Abstract
Different studies suggest a strong association between childhood abuse and alcohol use disorders (AUDs). The modulation of the startle response has been used to assess emotional processing in AUDs. The main objective of the study was to investigate the startle reflex responses to different stimuli in young adults with varying types of childhood abuse in comparison with a control group according to their current alcohol consumption and the presence of a parent with alcohol dependence or not. A clinical sample of 606 adolescents, divided into five groups: no abuse, physical neglect, emotional neglect, emotional abuse, physical abuse, and sexual abuse, were assessed on their pattern of alcohol consumption and their family history of alcoholism. The proportion of participants with at least one alcohol-dependent parent was higher in all types of abuse. The proportion of heavy drinkers and alcohol-dependent participants was higher in the groups with physical neglect and sexual abuse. Heavy drinkers and alcohol dependents showed a lower startle reflex response to emotional pictures, especially alcohol-related ones. Adolescents exposed to physical and sexual abuse during childhood showed a mitigated startle response to appetitive and alcohol-related pictures. The results of this exploratory study reveal that childhood maltreatment modulates emotional processing to alcohol-related stimuli during adolescence. The evaluation of these patients’ startle response could be considered a prognostic biomarker for establishing personalized preventive strategies during the adolescent stage to avoid, to a large extent, future problems derived from alcohol consumption.
Similar content being viewed by others
Alcohol consumption is common during adolescence, with secular trends toward earlier ages of alcohol initiation (Poznyak & Rekve, 2018). In Spain, adolescent alcohol consumption is a cause for concern, with similar rates to those in other European countries. However, the prevalence of recent drunkenness in Spain (17%) is higher than the European average (13%) (Drugs, 2021). Consumption of alcohol during adolescence increases the risk of later alcohol user disorders (AUDs) compared to non-alcohol-drinking adolescent peers (Lee et al., 2016; McCambridge et al., 2011). This has increased interest in public and clinical interventions in adolescents with the final goal of preventing AUDs in adulthood.
The etiology of alcohol use disorders (AUDs) includes biological, psychological, and environmental factors (Hill & O’Brien, 2015; Obeid et al., 2020; Yang et al., 2022; Young-Wolff et al., 2011). Parental alcohol consumption increases the prevalence of alcohol consumption in adolescents (Wahlstrom et al., 2023). Consuming alcohol in front of children can reduce their fear of negative consequences and normalize alcohol consumption. This behavior by parents contributes to earlier alcohol initiation and later use in adolescents (Rossow et al., 2016; Ryan et al., 2010; Smit et al., 2022). On the other hand, there is a close relationship between parental alcohol problems and parental childhood abuse and neglect. This relationship also contributes to an increased risk of adolescent drug abuse as a way to cope with these situations. Childhood abuse is another risk factor for AUDs (Baudin et al., 2022; Diaz et al., 2002; Dube et al., 2006; A. L. Goldstein et al., 2013; Kisely et al., 2020; Lotzin et al., 2016; Rehan et al., 2017; Rogers et al., 2022; Schwandt et al., 2013; Shin, Wang, et al., 2019,b). Data from the National Epidemiologic Survey on Alcohol and Related Conditions in the USA showed that childhood abuse significantly increases the risk for alcohol abuse or dependence in adulthood (Moore et al., 2019). Previous studies also related a close association between childhood maltreatment, especially sexual abuse and emotional neglect, and polydrug abuse, including alcohol abuse (Alvarez-Alonso et al., 2016). However, the pathways linking child maltreatment to later alcohol use remain unclear.
Some studies have explored adverse maltreatment outcomes such as post-traumatic stress disorder, depression, or antisocial behavior (Elmore & Crouch, 2022; Jin et al., 2022; Tan et al., 2022; Wang et al., 2022; White & Widom, 2008; Wilson & Widom, 2009). Dutcher et al. (Dutcher et al., 2017) found that emotional regulation problems mediated the association between childhood maltreatment severity and alcohol problems. This fact suggests that adults maltreated as children may develop emotional regulation difficulties like non-acceptance of negative emotions or issues controlling impulsive behaviors when distressed. Other studies indicate the role of self-regulation processes, such as behavioral dysregulation, as possible mediators. Thus, adults with a child maltreatment history could be more vulnerable to alcohol because of pre-existing regulatory problems in controlling stressful situations (Shin, Jiskrova, & Wills, 2019,b).
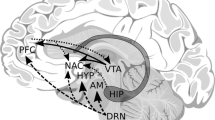
The link between childhood abuse and later AUDs also focused on the relationship between the stress resulting from maltreatment and the sensitization of the brain circuits involved in alcohol reward. The stress response consists of the release of glucocorticoids and cortisol. The activation of the hypothalamic-pituitary-adrenal (HPA) axis is responsible for the release of cortisol and catecholamines to cope with stressful situations. Chronic activation of this system has been associated with mental disorders such as depression, anxiety, and drug addiction (Das et al., 2022; Genis-Mendoza et al., 2022; S. C. Goldstein et al., 2022; Keller et al., 2017; Sapolsky et al., 2000). Moreover, some studies conducted with rodents found that exposure to stress increases dopamine concentrations in mesolimbic structures involved in reward (nucleus accumbens and ventral tegmental area), which in turn increases behaviors of self-administration of drugs such as alcohol and psychostimulants (Kalivas et al., 1993; Meaney et al., 2002; Ostroumov et al., 2016; Spanagel et al., 2014).
Processing alcohol-related stimuli is a crucial aspect of understanding the mechanisms associated with the development of alcohol dependence (Bollen et al., 2021; Dominguez-Centeno et al., 2020; Murray et al., 2022; Roberts & Fillmore, 2015). Moreover, the sensitization of the reward system influences the processing of emotional information (Walsh et al., 2019). The modulation of the startle response has been widely used to assess emotional processing in AUDs (Grusser et al., 2002; Jurado-Barba et al., 2015; Loeber et al., 2007; Mereish & Miranda Jr., 2021; Rubio et al., 2013). Previous studies found an attenuated startle response (appetitive response) in patients with AUDs to alcohol-related cues compared to healthy participants (Heinz et al., 2003; Lemenager et al., 2014; Loeber et al., 2007; Mucha et al., 2000). Furthermore, an attenuated startle reflex response to alcohol-related and aversive pictures could predict the alcohol dependence status (alcohol dependence versus non-dependence) after a 4-year follow-up (Jurado-Barba et al., 2017).
Startle reflex responses have also been explored in participants with childhood abuse. Although studies are very scarce, results showed that childhood abuse is associated with increased startle reactivity to acoustic no-emotional stimuli in adulthood (Jovanovic et al., 2009; Shalev et al., 2000). However, no studies have explored startle reflex responses to alcohol-related stimuli concerning childhood abuse and alcohol consumption. Therefore, the main objective of the present study was to investigate the startle reflex responses to different stimuli (alcohol-related, aversive, appetitive, and neutral pictures) in young adults with varying types of childhood abuse (physical neglect, emotional neglect, emotional abuse, physical abuse, and sexual abuse) in comparison with a control group (no abuse) according to their current alcohol consumption (no alcohol-abusers, alcohol-abusers, heavy-drinkers, and alcohol-dependents) and the presence of a parent with alcohol dependence or not.
Firstly, we consider that participants with more severe alcohol problems (i.e., heavy drinking and alcohol dependence) would show an attenuated startle response to alcohol-related pictures. Secondly, we hypothesized that patients with an alcohol-dependent parent would have a reduced startle reflex to alcohol-related pictures. Finally, our third hypothesis was that participants with more severe childhood abuse would show attenuated startle responses to stimuli, especially to alcohol-related pictures.
Materials and Methods
Participants
The participants were 606 adolescents (mean age: 16.4; range: 13–19 years) recruited from clinical programs (n = 355) and community sources (n = 300) in Madrid (Spain) (Alvarez-Alonso et al., 2016). Subjects were screened using The Childhood Trauma Questionnaire Short-Form (CTQ-SF, Spanish validation; (Hernandez et al., 2013). Using the CTQ-SF scores and cutoffs proposed by Bernstein et al. (2003), participants were classified into five groups according to the main abuse suffered in childhood: no abuse (N=372), physical neglect (N=48), emotional neglect (N=79), emotional abuse (N=24), physical abuse (N=32), and sexual abuse (N=51) (Bernstein et al., 2003).
