Abstract
Racial residential segregation is considered a fundamental cause of racial health disparities, with housing discrimination as a critical driver of residential segregation. Despite this link, racial discrimination in housing is far less studied than segregation in the population health literature. As a result, we know little about how discrimination in housing is linked to health beyond its connection to segregation. Furthermore, we need to understand how health impacts differ across different types of housing discrimination. This review aims to assess the state of the population health literature on the conceptualization, measurement, and health implications of housing discrimination. We used PRISMA guidelines for scoping reviews and presented the data on 32 articles that met our inclusion criteria published before January 1, 2022. Nearly half of the articles do not define housing discrimination explicitly. Additionally, there is considerable variation in how housing discrimination is operationalized across studies. Compared to studies using administrative data for housing discrimination exposures, studies using survey data were more likely to report a detrimental association with health outcomes. Synthesizing and comparing the results of these studies helps bridge methodological approaches to this research. Our review helps inform the debate on how racism impacts population health. Given the changing nature of racial discrimination over time and place, we discuss how population health researchers can approach studying various forms of housing discrimination.
Similar content being viewed by others
Introduction
A growing body of population health research recognizes the role of institutional racism in racial health inequities. Early scholarship in this area focused on racial residential segregation. Studying segregation as a form of racism was advantageous because health inequalities often map onto geographic patterns. Census data availability also makes segregation measures readily accessible. This large body of research provides evidence that segregation is a “fundamental cause of racial health disparities” [1, 2], because it influences multiple disease outcomes [3,4,5,6], impacts numerous risk factors [7,8,9], shapes flexible resources, and is reproduced over time [10, 11]. While it is clear that racial residential segregation is associated with multiple health and healthcare inequities, measures of segregation fail to identify specific policies or practices that produce and maintain these inequities.
More recently, population health researchers have highlighted the need to go beyond studying segregation to examining racialized institutional practices and their health implications. Racial residential segregation, the argument goes, is a consequence of racism and should not be considered a proxy for racism itself [12, 13]. Furthermore, the hyperfocus on segregation takes our attention away from developing interventions to improve health. The hypothetical solution goes as follows: if the way people are arranged in space (i.e., segregation) causes poor health, we can rearrange space and improve health. This line of reasoning encourages policies that seek to move people around without addressing the underlying factors determining where people live [14]. For example, several social experiments seeking to move public housing residents to “opportunity” did not change why some neighborhoods are “healthier” than others [15,16,17]. Unequal access to health-promoting resources remained intact even while families move away from places deprived of those resources. Thus, while segregation is an important indicator for understanding place-based racism, public health scholarship would be served by exploring the mechanisms by which segregation—and its underlying geographic inequality—is maintained.
Segregation is maintained by a dynamic system whereby prejudice, wealth inequality, neighborhood knowledge, and racialized housing discrimination interact with and exacerbate one another [10, 11, 18]. Among these factors, housing discrimination deserves attention as a driver of population health inequities because it refers to institutional actions that can be intervened on and that have the power to shape the distribution of harmful exposures and health-promoting resources [19].
Although housing discrimination is a crucial driver of residential segregation, it is far less studied in population health research. For example, a simple PubMed search on December 31, 2021, of “racial residential segregation” returns 149 results, “institutional racism” returns 222 results, while “housing discrimination” yields only 24 results. While this body of evidence is small in the fields of public and population health, the legacy of racialized housing discrimination in the USA is vast, and its connection to health is well documented. In 1899, W.E.B. Du Bois analyzed the relationship between housing discrimination and the health of Black people in Philadelphia [20]. He wrote,
“Negros live in unsanitary dwellings […] partly on account of the difficulty of securing decent houses by reason of race prejudice […] In very many cases, landlords refuse to repair and refit for Negro tenants because they know that there are few dwellings which Negros can hire, and they will not, therefore, be apt to leave a fair house on account of damp walls or poor sewer connections” [20].
Constrained housing markets, discriminatory practices, and unhealthy housing conditions continued to impact the health of Black communities throughout the twentieth century. As a result, housing discrimination was a central focus of the urban rebellions and the Civil Rights Movement of the 1960s [21,22,23]. Black communities and organizations demanded institutional changes to undo the government-sponsored uneven development in regions across the country. While the Fair Housing Act of 1968 outlawed racial discrimination in housing, it was limited in its enforceability. Therefore, since its passing, several studies have documented that racial discrimination in housing is still prevalent. Studies have also shown an intimate connection between housing discrimination and racial and economic residential segregation [24,25,26,27,28].
Within the context of this history, the study of racialized housing discrimination and health extends the research on segregation and health while also responding to the calls to consider institutional accountability in racism and health research. In fact, there has been an increase in the use of historical (e.g., Home Owner’s Loan Corporation [HOLC] security maps) and contemporary (e.g., Home Mortgage Disclosure Act [HMDA]) administrative data to measure racialized housing discrimination. However, there are two concerns regarding this literature.
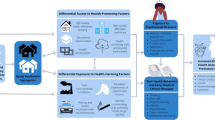
First, there is no consensus on how this body of work defines and measures housing discrimination. Currently, the Fair Housing Act of 1968 has a broad definition of housing discrimination which includes differential treatment while “renting or buying a home, getting a mortgage, seeking housing assistance, or engaging in other housing-related activities” [29]. The US Department of Housing and Urban Development (HUD) provides a list of activities that fall under this definition ranging from steering to delaying repairs, unjust evictions, and blockbusting [30]. We build on the HUD definition to specify racialized housing discrimination as differential treatment at any stage in the housing continuum—from acquisition, to remaining and maintaining, to selling or moving out—based on the race of the individual, family, or residents in a community. At each stage in the housing continuum, people engage with a range of individuals and institutions that can racially discriminate. Table 1 displays a non-exhaustive list of potential discrimination exposures and highlights which exposures public and population health scholars have explored.
Second, there are inconsistencies in the findings regarding how housing discrimination impacts health. For example, some studies of mortgage discrimination using the HMDA database show a protective effect on health; others show a detrimental impact on health, and still others find no association. We address these concerns by answering three questions: (1) How is racialized housing discrimination defined in the population health literature? (2) How is racialized housing discrimination measured? (3) What are the effects of racialized housing discrimination on health outcomes and health disparities? Then, we explain why the evidence is sometimes contradictory to our expectations. Finally, we inform the field of promising methodological and conceptual considerations that can be used to understand this relationship further.
Methods
Search Strategy
We conducted this scoping review using the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) guidelines [31]. We searched all available literature until December 31, 2021. We searched peer-reviewed and grey literature in databases that publish scholarship on discrimination and health. These include PubMed, CINAHL, PsychINFO, Sociological Abstracts, Social Welfare Abstracts, Academic Search Premier, ERIC, and ProQuest Theses and Dissertations. For grey literature, we searched Grey Literature Report and EMBASE. We also manually searched the reference lists of relevant articles to find additional relevant studies.
We developed a list of exposure terms after reviewing the housing discrimination scholarship. We found that housing discrimination is not always explicitly mentioned, so we included several terms associated with housing discrimination. The terms included mortgage discrimination, redlining, housing discrimination, rental discrimination, subprime lending, reverse redlining, predatory inclusion, and major discrimination. We did not include terms related to housing equity, such as "social housing," to focus on the impact of housing discrimination as a form of institutional racism.
We were interested in all mental and physical health outcomes and health inequalities. Our outcome search terms included health, mental health, health disparity, depression, disease, cancer, cardiovascular disease, diabetes, obesity, psychological distress, stress, self-rated health, BMI, overweight, chronic illness, pregnancy, birth outcomes, birth weight, preterm birth, asthma, “health outcomes,” “health disparities,” health effects,” and “health impacts.” In PubMed, we did not use health-related search terms because the database primarily focuses on health, healthcare, and biomedical outcomes. In PubMed, we only searched housing discrimination terms noted above. Due to changes in PubMed's interface, we used the PubMed import function in DistillerSR.
Inclusion and Exclusion Criteria
To be included in the study, articles had to quantitatively assess the relationship between exposure to racialized housing discrimination and health outcomes at the individual or neighborhood levels. To attend to racial health equity, we focus our analysis on members of minoritized racial groups as the targets of racialized housing discrimination, though we report the findings for all populations. Though racial and ethnic discrimination in housing is a global phenomenon, we limited our study to English language articles in the USA. We acknowledge that global scholarship on housing discrimination might reveal important associations with health outcomes as well as highlight potential interventions. However, the unique history of racialized housing policies and practices likely shapes processes in the USA differently from other countries. For dissertations and theses that were subsequently peer-reviewed and published, we included the published manuscripts and excluded the dissertation.
