Abstract
Background
Prediction of type 2 diabetes (T2DM) remission is an important part of risk-benefit assessment before bariatric surgery.
Study Design
Advanced-DiaRem (Ad-DiaRem) and ABCD diabetes remission scores for sleeve gastrectomy (SG) and Roux-en-Y gastric bypass (RYGB) were calculated using baseline data. Differences in model discrimination using area under the curve of receiver operating curve (AUC-ROC) and model calibration were tested for complete remission (HbA1c ≤ 6.0% without antidiabetic medications) in the two groups. Optimal cutoff scores were calculated using the Youden index.
Results
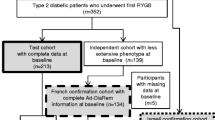
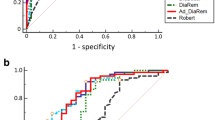
We randomized 109 patients to either SG or RYGB. With one patient lost to follow-up in each group, the scores were calculated for 54 patients in the SG group and 53 patients in the RYGB group. Both models showed moderate predictive power without any significant difference between the groups: AUC-ROCs (95% CI) for the Ad-DiaRem score (SG versus RYGB) were 0.872 (0.780–0.964) versus 0.843 (0.733–0.954), p = 0.69, and for the ABCD score 0.849 (0.752–0.946) versus 0.750 (0.580–0.920), p = 0.32, respectively. Using optimal cutoff points derived from the whole study population, the actual proportion of diabetes remission was significantly higher than predicted for both the Ad-DiaRem and ABCD scores in the RYGB group. Diabetes duration and glycated haemoglobin predicted diabetes remission in the entire Oseberg population.
Conclusion
Both the Ad-DiaRem and ABCD scores showed moderate ability to discriminate between those who achieved remission of T2DM and those who did not after SG and RYGB. Larger studies are needed for the identification of procedure-specific optimal cutoffs.
Trial Registration
ClinicalTrials.gov Identifier: NCT01778738
Graphical abstract




Similar content being viewed by others
References
Jakobsen GS, et al. Association of bariatric surgery vs medical obesity treatment with long-term medical complications and obesity-related comorbidities, (in eng). JAMA. 2018;319(3):291–301. https://doi.org/10.1001/jama.2017.21055.
Angrisani L, Santonicola A, Iovino P, Ramos A, Shikora S, Kow L. Bariatric surgery survey 2018: similarities and disparities among the 5 IFSO chapters, (in eng). Obes Surg. 1-12, Jan 12 2021. https://doi.org/10.1007/s11695-020-05207-7.
Coleman KJ, et al. Long-term microvascular disease outcomes in patients with type 2 diabetes after bariatric surgery: evidence for the legacy effect of surgery. Diabetes Care. 2016;39(8):1400–7. https://doi.org/10.2337/dc16-0194.
Lean ME, et al. Primary care-led weight management for remission of type 2 diabetes (DiRECT): an open-label, cluster-randomised trial. Lancet. 2018;391(10120):541–51. https://doi.org/10.1016/S0140-6736(17)33102-1.
Park JY. Prediction of type 2 diabetes remission after bariatric or metabolic surgery, (in eng). J Obes Metab Syndr. 2018;27(4):213–22. https://doi.org/10.7570/jomes.2018.27.4.213.
Zhang R, et al. Systematic review of risk prediction models for diabetes after bariatric surgery, (in eng). Br J Surg. 2016;103(11):1420–7. https://doi.org/10.1002/bjs.10255.
Aron-Wisnewsky J, et al. The advanced-DiaRem score improves prediction of diabetes remission 1 year post-Roux-en-Y gastric bypass. Diabetologia 2017;60(10):1892-1902. 2017/10/01. https://doi.org/10.1007/s00125-017-4371-7.
Still CD, et al. Preoperative prediction of type 2 diabetes remission after Roux-en-Y gastric bypass surgery: a retrospective cohort study, (in eng). Lancet Diabetes Endocrinol. 2014;2(1):38–45. https://doi.org/10.1016/s2213-8587(13)70070-6.
Lee WJ, et al. Predicting success of metabolic surgery: age, body mass index, C-peptide, and duration score, (in eng). Surg Obes Relat Dis. 2013;9(3):379-84. May-Jun 2013. https://doi.org/10.1016/j.soard.2012.07.015.