A group of 300 adolescents, matched for age and sex, did not report the use of more than one substance (non-drug users’ group), but who could be alcohol consumers were used for comparison with the group of adolescents with alcohol abuse problems. These were recruited in Primary Care Units of the same Health Care Centers.
The current laws on alcohol consumption in Spain are similar to those of other European countries: the consumption and purchase of alcohol are not permitted for minors, i.e., for those under 18 years of age. However, it is crucial to note that as per the Spanish Ministry of Health, the prevalence of alcohol consumption among minors aged 14 to 17 was 77.2%, compared to 89.0% among 18-year-old students (Spanish Drugs and Addictions Observatory, 2021).
Measures
Childhood Abuse
The Childhood Trauma Questionnaire Short-Form (Bernstein et al., 2003) is a 28-item self-report instrument for adults and adolescents that assesses retrospective child abuse and neglect. The CTQ-SF consists of five scales that assess five widely accepted types of abuse: physical neglect, emotional neglect, emotional abuse, physical abuse, and sexual abuse. Each scale comprises five items that are scored on a 5-point Likert-type scale. Three additional items compose the minimization scale for detecting socially desirable responses or false-negative trauma reports. The internal consistency coefficients of the Spanish version were like the English version: physical neglect, α=.66, emotional neglect, α=.83, emotional abuse, α=.87, physical abuse, α=.88, and sexual abuse, α=.94 (Hernandez et al., 2013).
Mental Disorder Diagnoses
Diagnoses of mental disorders were determined using a version of the Schedule for Affective Disorders and Schizophrenia for School-Age Children (K-SADS) (Kaufman et al., 1997), along with several rating scales for psychopathology such as anxiety, depression, post-traumatic stress disorder (PTSD), borderline personality disorder (BPD), attention deficit hyperactivity disorder (ADHD), and eating disorder (ED). These interviews were conducted with both the adolescent and one parent. Consensus for diagnoses was reached among the interviewer, assessment coordinator, and clinically experienced faculty psychiatrist or clinical psychologist.
Alcohol Consumption
Drinking patterns and alcohol use disorders were assessed using the Structured Clinical Interview for the DSM-IV-Patient Edition (SCID-I/P) (First et al., 2002). Participants in our study were classified according to their drinking pattern as no alcohol abusers (N=115), alcohol abusers (N=188), heavy drinkers (N=266), and alcohol-dependents (N=37).
Startle Reflex Response
The startle reflex procedure was similar to previous studies (Rubio et al., 2013). Every participant was exposed to 120 color photographs (30 alcohol-related, 30 aversive, 30 appetitive, and 30 neutral stimuli). Aversive, appetitive, and neutral pictures were selected from the International Affective Picture System (IAPS); (Lang et al., 2005) according to their valence and arousal normative values from Spanish validation (Moltó et al., 2013; Vila et al., 2001). The 30 alcohol-related images depicting alcoholic beverages and typical drinking situations were used in similar studies (Grusser et al., 2002; Lang et al., 1997). The participants were presented with 10 blocks. Pictures and blocks were presented randomly for every participant. Startle probes were presented 2.5 to 5 s after the onset of the visual stimulus (target startle) or 4 to 10 s after the beginning of the inter-stimulus interval. Each alcohol-related picture was exhibited 2 times during the experiment, and startle probes were presented in the 50% of them.
Two electrodes (Ag–AgCl) filled with saline gel were attached to each participant’s right orbicularis oculi region to record startle eye blink EMG. According to guidelines, the ground electrode was placed on the right ear over the mastoid (Blumenthal et al., 2005). The EMG signal was acquired and amplified using an EMG100A module (BIOPAC Systems, Goleta, CA, USA) connected to an MP100WSW bioamplifier (BIOPAC Systems) with a time constant of 1000 ms. Data were recorded and displayed using AcqKnowledge III data acquisition software (BIOPAC Systems). The acoustic startle stimulus consisted of a 100 ms burst of white noise at 95dB (A), with instantaneous rise time. The noise burst was presented binaurally with Sennheiser HD500 headphones (Wedemark, Germany). The startle response represents the difference between a stable baseline (using the 50ms before the startle probe) and the maximum amplitude of the startle reflex 5–150 ms after the startle probe was presented (Mucha et al., 2000). The startle reflex response was measured in microvolts (μV) (Fig. 1).
Startle reflex response. Thirty alcohol-related, 30 aversive, 30 appetitive, and 30 neutral stimuli pictures are presented randomly for every participant. Startle probes were presented 2.5 to 5 s after the onset of the visual stimulus (target startle) or 4 to 10 s after the beginning of the inter-stimulus interval. VS visual stimulus
Procedure
After providing informed consent, the CTQ-SF was completed to assess childhood abuse, and the SCID-P was administered to explore alcohol drinking patterns. A psychiatrist and a psychologist blinded to the hypotheses carried out interviews and self-report measures. Finally, participants completed the startle reflex response task. The study followed the Helsinki Declaration (1975), revised in 2000. Approval of the protocol by appropriate local ethics committees was also secured.
Statistical Analysis
A mixed linear model and Chi-square with continuity correction tests were conducted to analyze differences between childhood abuse groups in age, sex, presence of alcohol-dependent parents, and alcohol consumption, considering psychopathology as a covariant in all the studies. A mixed model followed by the Bonferroni post hoc test was used in all the analyses to evaluate the statistical differences between groups. Spearman correlation was used to explore the correlations between the collected data using in-house Phyton code developed with Pandas, Seaborn, and Pingouin packages. The alpha level was adjusted to 0.05 for all the statistics, including correlation analyses.
Results
Sample Characteristics
Table 1 shows demographic and alcohol consumption information according to the different types of childhood abuse. The results did not show differences between childhood abuse groups in age. However, Fisher’s exact test revealed statistically significant differences between groups regarding sex and the presence of alcohol-dependent parents. In general, males suffered more frequently from all types of abuse, except sexual abuse, which was higher among females. The proportion of participants with at least one alcohol-dependent parent was higher in the physical neglect, physical abuse, sexual abuse, and emotional neglect groups. Chi-square with continuity correction test revealed statistically significant differences between groups considering the type of alcohol consumption and childhood abuse (P < .001, 15 d.f.). The proportion of heavy drinkers was higher in all types of abuse than in the no-abuse group. A higher proportion of alcohol-dependent participants was found in the groups with physical neglect and sexual abuse. Finally, the percentage of participants without alcohol abuse was higher in the group with no childhood abuse.
Childhood abuse can cause various psychological disorders that can lead to alcohol consumption. Indeed, young adults who experienced abuse during childhood had poorer mental health. Among the initial sample of adolescents who participated in the study, 13.3% had anxiety, 15.4% had depression, 10.3% had PTSD, and 8.2% had BPD. Additionally, 3–6% had ED and ADHD, respectively. However, out of those with a depressive disorder, 86.5% had minimal or mild depression, according to the Beck scale.
Startle Reflex Response and Alcohol Consumption
Results from the mixed model are shown in Fig. 2. Psychopathology has been considered in the analyses to avoid confounding factors. Depression (F (596) = 11.242, P < .001), BPD (F (596) = 6.226, P = .013), and ED (F (596) = 10.613, P = .001) showed significant effects on startle reflex response. The results showed a significant effect for the type of image exposure on the startle response (F (1806) = 8306.515, P < .001). Post hoc Bonferroni analyses indicated that, in general, participants showed an attenuated startle reflex response to alcohol-related pictures in comparison with appetitive, neutral, and aversive ones (all p’s = .000). An attenuated startle response to appetitive pictures was also found in contrast with neutral and aversive stimuli (all p’s = .000). Lastly, startle response to neutral pictures was also less intense in comparison with aversive ones (p =.000).