In the full-text review, we excluded articles that did not specify the effect of housing discrimination (i.e., if housing discrimination was not separated from other items on a larger discrimination scale). We also excluded articles that focused primarily on health behaviors if they did not explicitly measure at least one health outcome. For example, when deciding whether to include drug use-related outcomes, we excluded those that measured “any” or “lifetime” drug use (which could pathologize recreational drug use) and included those that measured problematic drug use, drug dependence, or drug use disorders [32, 33].
Study Selection and Data Extraction
Once all identified records were compiled and deduplicated, all authors reviewed titles and abstracts to determine eligibility using the criteria listed above. After the title (n = 1710) and abstract (n = 314) exclusions, all four authors read a randomly selected sample of full-text articles (n = 71) to verify the inclusion criteria. At this stage, all four authors extracted relevant data from the articles that met the inclusion criteria. Articles that did not meet the criteria were excluded (n = 42). At least two authors read each article. RIC performed a quality check on all data extraction responses to ensure accuracy. All conflicts were resolved through discussion. The weighted overall kappa statistic was 0.88.
Reference review, data extraction, and analysis were conducted using DistillerSR web-based software by Evidence Partners Ottawa, Ontario, Canada.,
Results
Deriving the Sample
As shown in Fig. 1, the search retrieved 2094 unique publications. After excluding ineligible (n = 2023) studies through title and abstract screening, we reviewed 71 full articles. After a full-text review, 29 publications were included in the preliminary sample. We then manually searched the references of the included articles and found three additional relevant articles, bringing our final sample to 32.
Characteristics of Studies
Table 2 summarizes the key characteristics of the sample overall and by the type of housing discrimination measure (self-report or administrative). Overall, most studies used a cross-sectional design, and the levels of analysis varied. Thirty-six percent of studies used individual-level analysis, while 45% used multilevel analysis where the housing discrimination exposure was at the neighborhood level. The remaining six studies used an ecologic design. Samples were drawn from population-based settings, ranging from 99 to 651,000 individuals.
Regarding sample demographics, most of the studies used adult samples. Only one study had a sample of adolescents [13]. Two studies did not specify the age group of their samples. Concerning gender, 14 of the studies (45.2%) only included women in their samples. The remaining 18 (58.1%) studies included all genders. Over two-thirds (71%) of the studies used multi-racial and multi-ethnic samples, but considerable variability exists. For example, 6 (19.4%) restricted analyses to Black and white participants, and 5 (16.1%) studies used a sample comprising Black, Latinx, and white participants. Two studies had a sample of Black, Latinx, white, and “other” participants. Another 8 (25.8%) did not specify the racial/ethnic categorization of the sample. Among the studies with homogenous racial/ethnic samples, 8 (25.8%) restricted the sample to Black participants, and 1 used a Chinese American sample [34].
Concerning health outcomes examined in the sample studies, 42% of the studies examined a mental health outcome, including psychological distress, general mental health, depressive symptoms, and anxiety. One-third (32.3%) of the studies examined birth outcomes, including preterm birth, low birth weight, small for gestational age, and infant mortality. Another third of the studies (29.0%) focused on cancer, and another third (29.0%) examined general health, such as self-rated health and physical functioning. About one-fifth of the studies (22.6%) examined mortality. The remaining studies examined cardiovascular health (n = 2), lead poisoning (n = 1), and respiratory illness (n = 1).
Of the 11 studies using self-reported measures of discrimination, the majority were published before 2020 (90.9%), used a national US-based sample (63.6%), and employed individual level analysis (72.7%). In contrast, of the 21 studies using administrative measures of discrimination, the majority were published between 2020 and 2021 (52.4%), were set in a specific US state or municipality (85.7%) and applied multilevel analysis (57.1%). The racial/ethnic composition of samples also varied. For example, while 45.5% of studies using self-reported housing discrimination measures were restricted to a Black/African American sample, 42.9% of studies using administrative discrimination measures did not specify the racial/ethnic composition of the sample.
Conceptualization
About 69% of the sample studies did not include a specific definition of housing discrimination. There is a notable difference in studies examining housing discrimination at the individual and neighborhood levels. At the individual level (i.e., experiences of housing discrimination), studies overwhelmingly (80%) did not explicitly define housing discrimination. Those that did, defined discrimination broadly as “unfair treatment” in housing markets. Only one study, conducted by Osypuk et al. [35] names “white individuals” as the main perpetrators of housing discrimination.
At the neighborhood level, redlining was the most common conceptualization of housing discrimination. Most of the studies that examined “redlining”—historical and contemporary—explicitly defined the term in the article. However, there is not a universal conceptualization of redlining across the studies. Some defined redlining in terms of aggregated racial bias. For example, Mendez defined redlining as “the illegal practice of banks and financial institutions systematically denying mortgage loans, or providing loans with worse terms, to individuals and groups within an area based on race or socioeconomic status” [36]. While others define redlining as the area-based discrimination. For example, Beyer and colleagues defined redlining as “the process of systematically denying mortgages based on location, where these locations are often defined by a predominant race or socioeconomic group” [37]. Still, others included both area- and group-based mortgage discrimination in their definitions. For example, in a different paper, Mendez defined redlining as the “institutional practice in which banks and other financial institutions deny loans to communities and individuals based on race” [38].
Beyer and colleagues differentiate redlining from racial bias in mortgage lending [37]. According to them, redlining is area-based exclusion regardless of the applicant’s race, and “racial bias in mortgage lending is conceived as the denial of mortgages to Black applicants, regardless of the neighborhood in which they intend, through a mortgage application, to reside” [37].
In another study, Sewell uses different terminology to address redlining and mortgage bias. Sewell conceptualizes both as access discrimination which they define as “inequalities in the ability to get an application funded in the primary mortgage market” [13]. Sewell was also the only study to conceptualize regulation discrimination which refers to “inclusionary processes [consisting of] inequalities in the federal oversight of the applications that are funded in the primary or secondary markets” [13].
All studies except for two defined redlining as the discriminatory provision of mortgage loans. In contrast, Nardone defined redlining as “the practice of categorizing perceived neighborhood mortgage investment risk” [39, 40] (Table 3).
Measurement
Of the 11 studies that examined individual-level experiences of housing discrimination, five relied on data from the Black Women’s Health Study (BWHS) [41,42,43,44,45], one uses data from the Survey of the Health of Wisconsin (SHOW) [46] and one used data from Coronary Artery Risk Development in Young Adults (CARDIA). BWHS and SHOW use the Major Experiences of Discrimination Scale [47], and CARDIA uses the Experiences of Discrimination Scale [48] to measure housing discrimination. Each study used a similar approach to isolate housing discrimination. Participants were considered exposed if they responded that they ever experienced discrimination while trying to obtain housing or remain in their neighborhoods. None of these studies analyzed the frequency of housing discrimination experiences. Furthermore, none of these studies indicate when individuals experienced housing discrimination.
The remaining four studies used three other data sources to measure housing discrimination. Yang and colleagues [49, 50] used the Public Health Management Corporation’s (PHMC) Southeastern Pennsylvania Household Health Survey. This survey asked whether respondents experienced discrimination were “prevented from doing something, or made to feel inferior” in the housing market. Osypuk and colleagues used data from the Moving to Opportunity experiment [35]. This survey used two items to determine if people were exposed to housing discrimination. The first question asked if they were told that they could not rent a particular home. The second asked why they could not rent the home: race, children, source of income, and socioeconomic background. Finally, Rooks et al. [51] used multiple survey items to gauge whether respondents experienced any unfair treatment in housing. However, the authors are not explicit about the number of survey items.
A substantial number of studies examining neighborhood-level housing discrimination used the Home Mortgage Disclosure Act (HMDA) database to develop redlining and mortgage lending discrimination indices [13, 34, 36,37,38, 52,53,54,55,56]. The HMDA database provides information on applicant race, sex, and income as well as loan amount, location, and loan decision. These data allow scholars to determine where and to what extent there is a systematic bias in mortgage lending decisions. Scholars differed in how they operationalized redlining. Some studies operationalized a neighborhood as “redlined” if the odds of loan denial in a neighborhood were higher for racial minority applicants than white applicants. In comparison, others considered a neighborhood redlined if the odds of loan denial within the neighborhood were higher relative to other neighborhoods, regardless of the applicant’s race.