Lee WJ, Almulaifi A, Tsou JJ, Ser KH, Lee YC, Chen SC. Laparoscopic sleeve gastrectomy for type 2 diabetes mellitus: predicting the success by ABCD score, (in eng). Surg Obes Relat Dis. 2015;11(5):991-6. https://doi.org/10.1016/j.soard.2014.12.027.
Lee WJ, et al. Preoperative prediction of type 2 diabetes remission after gastric bypass surgery: a comparison of DiaRem scores and ABCD scores, (in eng). Obes Surg. 2016;26(10):2418–24. https://doi.org/10.1007/s11695-016-2120-5.
Lee WJ, et al. The effect and predictive score of gastric bypass and sleeve gastrectomy on type 2 diabetes mellitus patients with BMI < 30 kg/m(2), (in eng). Obes Surg. 2015;25(10):1772–8. https://doi.org/10.1007/s11695-015-1603-0.
Dicker D, et al. Prediction of long-term diabetes remission after RYGB, sleeve gastrectomy, and adjustable gastric banding using DiaRem and advanced-DiaRem scores. Obes Surg. 2019;29(3):796-804. 2019/03/01. https://doi.org/10.1007/s11695-018-3583-3.
Kam H, et al. Comparison of four risk prediction models for diabetes remission after Roux-en-Y gastric bypass surgery in obese Chinese patients with type 2 diabetes mellitus, (in eng). Obes Surg. 2020;30(6):2147–57. https://doi.org/10.1007/s11695-019-04371-9.
Shen SC, et al. Validating risk prediction models of diabetes remission after sleeve gastrectomy, (in eng). Obes Surg. 2019;29(1):221–9. https://doi.org/10.1007/s11695-018-3510-7.
Sjöholm K, et al. Evaluation of prediction models for type 2 diabetes relapse after post-bariatric surgery remission: a post hoc analysis of 15-year follow-up data from the Swedish obese subjects (SOS) study, (in eng). Obes Surg. 2020;30(10):3955–60. https://doi.org/10.1007/s11695-020-04763-2.
Aarts EO, Janssen J, Janssen IM, Berends FJ, Telting D, de Boer H. Preoperative fasting plasma C-peptide level may help to predict diabetes outcome after gastric bypass surgery, (in eng). Obes Surg. 2013;23(7):867–73. https://doi.org/10.1007/s11695-013-0872-8.
Bhasker AG, Remedios C, Batra P, Sood A, Shaikh S, Lakdawala M. Predictors of remission of T2DM and metabolic effects after laparoscopic Roux-en-y gastric bypass in obese Indian diabetics-a 5-year study, (in eng). Obes Surg. 2015;25(7):1191–7. https://doi.org/10.1007/s11695-014-1501-x.
Blackstone R, Bunt JC, Cortés MC, Sugerman HJ. Type 2 diabetes after gastric bypass: remission in five models using HbA1c, fasting blood glucose, and medication status, (in eng). Surg Obes Relat Dis. 2012;8(5):548-55. https://doi.org/10.1016/j.soard.2012.05.005.
Hayes MT, Hunt LA, Foo J, Tychinskaya Y, Stubbs RS. A model for predicting the resolution of type 2 diabetes in severely obese subjects following Roux-en Y gastric bypass surgery, (in eng). Obes Surg. 2011;21(7):910–6. https://doi.org/10.1007/s11695-011-0370-9.
Park JY, Kim YJ. Prediction of diabetes remission in morbidly obese patients after Roux-en-Y gastric bypass, (in eng). Obes Surg. 2016;26(4):749–56. https://doi.org/10.1007/s11695-015-1823-3.
Schauer PR, et al. Bariatric surgery versus intensive medical therapy for diabetes–3-year outcomes, (in eng). N Engl J Med. 2014;370(21):2002–13. https://doi.org/10.1056/NEJMoa1401329.
Robert M, et al. Predictive factors of type 2 diabetes remission 1 year after bariatric surgery: impact of surgical techniques, (in eng). Obes Surg. 2013;23(6):770–5. https://doi.org/10.1007/s11695-013-0868-4.
Hofso D, et al. Gastric bypass versus sleeve gastrectomy in patients with type 2 diabetes (Oseberg): a single-centre, triple-blind, randomised controlled trial, (in eng). Lancet Diabetes Endocrinol. 2019;7(12):912–24. https://doi.org/10.1016/s2213-8587(19)30344-4.
