Abstract
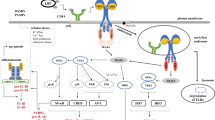
Necroptosis is considered a programmed necrosis that requires receptor-interacting protein kinase 1 (RIPK1), receptor-interacting protein kinase 3 (RIPK3), and pore-forming mixed lineage kinase domain-like protein (MLKL) to trigger a regulated cell membrane lysis. Membrane rupture in necroptosis has been shown to fuel innate immune response due to release of damage-associated molecular patterns (DAMPs). Recently published studies indicate that mature erythrocytes can undergo necroptosis as well. In this review, we provide an outline of multiple cell death modes occurring in erythrocytes, discuss possible immunological aspects of diverse erythrocyte cell deaths, summarize available evidence related to the ability of erythrocytes to undergo necroptosis, outline key involved molecular mechanisms, and discuss the potential implication of erythrocyte necroptosis in the physiology and pathophysiology. Furthermore, we aim to highlight the interplay between necroptosis and eryptosis signaling in erythrocytes, emphasizing specific characteristics of these pathways distinct from their counterparts in nucleated cells. Thus, our review provides a comprehensive summary of the current knowledge of necroptosis in erythrocytes. To reflect critical differences between necroptosis of nucleated cells and necroptosis of erythrocytes, we suggest a term erythronecroptosis for necroptosis of enucleated cells.



Similar content being viewed by others
Data availability
Not applicable.
References
Galluzzi L, Bravo-San Pedro JM, Vitale I, Aaronson SA, Abrams JM, Adam D, Alnemri ES, Altucci L, Andrews D, Annicchiarico-Petruzzelli M, Baehrecke EH, Bazan NG, Bertrand MJ, Bianchi K, Blagosklonny MV, Blomgren K, Borner C, Bredesen DE, Brenner C, Campanella M, Candi E, Cecconi F, Chan FK, Chandel NS, Cheng EH, Chipuk JE, Cidlowski JA, Ciechanover A, Dawson TM, Dawson VL, De Laurenzi V, De Maria R, Debatin KM, Di Daniele N, Dixit VM, Dynlacht BD, El-Deiry WS, Fimia GM, Flavell RA, Fulda S, Garrido C, Gougeon ML, Green DR, Gronemeyer H, Hajnoczky G, Hardwick JM, Hengartner MO, Ichijo H, Joseph B, Jost PJ, Kaufmann T, Kepp O, Klionsky DJ, Knight RA, Kumar S, Lemasters JJ, Levine B, Linkermann A, Lipton SA, Lockshin RA, López-Otín C, Lugli E, Madeo F, Malorni W, Marine JC, Martin SJ, Martinou JC, Medema JP, Meier P, Melino S, Mizushima N, Moll U, Muñoz-Pinedo C, Nuñez G, Oberst A, Panaretakis T, Penninger JM, Peter ME, Piacentini M, Pinton P, Prehn JH, Puthalakath H, Rabinovich GA, Ravichandran KS, Rizzuto R, Rodrigues CM, Rubinsztein DC, Rudel T, Shi Y, Simon HU, Stockwell BR, Szabadkai G, Tait SW, Tang HL, Tavernarakis N, Tsujimoto Y, Vanden Berghe T, Vandenabeele P, Villunger A, Wagner EF, Walczak H, White E, Wood WG, Yuan J, Zakeri Z, Zhivotovsky B, Melino G, Kroemer G (2015) Essential versus accessory aspects of cell death: recommendations of the NCCD 2015. Cell Death Differ 22:58–73. https://doi.org/10.1038/cdd.2014.137
Kerr JF, Wyllie AH, Currie AR (1972) Apoptosis: a basic biological phenomenon with wide-ranging implications in tissue kinetics. Br J Cancer 26:239–257. https://doi.org/10.1038/bjc.1972.33
Mishchenko T, Balalaeva I, Gorokhova A, Vedunova M, Krysko DV (2022) Which cell death modality wins the contest for photodynamic therapy of cancer? Cell Death Dis 13:455. https://doi.org/10.1038/s41419-022-04851-4
D’Arcy MS (2019) Cell death: a review of the major forms of apoptosis, necrosis and autophagy. Cell Biol Int 43:582–592. https://doi.org/10.1002/cbin.11137
Galluzzi L, Vitale I, Aaronson SA, Abrams JM, Adam D, Agostinis P, Alnemri ES, Altucci L, Amelio I, Andrews DW, Annicchiarico-Petruzzelli M, Antonov AV, Arama E, Baehrecke EH, Barlev NA, Bazan NG, Bernassola F, Bertrand MJM, Bianchi K, Blagosklonny MV, Blomgren K, Borner C, Boya P, Brenner C, Campanella M, Candi E, Carmona-Gutierrez D, Cecconi F, Chan FK, Chandel NS, Cheng EH, Chipuk JE, Cidlowski JA, Ciechanover A, Cohen GM, Conrad M, Cubillos-Ruiz JR, Czabotar PE, D’Angiolella V, Dawson TM, Dawson VL, De Laurenzi V, De Maria R, Debatin KM, DeBerardinis RJ, Deshmukh M, Di Daniele N, Di Virgilio F, Dixit VM, Dixon SJ, Duckett CS, Dynlacht BD, El-Deiry WS, Elrod JW, Fimia GM, Fulda S, García-Sáez AJ, Garg AD, Garrido C, Gavathiotis E, Golstein P, Gottlieb E, Green DR, Greene LA, Gronemeyer H, Gross A, Hajnoczky G, Hardwick JM, Harris IS, Hengartner MO, Hetz C, Ichijo H, Jäättelä M, Joseph B, Jost PJ, Juin PP, Kaiser WJ, Karin M, Kaufmann T, Kepp O, Kimchi A, Kitsis RN, Klionsky DJ, Knight RA, Kumar S, Lee SW, Lemasters JJ, Levine B, Linkermann A, Lipton SA, Lockshin RA, López-Otín C, Lowe SW, Luedde T, Lugli E, MacFarlane M, Madeo F, Malewicz M, Malorni W, Manic G, Marine JC, Martin SJ, Martinou JC, Medema JP, Mehlen P, Meier P, Melino S, Miao EA, Molkentin JD, Moll UM, Muñoz-Pinedo C, Nagata S, Nuñez G, Oberst A, Oren M, Overholtzer M, Pagano M, Panaretakis T, Pasparakis M, Penninger JM, Pereira DM, Pervaiz S, Peter ME, Piacentini M, Pinton P, Prehn JHM, Puthalakath H, Rabinovich GA, Rehm M, Rizzuto R, Rodrigues CMP, Rubinsztein DC, Rudel T, Ryan KM, Sayan E, Scorrano L, Shao F, Shi Y, Silke J, Simon HU, Sistigu A, Stockwell BR, Strasser A, Szabadkai G, Tait SWG, Tang D, Tavernarakis N, Thorburn A, Tsujimoto Y, Turk B, Vanden Berghe T, Vandenabeele P, Vander Heiden MG, Villunger A, Virgin HW, Vousden KH, Vucic D, Wagner EF, Walczak H, Wallach D, Wang Y, Wells JA, Wood W, Yuan J, Zakeri Z, Zhivotovsky B, Zitvogel L, Melino G, Kroemer G (2018) Molecular mechanisms of cell death: recommendations of the Nomenclature Committee on Cell Death 2018. Cell Death Differ 25:486–541. https://doi.org/10.1038/s41418-017-0012-4