Beyer et al. and Sewell [13] examine both forms of discrimination (i.e., area-based and applicant-based) using different measures. For area-based discrimination, Beyer and colleagues use areal spatial filters to determine neighborhoods and logistic regression to calculate the odds of loan denial. Using theoretically meaningful neighborhood clusters, Sewell compares the denials rate within each area to the city median. None of the papers operationalizing “redlining” as the area-based likelihood of loan denial differentiate between neighborhoods with different racial compositions. In other words, neighborhoods are considered redlined if they have a relatively high denial rate regardless of whether they are all white or all Black neighborhoods.
Two studies, Sewell [13] and Lynch et al. [56], measured inclusionary forms of discrimination using HMDA data. Sewell calculated two variables to estimate regulation discrimination: area-based and applicant-based. For the area-based variable, they compared the proportion of private loans in each neighborhood cluster to the median proportion of private loans across all clusters. Neighborhood clusters with rates higher than the city median were classified as high, and those with rates lower than the city median were low. For the applicant-based variable, Sewell calculated risk ratios for each neighborhood cluster that compares the risk of obtaining a private loan for minority applicants to the risk of obtaining such a loan for the entire neighborhood cluster. These risk ratios were then compared to the city median risk ratios. Neighborhood clusters above the median were considered to have high “racialized credit privateness.”
Lynch and colleagues [56] calculated rate spread to classify census tracts as being targeted for high-cost loans. Rate spread is the difference between the individual loan rate that was charged and the Average Prime Offer Rate (APOR) for that day. Census tracts in which more than 15% (median) of originated loans had rate spreads > 1.5 were classified as having high-cost loans.
Studies that examined historic redlining used the digitized Home Owners’ Loan Corporation (HOLC) security maps [57]. Historically “redlined” neighborhoods were labeled “Hazardous” or given a D grade on the HOLC maps. Most studies geocoded the HOLC maps and overlayed them with 2010 census maps. As a result, census tracts (or zip codes) were (1) fully captured within one HOLC designation, (2) partially captured in more than one HOLC designation, or (3) not captured at all by the HOLC maps. One study [56] used weighted scores to account for the neighborhoods with more than one HOLC designation. In this study, neighborhoods covered by redlined or “D” space were given a score of 4, while those with a coverage of 50% D grade and 50% C grade were given a score of 3.5 (Table 4).
Health Effects
Findings by Housing Discrimination Exposures
Experiences of housing discrimination. Among the 11 studies that examined experiences of housing discrimination at the individual level, 54.5% (n = 6) reported positive (detrimental) associations, 18% (n = 2) had mixed findings, and 27.3% (n = 3) reported null results. Three of the six studies that reported statistically significant findings were conditional on a third variable. One study [41] found that for women with less than 12 years of education, experiencing housing discrimination was associated with preterm birth. Another [51] found an interaction between SES and race such that housing discrimination was associated with lower life satisfaction among low-SES Black women compared to middle-SES white women. Another study [58] reported that the relationship between housing discrimination and cardiovascular health (CVH) was conditional on race. White women who reported housing discrimination (compared to those who did not) had diminished CVH.
Other studies found perceived housing discrimination to be directly detrimental to health. Osypuk and colleagues [35] reported that perceived housing discrimination was associated with higher psychological stress and slightly higher major depressive disorder among adult heads of households. Additionally, Yang and Park [49] found that perceived housing discrimination is associated with poor self-reported health (SRH), increased stress, and increased mental illness in a sample of Philadelphia adults. Finally, housing discrimination was associated with increased uterine leiomyomata [42] in a national sample of Black women.
The studies that report mixed findings examined the relationship between experiences of housing discrimination and multiple health outcomes and reported inconsistent associations. For example, Yang [50] found that neighborhood context conditions the relationship between housing discrimination and health and that different neighborhood conditions (e.g., economic conditions vs. racial composition) change the relationship. In neighborhoods with average housing values, residents who perceived discrimination are more likely to report poor SRH. In neighborhoods with higher concentrations of Black residents and single-parent households, residents who perceived discrimination are less likely to report poor SRH, but only marginally.
Historical Redlining
Among the ten studies that examined the relationship between historical redlining and present-day health outcomes, seven found that residence in historically redlined areas was associated with worse health outcomes [56]. Three of the ten used multilevel designs with geocoded birth record data to examine the relationship between current residence in a historically redlined area and adverse birth outcomes. Krieger et al. [59] found that compared to women living in areas graded A or “Best,” women living in those graded B, C, and D, had higher odds of delivering preterm. Hollenbach [61] also examined birth data but compared areas graded A or B to those graded C or D. They found lower grades were associated with higher odds of preterm birth. In the third study examining birth outcomes, Nardone et al. [39] had mixed results. The authors found a different relationship between HOLC grades and birth outcomes in the two California regions under study. In the San Francisco/Oakland metropolitan area, residence in grade C areas was associated with worse birth outcomes than in B-graded areas. However, compared to a residence in a C-graded census tract, living in D-graded census tracts was not associated with adverse birth outcomes. These patterns did not hold in Los Angeles. Surprisingly, residence in D-graded areas (compared to C) was associated with slightly better birth outcomes.
A multilevel analysis [64] of historical redlining and cancer reported mixed results. One study found that residing in a redlined census tract was not associated with breast cancer or cervical cancer risk. The same study found that living in a historically redlined census tract was associated with a higher risk of being diagnosed with lung cancer at a later stage.
The final multilevel study with historical redlining as the primary exposure, led by Mujahid, found that Black residents in D-rated neighborhoods had lower cardiovascular health (CVH) scores than those in A-rated neighborhoods. This association was not present for other racialized groups [40].
The remaining studies examining historical redlining used ecologic designs and found positive associations with aggregated health outcomes, including prevalence of poor mental health [56], poor physical health [56], infant mortality [56], COVID mortality [62], asthma [60], and heat-related emergency department visits [63], and racial disparities in heart disease, diabetes, and cancer [65].
Contemporary Residential Redlining
Overall, the evidence on the health implications of neighborhood-based mortgage exclusion is mixed. Two studies, one examining colorectal cancer mortality [55] and the other [13], lead poisoning and general health, found null results. One study demonstrated that area-based mortgage exclusion was associated with increased all-cause mortality among Black women with breast cancer but a slight decrease in breast cancer-specific mortality risk [37]. Another study [52] found redlining was associated with small increases in cancer mortality disparities. This association was positive for men and null for women.
Racial Bias in Mortgage Lending
The studies examining the health implications of systematic racial bias in mortgage lending were mixed. Some of these studies [34, 36, 38, 53, 54] use the terminology of “redlining,” but the methodology is consistent with mortgage discrimination studies.
Three studies reported null results. These studies examined various health outcomes, including general health status [13], stress [54], and infant birth weight [38]. Among those with statistically significant findings, the direction of the association was mixed. Three studies [37, 53, 55] reported that living in an area characterized by higher racial bias in mortgage lending is associated with worse health outcomes. Zhou [55] found that racial discrimination in mortgage lending was associated with a greater hazard rate for Black adults with colorectal cancer. There was no association for white adults. Racial bias in mortgage lending was also associated with poorer colorectal cancer survival for Black women compared to the overall sample. In a different study, the same authors [37] found that racial bias in lending increased the hazard rate by 49% as binary categorization. Finally, studying only Black women, Matoba et al. [53] found that residence in an area with racial discrimination in mortgage lending was associated with a slight increase in odds of preterm birth compared to women in areas without systematic bias.
Contrary to expectations, three studies found that living in a neighborhood with racial bias in mortgage lending has a protective effect on health. Gee [34] reported that residence in neighborhoods with higher odds of loan denials for Chinese applicants was associated with better self-reported health and mental health among Chinese adults. Mendez [36] found that residence in an area characterized by mortgage discrimination was associated with decreased risk of preterm birth for Black, Latinx, and white women. Finally, Collin et al. [66] found that residence in census tracts with high lending bias is associated with a 14% decrease in cancer mortality adjusting for age and cancer stage.
Inclusionary Discrimination
Only two studies examined inclusionary housing discrimination. Sewell [13] found mixed results. Racialized credit privateness was not associated with general health status or lead poisoning. However, the rate of lead poisoning was substantially higher in neighborhoods with a disproportionately high number of federally regulated loans. Lynch and colleagues [56] combined their measure of inclusionary discrimination (rate spread) with another indicator of discrimination to create a measure of contemporary lending discrimination. Therefore, they did not report the association between rate spread, alone, and health outcomes. However, they found that compared to residents in tracts with no present-day discrimination, those living in tracts with current discrimination (high-cost loans or lack of homeownership) had worse physical and mental health.
