Abstract
Purpose
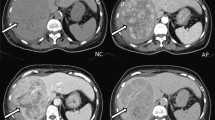
To evaluate the features of arterial enhancement pattern of focal nodular hyperplasia (FNH) and hepatocellular carcinoma (HCC) by triple-phase arterial magnetic resonance imaging (MRI).
Methods
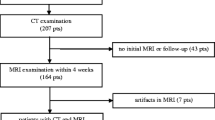
Data were retrospectively collected from 52 consecutive patients who underwent triple-phase arterial MRI using hepatocyte-specific contrast agents (Gd-EOB-DTPA) from January 2017 to October 2017, with a MR imaging diagnosis of HCC or FNH. The images were independently assessed by two blinded readers. Contrast enhancement ratio (CER) and liver-to-lesion contrast ratio (LLCR) were calculated. The lesions were classified visually and also based on the peak of LLCR into the following groups: (1) early arterial, (2) middle arterial and (3) late arterial. Data were eventually analysed using nonparametric tests.
Results
The CER analysis showed no significant difference between HCC and FNH patients (p > 0.05). LLCRFNH were significantly higher than LLCRHCC in the early arterial (p = 0.01), but not in the middle and late arterial phases (p = 0.20 and p = 0.82, respectively). LLCRHCC presented a meaningful increase from early to middle arterial phase (p = 0.009), whereas LLCRFNH showed a decrease from middle to late arterial phase (p = 0.004). Based on the peak of LLCR, 17 (55%) FNHs were classified into early, 11 (35%) in middle and only 3 (10%) in late arterial phase groups. Similarly, 14 (34%) HCCs were categorized into early, 13 (32%) in middle and 14 (33%) in late arterial phase groups. There was a good agreement between qualitative analysis and LLCR in 85% of cases.
Conclusion
The optimal visualization of FNH has been detected in early and middle arterial phases while HCC has been best observed during middle and late arterial phases.





Similar content being viewed by others
References
European Association for the Study of the Liver (EASL) (2016) EASL clinical practice guidelines on the management of benign liver tumours. J Hepatol 65:386–398. https://doi.org/10.1016/j.jhep.2016.04.001
European Association for the Study of the Liver. Electronic address: easloffice@easloffice.eu, European Association for the Study of the Liver (2018) EASL clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol 69:182–236. https://doi.org/10.1016/j.jhep.2018.03.019
Ippolito D, Inchingolo R, Grazioli L et al (2018) Recent advances in non-invasive magnetic resonance imaging assessment of hepatocellular carcinoma. World J Gastroenterol 24:2413–2426. https://doi.org/10.3748/wjg.v24.i23.2413
Inchingolo R, Faletti R, Grazioli L et al (2018) MR with Gd-EOB-DTPA in assessment of liver nodules in cirrhotic patients. World J Hepatol 10:462–473. https://doi.org/10.4254/wjh.v10.i7.462
Haradome H, Grazioli L, Tsunoo M et al (2010) Can MR fluoroscopic triggering technique and slow rate injection provide appropriate arterial phase images with reducing artifacts on gadoxetic acid-DTPA (Gd-EOB-DTPA)-enhanced hepatic MR imaging? J Magn Reson Imaging JMRI 32:334–340. https://doi.org/10.1002/jmri.22241
Kim YK, Lin W-C, Sung K et al (2017) Reducing artifacts during arterial phase of gadoxetate disodium-enhanced MR imaging: dilution method versus reduced injection rate. Radiology 283:429–437. https://doi.org/10.1148/radiol.2016160241
Yoon JH, Lee JM, Yu MH et al (2016) Triple arterial phase MR imaging with gadoxetic acid using a combination of contrast enhanced time robust angiography, keyhole, and viewsharing techniques and two-dimensional parallel imaging in comparison with conventional single arterial phase. Korean J Radiol 17:522–532. https://doi.org/10.3348/kjr.2016.17.4.522