Startle response to aversive, neutral, appetitive, and alcohol-related pictures in no-alcohol abusers and adolescents with different types of alcohol consumption (alcohol abusers, heavy drinkers, and alcohol-dependents). Two-way ANOVA, P < 0.001. * vs. the same picture in the no alcohol abusers group. # vs. aversive picture within the same group of alcohol consumption. & vs. neutral picture within the same group of alcohol consumption. @ vs. appetitive picture within the same group of alcohol consumption
A significant effect was also found for the alcohol group (F (596) = 20.611, P < .001). Post hoc analyses revealed that alcohol-dependent participants in general showed an attenuated startle response in comparison with heavy drinkers, alcohol abusers, and no alcohol abusers (all p’s = .000). Moreover, the startle reflex responses showed in heavy drinkers were lower compared to the ones observed in alcohol abusers and no alcohol abusers (all p’s = .000). No differences were found between alcohol abusers and no alcohol abusers (p = 1.00). The interaction between alcohol consumption and type of image exposure was also significant (F (1806) = 21.836, P < .001). Post hoc analyses revealed that heavy drinkers and alcohol-dependents showed a lower startle reflex response to emotional pictures (alcohol-related, aversive, and appetitive) in comparison with no abusers and alcohol abusers (all p’s =.000) (Supplementary figure 1). Moreover, alcohol-dependent participants showed the lowest startle reflex response to emotional pictures compared to other groups (all p’s =.000). For neutral pictures, alcohol-dependents showed a lower startle reflex response in comparison with alcohol-abusers (p =.005). However, when considering only <18 years patients, there are not a statistically significant differences in the startle response to appetitive pictures between alcohol dependent and non-dependent patients (p = .328) (Supplementary figure 2).
Startle Reflex Response and Childhood Abuse
Results from the mixed model are shown in Fig. 3. Psychopathology has been considered in the analyses to avoid confounding factors. Depression (F (594) = 18.468, P < .001) and ED (F (594) = 9.748, P = .002) showed significant effects on startle reflex response. The results showed a significant effect for the type of image exposure on the startle response (F (1800) = 7004.530, P < .001). Post hoc analyses revealed an attenuated startle reflex response to alcohol-related pictures compared to appetitive, neutral, and aversive stimuli (all p’s = .000). The main effect for childhood abuse group was also significant (F (594) = 25.638, P < .001). Post hoc analyses revealed that participants with any childhood abuse (physical neglect, emotional neglect, emotional abuse, physical abuse, and sexual abuse) showed a generally altered startle response (all p’s < .01) in comparison with the non-abused group (no childhood abuse).
Startle response to aversive, neutral, appetitive, and alcohol-related pictures in adolescents with a history of maltreatment or exposed to a different type of maltreatment (physical neglect, emotional neglect, emotional abuse, physical abuse, and sexual abuse). Two-way ANOVA, P < 0.001. * vs. the same picture in the no-abuse group. # vs. aversive picture within the same group of alcohol consumption. & vs. neutral picture within the same group of alcohol consumption. @ vs. appetitive picture within the same group of alcohol consumption
The interaction between startle response to different types of images and childhood maltreatment was also significant (F (1800) = 26.804, P < .001). The follow-up tests showed that participants with childhood abuse displayed lower startle reflex responses to alcohol-related, aversive, and appetitive stimuli (all p’s ≤ .01) than participants without childhood abuse. Participants who suffered sexual abuse showed lower startle reflex to alcohol-related pictures than physical neglect, emotional neglect, and non-abuse groups (all p’s ≤.004) (Table 2). No differences were found between the sexual abuse vs physical abuse, and sexual abuse vs emotional abuse groups concerning alcohol-related images. Regarding aversive stimuli, the physical abuse group differed from physical neglect, emotional neglect, and non-abuse groups showing a lower startle reflex response (all p’s ≤ .000). There were no differences between the physical and sexual abuse groups. Concerning appetitive pictures, the sexual, physical, emotional abuse, and emotional neglect groups differed from non-abuse group showing a lower startle reflex response (all p’s ≤ .001). Finally, no differences between different types of abuse were observed in the startle reflex response to neutral pictures (Supplementary figure 3). When considering only <18 years old patients, no differences were observed in the startle response to appetitive and alcohol-related pictures between those exposed to emotional neglect (p = .155) or physical neglect (p = .516) in comparison with patients non-exposed to childhood abuse. In addition, in this sample population, no differences were observed in the startle amplitude to appetitive (p = .175) and aversive (p = .086) pictures between patients exposed to the emotional neglect and those non-exposed to any type of childhood abuse (Supplementary figure 4).
Startle Reflex Response and Presence of Alcohol-Dependent Parent
Results from the mixed model are shown in Fig. 4. Psychopathology has been considered in the analyses to avoid confounding factors. Depression (F (598) = 12.979, P < .001), PTSD (F (598) = 11.440, P < .001), BPD (F (598) = 5.756, P = 0.017), and ED (F (598) = 7.222, P = .007) showed significant effects on startle reflex response. The main effect of image on the startle response was detected (F (1812) = 7152.004, P < .001). However, no differences were found considering paternal alcohol consumption (F (598) = 3.257, P = .072). Interestingly, the interaction between startle response to different types of images and progenitor alcohol consumption was also significant (F (1812) = 26.956, P < .001). The statistical analyses revealed that participants with alcohol-dependent parents showed an attenuated startle reflex response to aversive pictures in comparison with participants without alcohol-dependent parents (p = .000) (Supplementary figure 5). The results were the same excluding participants over 18 years of age (Supplementary figure 6).
Startle response to aversive, neutral, appetitive, and alcohol-related pictures in adolescents with and without familial history of alcohol consumption. Two-way ANOVA, P < 0.001. * vs. the same picture in the no alcohol-dependent parent group. # vs. aversive picture within the same group of alcohol consumption. & vs. neutral picture within the same group of alcohol consumption. @ vs. appetitive picture within the same group of alcohol consumption
Correlation Analyses
Correlation studies were performed to find associations between the type of alcohol consumption (no alcohol, alcohol abuse, dependence, and heavy drinking), type of abuse (no abuse, physical neglect, emotional neglect, physical abuse, emotional abuse, and sexual abuse) and the startle reflex data to aversive, neutral, appetitive, and alcohol-related pictures. The analyses were carried out in two separate populations considering the presence of familial alcohol consumption history (AFH). The associations between all these factors vary considerably in some significant points between AFH (Fig. 5A) and no AFH (Fig. 5B) groups (see Supplementary Tables I and II). A strong and positive correlation was found between the startle response to alcohol-related and aversive and alcohol-related and appetitive pictures. These correlations appear to be lower in patients with AFH (aversive vs. alcohol-related pictures: r = 0.65, P < .001; appetitive vs. alcohol-related pictures: r = 0.81, P < .001) in comparison with those without AFH (aversive vs. alcohol-related pictures: r = 0.83, P < .001; appetitive vs. alcohol-related pictures: r = 0.91, P < .001). Within the AFH group, a negative and moderate correlation was found between the startle response to aversive pictures and physical abuse (r = −0.36, P < .001) and a moderate positive correlation between the response to aversive and alcohol-related pictures and alcohol abuse (r=0.31, P< .01). Interestingly, the absence of any abuse and alcohol abuse was more positively correlated in the AFH (r = 0.61, P < .001) than in the no AFH group (r = 0.099, P < .05). Within this no AFH group, moderate negative associations were found between sexual abuse and the startle response to aversive (r = −0.3, P < .001) and alcohol-related (r = −0.37, P < .001) pictures, which has not been observed in patients with AFH. In addition, sexual abuse is positively associated with alcohol dependence in both AFH (r = 0.31, P < .01) and no AFH (r = 0.33, P < .001) groups.
