Abstract
Background
Infections in patients with chronic kidney disease (CKD) are a major cause of hospitalization. The pharmacokinetics of renally eliminated antibiotics may lead to drug accumulation, resulting in potential toxicity. The renal dosing adjustment of antibiotics is crucial to avoid toxicity and decrease mortality. In Lebanon, limited data are available on antibiotic dose adequacy in CKD.
Objectives
To estimate the prevalence of inappropriately dosed antibiotics in non-dialysis CKD patients and to identify possible risk factors that may be associated with unadjusted renal dosing.
Methods
A retrospective chart review was conducted at two tertiary-care hospitals in Lebanon. International Statistical Classification of Diseases (ICD-10) code for CKD was used to search the databases. Demographic and clinical data were collected for patients who received antibiotics that requires renal dosing adjustment. Lexi-Comp online Drug Information database was the guideline used to evaluate the appropriateness of dosing.
Results
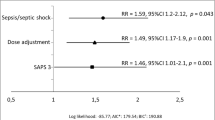
A total of 495 antibiotic orders were dispensed to 190 patients. 51.6% of patients received antibiotics without renal dose adjustments. The most inappropriately dosed class was penicillins (39.8%), while fluoroquinolones were the most adequately adjusted. Piperacillin/tazobactam was the most frequently prescribed drug (30.6%) without renal dose adjustment. Respiratory infections (OR 1.301, CI 95% 1.327–1.915) and multimorbidity (OR 1.183, CI 95% 1.358–2.081) were statistically highly significant associations for unadjusted antibiotic dosing from the fitted multivariable-adjusted logistic models.
Conclusion
Our study revealed a high frequency of guideline-discordant antibiotic dosing in patients with CKD. This dosing error is preventable by increasing awareness of prescribing physicians and collaborating with clinical pharmacists.
Similar content being viewed by others
Availability of data and materials
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
SPSS version 25 institutional license.
References
GBD Chronic Kidney Disease Collaboration (2020) Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 395(10225):709–733. https://doi.org/10.1016/S0140-6736(20)30045-3
Chang CH, Fan PC, Kuo G et al (2020) Infection in advanced chronic kidney disease and subsequent adverse outcomes after dialysis initiation: a nationwide cohort study. Sci Rep. 10(1):2938. https://doi.org/10.1038/s41598-020-59794-7 (Published 2020 Feb 19)
Morales-Alvarez MC (2020) Nephrotoxicity of antimicrobials and antibiotics. Adv Chronic Kidney Dis 27(1):31–37. https://doi.org/10.1053/j.ackd.2019.08.001
Lea-Henry TN, Carland JE, Stocker SL, Sevastos J, Roberts DM (2018) CJASN 13(7):1085–1095. https://doi.org/10.2215/CJN.00340118
Kocyigit I, Dortdudak S, Sipahioglu M et al (2012) Levofloxacin-induced delirium: is it a dangerous drug in patients with renal dysfunction? Ren Fail 34(5):634–636. https://doi.org/10.3109/0886022X.2012.660855
Roberts JA, Paul SK, Akova M et al (2014) DALI: defining antibiotic levels in intensive care unit patients: are current β-lactam antibiotic doses sufficient for critically ill patients? Clin Infect Dis 58(8):1072–1083. https://doi.org/10.1093/cid/ciu027
Lam SW, Eschenauer GA (2007) Identifying patients at risk of chronic kidney disease. Am Fam Physician 76:1454
Matzke GR, Dowling TC, Marks SA, Murphy JE (2016) Influence of kidney disease on drug disposition: an assessment of industry studies submitted to the FDA for new chemical entities 1999–2010. J Clin Pharmacol 56(4):390–398
Michels WM, Grootendorst DC, Verduijn M, Elliott EG, Dekker FW, Krediet RT (2010) Performance of the Cockcroft-Gault, MDRD, and new CKD-EPI formulas in relation to GFR, age, and body size. Clin J Am Soc Nephrol 5(6):1003–1009
Lew AK, Crass RL, Eschenauer G (2020) Evolution of equations for estimating renal function and their application to the dosing of new antimicrobials. Ann Pharmacother 54(5):496–503. https://doi.org/10.1177/1060028019890346
Hudson JQ, Nolin TD (2018) Pragmatic use of kidney function estimates for drug dosing: the tide is turning. Adv Chronic Kidney Dis 25(1):14–20. https://doi.org/10.1053/j.ackd.2017.10.003
Gallieni M, Cancarini G (2015) Drugs in the elderly with chronic kidney disease: beware of potentially inappropriate medications. Nephrol Dial Transpl 30:342–344
Bennett WM, Aronoff GR, Morrison G et al (1983) Drug prescribing in renal failure: dosing guidelines for adults. Am J Kidney Dis 3(3):155–193
Saleem A, Masood I (2016) Pattern and predictors of medication dosing errors in chronic kidney disease patients in pakistan: a single center retrospective analysis. PLoS ONE 11(7):e0158677. https://doi.org/10.1371/journal.pone.0158677 (Published 2016 Jul 1)
Sweileh WM, Janem SA, Sawalha AF et al (2007) Medication dosing errors in hospitalized patients with renal impairment: a study in Palestine. Pharmacoepidemiol Drug Saf 16(8):908–912. https://doi.org/10.1002/pds.1412