Franko J, Pomfy M, Prosbová T (2000) Apoptosis and cell death (mechanisms, pharmacology and promise for the future). Acta Med (Hradec Kralove) 43:63–68
Cookson BT, Brennan MA (2001) Pro-inflammatory programmed cell death. Trends Microbiol 9:113–114. https://doi.org/10.1016/s0966-842x(00)01936-3
Brinkmann V, Reichard U, Goosmann C, Fauler B, Uhlemann Y, Weiss DS, Weinrauch Y, Zychlinsky A (2004) Neutrophil extracellular traps kill bacteria. Science 303:1532–1535. https://doi.org/10.1126/science.1092385
Degterev A, Huang Z, Boyce M, Li Y, Jagtap P, Mizushima N, Cuny GD, Mitchison TJ, Moskowitz MA, Yuan J (2005) Chemical inhibitor of nonapoptotic cell death with therapeutic potential for ischemic brain injury. Nat Chem Biol 1:112–119. https://doi.org/10.1038/nchembio711
Overholtzer M, Mailleux AA, Mouneimne G, Normand G, Schnitt SJ, King RW, Cibas ES, Brugge JS (2007) A nonapoptotic cell death process, entosis, that occurs by cell-in-cell invasion. Cell 131:966–979. https://doi.org/10.1016/j.cell.2007.10.040
Andrabi SA, Dawson TM, Dawson VL (2008) Mitochondrial and nuclear cross talk in cell death: parthanatos. Ann N Y Acad Sci 1147:233–241. https://doi.org/10.1196/annals.1427.014
Dixon SJ, Lemberg KM, Lamprecht MR, Skouta R, Zaitsev EM, Gleason CE, Patel DN, Bauer AJ, Cantley AM, Yang WS, Morrison B 3rd, Stockwell BR (2012) Ferroptosis: an iron-dependent form of nonapoptotic cell death. Cell 149:1060–1072. https://doi.org/10.1016/j.cell.2012.03.042
Tsvetkov P, Coy S, Petrova B, Dreishpoon M, Verma A, Abdusamad M, Rossen J, Joesch-Cohen L, Humeidi R, Spangler RD, Eaton JK, Frenkel E, Kocak M, Corsello SM, Lutsenko S, Kanarek N, Santagata S, Golub TR (2022) Copper induces cell death by targeting lipoylated TCA cycle proteins. Science 375:1254–1261. https://doi.org/10.1126/science.abf0529
Tkachenko A, Onishchenko A (2023) Zincoptosis: does it exist? Apoptosis. https://doi.org/10.1007/s10495-023-01836-2
Koren E, Fuchs Y (2021) Modes of regulated cell death in cancer. Cancer Discov 11:245–265. https://doi.org/10.1158/2159-8290.Cd-20-0789
Peng F, Liao M, Qin R, Zhu S, Peng C, Fu L, Chen Y, Han B (2022) Regulated cell death (RCD) in cancer: key pathways and targeted therapies. Signal Transduct Target Ther 7:286. https://doi.org/10.1038/s41392-022-01110-y
Cui J, Zhao S, Li Y, Zhang D, Wang B, Xie J, Wang J (2021) Regulated cell death: discovery, features and implications for neurodegenerative diseases. Cell Commun Signal 19:120. https://doi.org/10.1186/s12964-021-00799-8
Aits S, Jäättelä M (2013) Lysosomal cell death at a glance. J Cell Sci 126:1905–1912. https://doi.org/10.1242/jcs.091181
Wang F, Gómez-Sintes R, Boya P (2018) Lysosomal membrane permeabilization and cell death. Traffic 19:918–931. https://doi.org/10.1111/tra.12613
Bock FJ, Tait SWG (2020) Mitochondria as multifaceted regulators of cell death. Nat Rev Mol Cell Biol 21:85–100. https://doi.org/10.1038/s41580-019-0173-8
Lang F, Qadri SM (2012) Mechanisms and significance of eryptosis, the suicidal death of erythrocytes. Blood Purif 33:125–130. https://doi.org/10.1159/000334163
Pretorius E, du Plooy JN, Bester J (2016) A comprehensive review on eryptosis. Cell Physiol Biochem 39:1977–2000. https://doi.org/10.1159/000447895
Tkachenko A, Onishchenko A (2022) Casein kinase 1α mediates eryptosis: a review. Apoptosis. https://doi.org/10.1007/s10495-022-01776-3
von Petersdorff-Campen K, Schmid Daners M (2022) Hemolysis Testing in vitro: a review of challenges and potential improvements. Asaio J 68:3–13. https://doi.org/10.1097/mat.0000000000001454
Tkachenko A, Onishchenko A, Myasoedov V, Yefimova S, Havranek O (2023) Assessing regulated cell death modalities as an efficient tool for in vitro nanotoxicity screening: a review. Nanotoxicology. https://doi.org/10.1080/17435390.2023.2203239
Alghareeb SA, Alfhili MA, Fatima S (2023) Molecular mechanisms and pathophysiological significance of eryptosis. Int J Mol Sci. https://doi.org/10.3390/ijms24065079
LaRocca TJ, Stivison EA, Hod EA, Spitalnik SL, Cowan PJ, Randis TM, Ratner AJ (2014) Human-specific bacterial pore-forming toxins induce programmed necrosis in erythrocytes. mBio 5:e01251-14. https://doi.org/10.1128/mBio.01251-14
Corrons JLV, Casafont LB, Frasnedo EF (2021) Concise review: how do red blood cells born, live, and die? Ann Hematol 100:2425–2433. https://doi.org/10.1007/s00277-021-04575-z
