Abstract
Background
Role of core stability exercises in ACL rehabilitation program is not well studied.
Purpose
To study the effect of addition of core stability exercise on outcome of ACL reconstruction surgery.
Materials and methods
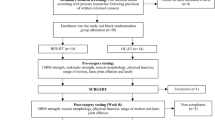
Ninety-two male sportspersons (18–40 years) who underwent ACL reconstruction were enrolled in the study. Sportspersons were divided into two groups depending upon the computer-generated random number sequence—group A (conventional rehabilitation; n = 46) and group B (core stabilization + conventional rehabilitation; n = 46). All sportspersons were assessed at 6, 9 and 12 months for the functional outcome (IKDC score, single hop test, triple hop test, and VAS score), return to sports, and knee laxity (KT-1000).
Results
IKDC scores were higher in group B as compared to group A at all follow-ups (p < 0.05). Similarly, single and triple hop test jump distances were wider in group B as compared to group A at all the follow-ups (p < 0.05). Incidence of return to sports was significantly higher in group B (35/45) as compared to group A (24/43; p = 0.02). Mean time to return to sports was 10.77 ± 1.7 months in group A and 9.44 ± 1.8 in group B (p = 0.006). There was no difference in knee laxity between the two groups.
Conclusion
The addition of core stability exercises in the ACL rehabilitation program results in better functional outcome and early return to sports. However, core stability exercises have no effect on knee stability.
Study design
Level III, prospective observational study.

Similar content being viewed by others
References
Kibler WB, Press J, Sciascia A (2006) The role of core stability in athletic function. Sports Med 36(3):189–198
Willson JD, Dougherty CP, Ireland ML, Davis IM (2005) Core stability and its relationship to lower extremity function and injury. J Am Acad Orthop Surg 13(5):316–325
Vleeming A, Pool-Goudzwaard A, Stoeckart R, van Wingerden J-P, Snijders C (1995) The posterior layer of the thoracolumbar fascia. Spine 20(7):753–758
Gupta R, Kapoor A, Khatri S, Masih GD (2019) Anterior cruciate ligament tear due to non-contact mode of injury associated with higher incidence of meniscal and chondral damage. J Clin Orthop Trauma 11(3):342–434
Hewett TE, Myer GD, Ford KR, Heidt RS Jr, Colosimo AJ, McLean SG, van den Bogert AJ, Paterno MV, Succop P (2005) Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: a prospective study. Am J Sports Med 33(4):492–501
Malinzak RA, Colby SM, Kirkendall DT, Yu B, Garrett WE (2001) A comparison of knee joint motion patterns between men and women in selected athletic tasks. Clin Biomech 16(5):438–445
Hewett TE, Myer GD, Ford KR, Heidt RS Jr, ColosimoMcLeanSuccop AJP (2005) Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: a prospective study. Am J Sports Med 33(4):492–501
Zazulak BT, Hewett TE, Peter Reeves N, Goldberg B, Cholewicki J (2007) Deficits in neuromuscular control of the trunk predict knee injury risk: prospective biomechanical-epidemiologic study. Am J Sports Med 35(7):1123–1130
Nyland J, Burden R, Krupp R, Caborn DNM (2011) Whole body, long-axis rotational training improves lower extremity neuromuscular control during single leg lateral drop landing and stabilization. Clin Biomech 26(4):363–370
Khayambashi K, Ghoddosi N, Straub RK, Powers CM (2016) Hip muscle strength predicts noncontact anterior cruciate ligament injury in male and female athletes: a prospective study. Am J Sports Med 44(2):355–361
Powers CM (2010) The influence of abnormal hip mechanics on knee injury: a biomechanical perspective. J Orthop Sports Phys Ther 40(2):42–51
Hewett TE, Myer GD, Ford KR et al (2005) Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: a prospective study. Am J Sports Med 33(4):492–501
Mehl J, Diermeier T, Herbst E, Imhoff AB, Stoffels T, Zantop T, Achtnich A (2018) Evidence-based concepts for prevention of knee and ACL injuries. 2017 guidelines of the ligament committee of the German Knee Society (DKG). Arch Orthop Trauma Surg 138(1):51–61
Leetun DT, Ireland ML, Willson JD, Ballantyne BT, Davis IM (2004) Core stability measures as risk factors for lower extremity injury in athletes. Med Sci Sports Exerc 36(6):926–934
Silvers-Granelli H, Mandelbaum B, Adeniji O, Insler S, Bizzini M, Pohlig R, Dvorak J (2015) Efficacy of the FIFA 11+ injury prevention program in the collegiate male soccer player. Am J Sports Med 43(11):2628–2637
Silvers-Granelli HJ, Bizzini M, Arundale A, Mandelbaum BR, Snyder-Mackler L (2017) Does the FIFA 11+ injury prevention program reduce the incidence of ACL injury in male soccer players? Clin Orthop Relat Res 475(10):2447–2455
Relph N, Herrington L, Tyson S (2014) The effects of ACL injury on knee proprioception: a meta-analysis. Physiotherapy 100(3):187–195
Vaugoyeau M, Viel S, Amblard B, Azulay JP, Assaiante C (2008) Proprioceptive contribution of postural control as assessed from very slow oscillations of the support in healthy humans. Gait Posture 27(2):294–302
Tecco S, Salini V, Calvisi V et al (2006) Effects of anterior cruciate ligament (ACL) injury on postural control and muscle activity of head, neck and trunk muscles. J Oral Rehabil 33(8):576–587