Discussion
In this review, we assessed the state of the scholarship examining the relationship between racialized housing discrimination and population health outcomes. First, we determined how this body of work defines housing discrimination. Second, we assessed the methodological tools and strategies used to measure housing discrimination. Finally, we synthesized the findings on the relationship between housing discrimination and health outcomes. Our results reveal limited literature on how racialized housing discrimination impacts health, as only 32 studies across 21 years met the inclusion criteria. While more research is needed, the studies included in the review suggest that this is a promising area of research to better understand and potentially intervene on this form of racism.
Defining Housing Discrimination
About half (47.2%) of the studies did not offer a conceptual definition of housing discrimination. Those that did tend to have housing discrimination as the sole exposure instead of in conjunction with other types of discrimination. The different conceptual definitions across studies have important implications for understanding how this pervasive form of discrimination impacts health and what can be done about it. Epidemiologically, specific conceptual definitions are needed to estimate causal relationships. More importantly, clear definitions are required to develop effective interventions to address discrimination from a public policy standpoint. Population health scholars might benefit from defining the parameters of various forms of housing discrimination to better capture complexity.
Among the studies that defined housing discrimination, there were inconsistencies in the linkage between conceptual and operational definitions. This was especially the case for the studies of contemporary “redlining.” In general, redlining refers to a system of marking neighborhoods as risky—or hazardous—for lenders, mainly based on the race of occupants in the area. The studies in this review raise two concerns related to conceptual and operational definitions. First, most studies define redlining as “neighborhood loan denials” rather than a “labeling of neighborhood risk.” This conceptual definition is problematic because systematic loan denials are only one consequence of the racial marking of neighborhoods. Thus, scholars operating from this definition will unintentionally ignore other consequences of redlining, such as predatory inclusion [67]. Racialized lending patterns included both disinvestment (i.e., systematic neighborhood loan denials), and exploitative investment [68]. There is historical evidence that the marking of an area as “risky” may result in the practice of economic exploitation [68]. For example, these neighborhoods might be targeted for high-interest (i.e., subprime) loans. This complicates how scholars may understand how this type of discrimination is related to health. Only one study reviewed here differentiated—in conceptualization and operationalization—between exclusionary and inclusionary discrimination in the mortgage market and found that each type related to health outcomes differently [13].
This imprecise definition of redlining also leads to the second issue, which centers on the question: which neighborhoods are being redlined? Standard measures of contemporary redlining do not indicate the extent to which racial composition is related to neighborhood loan denials or neighborhood high-cost loans. In other words, we do not know from these studies if neighborhoods with relatively higher mortgage denial rates are predominantly Black or another racialized group. The underlying assumption that neighborhoods with high rates of loan denial are non-white neighborhoods is supported by a recent study showing that neighborhoods with higher proportions of white residents have higher rates of loan approvals [69]. Nevertheless, nuances in the racialized housing market warrant more granular racial disaggregation. Thus, excluding the neighborhood’s racial composition from the measure may obscure relevant associations in these neighborhoods. The lack of racial variation in the redlining indices may explain why the results were null for these measures.
Given these challenges, we argue for a more specific definition of redlining that emphasizes the racial marking of space. Scholars, using this definition, can then explore various consequences of racial marking and their relationship to health.
Methodological Considerations: Limits of Current Measures
All studies in this review likely underestimated housing discrimination. More than a third of the studies examined self-reported experiences of housing discrimination and used one item of a larger discrimination scale. Though the prevalence of housing discrimination is high, particularly among Black women, it is unclear whether one item is sufficient to capture the complexity of housing discrimination. Research on eviction shows that multiple survey items could capture experiences of displacement better than one question because people often interpret “eviction” in a narrow way [70]. The same argument can be made for the term “housing discrimination.” In a 2002 study examining public knowledge about housing discrimination laws, respondents were asked to identify behavior that qualifies as housing discrimination in a set of eight hypothetical scenarios [71]. Less than 15% of the sample could correctly identify all eight, and those that could were more likely to have higher incomes. This suggests that the public is unaware of all the activities under the umbrella of housing discrimination. Therefore, studies asking about experiences of housing discrimination only using one item may unintentionally ignore a wide range of activities that should be considered.
The studies using administrative data to measure neighborhood-level housing discrimination also suffer from using single measures. This is because there are limitations in the available data sources to measure housing discrimination. About half of these studies used data from the HMDA database. While it is useful for this type of research, one of HMDA’s major limitations includes missing data—which is often missing not at random. In one of the studies reviewed here, Zhou and colleagues note that substantial data was missing in their Wisconsin-based study. They explain, “[o]f a total of 396,032 total applications for the purchase of an owner-occupied home, approximately 40% of applications were missing data on at least one of these variables; 32% of applications were missing approval/denial status” [55]. Thus, the validity of the measures using the HMDA database depends on the extent to which banks and other mortgage providers fully report their lending practices. So, while these data are “unobtrusive” they are not unbiased or objective. Research has shown that HMDA data on applicant race, for example, is disproportionately missing for loan denials in jurisdictions with more households of color; thus, housing discrimination prevalence in these studies may also be underestimated [72].
The remaining neighborhood-level studies in this review used historical “redlining” maps as the primary data source. These studies used slightly different methods to assign HOLC grades to modern-day spatial units of analysis ranging from census tracts to zip codes. However, the extent to which the HOLC grades are valid historical exposures is unclear. Studies suggest that the color-coding of neighborhoods as risky led to discriminatory lending practices, divestment, and the associated urban health sequelae. However, urban scholars have challenged several of these assumptions with detailed historical analysis. First, the assumption that ideas about race were systematically embedded in the map-making process is challenged by Michney’s historical work demonstrating that the on-the-ground fieldwork linking race and mortgage security risk was “idiosyncratic, arbitrary, and variable” [73]. Second, the assumption that HOLC used the maps to deny loans to Black residents is challenged by Fishback [74] who reminds us that HOLC did loan to Black people in relative proportion to their population size. This was because the HOLC program was devised as a refinancing program during the Great Depression. In fact, 97% of these refinance loans were already closed before the HOLC security maps were complete [73]. Taken together, these scholars argue that these maps were, at best, a proxy for previous exclusionary practices rather than a guide for future lending [68, 75]. Third, the assumption that neighborhoods with different color-coded grades were treated differently by lending institutions is partially challenged by Hillier [68, 76]. She found that, in the case of Philadelphia, HOLC grades were not linked to disinvestment as commonly thought, but rather to differences in interest rates. Mortgages in redlined areas had higher interest rates suggesting a form of inclusionary discrimination.
At the same time, the categorization or “spatial marking’ [77] of neighborhoods was not without consequences. There is a consensus among these scholars that HOLC and the FHA used their lending and insurance products in ways that reinforced segregation [74, 78, 79]. For example, Faber’s extensive historical research shows that while HOLC may not have contributed to large-scale disinvestment as previously thought, the cities that the organization mapped became more segregated than those that were not [77, 78]. As we discussed earlier, deeply entrenched segregation has health implications. These complexities highlight the limitations of using one data source—HOLC security maps—to explain structural health inequities. To understand the mechanisms by which historical discriminatory practices and policies may impact present-day patterns in health, population health scholars might benefit from historical analyses of additional data sources, as the relationship between the HOLC maps and actual historical lending practices is not straightforward.
Reconciling Unexpected and Contradictory Findings
Does mortgage discrimination improve health? It is widely accepted in the field of population health that housing discrimination is harmful to health, but several studies show a “protective” effect. Three studies [34, 36, 66] found that living in a neighborhood characterized by racialized mortgage discrimination was associated with better health outcomes. This finding can be explained by how area-level discrimination is measured. The individuals presumably excluded from neighborhoods where there is mortgage discrimination (i.e., the individuals experiencing discrimination) are not the same individuals currently living in the neighborhoods whose health outcomes are being measured. In other words, the people whose health is “protected” are the people who were not denied a loan. It is important to note that in these studies, minoritized households were systematically—but not totally—excluded from these neighborhoods. Thus, those who avoided that exclusion may have (1) been more likely to have better health to begin with and (2) benefitted from the resources available to other residents. Neighborhoods where minoritized people were more likely to get loans, on the other hand, may have fewer health-promoting resources. Suggesting, again, that exclusion is just one form of housing discrimination that should be captured in this body of work. Thus, these findings should not be interpreted as evidence that mortgage discrimination is beneficial for health. Instead, they should push scholars to conceptualize and measure the relational nature of space with attention to the role of power in being able to choose one’s residential location [80]. People excluded from one neighborhood via discrimination must live somewhere. Therefore, our discrimination measures should attempt to capture how processes of inclusion and exclusion and resource hoarding and deprivation are intertwined [81].
