Abstract
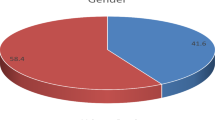
Fungal infection of the external auditory canal (otitis externa and otomycosis) is a chronic, acute, or subacute superficial mycotic infection that rarely involves middle ear. Otomycosis (swimmer’s ear) is usually unilateral infection and affects more females than males. The infection is usually symptomatic and main symptoms are pruritus, otalgia, aural fullness, hearing impairment, otorrhea, and tinnitus. Fungal species such as yeasts, molds, dermatophytes, and Malassezia species are agents for otitis externa. Among molds, Aspergillus niger was described as the most common agent in the literature. Candida albicans was more prevalent than other yeast species. Otomycosis has a worldwide distribution, but the prevalence of infection is related to the geographical location, areas with tropical and subtropical climate showing higher prevalence rates. Otomycosis is a secondary infection and is more prevalent among swimmers. As a result, a higher incidence is reported in summer season, when more people interested in swimming. Incidence of otomycosis in our review ranged from 5.7 to 81 %, with a mean value of 51.3 %. Our results showed that 78.59 % of otomycosis agents were Aspergillus, 16.76 % were Candida species, and the rest (4.65 %) were other saprophytic fungi. Among Iranian patients, incidence of infection was highest in summer, followed by autumn, winter, and spring. In Iran, otomycosis was most prevalent at the age of 20–40 years and the lowest prevalence was associated with being <10 years old. The sex ratio of otomycosis in our study was (M/F) 1:1.53.







Similar content being viewed by others
References
Bineshian F, Irajian G, Koochak-Alavi SK, Fredonian MR. A study on the frequency of fungal agents in otitis externa in Semnan. Iran J Pathol. 2006;1(4):141–4.
Saki N, Rafiei A, Nikakhlagh S, Amirrajab N, Saki S. Prevalence of otomycosis in Khouzestan province, south-west Iran. J Laryngol Otol. 2013;127(01):25–7.
Munguia R, Daniel SJ. Ototopical antifungals and otomycosis: a review. Int J Pediatr Otorhinolaryngol. 2008;72(4):453–9.
Nowrozi H, Arabi FD, Mehraban HG, Tavakoli A, Ghooshchi G. Mycological and clinical study of otomycosis in Tehran, Iran. Bull Environ Pharmacol Life Sci. 2014;3(2):29–31.
Barati B, Okhovvat S, Goljanian A, Omrani M. Otomycosis in central iran: a clinical and mycological study. Iran Red Crescent Med J. 2011;13(12):873–6.
Vennewald I, Klemm E. Otomycosis: diagnosis and treatment. Clin Dermatol. 2010;28(2):202–11.
Jia X, Liang Q, Chi F, Cao W. Otomycosis in Shanghai: aetiology, clinical features and therapy. Mycoses. 2012;55(5):404–9.
Elahi S, Zaini F. First case report of otomycosis due to hendersonula toruloidea. Acta Med Iran. 1994;32:131–5.
Pakshir K, Sabayan B, Javan H, Karamifar K. Mycoflora of human external auditory canal in Shiraz, southern Iran. Iran Red Crescent Med J. 2008;10(1):27–9.
Kazemi AH, Ghiaei S. Survey of otomycosis in north-western area of Iran, 1997–2004. J Manzandaran Univ Med Sci. 2005;48:112–9.
Shokoohi T, Ahanjan M, Kasiri AM. Bacteriological and mycological study of external otitis in patients referred to ENT clinic of Boo Ali Sina hospital in Sari in summer 1999. J Mazandran Uni Med Sci. 2001;21:1–10.
Viswanatha B, Sumatha D, Vijayashree MS. Otomycosis in immunocompetent and immunocompromised patients: comparative study and literature review. Ear Nose Throat J. 2012;91(3):114–21.
Yeganeh Mogadam A, Asadi MA, Dehghani R, Hooshyar H. The prevalence of otomycosis in Kashan, Iran, during 2001–2003. Jundishapur J Microbiol. 2011;2(1):18–21.
Sheikh MS, Qazi B, Rameen B. Otomycosis in Khozistan. Indian J Otolaryngol Head Neck Surg. 1993;45(2):73–7.
Prasad SC, Kotigadde S, Shekhar M, Thada ND, Prabhu P, D’Souza T. et al. (2014) Primary otomycosis in the Indian subcontinent: predisposing factors, microbiology, and classification. Int J Microbiol. 2014:Article ID 636493
Anwar K, Gohar MS. Otomycosis; clinical features, predisposing factors and treatment implications. Pak J Med Sci. 2014;30(3):564–7.
Latha R, Sasikala R, Muruganandam N. Chronic otomycosis due to Malassezia spp. J Global Infect Dis. 2010;2(2):189–90.