Spearman correlation studies between childhood maltreatment, current alcohol consumption during adolescence, and startle response to different types of pictures in patients with alcohol familial history (AFH) (A) or without (No AFH) (B). The color bar indicates the degree of positive (red) or negative (blue) association between the variables
Discussion
The present study is the first examining whether young adults with alcohol-dependent parents and a history of childhood abuse (physical neglect, emotional neglect, emotional abuse, physical abuse, and sexual abuse) showed disturbances in the startle reflex responses to different emotional stimuli, especially to alcohol-related pictures controlling for their current alcohol consumption (no alcohol-abusers, alcohol-abusers, heavy-drinkers, and alcohol-dependents). Interestingly, startling responses to aversive, appetitive, and alcohol-related pictures were more significantly attenuated in adolescents that suffered from emotional neglect or emotional, physical, or sexual abuse and who met the criteria for heavy drinking or alcohol dependence.
The startle reflex is a rapid, involuntary reflex muscle contraction caused by a sudden, intense stimulus (Wilkins et al., 1986). It is a psychophysiological measure primarily controlled by mesencephalic brain structures and easily modulated by the forebrain, exhibiting different forms of plasticity and finally reflecting the activation of the incentive-motivational system (M. Bradley & Sabatinelli, 2003; Swerdlow et al., 1992). Several previous studies have employed cue-modulated startle paradigms to evaluate the appetitive response to alcohol-related signs, in which the startle reflex is reliably modulated by the affective valence of foreground processing (Jurado-Barba et al., 2015; Jurado-Barba et al., 2017; Kang et al., 2018; Lemenager et al., 2014; Wietschorke et al., 2016). Thus, the startle reflex is increased with the presentation of unpleasant pictures and reduced with pleasant ones compared to neutral stimuli (Bradley et al., 1993).
The attenuation of the startle reflex to emotional stimuli may reflect the inhibition of defensive reflexes when appetitive motivation is high. At the same time, increasing this psychophysiological response may reveal an aversive and defensive reflex (Schupp et al., 1997). According to the results obtained, those adolescents having a parent with alcohol dependence, with past childhood abuse, or showing current alcohol use problems displayed significantly attenuated startle responses to emotional stimuli. These findings suggest altered processing of emotional information. Indeed, an appetitive response to any emotional stimuli (including aversive, appetitive, and alcohol-related pictures) could explain the association with alcohol-related problems observed in previous studies (Diaz et al., 2002; Dube et al., 2006; Hall et al., 2022; Kascakova et al., 2022; Sulejova et al., 2022).
Our first hypothesis considered that participants with more severe alcohol problems (i.e., heavy drinking and alcohol dependence) would show an attenuated startle response to emotional pictures. Alcohol dependents and heavy drinkers showed significantly reduced startle reflex responses to alcohol-related, appetitive, and aversive pictures compared to alcohol abusers and non-abusers (Fig. 2). However, alcohol abuse was positively correlated with increased startle reflex response to aversive and alcohol-related pictures (Fig. 5). These results are consistent with previous studies evaluating startling responses in the adult population with AUD (Grusser et al., 2002; Jurado-Barba et al., 2015; Jurado-Barba et al., 2017; Mucha et al., 2000; Rubio et al., 2013), suggesting that the greater the severity of the drinking problem, the greater the appetite for alcohol-associated stimuli (Jurado-Barba et al., 2017; Lemenager et al., 2014; Loeber et al., 2007).
The impact of a family history of alcoholism on the increased vulnerability to developing alcohol-related problems has been widely explored. Two recent large-scale observational studies suggested that parental alcohol problems increased the risk of offspring experiencing adversities during childhood (Haugland et al., 2021) and alcohol-related problems in adulthood (Haugland et al., 2021; Thor et al., 2022). Interestingly, another recent case-control study reported that family alcohol use increases the risk of developing an AUD to a greater extent than childhood trauma (Chen et al., 2021). In the sample of patients analyzed in this study, physical neglect, physical abuse, and sexual abuse were more associated with a familiar history of alcohol dependence (Table 1). On the other hand, young adults with alcohol dependence or heavy drinkers were the groups with the most significant proportion of parents with alcohol dependence (Table 1). Interestingly, the absence of maltreatment in the AFH group was strongly associated with alcohol abuse, indicating the importance of the familial history of consumption on alcohol misuse in adolescence (Fig. 5).
Our second hypothesis assumed that patients with an alcohol-dependent parent would have a reduced startle reflex, an effect that was indeed found, although it did not reach statistical significance (Fig. 4). The history of familial alcohol consumption also altered the correlation between the startle response to aversive, appetitive, and alcohol-related pictures, which was lower in the AFH than in the no AFH groups (Fig. 5A, B). Individual differences in startle reflex modulation in the offspring are not only controlled by genetic influences (heritability). Still, they would also be conceptualized as an environmentally mediated biological system (Vaidyanathan et al., 2014). Accordingly, altered emotional-related startle reactivity to environmental cues has been observed in young adults with a positive paternal history of alcoholism (Miranda Jr. et al., 2002; Rubio et al., 2013). Furthermore, the baseline acoustic startle response was lower in sons of alcoholics, while it was equally dampened by alcohol compared with participants without parental alcoholism (Zimmermann et al., 2004). Likewise, employing another psychophysiological paradigm such as electroencephalographic (EEG) recording, alterations in the processing of affective stimuli and alcohol-related information were shown in the offspring of alcohol-dependent patients (Dominguez-Centeno et al., 2020).
Exposure to adverse childhood experiences, including physical or psychological maltreatment, significantly increases the risk of initiating drug use during adolescence or adulthood (Alvarez-Alonso et al., 2016; Cicchetti & Handley, 2019; Diaz et al., 2002; Kascakova et al., 2022; Rogers et al., 2021), especially alcohol (Hall et al., 2022; Sulejova et al., 2022). Indeed, a previous study of our group showed that maternal deprivation in mice as a model of early life adverse experiences was critically associated with increased vulnerability to ethanol consumption in adolescence (Garcia-Gutierrez et al., 2016). Also, it is significant to mention that more adverse childhood experiences in nature, duration, and frequency are closely related to higher severity of alcohol consumption (Dube et al., 2006; Sulejova et al., 2022) or even polydrug use (Alvarez-Alonso et al., 2016; Diaz et al., 2002).
In this study, sexual abuse was strongly associated with alcohol dependence in AFH and no AFH groups (Fig. 5). According to the clinical characteristics of the participants of this study, sexual abuse was the kind of childhood maltreatment more closely linked to the most current harmful patterns of alcohol consumption (i.e., heavy drinking and alcohol dependence). In addition, 78.1 and 83.3% of young adults who suffered from emotional and physical abuse were classified as heavy drinkers (Table 1). This link between childhood abuse and alcohol-related problems could be explained by altered processing of emotional stimuli, especially for alcohol-related pictures.
Therefore, our third hypothesis was that participants with more severe childhood abuse would show attenuated startle responses. Indeed, participants who suffered sexual and physical abuse (the most severe forms of childhood abuse) showed the lowest startle responses to alcohol-related pictures compared with the control group (no abuse), as well as to aversive and appetitive cues (Fig. 3 and Table 2). Furthermore, sexual abuse was associated with reduced startle response to aversive and alcohol-related pictures (Fig. 5). These results are consistent with another study demonstrating that childhood trauma was associated with significantly reduced startle responses when anticipating negative images (Stout et al., 2021). However, when evaluating the baseline acoustic startle response (i.e., without the association with emotional-related pictures), high levels of physical or sexual abuse increased startle reflex. This may represent a possible biomarker of stress responsiveness as a long-lasting consequence of early trauma (Jovanovic et al., 2009). Recently, psychophysiological disturbances were identified by EEG recording in adolescents with problematic alcohol use exposed to childhood neglect (Nooner et al., 2022).
The mechanisms underlying the increased vulnerability to developing alcohol use problems due to child maltreatment and the alterations in emotional processing evidenced in this study are mainly unknown. Among the most recent evidence, a reduction of the structural connectivity of the amygdala could be pointed out in adult patients with a history of childhood trauma and a current diagnosis of AUD (Soravia et al., 2022). Moreover, smaller hippocampal and corpus callosum volumes appear closely linked to child abuse and psychophysiological response disturbances (Young et al., 2019).
