Abstract
Purpose
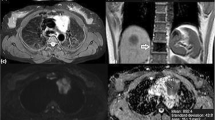
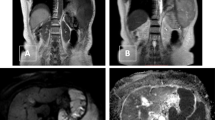
We retrospectively evaluated the role of diffusion-weighted imaging (DWI) with fat and background signal suppression in the differential diagnosis of benign and malignant lesions of the chest-mediastinum by calculating the mean apparent diffusion coefficient (ADC) values.
Materials and methods
Thirty-four patients with lung nodules/mediastinal masses underwent magnetic resonance (MR) imaging of the chest with conventional and DWI sequences. All patients had been previously studied with computed tomography (CT). After magnetic resonance (MR) imaging the patients underwent transthoracic CT-guided biopsy or mediastinoscopy. After the histopathological diagnosis had been obtained, the lesions were retrospectively divided into five groups: adenocarcinomas (n=16), squamous cell carcinomas (n=12), chronic pneumonias (n=2), malignant mediastinal tumours (n=2) and typical carcinoids (n=2). We compared ADC values in the different lesion groups using the Mann-Whitney U test.
Results
There were statistically significant differences (p<0.05) between ADC values of benign and malignant lesions. Using an ADC value of 1.25×10−3 mm2/s as a threshold, we were able to differentiate malignant from benign lesions with 91% diagnostic accuracy, 90% sensitivity, 100% specificity, 100% positive predictive value and 57% negative predictive value.
Conclusions
Short-tau inversion-recovery echo-planar imaging (STIR-EPI) sequences applied to the chest-mediastinum provided potentially useful images for the differential diagnosis of benign and malignant lesions.
Riassunto
Obiettivo
L’obiettivo del nostro lavoro è stato valutare retrospettivamente il ruolo delle sequenze pesate in diffusione con soppressione del segnale del grasso e del background nella diagnostica differenziale di lesioni benigne e maligne del distretto toraco-mediastinico, attraverso il calcolo dei valori medi del coefficiente di diffusione apparente (ADC).
Materiali e metodi
Trentaquattro pazienti portatori di noduli polmonari/masse mediastiniche, già sottoposti a tomografia computerizzata (TC) del torace sono stati sottoposti a risonanza magnetica (RM) del torace con sequenze pesate in diffusione. Dopo l’esame RM i pazienti sono stati sottoposti a biopsia transtoracica TC-guidata o a mediastinoscopia. Retrospettivamente, dopo aver ottenuto la diagnosi istopatologica, le lesioni sono state suddivise in cinque gruppi: adenocarcinomi (n=16), carcinomi squamocellulari (n=12), polmoniti croniche (n=2), tumori maligni mediastinici (n=2), carcinoidi tipici (n=2). Abbiamo confrontato i valori medi di ADC calcolati nei diversi gruppi utilizzando il test U di Mann-Whitney.
Risultati
Abbiamo ottenuto differenze statisticamente significative (p<0,05) tra i valori di ADC delle lesioni benigne e maligne. Utilizzando come valore soglia un valore di ADC di 1,25×10−3 mm2/s è stato possibile differenziare lesioni maligne dalle benigne con un’accuratezza diagnostica del 91%, sensibilità del 90%, specificità del 100%, valore predittivo positivo del 100% e valore predittivo negativo del 57%.
Conclusioni
Le sequenze short tau inversion recoveryecho-planar imaging (STIR-EPI) applicate al distretto toraco-mediastinico forniscono immagini potenzialmente utili per la diagnosi differenziale di lesioni benigne e maligne.
Similar content being viewed by others
References/Bibliografia
Carr HY, Purcell EM (1954) Effects of diffusion on free precession in nuclear magnetic resonance. Phys Rev 94:630–638
Guo Y, Cai YQ, Cai ZL et al (2002) Differentiation of clinically benign and malignant breast lesions using diffusion-weighted imaging. JMRI 16:172–178
Kinoshita T, Yashiro N, Ihara N et al (2002) Diffusion-weighted half-Fourier single-shot turbo spin echo imaging in breast tumors: differentiation of invasive ductal carcinoma from fibroadenoma. J Comput Assist Tomogr 26:1042–1046
Ichikawa T, Araki T (1999) Fast magnetic resonance imaging of liver. Eur J Radiol 29:186–210
Wang J, Takashima S, Takayama F et al (2001) Head and neck lesions: characterization with diffusionweighted echo-planar MR imaging. Radiology 220:621–630
Yoshino N, Yamada I, Ohbayashi N et al (2002) Salivary glands and lesions: evaluation of apparent diffusion coefficients with splitecho diffusionweighted MR imaging: initial results. Radiology 221:837–842
Sumi M, Takagi Y, Uetani M et al (2002) Diffusion-weighted echoplanar MR imaging of the salivary glands. AJR Am J Roentgenol 178:959–965
Sumi M, Sakihama N, Sumi T et al (2003) Discrimination of metastatic cervical lymph nodes with diffusionweighted MR imaging in patients with head and neck cancer. AJNR Am J Neuroradiol 24:1627–1634
Lyng H, Haraldseth O, Rofstad EK (2000) Measurement of cell density and necrotic fraction in human melanoma xenografts by diffusion weighted magnetic resonance imaging. Magn Reson Med 43:828–836
Stecco A, Romano G, Negru M et al (2009) Whole-body diffusionweighted magnetic resonance imaging in the staging of oncological patients: comparison with positron emission tomography computed tomography (PET-CT) in a pilot study. Radiol Med 114:1–17
Takahara T, Imai Y, Yamashita T et al (2004) Diffusion weighted whole body imaging with background body signal suppression (DWIBS): technical improvement using free breathing, STIR and high resolution 3D display. Radiation Medicine 22:275–282
Matoba M, Tonami H, Kondou T et al (2007) Lung carcinoma: diffusionweighted MR imaging-preliminary evaluation with apparent diffusion coefficient. Radiology 243:570–577
Mori T, Nomori H, Ikeda K et al (2008) Diffusion-weighted magnetic resonance imaging for diagnosis malignant pulmonary nodules/masses:comparison with positron emission tomography. J Thorac Oncol 3:358–364
Satoh S, Kitazume Y, Ohdama S et al (2008) Can malignant and benign pulmonary nodules be differentiated with diffusion-weighted MRI? AJR Am J Roentgenol 191:464–470
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tondo, F., Saponaro, A., Stecco, A. et al. Role of diffusion-weighted imaging in the differential diagnosis of benign and malignant lesions of the chest-mediastinum. Radiol med 116, 720–733 (2011). https://doi.org/10.1007/s11547-011-0629-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-011-0629-1