Abstract
Background
Considerable overlap in symptoms and disease comorbidity has been noted among medically unexplained and psychiatric conditions seen in the primary care setting, such as chronic fatigue syndrome, low back pain, irritable bowel syndrome, chronic tension headache, fibromyalgia, temporomandibular joint disorder, major depression, panic attacks, and posttraumatic stress disorder.
Objective
To examine interrelationships among these 9 conditions.
Design
Using data from a cross-sectional survey, we described associations and used latent class analysis to investigate complex interrelationships.
Participants
3,982 twins from the University of Washington Twin Registry.
Measurements
Twins self-reported a doctor’s diagnosis of the conditions.
Results
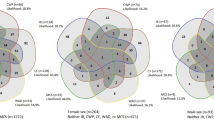
Comorbidity among these 9 conditions far exceeded chance expectations; 31 of 36 associations were significant. Latent class analysis yielded a 4-class solution. Class I (2% prevalence) had high frequencies of each of the 9 conditions. Class II (8% prevalence) had high proportions of multiple psychiatric diagnoses. Class III (17% prevalence) participants reported high proportions of depression, low back pain, and headache. Participants in class IV (73% prevalence) were generally healthy. Class I participants had the poorest markers of health status.
Conclusions
These results support theories suggesting that medically unexplained conditions share a common etiology. Understanding patterns of comorbidity can help clinicians care for challenging patients.
Similar content being viewed by others
References
Short D. Difficult patients. Br J Hosp Med. 1994;51:128–30.
Aaron LA, Herrell R, Ashton S, et al. Comorbid clinical conditions in chronic fatigue: a co-twin control study. J Gen Intern Med. 2001;16:24–31.
Wessely S, Nimnuan C, Sharpe M. Functional somatic syndromes: one or many? Lancet. 1999;354:936–9.
Torgersen S. The determination of twin zygosity by means of a mailed questionnaire. Acta Genet Med Gemellol (Roma). 1979;28:225–36.
McCutcheon AL. Latent Class Analysis. Beverly Hills, CA: Sage Publications; 1987.
Sullivan PF, Kessler RC, Kendler KS. Latent class analysis of lifetime depressive symptoms in the national comorbidity survey. Am J Psychiatry. 1998;155:1398–406.
Dempster AP, Laird NM, Rubin DB. Maximum likelihood from incomplete data via the EM algorithm. J R Stat Soc. 1977;39:1–38.
Williams LJ, Holahan PJ. Parsimony-based fit indices for multiple-indicator models: do they work? Struct Equation Model. 1994;1:161–89.
Clauw DJ, Schmidt M, Radulovic D, Singer A, Katz P, Bresette J. The relationship between fibromyalgia and interstitial cystitis. J Psychiatr Res. 1997;31:125–31.
Goertzel BN, Pennachin C, de Souza Coelho L, Gurbaxani B, Maloney EM, Jones JF. Combinations of single nucleotide polymorphisms in neuroendocrine effector and receptor genes predict chronic fatigue syndrome. Pharmacogenomics. 2006;7:475–83.
Kessler RC, Berglund P, Demler O, et al. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289:3095–105.
Linton SJ. A review of psychological risk factors in back and neck pain. Spine. 2000;25:1148–56.
Puca F, Genco S, Prudenzano MP, et al. Psychiatric comorbidity and psychosocial stress in patients with tension-type headache from headache centers in Italy. The Italian Collaborative Group for the Study of Psychopathological Factors in Primary Headaches. Cephalalgia. 1999;19:159–64.
Henningsen P, Zimmermann T, Sattel H. Medically unexplained physical symptoms, anxiety, and depression: a meta-analytic review. Psychosom Med. 2003;65:528–33.
Afari N, Buchwald D. Chronic fatigue syndrome: a review. Am J Psychiatry. 2003;160:221–36.
Andersson GB. Epidemiology of low back pain. Acta Orthop Scand Suppl. 1998;281:28–31.
Wolfe F, Ross K, Anderson J, Russell IJ, Hebert L. The prevalence and characteristics of fibromyalgia in the general population. Arthritis Rheum. 1995;38:19–28.
Kessler RC, McGonagle KA, Zhao S, et al. Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States: results from the National Comorbidity Survey. Arch Gen Psychiatry. 1994;51:8–19.
Kessler RC, Sonnega A, Bromet E, Hughes M, Nelson CB. Posttraumatic stress disorder in the National Comorbidity Survey. Arch Gen Psychiatry. 1995;52:1048–60.
Hahn BA, Saunders WB, Maier WC. Differences between individuals with self-reported irritable bowel syndrome (IBS) and IBS-like symptoms. Dig Dis Sci. 1997;42:2585–90.
Acknowledgements
This research was supported by National Institutes of Health awards 5 U19 AI038429 (Buchwald) and R55AR051524 (Afari). Dr. Schur is funded by a National Institutes of Health Career Development Award K23 DK070826.
Conflict of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schur, E.A., Afari, N., Furberg, H. et al. Feeling Bad in More Ways than One: Comorbidity Patterns of Medically Unexplained and Psychiatric Conditions. J GEN INTERN MED 22, 818–821 (2007). https://doi.org/10.1007/s11606-007-0140-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-007-0140-5