Thiagarajan P, Parker CJ, Prchal JT (2021) How do red blood cells die? Front Physiol. https://doi.org/10.3389/fphys.2021.655393
Zhang Q, Hu XM, Zhao WJ, Ban XX, Li Y, Huang YX, Wan H, He Y, Liao LS, Shang L, Jiang B, Qing GP, Xiong K (2023) Targeting Necroptosis: a novel therapeutic option for retinal degenerative diseases. Int J Biol Sci 19:658–674. https://doi.org/10.7150/ijbs.77994
Kaiser WJ, Sridharan H, Huang C, Mandal P, Upton JW, Gough PJ, Sehon CA, Marquis RW, Bertin J, Mocarski ES (2013) Toll-like receptor 3-mediated necrosis via TRIF, RIP3, and MLKL. J Biol Chem 288:31268–31279. https://doi.org/10.1074/jbc.M113.462341
Dhuriya YK, Sharma D (2018) Necroptosis: a regulated inflammatory mode of cell death. J Neuroinflammation 15:199. https://doi.org/10.1186/s12974-018-1235-0
Ye K, Chen Z, Xu Y (2023) The double-edged functions of necroptosis. Cell Death Dis 14:163. https://doi.org/10.1038/s41419-023-05691-6
Liu C, Zhang K, Shen H, Yao X, Sun Q, Chen G (2018) Necroptosis: a novel manner of cell death, associated with stroke (Review). Int J Mol Med 41:624–630. https://doi.org/10.3892/ijmm.2017.3279
Yan J, Wan P, Choksi S, Liu ZG (2022) Necroptosis and tumor progression. Trends Cancer 8:21–27. https://doi.org/10.1016/j.trecan.2021.09.003
Martens S, Bridelance J, Roelandt R, Vandenabeele P, Takahashi N (2021) MLKL in cancer: more than a necroptosis regulator. Cell Death Differ 28:1757–1772. https://doi.org/10.1038/s41418-021-00785-0
Liccardi G, Annibaldi A (2023) MLKL post-translational modifications: road signs to infection, inflammation and unknown destinations. Cell Death Differ 30:269–278. https://doi.org/10.1038/s41418-022-01061-5
Murao A, Aziz M, Wang H, Brenner M, Wang P (2021) Release mechanisms of major DAMPs. Apoptosis 26:152–162. https://doi.org/10.1007/s10495-021-01663-3
Bertheloot D, Latz E, Franklin BS (2021) Necroptosis, pyroptosis and apoptosis: an intricate game of cell death. Cell Mol Immunol 18:1106–1121. https://doi.org/10.1038/s41423-020-00630-3
Orning P, Lien E (2021) Multiple roles of caspase-8 in cell death, inflammation, and innate immunity. J Leukoc Biol 109:121–141. https://doi.org/10.1002/jlb.3mr0420-305r
Malireddi RKS, Kesavardhana S, Kanneganti TD (2019) ZBP1 and TAK1: master regulators of NLRP3 Inflammasome/pyroptosis, apoptosis, and necroptosis (PAN-optosis). Front Cell Infect Microbiol 9:406. https://doi.org/10.3389/fcimb.2019.00406
Jiang M, Qi L, Li L, Wu Y, Song D, Li Y (2021) Caspase-8: a key protein of cross-talk signal way in “PANoptosis” in cancer. Int J Cancer 149:1408–1420. https://doi.org/10.1002/ijc.33698
Roberts JZ, Crawford N, Longley DB (2022) The role of ubiquitination in apoptosis and necroptosis. Cell Death Differ 29:272–284. https://doi.org/10.1038/s41418-021-00922-9
Karlowitz R, van Wijk SJL (2023) Surviving death: emerging concepts of RIPK3 and MLKL ubiquitination in the regulation of necroptosis. Febs J 290:37–54. https://doi.org/10.1111/febs.16255
Zhu P, Ke ZR, Chen JX, Li SJ, Ma TL, Fan XL (2023) Advances in mechanism and regulation of PANoptosis: prospects in disease treatment. Front Immunol 14:1120034. https://doi.org/10.3389/fimmu.2023.1120034
Shan B, Pan H, Najafov A, Yuan J (2018) Necroptosis in development and diseases. Genes Dev 32:327–340. https://doi.org/10.1101/gad.312561.118
Orzalli MH, Kagan JC (2017) Apoptosis and necroptosis as host defense strategies to prevent viral infection. Trends Cell Biol 27:800–809. https://doi.org/10.1016/j.tcb.2017.05.007
Liu X, Xie X, Ren Y, Shao Z, Zhang N, Li L, Ding X, Zhang L (2020) The role of necroptosis in disease and treatment. MedComm 2:730–755. https://doi.org/10.1002/mco2.108
Choi ME, Price DR, Ryter SW, Choi AMK (2019) Necroptosis: a crucial pathogenic mediator of human disease. JCI Insight. https://doi.org/10.1172/jci.insight.128834
Negroni A, Colantoni E, Cucchiara S, Stronati L (2020) Necroptosis in intestinal inflammation and cancer: new concepts and therapeutic perspectives. Biomolecules. https://doi.org/10.3390/biom10101431
Gong Y, Fan Z, Luo G, Yang C, Huang Q, Fan K, Cheng H, Jin K, Ni Q, Yu X, Liu C (2019) The role of necroptosis in cancer biology and therapy. Mol Cancer 18:100. https://doi.org/10.1186/s12943-019-1029-8
Su Z, Yang Z, Xie L, DeWitt JP, Chen Y (2016) Cancer therapy in the necroptosis era. Cell Death Differ 23:748–756. https://doi.org/10.1038/cdd.2016.8
Wang T, Jin Y, Yang W, Zhang L, Jin X, Liu X, He Y, Li X (2017) Necroptosis in cancer: an angel or a demon? Tumour Biol 39:1010428317711539. https://doi.org/10.1177/1010428317711539
Wu Y, Dong G, Sheng C (2020) Targeting necroptosis in anticancer therapy: mechanisms and modulators. Acta Pharm Sin B 10:1601–1618. https://doi.org/10.1016/j.apsb.2020.01.007
Della Torre L, Nebbioso A, Stunnenberg HG, Martens JHA, Carafa V, Altucci L (2021) The role of necroptosis: biological relevance and its involvement in cancer. Cancers 13:684
Parker D, Prince A (2016) Immunoregulatory effects of necroptosis in bacterial infections. Cytokine 88:274–275. https://doi.org/10.1016/j.cyto.2016.09.024