Is contemporary redlining inconsequential? While most studies examining historical redlining demonstrate a detrimental association with health, there is little evidence that present-day neighborhood-based mortgage exclusion is associated with health outcomes. On the surface, it may seem that present-day discrimination is less influential for health than historical discrimination. However, several factors may explain the lack of a relationship. First, scholars do not include the racial composition of neighborhoods. As previously mentioned, this oversight may lead to misclassifying neighborhoods as racially marked, potentially obscuring health impacts. Second, wholesale exclusion in the mortgage market is less prevalent than popularly thought. Instead, modern-day discrimination in the mortgage market is more complex and includes reverse-redlining or predatory inclusion as well as racialized reinvestment [67, 82]. Explicit exclusionary discrimination is no longer legal, and exclusion may not be as profitable, so banks may be more likely to include racially marked areas on an exploitative basis. Third, when neighborhood-based exclusion from the mortgage market is a part of a larger system of community divestment, it is only one dimension. Structural neglect is caused by a combination of institutional actors, including municipalities. The studies included here may be proxying disinvestment but to measure multidimensional nature of disinvestment and structural neglect, scholars will have to look beyond mortgage discrimination and examine municipal behavior.
How are past and present housing discrimination related? Many of the studies reviewed here examine either historical or present-day housing discrimination. However, research incorporating both historical and contemporary measures can highlight important nuances between seemingly similar neighborhoods. Only two studies reviewed here attempted such an analysis. McClure and colleagues examined how the foreclosure recovery was slower in formerly redlined neighborhoods [83]. While Lynch et al. [56] estimated trajectories of housing disinvestment in Milwaukee. Both studies suggest a potentially compounding impact on neighborhood health inequalities. However, even in these studies, there is a large gap between the 1930s and today. Several housing and neighborhood processes could explain the associations between historical redlining and health. First, subprime lending. Many formerly redlined communities of color were targeted for subprime lending (i.e., reverse redlining) and were subsequently hit hard by foreclosures during the Great Recession [84, 85]. Subprime lending is a form of wealth extraction and could plausibly explain the relationships documented between historical redlining and present-day health. Second, gentrification. Other neighborhoods locked out of mortgages in the twentieth century became targets of postwar capital investment, fueling gentrification, changing the housing and demographic landscape. Gentrification continues today in many formerly redlined neighborhoods through tax policies like opportunity zones which reduce capital gains taxes for investors who build or purchase properties eligible neighborhoods [86]. Thus, gentrification could plausibly explain some of the associations documented in the historical redlining studies. For instance, Mujahid and colleagues’ analysis found that a higher rated present-day social environment reduced the strength of the association between redlining and health. However, this finding may reflect those who are able to stay in neighborhoods undergoing social transformations. Third, deindustrialization. The abrupt transition away from an industrial economy fueled capital flight and weakened property tax revenue in urban communities contributing to a host of economic and health effects [87,88,89]. As these three examples demonstrate, understanding how racialized housing discrimination as a form of institutional racism impacts health requires more attention to the intimate connection between the racialization of space, housing markets, and neighborhood processes over time.
A Research Agenda
Based on the findings of this review, we present a research agenda to address some of the gaps in our current knowledge base.
-
1.
Diversify data sources on housing discrimination. There are not enough data sources to measure housing discrimination in the population health literature. We suggest four ways these data sources can be improved. First, for individual-level exposures, we suggest more detailed survey data. Surveys are an important tool to link housing experiences with individual-level health outcomes. However, one item on a survey cannot capture the complexities of housing discrimination. A 2005 Urban Institute and HUD report used 17 items to assess respondents’ experiences with housing discrimination [90]. It asked about the type of perceived discrimination, why they think they were discriminated against (e.g., race, source of income, disability), the role or occupation of the discriminator, and included open-ended questions allowing for the respondents to describe the experience in their own words. Future surveys could additionally ask how the perceived discrimination impacted their subsequent living situation. Second, there are no neighborhood-level studies focused on rental market discrimination. Only 40.6% of Black households and 46.6% of Latinx households own their homes compared to 73.1% of white families [91]. To our knowledge, no database tracks rental decisions made in the public or private rental market. Recently, scholars have been using online search engines such as Craigslist to assess housing discrimination. However, like audit studies, online assessments of rental discrimination can tell us how prevalent discrimination is in an area but linking this information to health data might prove challenging. Third, population health scholars interested in racism in the housing market should examine inclusionary discrimination. Predatory inclusion may be a more common form of housing discrimination today than outright exclusion in the early twentieth century [67]. Only one study in this review examines high-cost loans as a type of housing discrimination [56]. HMDA provides data on interest rates that could be used to understand the link between subprime lending and racial health disparities. Another potentially fruitful area of research might be discrimination in the home appraisal process [92, 93]. Fourth, scholars must start going beyond redlining to understand how historical racism in housing impacts present-day health inequities. Due to data availability—notably the digitizing of HOLC maps by Mapping Inequality—there has been almost a fetishization of redlining as a measure of racism in the population health literature. Redlining only represents one component of the racist housing system in the USA, but scholars have increasingly used it as a proxy for institutional racism at large. However, as Alex Hill astutely argues, when researchers use redlining as a metaphor for structural or institutional racism, they unintentionally ignore the other discriminatory practices and policies that link race and value, which ultimately harms health for some and promotes health for others [94, 95]. These other discriminatory practices, from exclusionary zoning to the financialization of housing markets, continue to shape where people can live and should be studied with as much rigor in the public health literature [96].
-
2.
Explore displacement and dispossession. The studies in this review primarily focus on discrimination while accessing new housing. Future studies might consider discrimination across the housing continuum. These studies could examine discrimination related to the ability to remain in a home (e.g., informal evictions) or upkeep a home (e.g., home improvement loans). The literature on the impact of displacement and dispossession on health is largely missing from this review. Our search returned studies on the health implications of eviction [97,98,99,100,101] and foreclosures [102,103,104,105,106,107,108]. We found none specifically linked discriminatory (i.e., disparate intent or outcome) evictions or foreclosures to health outcomes. This may be an important research agenda as housing costs are increasing in most jurisdictions across the USA while wages remain stagnant. This research may be particularly relevant during the ongoing COVID-19 pandemic as landlords across the country found ways to circumvent the federal eviction moratorium put in place by the US Centers for Disease Control and Prevention (CDC) [109]. To capture discriminatory evictions, scholars might focus their attention on serial evictors that concentrate in Black and Brown neighborhoods [110, 111]. Regarding upkeep, discrimination might be directly associated with health outcomes as homes can literally become unhealthy with sustained structural neglect.
-
3.
Identify causal pathways. Studies included in this review mainly examined associations. But finding associations, particularly with historical exposures, should only be a first step. To build on this work, researchers should explore and test causal pathways to explain why some housing discrimination exposures are linked to health outcomes in specific populations in specific geographies. For example, historical redlining was associated with lung cancer but not breast or colorectal cancer. An exploration of causal pathways might explain why this is the case. Perhaps the association with lung cancer is related to the deliberate concentration of environmental pollutants in certain neighborhoods [112]. Research in this vein can help scholars and policymakers tease out these associations and make more informed decisions about place-based interventions. Several potential mechanisms linking housing discrimination and health exist, including mental health, built environment, and limited access to opportunities over time [113]. Furthermore, qualitative and mixed methods research can both deepen our knowledge about context-specific mechanisms (e.g., precarious wage labor, intersectional stigma and discrimination, government abandonment, and natural disasters) linking racialized housing discrimination and health and unveil new and/or understudied pathways [114,115,116]. In turn, these methods can reveal limitations in the dominant ways that housing discrimination is measured and interpreted.
Limitations
We did not include a meta-analysis due to the heterogeneity in the racialized housing discrimination exposures, outcomes, and study designs. Additionally, our review may suffer from publication bias as null findings may be less likely to make it into the peer-reviewed process. We also may have missed some published studies that reported the relationship between housing discrimination and health but did not emphasize the findings in the text of the articles. We attempted to limit these omissions by including in our search terms discrimination scales that specifically mention housing discrimination and thoroughly searching both the text and the tables for potential associations. We included all associations regardless of whether they were focal features of the respective articles. Our results are also limited by the specific search terms, databases, and protocols we used. However, our terms were broad, and we used a snowball method to identify additional articles that our search may have missed.
We limited our scope to studies that report at least one health outcome. We exclude drug use and other health behaviors which are important mediators for health. Future reviews could include how racialized housing discrimination shapes social and sexual networks, geographic access to healthcare, nutritious food options, exposure to hazardous toxin sites, and opportunities to engage in physical activity. Additionally, we intentionally avoid cross-national comparisons by limiting the search to publications focused on the USA. However, we acknowledge the global prevalence of racial and ethnic discrimination in housing. Future work should explore the heterogenous legal landscape regarding racialized housing discrimination to develop and understand global comparisons.