Sephidgar A, Kyakajouri K, Meyrzaei M, Sharifi F. Fungal infections of external ear canal in patients with otomycosis, Babol, 1991–2001. J Babol Med Sci. 2002;4(1):25–9.
Zarei Mahmoudabadi A, Abshirini H, Rahimi R. Fungal flora of hearing aid moulds and ear canal in hearing aid wearers in school children in Ahvaz, Iran. Jundishapur J Microbiol. 2009;2(1):22–4.
Zarei Mahmoudabadi A, Masoomi SA, Mohammadi H. Clinical and mycological studies of otomycosis. Pak J Med Sci. 2010;26(1):187–90.
Kaur R, Mittal N, Kakkar M, Aggarwal AK, Mathur MD. Otomycosis: a clinicomycologic study. Ear Nose Throat J. 2000;79(8):606–9.
Sturgulewski SK, Bankaitis A, Klodd DA, Haberkamp T. What’s still growing on your patients’ hearing aids? Hear J. 2006;59(9):45–6.
Ozcan KM, Ozcan M, Karaarslan A, Karaarslan F. Otomycosis in Turkey: predisposing factors, aetiology and therapy. J Laryngol Otol. 2003;117(01):39–42.
Paulose K, Khalifa SA, Shenoy P, Sharma R. Mycotic infection of the ear (otomycosis): a prospective study. J Laryngol Otol. 1989;103(01):30–5.
Jackman A, Ward R, April M, Bent J. Topical antibiotic induced otomycosis. Int J Pediatr Otorhinolaryngol. 2005;69(6):857–60.
Ghiacei S. Survey of otomycosis in north-western area of Iran. Med J Mashhad Univ Med Sci. 2001;43:85–7.
Pontes ZBVdS, Silva ADF, Lima EDO, Guerra MDH, Oliveira NMC, Carvalho MDFFP, et al. Otomycosis: a retrospective study. Braz J Otorhinolaryngol. 2009;75(3):367–70.
Szigeti G, Sedaghati E, Zarei Mahmoudabadi A, Naseri A, Kocsube S, Vágvölgyi C, et al. Species assignment and antifungal susceptibilities of black aspergilli recovered from otomycosis cases in Iran. Mycoses. 2012;55(4):333–8.
Kiakojuri K, Roushan MRH, Sepidgar SAA. Suction clearance and 2 % topical miconazole versus the same combination with acidic drops in the treatment of otomycosis. Southeast Asian J Trop Med Public Health. 2007;38:749–53.
Chadeganipour M, Shadzi S, Nilipour S, Ahmadi G. Airborne fungi in Isfahan and evaluation of allergenic responses of their extracts in animal model. Jundishapur J Microbiol. 2011;3(4):155–60.
Rajabnia R, Mahdavi Omran S, Majidian A, Aghajanpour S, Kiakojori K. Comparison of fungal flora in patients with acute otitis externa and healthy subjects. J Babol Univ Med Sci. 2010;12(3):32–7.
Moharram AM, Ahmed HE, Salma AMN. Otomycosis in Assiut, Egypt. J Basic Appl Mycol (Egypt). 2013;4:1–11.
Değerli K, Ecemiş T, Günhan K, Başkesen T, Kal E. Agents of otomycosis in Manisa region, Turkey, 1995–2011. Mikrobiyol Bul. 2012;46(1):79–87.
García-Agudo L, Aznar-Marín P, Galán-Sánchez F, García-Martos P, Marín-Casanova P, Rodríguez-Iglesias M. Otomycosis due to filamentous fungi. Mycopathologia. 2011;172(4):307–10.
Badr Jabir H, Naeem Abbas F, Muhsin Khalaf R. In vitro assessment of antifungal potential of apple cider vinegar and acetic acid versus fluconazole in clinical isolates of otomycosis. Thi Qar Med J. 2011;5(1):126–33.
Fayemiwo S, Ogunleye V, Adeosun A, Bakare R. Prevalence of otomycosis in Ibadan: a review of laboratory reports. Afr J Med Med Sci. 2010;39:219–22.
Kiakojuri K, Rajabnia R, Jalili B, Khafri S, Mahdavi Omran SS. Otomycosis in adolescent patients who referred to therapeutical centers, Babol, report of 56 cases. Jundishapur J Microbiol 2015;8:17138 (in press).
Berjis N, Okhovat SA, Soleimani Koujani Z, Baradaran S. Comparing the therapeutic effect of clotrimazole and tolnaftate in treating the variety of fungal species producing otomycosis in two educational hospital, Isfahan, Iran. J Isfahan Med Sch. 2012;29(164):2117–26.
Ettehad GH, Refahi S, Nemmati A, Pirzadeh A, Daryani A. Microbial and antimicrobial susceptibility patterns from patients with chronic otitis media in Ardebil. Int J Trop Med. 2006;1(2):62–5.