Ahn D, Prince A (2017) Participation of necroptosis in the host response to acute bacterial pneumonia. J Innate Immun 9:262–270. https://doi.org/10.1159/000455100
Xia X, Lei L, Wang S, Hu J, Zhang G (2020) Necroptosis and its role in infectious diseases. Apoptosis 25:169–178. https://doi.org/10.1007/s10495-019-01589-x
Zhang G, Wang J, Zhao Z, Xin T, Fan X, Shen Q, Raheem A, Lee CR, Jiang H, Ding J (2022) Regulated necrosis, a proinflammatory cell death, potentially counteracts pathogenic infections. Cell Death Dis 13:637. https://doi.org/10.1038/s41419-022-05066-3
Turpin C, Catan A, Meilhac O, Bourdon E, Canonne-Hergaux F, Rondeau P (2021) Erythrocytes: central actors in multiple scenes of atherosclerosis. Int J Mol Sci. https://doi.org/10.3390/ijms22115843
Lux SE (2016) Anatomy of the red cell membrane skeleton: unanswered questions. Blood 127:187–199. https://doi.org/10.1182/blood-2014-12-512772
Pretini V, Koenen MH, Kaestner L, Fens MHAM, Schiffelers RM, Bartels M, Van Wijk R (2019) Red blood cells: chasing interactions. Front Physiol. https://doi.org/10.3389/fphys.2019.00945
Moras M, Lefevre SD, Ostuni MA (2017) From erythroblasts to mature red blood cells: organelle clearance in mammals. Front Physiol 8:1076. https://doi.org/10.3389/fphys.2017.01076
McMahon TJ, Darrow CC, Hoehn BA, Zhu H (2021) Generation and export of red blood cell ATP in health and disease. Front Physiol. https://doi.org/10.3389/fphys.2021.754638
Kerkelä E, Lahtela J, Larjo A, Impola U, Mäenpää L, Mattila P (2022) Exploring transcriptomic landscapes in red blood cells, in their extracellular vesicles and on a single-cell level. Int J Mol Sci 23:12897
Sun L, Yu Y, Niu B, Wang D (2020) Red Blood cells as potential repositories of MicroRNAs in the circulatory system. Front Genet 11:442. https://doi.org/10.3389/fgene.2020.00442
Kontidou E, Collado A, Pernow J, Zhou Z (2023) Erythrocyte-derived microRNAs: emerging players in cardiovascular and metabolic disease. Arterioscler Thromb Vasc Biol 43:628–636. https://doi.org/10.1161/atvbaha.123.319027
Ren Y, Yan C, Yang H (2023) Erythrocytes: member of the immune system that should not be ignored. Crit Rev Oncol Hematol 187:104039. https://doi.org/10.1016/j.critrevonc.2023.104039
Nielsen CH, Matthiesen SH, Lyng I, Leslie RG (1997) The role of complement receptor type 1 (CR1, CD35) in determining the cellular distribution of opsonized immune complexes between whole blood cells: kinetic analysis of the buffering capacity of erythrocytes. Immunology 90:129–137. https://doi.org/10.1046/j.1365-2567.1997.00138.x
Zhang Y, Liu Q, Yang S, Liao Q (2021) CD58 immunobiology at a glance. Front Immunol 12:705260. https://doi.org/10.3389/fimmu.2021.705260
Novitzky-Basso I, Rot A (2012) Duffy antigen receptor for chemokines and its involvement in patterning and control of inflammatory chemokines. Front Immunol 3:266. https://doi.org/10.3389/fimmu.2012.00266
Lam LKM, Murphy S, Kokkinaki D, Venosa A, Sherrill-Mix S, Casu C, Rivella S, Weiner A, Park J, Shin S, Vaughan AE, Hahn BH, Odom John AR, Meyer NJ, Hunter CA, Worthen GS, Mangalmurti NS (2021) DNA binding to TLR9 expressed by red blood cells promotes innate immune activation and anemia. Sci Transl Med 13:eabj1008. https://doi.org/10.1126/scitranslmed.abj1008
Minton K (2021) Red blood cells join the ranks as immune sentinels. Nat Rev Immunol 21:760–761. https://doi.org/10.1038/s41577-021-00648-2
Korns D, Frasch S, Fernandez-Boyanapalli R, Henson P, Bratton D (2011) Modulation of macrophage efferocytosis in inflammation. Front Immunol. https://doi.org/10.3389/fimmu.2011.00057
Doran AC, Yurdagul A, Tabas I (2020) Efferocytosis in health and disease. Nat Rev Immunol 20:254–267. https://doi.org/10.1038/s41577-019-0240-6
Riera Romo M (2021) Cell death as part of innate immunity: cause or consequence? Immunology 163:399–415. https://doi.org/10.1111/imm.13325
Burger P, de Korte D, van den Berg TK, van Bruggen R (2012) CD47 in erythrocyte ageing and clearance—the dutch point of view. Transfus Med Hemother 39:348–352. https://doi.org/10.1159/000342231
Wang F, Liu YH, Zhang T, Gao J, Xu Y, Xie GY, Zhao WJ, Wang H, Yang YG (2020) Aging-associated changes in CD47 arrangement and interaction with thrombospondin-1 on red blood cells visualized by super-resolution imaging. Aging Cell 19:e13224. https://doi.org/10.1111/acel.13224
Arashiki N, Takakuwa Y, Mohandas N, Hale J, Yoshida K, Ogura H, Utsugisawa T, Ohga S, Miyano S, Ogawa S, Kojima S, Kanno H (2016) ATP11C is a major flippase in human erythrocytes and its defect causes congenital hemolytic anemia. Haematologica 101:559–565. https://doi.org/10.3324/haematol.2016.142273
Nagata S, Suzuki J, Segawa K, Fujii T (2016) Exposure of phosphatidylserine on the cell surface. Cell Death Differ 23:952–961. https://doi.org/10.1038/cdd.2016.7
Bogdanova A, Lutz H (2013) Mechanisms tagging senescent red blood cells for clearance in healthy humans. Front Physiol. https://doi.org/10.3389/fphys.2013.00387
Mohanty J, Nagababu E, Rifkind J (2014) Red blood cell oxidative stress impairs oxygen delivery and induces red blood cell aging. Front Physiol. https://doi.org/10.3389/fphys.2014.00084