Werner DM, Barrios JA (2018) Trunk muscle endurance in individuals with and without a history of anterior cruciate ligament reconstruction. J Strength Cond Res. https://doi.org/10.1519/JSC.0000000000002395
Escamilla RF, Lewis C, Bell D et al (2010) Core muscle activation during Swiss ball and traditional abdominal exercises. J Orthop Sports Phys Ther 40(5):265–276
Cugliari G, Boccia G (2017) Core muscle activation in suspension training exercises. J Hum Kinet 56:61–71
Boyle M (2004) Functional training for sports. Hum Kinet
Vera-Garcia FJ, Grenier SG, McGill SM (2000) Abdominal muscle response during curl-ups on both stable and labile surfaces. Phys Therapy 80(6):564–569
Gambetta V (1999) Let’s get physio: for swim-specific weight training, get on the ball It’s easy with our simple but effective physioball routine. Rodales Fit Swim 8(3):30–33
Shi D-L, Li J-L, Zhai H, Wang H-F, Meng H, Wang Y-B (2012) Specialized core stability exercise: a neglected component of anterior cruciate ligament rehabilitation programs. J Back Musculoskelet 25(4):291–297
Myer GD, Ford KR, OP P, Hewett TE (2005) Neuromuscular training improves performance and lower-extremity biomechanics in female athletes. J Strength Cond Res 19(1):51–60
Roetert P (2001) 3D balance and core stabilty. High-performance sports conditioning: modern training for ultimate athletic development. Hum Kinet 7:119–138
Stanton R, Reaburn PR, Humphries B (2004) The effect of short-term Swiss ball training on core stability and running economy. J Strength Cond Res 18(3):522–528
Tse MA, McManus AM, Masters RS (2005) Development and validation of a core endurance intervention program: implications for performance in college-age rowers. J Strength Cond Res 19(3):547–552
Jin ZH et al (2008) The role of core stability in athletic function. J Beijing Sports Univ 12:039
Hodges PW, Richardson CA (1997) Contraction of the abdominal muscles associated with movement of the lower limb. Phys Therapy 77(2):132–142
Cinar-Medeni O, Baltaci G, Bayramlar K, Yanmis I (2015) Core stability, knee muscle strength, and anterior translation are correlated with postural stability in anterior cruciate ligament-reconstructed patients. Am J Phys Med Rehabil 94(4):280–287
Nesser TW, Huxel KC, Tincher JL, Okada T (2008) The relationship between core stability and performance in division I football players. J Strength Cond Res 22(6):1750–2175
Chaudhari AM, McKenzie CS, Borchers JR, Best TM (2011) Lumbopelvic control and pitching performance of professional baseball pitchers. J Strength Cond Res 25(8):2127–2132
Ozmen T (2016) Relationship between core stability, dynamic balance and jumping performance in soccer players. Turk J Sport Exerc 18(1):110–113
Yabroudi MA, Irrgang JJ (2003) Rehabilitation and return to play after anatomic anterior cruciate ligament reconstruction. Clin Sports Med 32(1):165–175
Bien DP, Dubuque TJ (2005) Considerations for late stage ACL rehabilitation and return to sport to limit re-injury risk and maximize athletic performance. Int J Sports Phys Therapy 10(2):256
Van Grinsven S et al (2010) Evidence-based rehabilitation following anterior cruciate ligament reconstruction. Knee Surg Sport Traumatol Arthrosc 18(8):1128–1144
Bigoni M, Turati M (2017) Healing potential and surgical treatment of anterior cruciate ligament rupture in pediatric population. Sport Sci Health 13(3):645–646
Hinterwimmer S et al (2003) Operative or conservative treatment of anterior cruciate ligament rupture: a systematic review of the literature. Unfallchirurg 106(5):374–379
Awad OB, Alqarni SAM, Alkhalaf HM et al (2017) A systematic review of ACL reconstruction rehabilitation. Egypt J Hosp Med 68(1):845–864
Naik AA, Das B, Kamat YD (2019) Avoid post operative bracing to reduce ACL rerupture rates. Eur J Orthop Surg Traumatol 29(8):1743–1747
Janssen RP, Van Melick N, Van Mourik JB, Reijman M, van Rhijn LW (2018) ACL reconstruction with hamstring tendon autograft and accelerated brace-free rehabilitation: a systematic review of clinical outcomes. BMJ Open Sport Exerc Med 4(1):e000301
Ardern CL et al (2018) 2018 International Olympic Committee consensus statement on prevention, diagnosis and management of paediatric anterior cruciate ligament (ACL) injuries. Br J Sports Med 52(7):422–438
Pedersen MT, Randers MB, Skotte JH, Krustrup P (2009) Recreational soccer can improve the reflex response to sudden trunk loading among untrained women. J Strength Cond Res 23(9):2621–2626
Steve T, McNeilan RJ, Young GS, Givens DL, Best TM, Chaudhari AMW (2012) Randomized controlled trial of the effects of a trunk stabilization program on trunk control and knee loading. Med Sci Sports Exerc 44(10):1924–1934
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest for any author exist.
Ethical approval
This study was approved by the institutional ethical committee (GMCH, Chandigarh).
Informed consent
Written and informed consent was received from all the patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gupta, R., Rana, S., Kapoor, A. et al. Better and early recovery in ACL reconstructed elite players with addition of core stability exercises in postoperative rehabilitation program. Sport Sci Health 17, 357–362 (2021). https://doi.org/10.1007/s11332-020-00696-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11332-020-00696-6