Finally, our results are limited to studies examining racial discrimination in housing. We recognize that individuals and institutions engage in housing discrimination based on disability, gender, sexual orientation, children, age, unsheltered status, felony status, drug use, and other experiences. These identities and experiences intersect with race in important ways [117, 118]. We limited the scope of our search to those directly assessing racialized housing discrimination in order to highlight its impact as a form of institutional racism.
Conclusion
Critical conceptual and methodological gaps exist in the literature exploring racialized housing discrimination and health. This crucial lever in the “race discrimination system” [119] must be better understood to improve population health equity. Our review highlights the merits of housing discrimination measures using survey and administrative data. However, inconsistencies in how various forms of housing discrimination were defined and measured hinder our understanding. Future research should seek to diversify data sources, examine discrimination across the housing continuum, including dispossession and displacement, and explore causal pathways from housing discrimination to health. This research should be grounded in the history and political economy of specific places to improve how we measure housing discrimination, understand its relationship to health, and develop meaningful policy interventions (Table 5).
References
Link BG, Phelan J. Social conditions as fundamental causes of disease. J Health Soc Behav. 1995;80–94.
Williams DR, Collins C. Racial residential segregation: a fundamental cause of racial disparities in health. Public Health Rep Wash DC. 1974;2001(116):404–16.
Acevedo-Garcia D. Residential segregation and the epidemiology of infectious diseases. Soc Sci Med. 2000;51:1143.
Bower KM, Thorpe RJ, Yenokyan G, McGinty EEE, Dubay L, Gaskin DJ. Racial Residential segregation and disparities in obesity among women. J Urban Health. 2015;92:843–852.
Yang T-C, Zhao Y, Song Q. Residential segregation and racial disparities in self-rated health: how do dimensions of residential segregation matter? Soc Sci Res. 2017;61:29–42.
Britton ML, Goldsmith PR. Keeping people in their place? Young-adult mobility and persistence of residential segregation in US metropolitan areas. Urban Stud. 2013;50:2886–903.
Caldwell JT, Ford CL, Wallace SP, Wang MC, Takahashi LM. Racial and ethnic residential segregation and access to health care in rural areas. Health Place. 2017;43:104–12.
Moon G, Pearce J, Barnett R. Smoking, ethnic residential segregation, and ethnic diversity: a spatio-temporal analysis. Ann Assoc Am Geogr. 2012;102:912–21.
Nuru-Jeter AM, LaVeist TA. Racial segregation, income inequality, and mortality in US metropolitan areas. J Urban Health. 2011;88:270–82.
Dawkins CJ. Recent evidence on the continuing causes of Black-White residential segregation. J Urban Aff Routledge. 2004;26:379–400.
Krysan M, Crowder K. Cycle of segregation: social processes and residential stratification. New York: Russell Sage Foundation; 2017.
Riley AR. Neighborhood disadvantage, residential segregation, and beyond—lessons for studying structural racism and health. J Racial Ethn Health Disparities. 2018;5:357–65.
Sewell AA. The racism-race reification process: a mesolevel political economic framework for understanding racial health disparities. Sociol Race Ethn. 2016;2:402–32.
Slater T. Your life chances affect where you live: a critique of the “cottage industry” of neighbourhood effects research. Int J Urban Reg Res. 2013;37:367–87.
Clark WAV. Reexamining the moving to opportunity study and its contribution to changing the distribution of poverty and ethnic concentration. Demography. 2008;45:515–35.
Graif C, Arcaya MC, Diez Roux AV. Moving to opportunity and mental health: exploring the spatial context of neighborhood effects. Soc Sci Med. 1982;2016(162):50–8.
Jackson L, Langille L, Lyons R, Hughes J, Martin D, Winstanley V. Does moving from a high-poverty to lower-poverty neighborhood improve mental health? A realist review of ‘Moving to Opportunity.’ Health Place. 2009;15:961–70.
Sharkey P. Residential mobility and the reproduction of unequal neighborhoods. Cityscape. 2012;14:9–31.
Swope CB, Hernández D. Housing as a determinant of health equity: a conceptual model. Soc Sci Med. 2019;243:112571.
Du Bois WEB. The Philadelphia Negro: a social study. Philadelphia: University of Pennsylvania Press; 1996.
Taylor KY. Back story to the neoliberal moment: race taxes and the political economy of black urban housing in the 1960s. Souls. 2013;14:185–206.
Mclaughlin M. Long, Hot summer of 1967: urban rebellion in America. New York, NY: Palgrave Macmillan; 2014.
United States Kerner Commission. Report of the National Advisory Commission on Civil Disorders. New York: Bantam Books; 1968.
Yinger J. Housing discrimination and residential segregation as causes of poverty. Understanding Poverty. Russell Sage; 2001. p. 359–91.
Turner MA, Santos R, Levy DK, Wissoker DA, Aranda C, Pitingolo R, et al. Housing discrimination against racial and ethnic minorities 2012. Washington, D.C.: U.S. Department of Housing and Urban Development; 2013. p. 190.
Pager D, Shepherd H. The sociology of discrimination: racial discrimination in employment, housing, credit, and consumer markets. Annu Rev Sociol. 2008;34:181–209.
Ross SL, Turner MA. Housing discrimination in metropolitan America: explaining changes between 1989 and 2000. Soc Probl. 2005;52:152–80.
Turner MA, Struyk RJ, Yinger, The urban institute. Housing discrimination study: synthesis. Washington, D.C.: U.S. Department of Housing and Urban Development. 1991. Available from: https://www.huduser.gov/Portal/sites/default/files/pdf/HDS-Synthesis.pdf. Accessed 30 Oct 2021.
The Fair Housing Act. 2015. Available from: https://www.justice.gov/crt/fair-housing-act-1. Accessed 23 Feb 2022.
HUD. Housing Discrimination Under the Fair Housing Act. Available from: https://www.hud.gov/program_offices/fair_housing_equal_opp/fair_housing_act_overview. Accessed 19 Oct 2021.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group TP. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151:264–69.
Schlag AK. Percentages of problem drug use and their implications for policy making: a review of the literature. Drug Sci Policy Law. 2020;6:1–9.
Kardefelt-Winther D, Heeren A, Schimmenti A, van Rooij A, Maurage P, Carras M, et al. How can we conceptualize behavioural addiction without pathologizing common behaviours? Addiction. 2017;112:1709–15.
Gee GC. A multilevel analysis of the relationship between institutional and individual racial discrimination and health status. Am J Public Health. 2008;98:S48-56.
Osypuk TL, Schmidt NM, Kehm RD, Tchetgen Tchetgen EJ, Glymour MM. The price of admission: does moving to a low-poverty neighborhood increase discriminatory experiences and influence mental health? Soc Psychiatry Psychiatr Epidemiol. 2019;54:181–190.
Mendez DD, Hogan VK, Culhane JF. Institutional racism, neighborhood factors, stress, and preterm birth. Ethn Health. 2014;19:479–99.
Beyer KMM, Zhou Y, Matthews K, Bemanian A, Laud PW, Nattinger AB. New spatially continuous indices of redlining and racial bias in mortgage lending: links to survival after breast cancer diagnosis and implications for health disparities research. Health Place. 2016;40:34–43.
Mendez DD, Hogan VK, Culhane J. Institutional racism and pregnancy health: using Home Mortgage Disclosure act data to develop an index for mortgage discrimination at the community level. Public Health Rep Wash DC. 1974;2011(126 Suppl 3):102–14.
Nardone AL, Casey JA, Rudolph KE, Karasek D, Mujahid M, Morello-Frosch R. Associations between historical redlining and birth outcomes from 2006 through 2015 in California. PLOS ONE. 2020;15:e0237241.
Mujahid MS, Gao X, Tabb LP, Morris C, Lewis TT. Historical redlining and cardiovascular health: the multi-ethnic study of atherosclerosis. Proc Natl Acad Sci U S A. 2021;118:e2110986118.
Rosenberg L, Palmer JR, Wise LA, Horton NJ, Corwin MJ. Perceptions of racial discrimination and the risk of preterm birth. Epidemiol. 2002;13:646–52.
Wise LA, Palmer JR, Cozier YC, Hunt MO, Stewart EA, Rosenberg L. Perceived racial discrimination and risk of uterine leiomyomata. Epidemiol Camb Mass. 2007;18:747–57.