One neurobiological phenomenon related is the impaired regulation of the HPA axis that modulates the stress response. Maltreated children are at risk for subsequent dysregulation of the HPA axis, enhancing the probability of developing psychopathology. Neuroendocrine disruption may also be critical in maltreated children’s liability for developing substance use disorders (SUD) (Cicchetti & Handley, 2019). This is consistent with the stress-incubation/corticolimbic developmental cascade hypothesis proposed by Andersen and Teicher, in which it is theorized that the link between early life adversity and SUD may be partially mediated by a highly reactive HPA axis and using substances to cope with negative affect (Andersen & Teicher, 2009). Future investigations into the complex relations between child maltreatment, neuroendocrine dysregulation, internalizing symptoms, and the development of SUD are necessary.
Limitations
The fact that our sample was composed of adolescents seeking treatment limits the extrapolation to other populations of consumers. Accounting that participants went to consultation accompanied by a relative, it is possible that only less severe maltreatment cases were accepted to complete the study, and those who perpetrated maltreatment were not their family members. Furthermore, retrospective data collection has the risk of enlarging or reducing past experiences.
The variable sex was not considered because many of the samples comprised men. Although it is assumed that it would not change the conclusions of this study, a larger sample size and more significant women representation should be considered in future studies. In addition, the variable “chronicity of abuse” was not collected, which could be a confounder.
Conclusions
According to the published literature, this is the first exploratory study conducted on a Mediterranean sample with these features. More than 600 adolescents from a clinical population were assessed to evaluate their startle response to emotional-related stimuli considering their familiar history of alcoholism, childhood trauma, and current alcohol consumption problems.
In light of the results obtained in this cross-sectional and retrospective observational study, the evaluation of emotional processing impairments in adolescents with problematic alcohol consumption, together with the anamnesis of family antecedents of alcoholism and history of maltreatment, should be considered a valuable diagnostic classification tool. Those participants with alcohol-dependent parents, exposed to childhood traumatic experiences, and developing more harmful consumption patterns displayed the most significant alterations in reducing the startle response. It is tempting to hypothesize that the combination of these factors may have a relevant impact on the vulnerability to chronic alcohol consumption during adulthood, a worse response to therapeutic approaches, or a greater susceptibility to relapse. Thus, evaluating these patients’ startle response could be considered a prognostic biomarker for establishing personalized preventive strategies during the adolescent stage to avoid, to a large extent, future problems derived from alcohol consumption.
References
Alvarez-Alonso, M. J., Jurado-Barba, R., Martinez-Martin, N., Espin-Jaime, J. C., Bolanos-Porrero, C., Ordonez-Franco, A., . . . Rubio, G. (2016). Association between maltreatment and polydrug use among adolescents. Child Abuse & Neglect, 51, 379-389. https://doi.org/10.1016/j.chiabu.2015.07.014
Andersen, S. L., & Teicher, M. H. (2009). Desperately driven and no brakes: Developmental stress exposure and subsequent risk for substance abuse. Neuroscience & Biobehavioral Reviews, 33(4), 516–524. https://doi.org/10.1016/j.neubiorev.2008.09.009
Baudin, G., Barrault, S., El Ayoubi, H., Kazour, F., Ballon, N., Mauge, D., . . . El-Hage, W. (2022). Childhood trauma and dissociation correlates in alcohol use disorder: A cross-sectional study in a sample of 587 French subjects hospitalized in a rehabilitation center. Brain Sciences, 12(11). https://doi.org/10.3390/brainsci12111483
Bernstein, D. P., Stein, J. A., Newcomb, M. D., Walker, E., Pogge, D., Ahluvalia, T., . . . Zule, W. (2003). Development and validation of a brief screening version of the Childhood Trauma Questionnaire. Child Abuse & Neglect, 27(2), 169-190. https://doi.org/10.1016/s0145-2134(02)00541-0
Blumenthal, T. D., Cuthbert, B. N., Filion, D. L., Hackley, S., Lipp, O. V., & van Boxtel, A. (2005). Committee report: Guidelines for human startle eyeblink electromyographic studies. Psychophysiology, 42(1), 1–15. https://doi.org/10.1111/j.1469-8986.2005.00271.x
Bollen, Z., Pabst, A., Masson, N., Billaux, P., D’Hondt, F., Deleuze, J., . . . Maurage, P. (2021). Alcohol-related attentional biases in recently detoxified inpatients with severe alcohol use disorder: An eye-tracking approach. Drug Alcohol Depend, 225, 108803. https://doi.org/10.1016/j.drugalcdep.2021.108803
Bradley, M., & Sabatinelli, D. (2003). Startle reflex modulation: Perception, attention and emotion. In K. Hugdahl (Ed.), Experimental methods in neuropsychology (pp. 65–88). Kluwer Academic Publishers.
Bradley, M. M., Cuthbert, B. N., & Lang, P. J. (1993). Pictures as prepulse: attention and emotion in startle modification. Psychophysiology, 30(5), 541–545. https://doi.org/10.1111/j.1469-8986.1993.tb02079.x
Chen, X., Pan, Y., Xu, P., Huang, Y., Li, N., & Song, Y. (2021). Family alcohol use, rather than childhood trauma, is more likely to cause male alcohol use disorder: Findings from a case-control study in northern China. BMC Psychiatry, 21(1), 555. https://doi.org/10.1186/s12888-021-03566-8
Cicchetti, D., & Handley, E. D. (2019). Child maltreatment and the development of substance use and disorder. Neurobiology of Stress, 10, 100144. https://doi.org/10.1016/j.ynstr.2018.100144
Das, U., Gangisetty, O., Chaudhary, S., Tarale, P., Rousseau, B., Price, J., . . . Sarkar, D. K. (2022). Epigenetic insight into effects of prenatal alcohol exposure on stress axis development: Systematic review with meta-analytic approaches. Alcoholism: Clinical and Experimental Research https://doi.org/10.1111/acer.14972
Diaz, A., Simantov, E., & Rickert, V. I. (2002). Effect of abuse on health: Results of a national survey. Archives of Pediatrics & Adolescent Medicine, 156(8), 811–817. https://doi.org/10.1001/archpedi.156.8.811
Dominguez-Centeno, I., Jurado-Barba, R., Sion, A., Martinez-Maldonado, A., Castillo-Parra, G., Lopez-Munoz, F., . . . Martinez-Gras, I. (2020). Psychophysiological correlates of emotional- and alcohol-related cues processing in offspring of alcohol-dependent patients. Alcohol Alcohol, 55(4), 374-381. https://doi.org/10.1093/alcalc/agaa006
Drugs, G. D. F. T. N. P. O. (2021). Spanish observatory on drugs and addictions. Monograph alcohol 2021. In Consumption and consequences. Ministerio de Sanidad.
Dube, S. R., Miller, J. W., Brown, D. W., Giles, W. H., Felitti, V. J., Dong, M., & Anda, R. F. (2006). Adverse childhood experiences and the association with ever using alcohol and initiating alcohol use during adolescence. Journal of Adolescent Health, 38(4), 444 e441-410. https://doi.org/10.1016/j.jadohealth.2005.06.006
Dutcher, C. D., Vujanovic, A. A., Paulus, D. J., & Bartlett, B. A. (2017). Childhood maltreatment severity and alcohol use in adult psychiatric inpatients: The mediating role of emotion regulation difficulties. General Hospital Psychiatry, 48, 42–50. https://doi.org/10.1016/j.genhosppsych.2017.06.014
Elmore, A. L., & Crouch, E. (2022). Anxiety, depression, and adverse childhood experiences: An update on risks and protective factors among children and youth. Academic Pediatrics. https://doi.org/10.1016/j.acap.2022.11.013
First, M. B., Spitzer, R. L., Gibbon, M., & Williams, J. B. W. (2002). Structured clinical interview for DSM-IV-TR axis I disorders, research version, non-patient edition. Biometrics Research, New York State Psychiatric Institute.