Huang C, Gao J, Wei T, Shen W (2022) Angiotensin II-induced erythrocyte senescence contributes to oxidative stress. Rejuvenation Res 25:30–38. https://doi.org/10.1089/rej.2021.0054
Nakashima K, Nishizaki O, Andoh Y (1993) Acceleration of hemoglobin glycation with aging. Clin Chim Acta 215:111–118. https://doi.org/10.1016/0009-8981(93)90254-2
Inaba M, Gupta KC, Kuwabara M, Takahashi T, Benz EJ Jr, Maede Y (1992) Deamidation of human erythrocyte protein 4.1: possible role in aging. Blood 79:3355–3361
Bosman GJ, Stappers M, Novotný VM (2010) Changes in band 3 structure as determinants of erythrocyte integrity during storage and survival after transfusion. Blood Transfus 8(Suppl 3):s48-52. https://doi.org/10.2450/2010.008s
Asaro RJ, Zhu Q, Cabrales P (2018) Erythrocyte aging, protection via vesiculation: an analysis methodology via oscillatory flow. Front Physiol 9:1607. https://doi.org/10.3389/fphys.2018.01607
Ghashghaeinia M, Cluitmans JC, Akel A, Dreischer P, Toulany M, Köberle M, Skabytska Y, Saki M, Biedermann T, Duszenko M, Lang F, Wieder T, Bosman GJ (2012) The impact of erythrocyte age on eryptosis. Br J Haematol 157:606–614. https://doi.org/10.1111/j.1365-2141.2012.09100.x
Repsold L, Joubert AM (2018) Eryptosis: an erythrocyte’s suicidal type of cell death. Biomed Res Int 2018:9405617. https://doi.org/10.1155/2018/9405617
Lang E, Lang F (2015) Mechanisms and pathophysiological significance of eryptosis, the suicidal erythrocyte death. Semin Cell Dev Biol 39:35–42. https://doi.org/10.1016/j.semcdb.2015.01.009
Pyrshev KA, Klymchenko AS, Csúcs G, Demchenko AP (2018) Apoptosis and eryptosis: striking differences on biomembrane level. Biochimica et Biophysica Acta (BBA)—Biomembranes 1860:1362–1371. https://doi.org/10.1016/j.bbamem.2018.03.019
Dreischer P, Duszenko M, Stein J, Wieder T (2022) Eryptosis: programmed death of nucleus-free iron-filled blood cells. Cells 11:503
Tkachenko A (2023) Apoptosis and eryptosis: similarities and differences. Apoptosis. https://doi.org/10.1007/s10495-023-01915-4
de Back D, Kostova E, van Kraaij M, van den Berg T, Van Bruggen R (2014) Of macrophages and red blood cells; a complex love story. Front Physiol. https://doi.org/10.3389/fphys.2014.00009
Bozza MT, Jeney V (2020) Pro-inflammatory Actions of heme and other hemoglobin-derived DAMPs. Front Immunol. https://doi.org/10.3389/fimmu.2020.01323
Mendonça R, Silveira AA, Conran N (2016) Red cell DAMPs and inflammation. Inflamm Res 65:665–678. https://doi.org/10.1007/s00011-016-0955-9
Jeney V (2018) Pro-Inflammatory Actions of red blood cell-derived DAMPs. Exp Suppl 108:211–233. https://doi.org/10.1007/978-3-319-89390-7_9
Fibach E, Rachmilewitz E (2008) The role of oxidative stress in hemolytic anemia. Curr Mol Med 8:609–619. https://doi.org/10.2174/156652408786241384
Regen SL (2021) Membrane-Disrupting molecules as therapeutic agents: a cautionary note. JACS Au 1:3–7. https://doi.org/10.1021/jacsau.0c00037
Baldwin C, Pandey J, Olarewaju O (2023) Hemolytic Anemia. StatPearls, StatPearls Publishing, St. Petersburg
LaRocca TJ, Stivison EA, Mal-Sarkar T, Hooven TA, Hod EA, Spitalnik SL, Ratner AJ (2015) CD59 signaling and membrane pores drive Syk-dependent erythrocyte necroptosis. Cell Death Dis 6:e1773. https://doi.org/10.1038/cddis.2015.135
LaRocca TJ, Sosunov SA, Shakerley NL, Ten VS, Ratner AJ (2016) Hyperglycemic conditions prime cells for RIP1-dependent necroptosis. J Biol Chem 291:13753–13761. https://doi.org/10.1074/jbc.M116.716027
McCaig WD, Hodges AL, Deragon MA, Haluska RJ Jr, Bandyopadhyay S, Ratner AJ, Spitalnik SL, Hod EA, LaRocca TJ (2019) Storage primes erythrocytes for necroptosis and clearance. Cell Physiol Biochem 53:496–507. https://doi.org/10.33594/000000153
Seo J, Kim Y, Ji S, Kim HB, Jung H, Yi EC, Lee YH, Shin I, Yang WH, Cho JW (2023) O-GlcNAcylation of RIPK1 rescues red blood cells from necroptosis. Front Immunol 14:1160490. https://doi.org/10.3389/fimmu.2023.1160490
Gladwin MT, Ofori-Acquah SF (2014) Erythroid DAMPs drive inflammation in SCD. Blood 123:3689–3690. https://doi.org/10.1182/blood-2014-03-563874
Erdei J, Tóth A, Balogh E, Nyakundi BB, Bányai E, Ryffel B, Paragh G, Cordero MD, Jeney V (2018) Induction of NLRP3 inflammasome activation by heme in human endothelial cells. Oxid Med Cell Longev 2018:4310816. https://doi.org/10.1155/2018/4310816
Salgar S, Bolívar BE, Flanagan JM, Anum SJ, Bouchier-Hayes L (2023) The NLRP3 inflammasome fires up heme-induced inflammation in hemolytic conditions. Transl Res 252:34–44. https://doi.org/10.1016/j.trsl.2022.08.011
Chen G, Zhang D, Fuchs TA, Manwani D, Wagner DD, Frenette PS (2014) Heme-induced neutrophil extracellular traps contribute to the pathogenesis of sickle cell disease. Blood 123:3818–3827. https://doi.org/10.1182/blood-2013-10-529982
Karsten E, Breen E, Herbert BR (2018) Red blood cells are dynamic reservoirs of cytokines. Sci Rep 8:3101. https://doi.org/10.1038/s41598-018-21387-w