Laville SM, Gras-Champel V, Moragny J, Metzger M, Jacquelinet C, Combe C, Fouque D, Laville M, Frimat L, Robinson BM, Stengel B, Massy ZA, Liabeuf S, on behalf of the Chronic Kidney Disease-Renal Epidemiology and Information Network (CKD-REIN) Study Group CJASN 15(8):1090–1102; https://doi.org/10.2215/CJN.01030120
Hall WH, Ramachandran R, Narayan S, Jani AB, Vijayakumar S (2004) An electronic application for rapidly calculating Charlson comorbidity score. BMC Cancer 4:94. https://doi.org/10.1186/1471-2407-4-94
Wolters Kluwer. Lexicomp. Database. https://www.wolterskluwercdi.com/lexicomp-online/. Accessed 19 Aug 2020
Jang SM, Lewis SJ, Mueller BA (2020) Harmonizing antibiotic regimens with renal replacement therapy. Expert Rev Anti Infect Ther 18(9):887–895. https://doi.org/10.1080/14787210.2020.1764845
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group (2013) KDIGO clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int Suppl. 3:1–150
Jarab F, Jarab AS, Mukattash TL, Nusairat B, Alshogran OY (2020) Antibiotic dosing adjustments in patients with declined kidney function at a tertiary hospital in Jordan. Int J Clin Pract 74(10):e13579. https://doi.org/10.1111/ijcp.13579
Silva M, Dias G, Cardoso T (2020) Estimated Creatinine Clearance and Glomerular Filtration Rate in Very Elderly Patients and Antibiotic Prescribing Errors: Cohort Study [published online ahead of print, 2020 Jul 29]. Acta Med Port. 2020;https://doi.org/10.20344/amp.12408. https://doi.org/10.20344/amp.12408
Reza A, Maini M, Hossein S (2019) Evaluation of antibiotic dose adjustment based on glomerular filtration rate in Patients who were admitted to rasool-akram hospital, Tehran, in 6months of 2015. J Adv Pharm Edu Res 9(S):183–187
Zeenny R, Nasr Z, Adaimy I (2014) Retrospective evaluation of the appropriate use of Piperacillin/Tazobactam in a tertiary care teaching hospital in Lebanon. Acta Medica Mediterranea 30(3):655–663
Alsaleh NA, Al-Omar HA, Mayet AY, Mullen AB (2020) Evaluating the appropriateness of carbapenem and piperacillin-tazobactam prescribing in a tertiary care hospital in Saudi Arabia. Saudi Pharm J 28(11):1492–1498. https://doi.org/10.1016/j.jsps.2020.09.015
Fahimi F, Emami S, Rashid FF (2012) The rate of antibiotic dosage adjustment in renal dysfunction. Iran J Pharm Res 11(1):157–161
Morimoto T, Nagashima H, Morimoto Y, Tokuyama S (2017) Frequency of acute kidney injury caused by Tazobactam/Piperacillin in patients with pneumonia and chronic kidney disease: a retrospective observational study. Yakugaku Zasshi 137(9):1129–1136. https://doi.org/10.1248/yakushi.17-00002
Tesfaye WH, Castelino RL, Wimmer BC et al (2017) Inappropriate prescribing in chronic kidney disease: a systematic review of prevalence, associated clinical outcomes and impact of interventions. Int J Clin Pract 71(7):e12960
Fiore DC, Fettic LP, Wright SD, Ferrara BR (2017) Antibiotic overprescribing: Still a major concern. J Fam Pract 66(12):730–736
van Dijk EA, Drabbe NR, Kruijtbosch M, De Smet PA (2006) Drug dosage adjustments according to renal function at hospital discharge. Ann Pharmacother 40(7–8):1254–1260. https://doi.org/10.1345/aph.1G742
Kulwicki BD, Brandt KL, Wolf LM, Weise AJ, Dumkow LE (2019) Impact of an emergency medicine pharmacist on empiric antibiotic prescribing for pneumonia and intra-abdominal infections. Am J Emerg Med 37(5):839–844. https://doi.org/10.1016/j.ajem.2018.07.052
Hassan Y, Al-Ramahi RJ, Aziz NA, Ghazali R (2009) Impact of a renal drug dosing service on dose adjustment in hospitalized patients with chronic kidney disease. Ann Pharmacother 43(10):1598–1605. https://doi.org/10.1345/aph.1M187
Jiang SP, Zhu ZY, Ma KF, Zheng X, Lu XY (2013) Impact of pharmacist antimicrobial dosing adjustments in septic patients on continuous renal replacement therapy in an intensive care unit. Scand J Infect Dis 45(12):891–899. https://doi.org/10.3109/00365548.2013.827338
Aloy B, Launay-Vacher V, Bleibtreu A et al (2020) Antibiotics and chronic kidney disease: dose adjustment update for infectious disease clinical practice. Med Mal Infect 50(4):323–331. https://doi.org/10.1016/j.medmal.2019.06.010
Funding
No sources of funding were used in the preparation of this study.
Author information
Authors and Affiliations
Contributions
All authors were involved in the conception or design of the analysis, interpretation of data, drafting the manuscript or revising it critically for important intellectual content, and final approval of the version to be published.
Corresponding author
Ethics declarations
Conflicts of interest
The author declares no conflict of interest.
Ethics approval
Ethical approval was obtained for the study (Ref: INV-2017–306).
Consent to participate
Not applicable.
Consent to publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chahine, B. Antibiotic dosing adjustments in hospitalized patients with chronic kidney disease: a retrospective chart review. Int Urol Nephrol 54, 157–163 (2022). https://doi.org/10.1007/s11255-021-02834-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-021-02834-6