Garcia-Gutierrez, M. S., Navarrete, F., Aracil, A., Bartoll, A., Martinez-Gras, I., Lanciego, J. L., . . . Manzanares, J. (2016). Increased vulnerability to ethanol consumption in adolescent maternal separated mice. Addiction Biology, 21(4), 847-858. https://doi.org/10.1111/adb.12266
Genis-Mendoza, A. D., Dionisio-Garcia, D. M., Gonzalez-Castro, T. B., Tovilla-Zarate, C. A., Juarez-Rojop, I. E., Lopez-Narvaez, M. L., . . . Nicolini, H. (2022). Increased levels of cortisol in individuals with suicide attempt and its relation with the number of suicide attempts and depression. Frontiers in Psychiatry, 13, 912021. https://doi.org/10.3389/fpsyt.2022.912021
Goldstein, A. L., Henriksen, C. A., Davidov, D. M., Kimber, M., Pitre, N. Y., & Afifi, T. O. (2013). Childhood maltreatment, alcohol use disorders, and treatment utilization in a national sample of emerging adults. Journal of Studies on Alcohol and Drugs, 74(2), 185–194. https://doi.org/10.15288/jsad.2013.74.185
Goldstein, S. C., Schick, M. R., Weyandt, L. L., Sullivan, T. P., Saint-Eloi Cadely, H., & Weiss, N. H. (2022). Post-traumatic stress as a moderator of the association between HPA-axis functioning and alcohol use disorder among a community sample of women currently experiencing intimate partner violence. Experimental and Clinical Psychopharmacology. https://doi.org/10.1037/pha0000543
Grusser, S. M., Heinz, A., Raabe, A., Wessa, M., Podschus, J., & Flor, H. (2002). Stimulus-induced craving and startle potentiation in abstinent alcoholics and controls. European Psychiatry, 17(4), 188–193. https://doi.org/10.1016/s0924-9338(02)00666-1
Hall, O. T., Phan, K. L., & Gorka, S. (2022). Childhood adversity and the association between stress sensitivity and problematic alcohol use in adults. Journal of Traumatic Stress, 35(1), 148–158. https://doi.org/10.1002/jts.22709
Haugland, S. H., Carvalho, B., Stea, T. H., Strandheim, A., & Vederhus, J. K. (2021). Associations between parental alcohol problems in childhood and adversities during childhood and later adulthood: A cross-sectional study of 28047 adults from the general population. Substance Abuse Treatment, Prevention, and Policy, 16(1), 47. https://doi.org/10.1186/s13011-021-00384-9
Heinz, A., Lober, S., Georgi, A., Wrase, J., Hermann, D., Rey, E. R., . . . Mann, K. (2003). Reward craving and withdrawal relief craving: Assessment of different motivational pathways to alcohol intake. Alcohol Alcohol, 38(1), 35-39. https://doi.org/10.1093/alcalc/agg005
Hernandez, A., Gallardo-Pujol, D., Pereda, N., Arntz, A., Bernstein, D. P., Gaviria, A. M., . . . Gutierrez-Zotes, J. A. (2013). Initial validation of the Spanish childhood trauma questionnaire-short form: Factor structure, reliability and association with parenting. Journal of Interpersonal Violence, 28(7), 1498-1518. https://doi.org/10.1177/0886260512468240
Hill, S. Y., & O’Brien, J. (2015). Psychological and neurobiological precursors of alcohol use disorders in high risk youth. Current Addiction Reports, 2(2), 104–113. https://doi.org/10.1007/s40429-015-0051-1
Jin, Y., Xu, S., Wang, Y., Li, H., Wang, X., Sun, X., & Wang, Y. (2022). Associations between PTSD symptoms and other psychiatric symptoms among college students exposed to childhood sexual abuse: A network analysis. European Journal of Psychotraumatology, 13(2), 2141508. https://doi.org/10.1080/20008066.2022.2141508
Jovanovic, T., Blanding, N. Q., Norrholm, S. D., Duncan, E., Bradley, B., & Ressler, K. J. (2009). Childhood abuse is associated with increased startle reactivity in adulthood. Depress Anxiety, 26(11), 1018–1026. https://doi.org/10.1002/da.20599
Jurado-Barba, R., Duque, A., Lopez-Trabada, J. R., Martinez-Gras, I., Garcia-Gutierrez, M. S., Navarrete, F., . . . Rubio, G. (2017). The modulation of the startle reflex as predictor of alcohol use disorders in a sample of heavy drinkers: A 4-year follow-up study. Alcoholism: Clinical and Experimental Research, 41(6), 1212-1219. https://doi.org/10.1111/acer.13399
Jurado-Barba, R., Rubio Valladolid, G., Martinez-Gras, I., Alvarez-Alonso, M. J., Ponce Alfaro, G., Fernandez, A., . . . Jimenez-Arriero, M. A. (2015). Changes on the modulation of the startle reflex in alcohol-dependent patients after 12 weeks of a cognitive-behavioral intervention. European Addiction Research, 21(4), 195-203. https://doi.org/10.1159/000371723
Kalivas, P. W., Sorg, B. A., & Hooks, M. S. (1993). The pharmacology and neural circuitry of sensitization to psychostimulants. Behavioural Pharmacology, 4(4), 315–334.
Kang, D., Bresin, K., & Fairbairn, C. E. (2018). The impact of alcohol and social context on the startle eyeblink reflex. Alcoholism: Clinical and Experimental Research, 42(10), 1951–1960. https://doi.org/10.1111/acer.13838
Kascakova, N., Petrikova, M., Furstova, J., Hasto, J., Geckova, A. M., & Tavel, P. (2022). Associations of childhood trauma with long-term diseases and alcohol and nicotine use disorders in Czech and Slovak representative samples. BMC Public Health, 22(1), 1769. https://doi.org/10.1186/s12889-022-14160-2
Kaufman, J., Birmaher, B., Brent, D., Rao, U., Flynn, C., Moreci, P., . . . Ryan, N. (1997). Schedule for affective disorders and schizophrenia for school-age children—present and lifetime version (K-SADS-PL): Initial reliability and validity data. Journal of the American Academy of Child & Adolescent Psychiatry, 36(7), 980-988. https://doi.org/10.1097/00004583-199707000-00021
Keller, J., Gomez, R., Williams, G., Lembke, A., Lazzeroni, L., Murphy, G. M., Jr., & Schatzberg, A. F. (2017). HPA axis in major depression: cortisol, clinical symptomatology and genetic variation predict cognition. Molecular Psychiatry, 22(4), 527–536. https://doi.org/10.1038/mp.2016.120
Kisely, S., Mills, R., Strathearn, L., & Najman, J. M. (2020). Does child maltreatment predict alcohol use disorders in young adulthood? A cohort study of linked notifications and survey data. Addiction, 115(1), 61–68. https://doi.org/10.1111/add.14794
Lang, P. J., Bradley, M. M., & Cuthbert, B. N. (1997). In P. J. Lang & B. RF (Eds.), Motivated attention: Affect, activation and action. Erlbaum.