Xie J, Yao Y, Yang C, Liu W, Zhou X, Zhang M (2022) Erythrocyte immune system: beyond the gas transporter. Blood&Genomics. https://doi.org/10.46701/bg.2022012022009
Kolosova IA, Mirzapoiazova T, Moreno-Vinasco L, Sammani S, Garcia JG, Verin AD (2008) Protective effect of purinergic agonist ATPgammaS against acute lung injury. Am J Physiol Lung Cell Mol Physiol 294:L319–L324. https://doi.org/10.1152/ajplung.00283.2007
Gibb DR, Calabro S, Liu D, Tormey CA, Spitalnik SL, Zimring JC, Hendrickson JE, Hod EA, Eisenbarth SC (2016) The Nlrp3 inflammasome does not regulate alloimmunization to transfused red blood cells in mice. EBioMedicine 9:77–86. https://doi.org/10.1016/j.ebiom.2016.06.008
McMahon TJ, Darrow CC, Hoehn BA, Zhu H (2021) Generation and export of red blood cell ATP in health and disease. Front Physiol 12:754638. https://doi.org/10.3389/fphys.2021.754638
Wei J, Zhao J, Schrott V, Zhang Y, Gladwin M, Bullock G, Zhao Y (2015) Red Blood cells store and release interleukin-33. J Investig Med 63:806–810. https://doi.org/10.1097/jim.0000000000000213
Lu Y, Basatemur G, Scott IC, Chiarugi D, Clement M, Harrison J, Jugdaohsingh R, Yu X, Newland SA, Jolin HE, Li X, Chen X, Szymanska M, Haraldsen G, Palmer G, Fallon PG, Cohen ES, McKenzie ANJ, Mallat Z (2020) Interleukin-33 signaling controls the development of iron-recycling macrophages. Immunity 52:782-793.e5. https://doi.org/10.1016/j.immuni.2020.03.006
Mathangasinghe Y, Fauvet B, Jane SM, Goloubinoff P, Nillegoda NB (2021) The Hsp70 chaperone system: distinct roles in erythrocyte formation and maintenance. Haematologica 106:1519–1534. https://doi.org/10.3324/haematol.2019.233056
Olayanju AOD, Adeleke A, Okolo CS, Ogunyemi OO, Mary OK (2022) Association between haematological values and heat shock protein 70 of sickle cell disease patients in Ado-Ekiti, Ekiti State. Nigeria Pan Afr Med J 43:47. https://doi.org/10.11604/pamj.2022.43.47.33346
Hulina A, Grdić Rajković M, Jakšić Despot D, Jelić D, Dojder A, Čepelak I, Rumora L (2018) Extracellular Hsp70 induces inflammation and modulates LPS/LTA-stimulated inflammatory response in THP-1 cells. Cell Stress Chaperones 23:373–384. https://doi.org/10.1007/s12192-017-0847-0
Tukaj S (2020) Heat shock protein 70 as a double agent acting inside and outside the cell: insights into autoimmunity. Int J Mol Sci 21:5298
Rarick KR, Pritchard KA (2021) The sickle erythrocyte yields another DAMP. Blood 137:3010–3011. https://doi.org/10.1182/blood.2021011143
Tumburu L, Ghosh-Choudhary S, Seifuddin FT, Barbu EA, Yang S, Ahmad MM, Wilkins LHW, Tunc I, Sivakumar I, Nichols JS, Dagur PK, Yang S, Almeida LEF, Quezado ZMN, Combs CA, Lindberg E, Bleck CKE, Zhu J, Shet AS, Chung JH, Pirooznia M, Thein SL (2021) Circulating mitochondrial DNA is a proinflammatory DAMP in sickle cell disease. Blood 137:3116–3126. https://doi.org/10.1182/blood.2020009063
Helms CC, Marvel M, Zhao W, Stahle M, Vest R, Kato GJ, Lee JS, Christ G, Gladwin MT, Hantgan RR, Kim-Shapiro DB (2013) Mechanisms of hemolysis-associated platelet activation. J Thromb Haemost 11:2148–2154. https://doi.org/10.1111/jth.12422
Dutra FF, Bozza MT (2014) Heme on innate immunity and inflammation. Front Pharmacol 5:115. https://doi.org/10.3389/fphar.2014.00115
Rapido F (2017) The potential adverse effects of haemolysis. Blood Transfus 15:218–221. https://doi.org/10.2450/2017.0311-16
Yatim N, Cullen S, Albert ML (2017) Dying cells actively regulate adaptive immune responses. Nat Rev Immunol 17:262–275. https://doi.org/10.1038/nri.2017.9
Birmpilis AI, Paschalis A, Mourkakis A, Christodoulou P, Kostopoulos IV, Antimissari E, Terzoudi G, Georgakilas AG, Armpilia C, Papageorgis P, Kastritis E, Terpos E, Dimopoulos MA, Kalbacher H, Livaniou E, Christodoulou MI, Tsitsilonis OE (2022) Immunogenic cell death, DAMPs and prothymosin α as a putative anticancer immune response biomarker. Cells. https://doi.org/10.3390/cells11091415
Greenberg ME, Sun M, Zhang R, Febbraio M, Silverstein R, Hazen SL (2006) Oxidized phosphatidylserine-CD36 interactions play an essential role in macrophage-dependent phagocytosis of apoptotic cells. J Exp Med 203:2613–2625. https://doi.org/10.1084/jem.20060370
Scovino AM, Totino PRR, Morrot A (2022) Eryptosis as a new insight in malaria pathogenesis. Front Immunol. https://doi.org/10.3389/fimmu.2022.855795
Dias GF, Grobe N, Rogg S, Jörg DJ, Pecoits-Filho R, Moreno-Amaral AN, Kotanko P (2020) The role of eryptosis in the pathogenesis of renal anemia: insights from basic research and mathematical modeling. Front Cell Dev Biol. https://doi.org/10.3389/fcell.2020.598148
Chang CF, Goods BA, Askenase MH, Hammond MD, Renfroe SC, Steinschneider AF, Landreneau MJ, Ai Y, Beatty HE, da Costa LHA, Mack M, Sheth KN, Greer DM, Huttner A, Coman D, Hyder F, Ghosh S, Rothlin CV, Love JC, Sansing LH (2018) Erythrocyte efferocytosis modulates macrophages towards recovery after intracerebral hemorrhage. J Clin Invest 128:607–624. https://doi.org/10.1172/jci95612
Fang M, Xia F, Chen Y, Shen Y, Ma L, You C, Tao C, Hu X (2022) Role of eryptosis in hemorrhagic stroke. Front Mol Neurosci. https://doi.org/10.3389/fnmol.2022.932931