Borgeraas H, et al. Single-centre, triple-blinded, randomised, 1-year, parallel-group, superiority study to compare the effects of Roux-en-Y gastric bypass and sleeve gastrectomy on remission of type 2 diabetes and beta-cell function in subjects with morbid obesity: a protocol for the Obesity surgery in Tonsberg (Oseberg) study, (in eng).BMJ open 2019;9(6):e024573. https://doi.org/10.1136/bmjopen-2018-024573.
Collins GS, Reitsma JB, Altman DG, Moons KG. Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD Statement, (in eng). BMC Med. 2015;13:1. https://doi.org/10.1186/s12916-014-0241-z.
Swets JA. Measuring the accuracy of diagnostic systems, (in eng). Science. 1988;240(4857):1285–93. https://doi.org/10.1126/science.3287615.
Youden WJ. Index for rating diagnostic tests, (in eng). Cancer. 1950;3(1):32–5. https://doi.org/10.1002/1097-0142(1950)3:1%3c32::aid-cncr2820030106%3e3.0.co;2-3.
Warner RM. Applied Statistics: From Bivariate through Multivariate Techniques. 2nd ed. Thousand Oaks (in English): SAGE Publications; 2013.
Borgeraas H, Hofso D, Hertel JK, Hjelmesaeth J. Comparison of the effect of Roux-en-Y gastric bypass and sleeve gastrectomy on remission of type 2 diabetes: a systematic review and meta-analysis of randomized controlled trials, (in eng). Obes Rev. 2020. https://doi.org/10.1111/obr.13011.
Hjelmesæth J, Fatima F, Birkeland KI, Svanevik M, Hofsø D. Metabolic surgery: one size fits all? – Authors’ reply, (in eng). Lancet Diabetes Endocrinol. 2020;8(4):273. https://doi.org/10.1016/s2213-8587(20)30027-9.
Acknowledgements
We thank the participants, the patient representative and all the study personnel. We particularly thank Linda Mathisen, Karina Bautz, Berit Mossing Bjørkås, Andreas Aarvik, Heidi Omre Fon, Hanna Lakso, Carina Rambo, Inger Mari Flakstad and Astrid Hillestad (Morbid Obesity Center, Vestfold Hospital Trust, Tønsberg, Norway) for their continuous efforts, enthusiasm and patient care, thereby ensuring the collection of high-quality data in the Oseberg study. We also thank Matthew McGee (Morbid Obesity Center, Vestfold Hospital Trust) for proofreading the manuscript.
Author information
Authors and Affiliations
Contributions
D.H. and J.H. conceived the study and are the principal investigators. D.H., F.F., J.K.H., M.S., R.S. and J.H. contributed to the design and overlooked the study conduct. F.F., D.H. and J.H. wrote the manuscript. M.C.S. was responsible for the statistical analyses. All authors critically participated in the interpretation of the data, reviewed the manuscript for intellectual content and approved the final version of the manuscript. All authors had independent access to the data and took responsibility for data completeness and accuracy, as well as the fidelity of the trial to the protocol.
Corresponding author
Ethics declarations
Ethical Approval
All participants provided a written informed consent. The study protocol was approved by the Regional Committees for Medical and Health Research Ethics (ref: 2012/1427/REK sør-øst) and is in accordance with the Helsinki-II declaration.
Conflict of Interest
F.F. declares an educational grant (PhD) from South-Eastern Norway, Regional Health Authority during the conduct of the study. J.H. declares honoraria from Novo Nordisk, Boehringer Ingelheim and Navamedic, outside the submitted work. D.H. declares honoraria from Novo Nordisk, Lilly and Sanofi, outside the submitted work. Other authors have no conflict of interest.
Disclaimer
The funder of the study had no role in study design, data collection, data analyses, data interpretation or writing of the report. All authors had independent access to the data and took responsibility for data completeness and accuracy, and for the fidelity of the trial to the protocol. The corresponding author had full access to all the data in the study and had final responsibility for the decision to submit for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points
1. Ad-DiaRem and ABCD scores predicted T2DM remission after SG and RYGB.
2. Observed diabetes remission was significantly higher than predicted in the RYGB group.
3. Larger studies are needed to identify procedure-specific optimal cutoffs.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Fatima, F., Hjelmesæth, J., Hertel, J.K. et al. Validation of Ad-DiaRem and ABCD Diabetes Remission Prediction Scores at 1-Year After Roux-en-Y Gastric Bypass and Sleeve Gastrectomy in the Randomized Controlled Oseberg Trial. OBES SURG 32, 801–809 (2022). https://doi.org/10.1007/s11695-021-05856-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-021-05856-2