Ikram NS, Yee J, Weinstein S et al (2017) Multiple arterial phase MRI of arterial hypervascular hepatic lesions: improved arterial phase capture and lesion enhancement. Abdom Radiol N Y 42:870–876. https://doi.org/10.1007/s00261-016-0948-8
Grazioli L, Faletti R, Frittoli B et al (2018) Evaluation of incidence of acute transient dyspnea and related artifacts after administration of gadoxetate disodium: a prospective observational study. Radiol Med (Torino). https://doi.org/10.1007/s11547-018-0927-y
Murakami T, Kim T, Takamura M et al (2001) Hypervascular hepatocellular carcinoma: detection with double arterial phase multi-detector row helical CT. Radiology 218:763–767. https://doi.org/10.1148/radiology.218.3.r01mr39763
Takahashi N, Yoshioka H, Yamaguchi M et al (2003) Accelerated dynamic MR imaging with a parallel imaging technique for hypervascular hepatocellular carcinomas: usefulness of a test bolus in examination and subtraction imaging. J Magn Reson Imaging JMRI 18:80–89. https://doi.org/10.1002/jmri.10319
Mori K, Yoshioka H, Takahashi N et al (2005) Triple arterial phase dynamic MRI with sensitivity encoding for hypervascular hepatocellular carcinoma: comparison of the diagnostic accuracy among the early, middle, late, and whole triple arterial phase imaging. AJR Am J Roentgenol 184:63–69. https://doi.org/10.2214/ajr.184.1.01840063
Hope TA, Saranathan M, Petkovska I et al (2013) Improvement of gadoxetate arterial phase capture with a high spatio-temporal resolution multiphase three-dimensional SPGR-Dixon sequence. J Magn Reson Imaging JMRI 38:938–945. https://doi.org/10.1002/jmri.24048
Rousseau C, Ronot M, Vilgrain V, Zins M (2016) Optimal visualization of focal nodular hyperplasia: quantitative and qualitative evaluation of single and multiphasic arterial phase acquisition at 1.5 T MR imaging. Abdom Radiol N Y 41:990–1000. https://doi.org/10.1007/s00261-015-0630-6
Neri E, Bali MA, Ba-Ssalamah A et al (2016) ESGAR consensus statement on liver MR imaging and clinical use of liver-specific contrast agents. Eur Radiol 26:921–931. https://doi.org/10.1007/s00330-015-3900-3
Vignaux O, Legmann P, Coste J et al (1999) Cirrhotic liver enhancement on dual-phase helical CT: comparison with noncirrhotic livers in 146 patients. AJR Am J Roentgenol 173:1193–1197. https://doi.org/10.2214/ajr.173.5.10541087
Hashimoto K, Murakami T, Dono K et al (2006) Assessment of the severity of liver disease and fibrotic change: the usefulness of hepatic CT perfusion imaging. Oncol Rep 16:677–683
Semela D, Dufour J-F (2004) Angiogenesis and hepatocellular carcinoma. J Hepatol 41:864–880. https://doi.org/10.1016/j.jhep.2004.09.006
Scoazec JY, Flejou JF, D’Errico A et al (1995) Focal nodular hyperplasia of the liver: composition of the extracellular matrix and expression of cell-cell and cell-matrix adhesion molecules. Hum Pathol 26:1114–1125
Fukukura Y, Nakashima O, Kusaba A et al (1998) Angioarchitecture and blood circulation in focal nodular hyperplasia of the liver. J Hepatol 29:470–475
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gatti, M., Calandri, M., Bergamasco, L. et al. Characterization of the arterial enhancement pattern of focal liver lesions by multiple arterial phase magnetic resonance imaging: comparison between hepatocellular carcinoma and focal nodular hyperplasia. Radiol med 125, 348–355 (2020). https://doi.org/10.1007/s11547-019-01127-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-019-01127-4