Catanzaro E, Feron O, Skirtach AG, Krysko DV (2022) Immunogenic Cell Death and role of nanomaterials serving as therapeutic vaccine for personalized cancer immunotherapy. Front Immunol 13:925290. https://doi.org/10.3389/fimmu.2022.925290
Bissinger R, Bouguerra G, Al Mamun Bhuyan A, Waibel S, Abbès S, Lang F (2015) Efavirenz Induced suicidal death of human erythrocytes. Cell Physiol Biochem 37:2496–2507. https://doi.org/10.1159/000438602
Mischitelli M, Jemaà M, Almasry M, Faggio C, Lang F (2016) Stimulation of erythrocyte cell membrane scrambling by quinine. Cell Physiol Biochem 40:657–667. https://doi.org/10.1159/000452578
Jemaà M, Mischitelli M, Fezai M, Almasry M, Faggio C, Lang F (2016) Stimulation of suicidal erythrocyte death by the CDC25 inhibitor NSC-95397. Cell Physiol Biochem 40:597–607. https://doi.org/10.1159/000452573
Alfhili MA, Nkany MB, Weidner DA, Lee MH (2019) Stimulation of eryptosis by broad-spectrum insect repellent N, N-Diethyl-3-methylbenzamide (DEET). Toxicol Appl Pharmacol 370:36–43. https://doi.org/10.1016/j.taap.2019.03.011
Alfhili MA, Weidner DA, Lee MH (2019) Disruption of erythrocyte membrane asymmetry by triclosan is preceded by calcium dysregulation and p38 MAPK and RIP1 stimulation. Chemosphere 229:103–111. https://doi.org/10.1016/j.chemosphere.2019.04.211
Alamri HS, Alsughayyir J, Akiel M, Al-Sheikh YA, Basudan AM, Dera A, Barhoumi T, Basuwdan AM, Alfhili MA (2021) Stimulation of calcium influx and CK1α by NF-κB antagonist [6]-Gingerol reprograms red blood cell longevity. J Food Biochem 45:e13545. https://doi.org/10.1111/jfbc.13545
Alfhili MA, Alamri HS, Alsughayyir J, Basudan AM (2022) Induction of hemolysis and eryptosis by occupational pollutant nickel chloride is mediated through calcium influx and p38 MAP kinase signaling. Int J Occup Med Environ Health 35:1–11. https://doi.org/10.13075/ijomeh.1896.01814
Alfhili MA, Basudan AM, Aljaser FS, Dera A, Alsughayyir J (2021) Bioymifi, a novel mimetic of TNF-related apoptosis-induced ligand (TRAIL), stimulates eryptosis. Med Oncol 38:138. https://doi.org/10.1007/s12032-021-01589-5
Freitas Leal JK, Preijers F, Brock R, Adjobo-Hermans M, Bosman G (2019) Red blood cell homeostasis and altered vesicle formation in patients with paroxysmal nocturnal hemoglobinuria. Front Physiol. https://doi.org/10.3389/fphys.2019.00578
Gwamaka M, Fried M, Domingo G, Duffy PE (2011) Early and extensive CD55 loss from red blood cells supports a causal role in malarial anaemia. Malar J 10:386. https://doi.org/10.1186/1475-2875-10-386
Waitumbi JN, Opollo MO, Muga RO, Misore AO, Stoute JA (2000) Red cell surface changes and erythrophagocytosis in children with severe plasmodium falciparum anemia. Blood 95:1481–1486
Waitumbi JN, Donvito B, Kisserli A, Cohen JHM, Stoute JA (2004) Age-related changes in red blood cell complement regulatory proteins and susceptibility to severe malaria. J Infect Dis 190:1183–1191. https://doi.org/10.1086/423140
Oyong DA, Loughland JR, SheelaNair A, Andrew D, Rivera FDL, Piera KA, William T, Grigg MJ, Barber BE, Haque A, Engwerda CR, McCarthy JS, Anstey NM, Boyle MJ (2019) Loss of complement regulatory proteins on red blood cells in mild malarial anaemia and in Plasmodium falciparum induced blood-stage infection. Malar J 18:312. https://doi.org/10.1186/s12936-019-2962-0
Mahtout H, Curt S, Chandad F, Rouabhia M, Grenier D (2011) Effect of periodontopathogen lipopolysaccharides and proinflammatory cytokines on CD46, CD55, and CD59 gene/protein expression by oral epithelial cells. FEMS Immunol Med Microbiol 62:295–303. https://doi.org/10.1111/j.1574-695X.2011.00813.x
Dammermann W, Schipper P, Ullrich S, Fraedrich K, Schulze Zur Wiesch J, Fründt T, Tiegs G, Lohse A, Lüth S (2013) Increased expression of complement regulators CD55 and CD59 on peripheral blood cells in patients with EAHEC O104:H4 infection. PloS one 8:e74880. https://doi.org/10.1371/journal.pone.0074880
Antonelou MH, Kriebardis AG, Papassideri IS (2010) Aging and death signalling in mature red cells: from basic science to transfusion practice. Blood Transfus 8(Suppl 3):s39-47. https://doi.org/10.2450/2010.007s
Zhang Y, Su SS, Zhao S, Yang Z, Zhong CQ, Chen X, Cai Q, Yang ZH, Huang D, Wu R, Han J (2017) RIP1 autophosphorylation is promoted by mitochondrial ROS and is essential for RIP3 recruitment into necrosome. Nat Commun 8:14329. https://doi.org/10.1038/ncomms14329
Deragon MA, McCaig WD, Patel PS, Haluska RJ, Hodges AL, Sosunov SA, Murphy MP, Ten VS, LaRocca TJ (2020) Mitochondrial ROS prime the hyperglycemic shift from apoptosis to necroptosis. Cell Death Discovery 6:132. https://doi.org/10.1038/s41420-020-00370-3
Wei J, Chen L, Wang D, Tang L, Xie Z, Chen W, Zhang S, Weng G (2021) Upregulation of RIP3 promotes necroptosis via a ROS-dependent NF-κB pathway to induce chronic inflammation in HK-2 cells. Mol Med Rep. https://doi.org/10.3892/mmr.2021.12423