Cozier Y, Palmer JR, Horton NJ, Fredman L, Wise LA, Rosenberg L. Racial discrimination and the incidence of hypertension in US black women. Ann Epidemiol. 2006;16:681–7.
Taylor TR, Williams CD, Makambi KH, Mouton C, Harrell JP, Cozier Y, et al. Racial discrimination and breast cancer incidence in US Black women: the Black Women’s Health Study. Am J Epidemiol. 2007;166:46–54.
Albert MA, Cozier Y, Ridker PM, Palmer JR, Glynn RJ, Rose L, et al. Perceptions of race/ethnic discrimination in relation to mortality among Black women: results from the Black Women’s Health Study. Arch Intern Med. 2010;170:896–904.
Cancel Martinez Y. New insights on disadvantage in Wisconsin: perceived housing discrimination and its association with residential conditions and poor mental health [PhD Thesis]. ProQuest Diss. Theses. [Ann Arbor]: The University of Wisconsin – Madison. 2019. Available from: https://search.proquest.com/docview/2338533838?accountid=14512http://ucelinks.cdlib.org:8888/sfx_local?url_ver=Z39.88-2004&rft_val_fmt=info:ofi/fmt:kev:mtx:dissertation&genre=dissertations+%26+theses&sid=ProQ:ProQuest+Dissertations+%26+Theses+Global&atit. Accessed 23 Feb 2020.
Williams DR, Gonzalez HM, Williams S, Mohammed SA, Moomal H, Stein DJ. Perceived discrimination, race and health in South Africa. Soc Sci. 2008;67:441–52.
Krieger N, Smith K, Naishadham D, Hartman C, Barbeau EM. Experiences of discrimination: validity and reliability of a self-report measure for population health research on racism and health. Soc Sci Med. 2005;61:1576–96.
Yang T-C, Park K. To what extent do sleep quality and duration mediate the effect of perceived discrimination on health? Evidence from Philadelphia. J Urban Health. 2015;92:1024–37.
Yang T-C, Chen D, Park K. Perceived housing discrimination and self-reported health: how do neighborhood features matter? Ann Behav Med. 2016;50:789–801.
Rooks RN, Xu Y, Holliman BD, Williams DR. Discrimination and mental health among Black and white adults in the YES health study. Race Soc Probl. 2011;3:182–96.
Beyer KMM, Laud PW, Zhou Y, Hettinger AB. Housing discrimination and racial cancer disparities among the 100 largest US metropolitan areas. Cancer. 2019;125:3818–27.
Matoba N, Suprenant S, Rankin K, Yu H, Collins JW. Mortgage discrimination and preterm birth among African American women: an exploratory study. Health Place. 2019;59:102193.
Mendez DD, Hogan VK, Culhane JF. Stress during pregnancy: the role of institutional racism. Stress Health J Int Soc Investig Stress. 2013;29:266–74.
Zhou Y, Bemanian A, Beyer KMM. Housing discrimination, residential racial segregation, and colorectal cancer survival in Southeastern Wisconsin. Cancer Epidemiol Biomark Prev Publ Am Assoc Cancer Res Cosponsored Am Soc Prev Oncol. 2017;26:561–8.
Lynch EE, Malcoe LH, Laurent SE, Richardson J, Mitchell BC, Meier HCS. The legacy of structural racism: associations between historic redlining, current mortgage lending, and health. SSM - Popul Health. 2021;14:100793.
Nelson RK, Winling L, Marciano R. Mapping inequality. Available from: https://dsl.richmond.edu/panorama/redlining/#loc=5/39.1/-94.58. Accessed 10 Sep 2020.
Bey GS, Person SD, Kiefe C. Gendered race and setting matter: sources of complexity in the relationships between reported interpersonal discrimination and cardiovascular health in the CARDIA study. J Racial Ethn Health Disparities. 2020;7:687–97.
Krieger N, Van Wye G, Huynh M, Waterman PD, Maduro G, Li W, et al. Structural racism, historical redlining, and risk of preterm birth in New York city, 2013–2017. Am J Public Health. 2020;110:1046–53.
Nardone AL, Casey JA, Morello-Frosch R, Mujahid M, Balmes JR, Thakur N. Associations between historical residential redlining and current age-adjusted rates of emergency department visits due to asthma across eight cities in California: an ecological study. Lancet Planet Health. 2020;4:e24-31.
Hollenbach SJ, Thornburg LL, Glantz JC, Hill E. Associations between historically redlined districts and racial disparities in current obstetric outcomes. JAMA Netw Open. 2021;4:e2126707.
Li M, Yuan F. Historical redlining and resident exposure to COVID-19: a study of New York city. Race Soc Probl. 2021. Available from: https://link.springer.com/10.1007/s12552-021-09338-z. Accessed 18 Oct 2021.
Li D, Newman GD, Wilson B, Zhang Y, Brown RD. Modeling the relationships between historical redlining, urban heat, and heat-related emergency department visits: an examination of 11 Texas cities. Environ Plan B Urban Anal City Sci. 2021;49:933–52
Krieger N, Wright E, Chen JT, Waterman PD, Huntley ER, Arcaya M. Cancer stage at diagnosis, historical redlining, and current neighborhood characteristics: breast, cervical, lung, and colorectal cancers, Massachusetts, 2001–2015. Am J Epidemiol [Internet]. 2020. [cited 2020 Sep 3]; Available from: https://academic.oup.com/aje/advance-article/doi/10.1093/aje/kwaa045/5812653
Nardone AL, Chiang J, Corburn J. Historic redlining and urban health today in U.S. cities. Environ Justice. 2020;13:109–19.
Collin LJ, Gaglioti AH, Beyer KM, Zhou Y, Moore MA, Nash R, et al. Neighborhood-level redlining and lending bias are associated with breast cancer mortality in a large and diverse metropolitan area. Cancer Epidemiol Biomarkers Prev. 2021;30:53–60.
Taylor K-Y. Race for profit [Internet]. S.I.: University of North Carolina Press. 2019. [cited 2020 Oct 2]. Available from: https://api.overdrive.com/v1/collections/v1L2BaQAAAJcBAAA1M/products/096d080f-299b-44d7-91d9-f919d7b5a6a2
Hillier AE. Redlining and the home owners’ loan corporation. J Urban Hist. 2003;29:394–420.
Haupert T. Racial patterns in mortgage lending outcomes during and after the subprime boom. Hous Policy Debate. 2019;29:947–76.
Desmond M, Gershenson C, Kiviat B. Forced relocation and residential instability among urban renters. Soc Serv Rev. 2015;89:227–62.
Abravanel MD. Public knowledge of fair housing law: does it protect against housing discrimination? Hous Policy Debate. 2002;13:469–504.
Avery R, Brevoort K, Canner G. Opportunities and issues in using HMDA data. J Real Estate Res. 2007;29:351–80.
Michney TM. How the city survey’s redlining maps were made: a closer look at HOLC’s mortgage rehabilitation division. J Plan Hist. 2022;21:316–44
Fishback P, Rose J, Snowden KA, Storrs T. New evidence on redlining by federal housing programs in the 1930s. J Urban Econ. 2022;103462.
Hillier AE. Spatial analysis of historical redlining: a methodological exploration. J Hous Res. 2003;14:137–67.
Hillier AE. Residential security maps and neighborhood appraisals: the home owners’ loan corporation and the case of Philadelphia. Soc Sci Hist. 2005;29:207–33.
Faber J. Contemporary echoes of segregationist policy: spatial marking and the persistence of inequality. Urban Stud. 2021;58:1067–86.
Faber JW. We built this: consequences of new deal era intervention in America’s racial geography. Am Sociol Rev. 2020;85:739–75.
Michney TM, Winling L. New perspectives on new deal housing policy: explicating and mapping HOLC loans to African Americans. J Urban Hist. 2020;46:150–80.
Lawton P. Unbounding gentrification theory: multidimensional space, networks and relational approaches. Reg Stud Routledge. 2020;54:268–79.
Mitchell D. A relational approach to landscape and urbanism: the view from an exclusive suburb. Landsc Res. 2017;42:277–90.
Wyly EK, Atia M, Hammel DJ. Has mortgage capital found an inner‐city spatial fix? Hous Policy Debate. 2004;15:623–85.
McClure E, Feinstein L, Cordoba E, Douglas C, Emch M, Robinson W, et al. The legacy of redlining in the effect of foreclosures on Detroit residents’ self-rated health. Health Place. 2019;55:9–19.
