Abstract
Purpose
This study aims to characterize complications, metabolic improvement, and change in ambulation status for patients with impaired mobility undergoing bariatric surgery.
Material and Methods
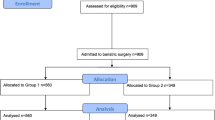
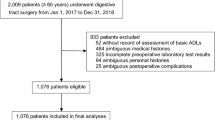
Individuals undergoing primary sleeve gastrectomy (SG) or Roux-en-Y gastric bypass (RYGB) from February 2008 to December 2015 were included. Impaired mobility (WC) was defined as using a wheelchair or motorized scooter for at least part of a typical day. The WC group was propensity score matched to ambulatory patients (1:5 ratio). Comparisons were made for 30-day morbidity and mortality and 1-year improvement in weight-related comorbidities.
Results
There were 93 patients in the WC group matched to 465 ambulatory controls. The median operative time (180 vs 159 min, p = 0.003) and postoperative length of stay (4 vs 3 days, p ≤ 0.001) was higher in the WC group. There were no differences in readmission or all-cause morbidity within 30 days. The median percent excess weight loss (%EWL) at 1 year was similar (WC group, 65% available, 53% EWL vs AMB group, 73% available, 54% EWL); however, patients with impaired mobility were less likely to experience improvement in diabetes (76 vs 90%, p = 0.046), hypertension (63 vs 82%, p < 0.005), and obstructive sleep apnea (53 vs 71%, p < 0.001). Within the WC group, 62% had improvement in their mobility status, eliminating dependence on wheelchair or scooter assistance.
Conclusion
Patients with both obesity and impaired mobility experience similar rates of perioperative morbidity and weight loss at 1 year compared to ambulatory controls. However, improvement in weight-related comorbidities may be less likely with impaired mobility.
Similar content being viewed by others
References
Garver MJ, Focht BC, Dials J, et al. Weight status and differences in mobility performance, pain symptoms, and physical activity in older, knee osteoarthritis patients. Arthritis. 2014;2014:1–7. https://doi.org/10.1155/2014/375909.
Hergenroeder AL, Wert DM, Hile ES, et al. Association of body mass index with self-report and performance-based measures of balance and mobility. Phys Ther. 2011;91(8):1223–34. https://doi.org/10.2522/ptj.20100214.
Peytremann-Bridevaux I, Santos-Eggimann B. Health correlates of overweight and obesity in adults aged 50 years and over: results from the Survey of Health, Ageing and Retirement in Europe (SHARE). Obesity and health in Europeans aged ≥ or = 50 years. Swiss Med Wkly. 2008;138(17–18):261–6.
Oliveria SA, Felson DT, Cirillo PA, et al. Body weight, body mass index, and incident symptomatic osteoarthritis of the hand, hip, and knee. Epidemiology. 1999;10(2):161–6. https://doi.org/10.1097/00001648-199903000-00013.
Johnson VL, Hunter DJ. The epidemiology of osteoarthritis. Best Pract Res Clin Rheumatol. 2014;28(1):5–15. https://doi.org/10.1016/j.berh.2014.01.004.
Sellam J, Berenbaum F. Is osteoarthritis a metabolic disease? Joint Bone Spine. 2013;80(6):568–73. https://doi.org/10.1016/j.jbspin.2013.09.007.
Ratneswaran A, LeBlanc EA, Walser E, et al. Peroxisome proliferator-activated receptor δ promotes the progression of posttraumatic osteoarthritis in a mouse model. Arthritis Rheumatol (Hoboken, NJ). 2015;67(2):454–64. https://doi.org/10.1002/art.38915.
Hulens M, Vansant G, Lysens R, et al. Exercise capacity in lean versus obese women. Scand J Med Sci Sports. 2001;11(5):305–9. https://doi.org/10.1034/j.1600-0838.2001.110509.x.
Vincent HK, Heywood K, Connelly J, et al. Obesity and weight loss in the treatment and prevention of osteoarthritis. PM&R. 2012;4(5):S59–67. https://doi.org/10.1016/j.pmrj.2012.01.005.
de Souza SAF, Faintuch J, Valezi AC, et al. Gait cinematic analysis in morbidly obese patients. Obes Surg. 2005;15(9):1238–42. https://doi.org/10.1381/096089205774512627.
Vincent H, Zdziarski L, Wasser J. Chronic pain management in the obese patient: a focused review of key challenges and potential exercise solutions. J Pain Res. 2015;8:63. https://doi.org/10.2147/JPR.S55360.
Courcoulas AP, Christian NJ, Belle SH, et al. Weight change and health outcomes at 3 years after bariatric surgery among individuals with severe obesity. JAMA. 2013;310:2416–25. https://doi.org/10.1001/jama.2013.280928.
King WC, Chen J-Y, Belle SH, et al. Change in pain and physical function following bariatric surgery for severe obesity. JAMA. 2016;315(13):1362–71. https://doi.org/10.1001/jama.2016.3010.
Abu-Abeid S, Wishnitzer N, Szold A, et al. The influence of surgically-induced weight loss on the knee joint. Obes Surg. 2005;15(10):1437–42. https://doi.org/10.1381/096089205774859281.
Hooper MM, Stellato TA, Hallowell PT, et al. Musculoskeletal findings in obese subjects before and after weight loss following bariatric surgery. Int J Obes. 2007;31(1):114–20. https://doi.org/10.1038/sj.ijo.0803349.
Bairdain S, Flint RS, Lien C, et al. A case report of the early results of laparoscopic bariatric surgery in six completely nonambulatory patients. Surg Obes Relat Dis. 2013;9(5):e74–6. https://doi.org/10.1016/j.soard.2013.06.007.