Mikaeili A, Nazari S. Aspergillus and otomycosis in Kermanshah Iran. 5th Advances against Aspergillosis, 26–28 January 2012—Istanbul, Turkey. 2012
Balouchi M, Berjis N, Okhovat A. Investigation of ear fungal infection. J Isfahan Med Sch. 2006;82(4):72–5.
Nemati S, Hassanzadeh R, Jahromi SK, Abadi ADN. Otomycosis in the north of Iran: common pathogens and resistance to antifungal agents. Eur Arch Otorhino Laryngol. 2014;271(5):953–7.
Kiakojuri K, Roushan MRH, Sepidgar SAA. Suction clearance and 2% topical miconazole versus the same combination with acidic drops in the treatment of otomycosis. Southeast Asian J Trop Med Public Health. 2007;38:749–53.
Afshari MA, Kachooei R, Ajalloeian M. Assessment of prevalence of otomycosis in ENT clinic in Baqiyatallah (AS) hospital. J Mil Med. 2005;2:121–4.
Jalali MM, Kousha AAR, Hashemi SJ, Forghan Parast K, Karimi HR. Frequency of fungi in the middle ear effusion of patients suffering from serous otitis media in Rasht Amiralmomenin hospital (2004–2005). J Ilam Univ Med Sci. 2006;14(1):39–43.
Zarei Mahmoudabadi A. Mycological studies in 15 cases of otomycosis. Pak J Med Sci. 2006;22(4):486–8.
Yaganeh Moghadam A, Asadi M, Dehghani R, Zarei Mahmoudabadi A, Rayegan F, Hooshyar H, Khorshidi A. Evaluating the effect of a mixture of alcohol and acetic acid for otomycosis therapy. Jundishapur J Microbiol. 2010;3(2):66–70.
Desai KJ, Malek SS, Italia IK, Jha S, Pndya V, Shah H. Fungal spectrum in otomycosis at tertiary care hospital. Natl J Integr Res Med. 2012;3(5):58–61.
Aneja K, Sharma C, Joshi R. Fungal infection of the ear: a common problem in the north eastern part of Haryana. Int J Pediatr Otorhinolaryngol. 2010;74(6):604–7.
Adoubryn K, N’gattia V, Kouadio-Yapo G, Nigué L, Zika D, Ouhon J. Epidemiology of otomycoses at the university hospital of Yopougon (Abidjan-Ivory Coast). J Mycol Med. 2014;24(2):e9–15.
Deshmukh J, Surpam R, Band A, Jalgaon KD, India M. Mycological study of Aspergillus infections in otomycosis in eastern part of Maharashtra. Int J Health Sci Res. 2014;4(10):77–82.
Gutiérrez PH, Álvarez SJ, Sanudo E, García LG-C, Sánchez CR, VallejoValdezate L. Presumed diagnosis: otomycosis. A study of 451 patients. Acta Otorrinolaringol Esp. 2005;56:181–6.
Panchal P, Pethani J, Patel D, Rathod S, Shah P. Analysis of various fungal agents in clinically suspected cases of otomycosis. Indian J Basic Appl Med Res. 2013;2:865–9.
Zarei Mahmoudabadi A, Seifi Z, Gharaghani M. Lamisil, a potent alternative antifungal drug for otomycosis. Adv Med Mycol. 2015;1(1):18–21.
Sagit M, Somdas MA, Korkmaz F, Akcadag A. The ototoxic effect of intratympanic terbinafine applied in the middle ear of rats. J Otolaryngol Head Neck Surg. 2013;42(1):13.
Alnawaiseh S, Almomani O, Alassaf S, Elessis A, Shawakfeh N, Altubeshi K, et al. Treatment of otomycosis: a comparative study using miconazole cream with clotrimazole otic drops. J Roy Med Serv. 2011;18(3):34–7.
Philip A, Thomas R, Job A, Sundaresan VR, Anandan S, Albert RR. Effectiveness of 7.5 percent povidone iodine in comparison to 1 percent clotrimazole with lignocaine in the treatment of otomycosis. ISRN Otolaryngol. 2013. doi:10.1155/2013/239730.
Zarei Mahmoudabadi A, Abshirini H, Ahmadi K, Moghimipour E. Lamisil ear drop, a newly prepared antifungal for otomycosis treatment. In: The 3rd Iranian Congress of Clinical Microbiology (ICCM), Shiraz, Iran, 6–8 Oct, 2009. (Abstract book), p. 40.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gharaghani, M., Seifi, Z. & Zarei Mahmoudabadi, A. Otomycosis in Iran: A Review. Mycopathologia 179, 415–424 (2015). https://doi.org/10.1007/s11046-015-9864-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-015-9864-7