Hernandez J. Redlining revisited: mortgage lending patterns in Sacramento 1930–2004. Subprime Cities Polit Econ Mortg Mark [Internet]. John Wiley & Sons, Ltd. 2012. [cited 2023 Feb 22]. p. 185–218. Available from: https://onlinelibrary.wiley.com/doi/abs/10.1002/9781444347456.ch7
Squires GD. Predatory lending: redlining in reverse. Shelterforce. 2005. Available from: https://shelterforce.org/2005/01/01/predatory-lending-redlining-in-reverse/. Accessed 22 Feb 2023.
Kurban H, Otabor C, Cole-Smith B, Gautam GS. Gentrification and opportunity zones: a study of 100 most populous cities with D.C. as a case study. Cityscape. 2022;24:149–86.
Renner C, Navarro V. Why is our population of uninsured and underinsured persons growing? The consequences of the “deindustrialization” of America. Annu Rev Public Health. 1989;10:85–94.
Nosrati E, Ash M, Marmot M, McKee M, King LP. The association between income and life expectancy revisited: deindustrialization, incarceration and the widening health gap. Int J Epidemiol. 2018;47:720–30.
Winant G. “Hard Times make for hard arteries and hard livers”: deindustrialization, biopolitics, and the making of a new working class. J Soc Hist. 2019;53:107–32.
Abravanel MD. Do we know more now: trends in public knowledge, support and use of fair housing law. U.S. Department of Housing and Urban Development. 2006. Available from: https://www.huduser.gov/publications/pdf/fairhousingsurveyreport.pdf. Accessed 23 Feb 2022.
Haughwout A, Lee D, Scally J, van der Klaauw W. Inequality in U.S. homeownership rates by race and ethnicity -liberty street economics. Federal Reserve Bank of New York. 2020. Available from: https://libertystreeteconomics.newyorkfed.org/2020/07/inequality-in-us-homeownership-rates-by-race-and-ethnicity.html. Accessed 23 Feb 2022.
Perry AM, Rothwell J, Harshbarger D. The devaluation of assets in Black neighborhoods [Internet]. Brookings. 2018. [cited 2021 Apr 13]. Available from: https://www.brookings.edu/research/devaluation-of-assets-in-black-neighborhoods/
Howell J, Korver-Glenn E. Neighborhoods, race, and the twenty-first-century housing appraisal industry. Sociol Race Ethn. 2018;4:473–90.
Hill AB. Before redlining and beyond: how data-driven neighborhood classification masks spatial racism. 2021 [cited 2022 Sep 6]; Available from: https://metropolitics.org/IMG/pdf/met-hill.pdf
Imbroscio D. Race matters (even more than you already think): racism, housing, and the limits of The Color of Law. J Race Ethn City. 2021;2:29–53.
Gioielli R. The tyranny of the map: rethinking redlining. The Metropole. 2022. Available from: https://themetropole.blog/2022/11/03/the-tyranny-of-the-map-rethinking-redlining/. Accessed 23 Feb 2023.
Desmond M, Kimbro RT. Eviction’s fallout: housing, hardship, and health. Soc Forces. 2015;94:295–324.
Willie TC, Linton SL, Whittaker S, Martinez I, Sharpless L, Kershaw T. “There’s no place like home”: examining the associations between state eviction defense protections and indicators of biopsychosocial stress among survivors of intimate partner violence. Soc Sci Med. 2021;279:113957.
Leifheit KM, Jennings JM. Eviction as a social determinant of sexual health outcomes. Sex Transm Dis. 2019;46:69–71.
Hazekamp C, Yousuf S, Day K, Daly MK, Sheehan K. Eviction and pediatric health outcomes in Chicago. J Community Health. 2020:891–99
Sealy-Jefferson S, Butler B, Chettri S, Elmi H, Stevens A, Bosah C, et al. Neighborhood evictions, marital/cohabiting status, and preterm birth among African American Women. Ethn Dis. 2021;31:197–204.
Chambers EC, Hanna DB, Hua S, Duncan DT, Camacho-Rivera M, Zenk SN, et al. Relationship between area mortgage foreclosures, homeownership, and cardiovascular disease risk factors: the Hispanic Community Health Study/Study of Latinos. BMC Public Health. 2019;19:77.
Christine PJ, Moore K, Crawford ND, Barrientos-Gutierrez T, Sánchez BN, Seeman T, et al. Exposure to neighborhood foreclosures and changes in cardiometabolic health: results from MESA. Am J Epidemiol. 2017;185:106–14.
Duran AC, Zenk SN, Tarlov E, Duda S, Smith G, Lee JM, et al. Foreclosures and weight gain: differential associations by longer neighborhood exposure. Prev Med. 2019;118:23–9.
Hoyle ME, Chamberlain AW, Wallace D. The effect of home foreclosures on child maltreatment rates: a longitudinal examination of neighborhoods in Cleveland, Ohio. J Interpers Violence. 2022;37:NP2768–NP2790
Schootman M, Deshpande AD, Pruitt SL, Jeffe DB. Neighborhood foreclosures and self-rated health among breast cancer survivors. Qual Life Res Int J Qual Life Asp Treat Care Rehabil. 2012;21:133–41.
Sealy-Jefferson S, Misra DP. Neighborhood tax foreclosures, educational attainment, and preterm birth among urban African American women. Int J Environ Res Public Health. 2019;16:904
Downing B. Subprime babies: the foreclosure crisis and initial health endowments. RSF Russell Sage Found J Soc Sci. 2019;5:123.
Higgins A. One millionaire landlord was behind half of Milwaukee’s evictions during Covid lockdowns last June. Here’s the story of how corporate landlords helped drive the evictions crisis. Bus. Insid. 2021. Available from: https://www.businessinsider.com/how-corporate-landlords-helped-drive-the-covid-evictions-crisis-2021-3. Accessed 13 Apr 2021.
Anti-eviction mapping project. EvictorBook [Internet]. [cited 2021 Oct 30]. Available from: https://evictorbook.com/
McElroy E, Amir-Ghassemi A. Evictor Structures: Erin McElroy and Azad Amir-Ghassemi on fighting displacement. Log Mag. 2020. Available from: https://logicmag.io/commons/evictor-structures-erin-mcelroy-and-azad-amir-ghassemi-on-fighting/. Accessed 29 Oct 2021.
Hoffman JS, Shandas V, Pendleton N. The effects of historical housing policies on resident exposure to intra-urban heat: a study of 108 us urban areas. Climate. 2020;8:12.
Mehdipanah R, Ramirez J, Abedin S, F. Brown S. Housing discrimination and health: understanding potential linking pathways using a mixed-methods approach. Soc Sci. 2018;7:194.
Keene DE, Cowan SK, Baker AC. “When you’re in a crisis like that, you don’t want people to know”: mortgage strain, stigma, and mental health. Am J Public Health. 2015;105:1008–12.
Whittle HJ, Leddy AM, Shieh J, Tien PC, Ofotokun I, Adimora AA, et al. Precarity and health: theorizing the intersection of multiple material-need insecurities, stigma, and illness among women in the United States. Soc Sci Med. 2020;245:1.
Brennan M, Srini T, Steil J, Mazereeuw M, Ovalles L. A perfect storm? Disasters and evictions. Hous Policy Debate Routledge. 2022;32:52–83.
Beltran T, Allen AM, Lin J, Turner C, Ozer EJ, Wilson EC. Intersectional discrimination is associated with housing instability among trans women living in the San Francisco Bay Area. Int J Environ Res Public Health. 2019;16:4521.
Hanley J, Ives N, Lenet J, Hordyk S-R, Walsh C, Ben Soltane S, et al. Migrant women’s health and housing insecurity: an intersectional analysis. Int J Migr Health Soc Care. 2019;15:90–106.
Reskin B. The race discrimination system. Annu Rev Sociol. 2012;38:17–35.
Acknowledgements
The authors thank the reviewers for generous and generative feedback and Rafik Wahbi for helpful comments on an earlier draft. Cross, Huỳnh, and Francis received support from the Robert Wood Johnson Foundation Health Policy Research Scholars Program. Cross additionally received support from the UCLA Ziman Center for Real Estate.
Author information
Authors and Affiliations
Contributions
RIC: conceptualized study, project management, data screening, data extraction, wrote first full draft, edited 2nd draft; JH: data screening, data extraction, edited 1st draft, edited 3rd draft; NJB: data screening, data extraction, edited 3rd draft; BF: data screening, data extraction, edited 3rd draft.
Corresponding author
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cross, R.I., Huỳnh, J., Bradford, N.J. et al. Racialized Housing Discrimination and Population Health: a Scoping Review and Research Agenda. J Urban Health 100, 355–388 (2023). https://doi.org/10.1007/s11524-023-00725-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11524-023-00725-y