Williams GJ, Georgiou PA, Cocker DM, et al. The safety and efficacy of bariatric surgery for obese, wheelchair bound patients. Ann R Coll Surg Engl. 2014;96(5):373–6. https://doi.org/10.1308/003588414X13946184901083.
Lutrzykowski M. Bariatric surgery in morbidly obese patients in wheelchairs. Obes Surg. 2008;18(12):1647–8. https://doi.org/10.1007/s11695-008-9466-2.
Miyano G, Kalra M, Inge TH. Adolescent paraplegia, morbid obesity, and pickwickian syndrome: outcome of gastric bypass surgery. J Pediatr Surg. 2009;44(3):e41–4. https://doi.org/10.1016/j.jpedsurg.2008.12.014.
Alaedeen DI, Jasper J. Gastric bypass surgery in a paraplegic morbidly obese patient. Obes Surg. 2006;16(8):1107–8. https://doi.org/10.1381/096089206778026389.
Perreault JR, Geigle PR, Gorman PH, et al. Improvement in weight loss and ambulation outcomes after gastric sleeve surgery for a person with chronic motor-incomplete tetraplegia: clinical case report. Spinal Cord. 2016;54(9):750–3. https://doi.org/10.1038/sc.2016.22.
Brethauer SA, Kim J, Chaar M, et al. Standardized outcomes reporting in metabolic and bariatric surgery. Surg Obes Relat Dis. 2015;11(3):489–506. https://doi.org/10.1016/j.soard.2015.02.003.
Harris PA, Taylor R, Thielke R, et al. Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42(2):377–81. https://doi.org/10.1016/j.jbi.2008.08.010.
Harrell FE Jr. Hmisc: Harrell Miscellaneous. R package version 3.17-0. 2015. https://CRAN.R-project.org/package=Hmisc.
O’Rourke RW, Andrus J, Diggs BS, et al. Perioperative morbidity associated with bariatric surgery. Arch Surg. 2006;141(3):262–8. https://doi.org/10.1001/archsurg.141.3.262.
Livingston EH, Huerta S, Arthur D, et al. Male gender is a predictor of morbidity and age a predictor of mortality for patients undergoing gastric bypass surgery. Ann Surg. 2002;236(5):576–82. https://doi.org/10.1097/01.SLA.0000033321.22614.D6.
Still CD, Wood GC, Chu X, et al. Clinical factors associated with weight loss outcomes after Roux-en-Y gastric bypass surgery. Obesity (Silver Spring). 2014;22(3):888–94. https://doi.org/10.1002/oby.20529.
Stroh C, Michel N, Luderer D, et al. Risk of thrombosis and thromboembolic prophylaxis in obesity surgery: data analysis from the German Bariatric Surgery Registry. Obes Surg. 2016;26(11):2562–71. https://doi.org/10.1007/s11695-016-2182-4.
Cawley J, Sweeney MJ, Kurian M, et al. Predicting complications after bariatric surgery using obesity-related co-morbidities. Obes Surg. 2007;17(11):1451–6. https://doi.org/10.1007/s11695-008-9422-1.
Sekhon JS. Multivariate and propensity score matching software with automated balance optimization: the matching package for R. J Stat Softw. 2011;42(7). https://doi.org/10.18637/jss.v042.i07.
R Core Team. R: a language and environment for statistical computing. Vienna: R Foundation for Statistical Computing; 2015.
Santry HP, Lauderdale DS, Cagney KA, et al. Predictors of patient selection in bariatric surgery. Ann Surg. 2007;245(1):59–67. https://doi.org/10.1097/01.sla.0000232551.55712.b3.
King WC, Engel SG, Elder KA, et al. Walking capacity of bariatric surgery candidates. Surg Obes Relat Dis. 2012;8(1):48–59. https://doi.org/10.1016/j.soard.2011.07.003.
Miller GD, Nicklas BJ, You T, et al. Physical function improvements after laparoscopic Roux-en-Y gastric bypass surgery. Surg Obes Relat Dis. 2009;5(5):530–7. https://doi.org/10.1016/j.soard.2008.11.003.
Vincent HK, Ben-David K, Conrad BP, et al. Rapid changes in gait, musculoskeletal pain, and quality of life after bariatric surgery. Surg Obes Relat Dis. 2012;8(3):346–54. https://doi.org/10.1016/j.soard.2011.11.020.
Tompkins J, Bosch PR, Chenowith R, et al. Changes in functional walking distance and health-related quality of life after gastric bypass surgery. Phys Ther. 2008;88(8):928–35. https://doi.org/10.2522/ptj.20070296.
Josbeno DA, Jakicic JM, Hergenroeder A, et al. Physical activity and physical function changes in obese individuals after gastric bypass surgery. Surg Obes Relat Dis. 2010;6(4):361–6. https://doi.org/10.1016/j.soard.2008.08.003.
Vargas CB, Picolli F, Dani C, et al. Functioning of obese individuals in pre- and postoperative periods of bariatric surgery. Obes Surg. 2013;23(10):1590–5. https://doi.org/10.1007/s11695-013-0924-0.
Picone G, Mark Wilson R, Chou S-Y. Analysis of hospital length of stay and discharge destination using hazard functions with unmeasured heterogeneity. Health Econ. 2003;12(12):1021–34. https://doi.org/10.1002/hec.800.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
For this type of study, formal consent is not required
Informed Consent
This study does not require informed consent.
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Sharma, G., Nor-Hanipah, Z., Haskins, I.N. et al. Comparative Outcomes of Bariatric Surgery in Patients with Impaired Mobility and Ambulatory Population. OBES SURG 28, 2014–2024 (2018). https://doi.org/10.1007/s11695-018-3132-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3132-0