Lang, P. J., Bradley, M. M., & Cuthbert, B. N. (2005). International affective picture system (IAPS). Affective ratings of pictures and instruction manual. Technical Report, A-6
Lee, J. Y., Brook, J. S., Nezia, N., & Brook, D. W. (2016). Adolescent predictors of alcohol use in adulthood: A 22-year longitudinal study. The American Journal on Addictions, 25(7), 549–556. https://doi.org/10.1111/ajad.12438
Lemenager, T., Hill, H., Reinhard, I., Hoffmann, S., Zimmermann, U. S., Hermann, D., . . . Mann, K. (2014). Association between alcohol-cue modulated startle reactions and drinking behaviour in alcohol dependent patients—Results of the PREDICT study. International Journal of Psychophysiology, 94(3), 263-271. https://doi.org/10.1016/j.ijpsycho.2014.09.009
Loeber, S., Croissant, B., Nakovics, H., Zimmer, A., Georgi, A., Klein, S., . . . Flor, H. (2007). The startle reflex in alcohol-dependent patients: Changes after cognitive-behavioral therapy and predictive validity for drinking behavior. A pilot study. Psychotherapy and Psychosomatics, 76(6), 385-390. https://doi.org/10.1159/000107567
Lotzin, A., Haupt, L., von Schonfels, J., Wingenfeld, K., & Schafer, I. (2016). Profiles of childhood trauma in patients with alcohol dependence and their associations with addiction-related problems. Alcoholism: Clinical and Experimental Research, 40(3), 543–552. https://doi.org/10.1111/acer.12990
McCambridge, J., McAlaney, J., & Rowe, R. (2011). Adult consequences of late adolescent alcohol consumption: A systematic review of cohort studies. PLoS Medicine, 8(2), e1000413. https://doi.org/10.1371/journal.pmed.1000413
Meaney, M. J., Brake, W., & Gratton, A. (2002). Environmental regulation of the development of mesolimbic dopamine systems: A neurobiological mechanism for vulnerability to drug abuse? Psychoneuroendocrinology, 27(1-2), 127–138. https://doi.org/10.1016/s0306-4530(01)00040-3
Mereish, E. H., & Miranda, R., Jr. (2021). A preliminary experimental study of minority stress, startle reactivity, and alcohol use among heavy drinking sexual minority young adults. Substance Use & Misuse, 56(1), 162–168. https://doi.org/10.1080/10826084.2020.1846197
Miranda, R., Jr., Meyerson, L. A., Buchanan, T. W., & Lovallo, W. R. (2002). Altered emotion-modulated startle in young adults with a family history of alcoholism. Alcoholism: Clinical and Experimental Research, 26(4), 441–448.
Moltó, J., Segarra, P., López, R., Esteller, À., Fonfría, A., Pastor, M. C., & Poy, R. (2013). Adaptación española del “International Affective Picture System” (IAPS). Anales de Psicología, 29(3), 965–984. https://doi.org/10.6018/analesps.29.3.153591
Moore, K. E., Oberleitner, L. M. S., Zonana, H. V., Buchanan, A. W., Pittman, B. P., Verplaetse, T. L., . . . McKee, S. A. (2019). Psychiatric disorders and crime in the US population: Results from the National Epidemiologic Survey on Alcohol and Related Conditions Wave III. The Journal of Clinical Psychiatry, 80(2). https://doi.org/10.4088/JCP.18m12317
Mucha, R. F., Geier, A., Stuhlinger, M., & Mundle, G. (2000). Appetitve effects of drug cues modelled by pictures of the intake ritual: Generality of cue-modulated startle examined with inpatient alcoholics. Psychopharmacology (Berl), 151(4), 428–432. https://doi.org/10.1007/s002130000508
Murray, L., Welsh, J. C., Johnson, C. G., Kaiser, R. H., Farchione, T. J., & Janes, A. C. (2022). Alcohol- and non-alcohol-related interference: An fMRI study of treatment-seeking adults with alcohol use disorder. Drug and Alcohol Dependence, 235, 109462. https://doi.org/10.1016/j.drugalcdep.2022.109462
Nooner, K. B., Meiers, G., Treadwell, T., & Butler, L. B. (2022). Changes in electroencephalography alpha associated with childhood neglect and adolescent alcohol use. Child Maltreatment, 10775595221098029. https://doi.org/10.1177/10775595221098029
Obeid, S., Akel, M., Haddad, C., Fares, K., Sacre, H., Salameh, P., & Hallit, S. (2020). Factors associated with alcohol use disorder: The role of depression, anxiety, stress, alexithymia and work fatigue—A population study in Lebanon. BMC Public Health, 20(1), 245. https://doi.org/10.1186/s12889-020-8345-1
Ostroumov, A., Thomas, A. M., Kimmey, B. A., Karsch, J. S., Doyon, W. M., & Dani, J. A. (2016). Stress increases ethanol self-administration via a shift toward excitatory GABA signaling in the ventral tegmental area. Neuron, 92(2), 493–504. https://doi.org/10.1016/j.neuron.2016.09.029
Poznyak, V., & Rekve, D. (Eds.). (2018). Global status report on alcohol and health 2018. World Health Organization.
Rehan, W., Antfolk, J., Johansson, A., Jern, P., & Santtila, P. (2017). Experiences of severe childhood maltreatment, depression, anxiety and alcohol abuse among adults in Finland. PLoS One, 12(5), e0177252. https://doi.org/10.1371/journal.pone.0177252
Roberts, W., & Fillmore, M. T. (2015). Attentional bias to alcohol-related stimuli as an indicator of changes in motivation to drink. Psychology of Addictive Behaviors, 29(1), 63–70. https://doi.org/10.1037/adb0000005
Rogers, C. J., Forster, M., Grigsby, T. J., Albers, L., Morales, C., & Unger, J. B. (2021). The impact of childhood trauma on substance use trajectories from adolescence to adulthood: Findings from a longitudinal Hispanic cohort study. Child Abuse & Neglect, 120, 105200. https://doi.org/10.1016/j.chiabu.2021.105200
Rogers, C. J., Pakdaman, S., Forster, M., Sussman, S., Grigsby, T. J., Victoria, J., & Unger, J. B. (2022). Effects of multiple adverse childhood experiences on substance use in young adults: A review of the literature. Drug and Alcohol Dependence, 234, 109407. https://doi.org/10.1016/j.drugalcdep.2022.109407
Rossow, I., Keating, P., Felix, L., & McCambridge, J. (2016). Does parental drinking influence children’s drinking? A systematic review of prospective cohort studies. Addiction, 111(2), 204–217. https://doi.org/10.1111/add.13097
Rubio, G., Borrell, J., Jimenez, M., Jurado, R., Grusser, S. M., & Heinz, A. (2013). Variables involved in the cue modulation of the startle reflex in alcohol-dependent patients. Addiction Biology, 18(1), 170–180. https://doi.org/10.1111/j.1369-1600.2011.00371.x
Ryan, S. M., Jorm, A. F., & Lubman, D. I. (2010). Parenting factors associated with reduced adolescent alcohol use: A systematic review of longitudinal studies. Australian and New Zealand Journal of Psychiatry, 44(9), 774–783. https://doi.org/10.1080/00048674.2010.501759
Sapolsky, R. M., Romero, L. M., & Munck, A. U. (2000). How do glucocorticoids influence stress responses? Integrating permissive, suppressive, stimulatory, and preparative actions. Endocrine Reviews, 21(1), 55–89. https://doi.org/10.1210/edrv.21.1.0389
Schupp, H. T., Cuthbert, B. N., Bradley, M. M., Birbaumer, N., & Lang, P. J. (1997). Probe P3 and blinks: Two measures of affective startle modulation. Psychophysiology, 34(1), 1–6. https://doi.org/10.1111/j.1469-8986.1997.tb02409.x
Schwandt, M. L., Heilig, M., Hommer, D. W., George, D. T., & Ramchandani, V. A. (2013). Childhood trauma exposure and alcohol dependence severity in adulthood: Mediation by emotional abuse severity and neuroticism. Alcoholism: Clinical and Experimental Research, 37(6), 984–992. https://doi.org/10.1111/acer.12053
Shalev, A. Y., Peri, T., Brandes, D., Freedman, S., Orr, S. P., & Pitman, R. K. (2000). Auditory startle response in trauma survivors with post-traumatic stress disorder: A prospective study. American Journal of Psychiatry, 157(2), 255–261. https://doi.org/10.1176/appi.ajp.157.2.255
Shin, S. H., Jiskrova, G. K., & Wills, T. A. (2019). Childhood maltreatment and alcohol use in young adulthood: The role of self-regulation processes. Addictive Behaviors, 90, 241–249. https://doi.org/10.1016/j.addbeh.2018.11.006
Shin, S. H., Wang, X., Yoon, S. H., Cage, J. L., Kobulsky, J. M., & Montemayor, B. N. (2019). Childhood maltreatment and alcohol-related problems in young adulthood: The protective role of parental warmth. Child Abuse & Neglect, 98, 104238. https://doi.org/10.1016/j.chiabu.2019.104238
Smit, K., Zucker, R. A., & Kuntsche, E. (2022). Exposure to parental alcohol use is associated with adolescent drinking even when accounting for alcohol exposure of best friend and peers. Alcohol and Alcoholism, 57(4), 483–489. https://doi.org/10.1093/alcalc/agab081
Soravia, L. M., Denier, N., Moggi, F., Grieder, M., Federspiel, A., Tschuemperlin, R. M., . . . Bracht, T. (2022). Reduced structural connectivity of the amygdala is associated with childhood trauma in adult patients with alcohol use disorder. Addiction Biology, 27(3), e13164. https://doi.org/10.1111/adb.13164
Spanagel, R., Noori, H. R., & Heilig, M. (2014). Stress and alcohol interactions: Animal studies and clinical significance. Trends in Neurosciences, 37(4), 219–227. https://doi.org/10.1016/j.tins.2014.02.006
Spanish Drugs and Addictions Observatory. (2021). Technical Report 2021. Consumption and consequences. Spanish Alcohol Report.
