postoperative pulmonary complications. J Laparoendosc Adv Surg Tech A. 2019;29(11):1456–61.
Pantel H, Hwang J, Brams D, et al. Effect of incentive spirometry on postoperative hypoxemia and pulmonary complications after bariatric surgery: a randomized clinical trial. JAMA Surg. 2017;152(5):422–8.
van Huisstede A, Biter LU, Luitwieler R, et al. Pulmonary function testing and complications of laparoscopic bariatric surgery. Obes Surg. 2013;23(10):1596–603.
Series F, Genest C, Martin M, et al. CPAP is not needed in every sleep apnea patient awaiting bariatric surgery. Obes Surg. 2021;31(5):2161–7.
Author information
Authors and Affiliations
Contributions
All the authors have contributed equally to this work.
Corresponding author
Ethics declarations
Ethics Approval and Informed Consent
Consent was not required for this retrospective study. The MBSAQIP database is maintained in compliance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• Pulmonary complications after bariatric surgery are predictors of 30-day mortality.
• Patients with pulmonary complications have more baseline co-morbidities.
• Identifying high-risk patients pre-operatively may enable optimization prior to bariatric surgery.
Rights and permissions
About this article
Cite this article
Jogiat, U., Mocanu, V., Birch, D.W. et al. Pulmonary Complications Are a Strong Independent Predictor of 30-Day Mortality Following Elective Bariatric Surgery. OBES SURG 32, 696–703 (2022). https://doi.org/10.1007/s11695-021-05882-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-021-05882-0