Stout, D. M., Powell, S., Kangavary, A., Acheson, D. T., Nievergelt, C. M., Kash, T., . . . Risbrough, V. B. (2021). Dissociable impact of childhood trauma and deployment trauma on affective modulation of startle. Neurobiology of Stress, 15, 100362. https://doi.org/10.1016/j.ynstr.2021.100362
Sulejova, K., Liska, D., Liptakova, E., Szantova, M., Patarak, M., Koller, T., . . . Skladany, L. (2022). Relationship between alcohol consumption and adverse childhood experiences in college students—A cross-sectional study. Frontiers in Psychology, 13, 1004651. https://doi.org/10.3389/fpsyg.2022.1004651
Swerdlow, N. R., Caine, S. B., Braff, D. L., & Geyer, M. A. (1992). The neural substrates of sensorimotor gating of the startle reflex: A review of recent findings and their implications. Journal of Psychopharmacology, 6(2), 176–190. https://doi.org/10.1177/026988119200600210
Tan, G. K. Y., Symons, M., Fitzpatrick, J., Connor, S. G., Cross, D., & Pestell, C. F. (2022). Adverse childhood experiences, associated stressors and comorbidities in children and youth with fetal alcohol spectrum disorder across the justice and child protection settings in Western Australia. BMC Pediatrics, 22(1), 587. https://doi.org/10.1186/s12887-022-03654-y
Thor, S., Hemmingsson, T., Danielsson, A. K., & Landberg, J. (2022). Fathers’ alcohol consumption and risk of substance-related disorders in offspring. Drug and Alcohol Dependence, 233, 109354. https://doi.org/10.1016/j.drugalcdep.2022.109354
Vaidyanathan, U., Malone, S. M., Miller, M. B., McGue, M., & Iacono, W. G. (2014). Heritability and molecular genetic basis of acoustic startle eye blink and affectively modulated startle response: A genome-wide association study. Psychophysiology, 51(12), 1285–1299. https://doi.org/10.1111/psyp.12348
Vila, J. S. M., Ramirez, I., Fernández, M. C., Cobos, P., & Rodriguez, S. (2001). El Sistema Internacional de Imágenes Afectivas (IAPS) Adaptación española. Revista de Psicología Aplicada, 54, 635–657.
Wahlstrom, J., Magnusson, C., Laftman, S. B., & Svensson, J. (2023). Parents’ drinking, childhood hangover? Parental alcohol use, subjective health complaints and perceived stress among Swedish adolescents aged 10-18 years. BMC Public Health, 23(1), 162. https://doi.org/10.1186/s12889-023-15097-w
Walsh, A. T., Carmel, D., & Grimshaw, G. M. (2019). Reward elicits cognitive control over emotional distraction: Evidence from pupillometry. Cognitive, Affective, & Behavioral Neuroscience, 19(3), 537–554. https://doi.org/10.3758/s13415-018-00669-w
Wang, P., Xie, X., Chen, M., Zhang, N., Wang, W., Ma, S., . . . Liu, Z. (2022). Measuring childhood trauma in young adults with depression: A latent profile analysis. Asian Journal of Psychiatry, 80, 103387. https://doi.org/10.1016/j.ajp.2022.103387
White, H. R., & Widom, C. S. (2008). Three potential mediators of the effects of child abuse and neglect on adulthood substance use among women. Journal of Studies on Alcohol and Drugs, 69(3), 337–347. https://doi.org/10.15288/jsad.2008.69.337
Wietschorke, K., Lippold, J., Jacob, C., Polak, T., & Herrmann, M. J. (2016). Transcranial direct current stimulation of the prefrontal cortex reduces cue-reactivity in alcohol-dependent patients. Journal of Neural Transmission, 123(10), 1173–1178. https://doi.org/10.1007/s00702-016-1541-6
Wilkins, D. E., Hallett, M., & Wess, M. M. (1986). Audiogenic startle reflex of man and its relationship to startle syndromes A review. Brain, 109(Pt 3), 561–573. https://doi.org/10.1093/brain/109.3.561
Wilson, H. W., & Widom, C. S. (2009). A prospective examination of the path from child abuse and neglect to illicit drug use in middle adulthood: The potential mediating role of four risk factors. Journal of Youth and Adolescence, 38(3), 340–354. https://doi.org/10.1007/s10964-008-9331-6
Yang, W., Singla, R., Maheshwari, O., Fontaine, C. J., & Gil-Mohapel, J. (2022). Alcohol use disorder: Neurobiology and therapeutics. Biomedicines, 10(5). https://doi.org/10.3390/biomedicines10051192
Young, D. A., Neylan, T. C., Chao, L. L., O’Donovan, A., Metzler, T. J., & Inslicht, S. S. (2019). Child abuse interacts with hippocampal and corpus callosum volume on psychophysiological response to startling auditory stimuli in a sample of veterans. Journal of Psychiatric Research, 111, 16–23. https://doi.org/10.1016/j.jpsychires.2019.01.011
Young-Wolff, K. C., Enoch, M. A., & Prescott, C. A. (2011). The influence of gene-environment interactions on alcohol consumption and alcohol use disorders: A comprehensive review. Clinical Psychology Review, 31(5), 800–816. https://doi.org/10.1016/j.cpr.2011.03.005
Zimmermann, U., Spring, K., Wittchen, H. U., & Holsboer, F. (2004). Effects of ethanol administration and induction of anxiety-related affective states on the acoustic startle reflex in sons of alcohol-dependent fathers. Alcoholism: Clinical and Experimental Research, 28(3), 424–432. https://doi.org/10.1097/01.alc.0000117835.49673.cf
Acknowledgements
The authors would like to thank Victoria Fornes Ferrer for her help in the statistical analyses.
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Contributions
GR and AD performed material preparation and data collection. GR, AD, and JM wrote the first draft of the manuscript, and all authors commented on previous versions. GR, AD, MSGG, FN, AG, DN, and JM participated in the manuscript writing. All the authors critically reviewed, and JM approved the final version of the manuscript.
Corresponding author
Ethics declarations
Consent to Participate
All procedures followed the ethical standards and the Helsinki Declaration of 1975, revised in 2000. All participants signed informed consent to be part of the study. Approval of the protocol by appropriate local ethics committees was also secured.
Conflict of Interest
The authors declare no competing interests.
Statements
The preparation of the manuscript was supported by “Instituto de Salud Carlos III” (RD. PI18/00576) and RD21/0009/0008 “Red de Investigación en Atención Primaria de Adicciones”) to Jorge Manzanares.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Rubio, G., Gasparyan, A., Duque, A. et al. Emotional Processing and Maltreatment During Childhood as Factors of Vulnerability to Alcohol Abuse in Young Adults. Int J Ment Health Addiction (2023). https://doi.org/10.1007/s11469-023-01097-9
Accepted:
Published:
DOI: https://doi.org/10.1007/s11469-023-01097-9