Yang Z, Wang Y, Zhang Y, He X, Zhong C-Q, Ni H, Chen X, Liang Y, Wu J, Zhao S, Zhou D, Han J (2018) RIP3 targets pyruvate dehydrogenase complex to increase aerobic respiration in TNF-induced necroptosis. Nat Cell Biol 20:186–197. https://doi.org/10.1038/s41556-017-0022-y
Chu Q, Gu X, Zheng Q, Wang J, Zhu H (2021) Mitochondrial Mechanisms of apoptosis and necroptosis in liver diseases. Anal Cell Pathol (Amst) 2021:8900122. https://doi.org/10.1155/2021/8900122
Kim S, Lee H, Lim JW, Kim H (2021) Astaxanthin induces NADPH oxidase activation and receptor-interacting protein kinase 1-mediated necroptosis in gastric cancer AGS cells. Mol Med Rep. https://doi.org/10.3892/mmr.2021.12477
Alu A, Han X, Ma X, Wu M, Wei Y, Wei X (2020) The role of lysosome in regulated necrosis. Acta Pharm Sin B 10:1880–1903. https://doi.org/10.1016/j.apsb.2020.07.003
Faizan MI, Ahmad T (2021) Altered mitochondrial calcium handling and cell death by necroptosis: an emerging paradigm. Mitochondrion 57:47–62. https://doi.org/10.1016/j.mito.2020.12.004
Dhaouadi N, Vitto VAM, Pinton P, Galluzzi L, Marchi S (2023) Ca2+ signaling and cell death. Cell Calcium 113:102759. https://doi.org/10.1016/j.ceca.2023.102759
Vanden Berghe T, Kaiser WJ, Bertrand MJ, Vandenabeele P (2015) Molecular crosstalk between apoptosis, necroptosis, and survival signaling. Mol Cell Oncol 2:e975093. https://doi.org/10.4161/23723556.2014.975093
Ning B, Guo C, Kong A, Li K, Xie Y, Shi H, Gu J (2021) Calcium signaling mediates cell death and crosstalk with autophagy in kidney disease. Cells. https://doi.org/10.3390/cells10113204
Zhang X, Matsuda M, Yaegashi N, Nabe T, Kitatani K (2020) Regulation of necroptosis by phospholipids and sphingolipids. Cells 9:627
Thornton C, Hagberg H (2015) Role of mitochondria in apoptotic and necroptotic cell death in the developing brain. Clin Chim Acta 451:35–38. https://doi.org/10.1016/j.cca.2015.01.026
Kavčič N, Pegan K, Turk B (2017) Lysosomes in programmed cell death pathways: from initiators to amplifiers. Biol Chem 398:289–301. https://doi.org/10.1515/hsz-2016-0252
Zhu SY, Yao RQ, Li YX, Zhao PY, Ren C, Du XH, Yao YM (2020) Lysosomal quality control of cell fate: a novel therapeutic target for human diseases. Cell Death Dis 11:817. https://doi.org/10.1038/s41419-020-03032-5
Nano M, Mondo JA, Harwood J, Balasanyan V, Montell DJ (2023) Cell survival following direct executioner-caspase activation. Proc Natl Acad Sci USA 120:e2216531120. https://doi.org/10.1073/pnas.2216531120
Sukumaran P, Nascimento Da Conceicao V, Sun Y, Ahamad N, Saraiva LR, Selvaraj S, Singh BB (2021) Calcium signaling regulates autophagy and apoptosis. Cells. https://doi.org/10.3390/cells10082125
Green DR (2022) The mitochondrial pathway of apoptosis: part I: MOMP and beyond. Cold Spring Harb Perspect Biol. https://doi.org/10.1101/cshperspect.a041038
Zhou M, Li Y, Hu Q, Bai XC, Huang W, Yan C, Scheres SH, Shi Y (2015) Atomic structure of the apoptosome: mechanism of cytochrome c- and dATP-mediated activation of Apaf-1. Genes Dev 29:2349–2361. https://doi.org/10.1101/gad.272278.115
Dadsena S, Jenner A, García-Sáez AJ (2021) Mitochondrial outer membrane permeabilization at the single molecule level. Cell Mol Life Sci 78:3777–3790. https://doi.org/10.1007/s00018-021-03771-4
Kalkavan H, Green DR (2018) MOMP, cell suicide as a BCL-2 family business. Cell Death Differ 25:46–55. https://doi.org/10.1038/cdd.2017.179
Oh S-J, Ikeda M, Ide T, Hur KY, Lee M-S (2022) Mitochondrial event as an ultimate step in ferroptosis. Cell Death Discovery 8:414. https://doi.org/10.1038/s41420-022-01199-8
Tang D, Chen X, Kroemer G (2022) Cuproptosis: a copper-triggered modality of mitochondrial cell death. Cell Res 32:417–418. https://doi.org/10.1038/s41422-022-00653-7
Tian C, Liu Y, Li Z, Zhu P, Zhao M (2022) Mitochondria related cell death modalities and disease. Front Cell Dev Biol. https://doi.org/10.3389/fcell.2022.832356
Zheng J, Kong C, Yang X, Cui X, Lin X, Zhang Z (2017) Protein kinase C-α (PKCα) modulates cell apoptosis by stimulating nuclear translocation of NF-kappa-B p65 in urothelial cell carcinoma of the bladder. BMC Cancer 17:432. https://doi.org/10.1186/s12885-017-3401-7
Xu W, Huang Z, Gan Y, Chen R, Huang Y, Xue B, Jiang S, Yu Z, Yu K, Zhang S (2020) Casein kinase 1α inhibits p53 downstream of MDM2-mediated autophagy and apoptosis in acute myeloid leukemia. Oncol Rep 44:1895–1904. https://doi.org/10.3892/or.2020.7760
Almasry M, Jemaà M, Mischitelli M, Faggio C, Lang F (2016) Stimulation of suicidal erythrocyte death by phosphatase inhibitor calyculin A. Cell Physiol Biochem 40:163–171. https://doi.org/10.1159/000452534
Villalpando-Rodriguez GE, Gibson SB (2021) Reactive oxygen species (ROS) Regulates different types of cell death by acting as a rheostat. Oxid Med Cell Longev 2021:9912436. https://doi.org/10.1155/2021/9912436
Saddoughi SA, Ogretmen B (2013) Diverse functions of ceramide in cancer cell death and proliferation. Adv Cancer Res 117:37–58. https://doi.org/10.1016/b978-0-12-394274-6.00002-9
Dadsena S, Bockelmann S, Mina JGM, Hassan DG, Korneev S, Razzera G, Jahn H, Niekamp P, Müller D, Schneider M, Tafesse FG, Marrink SJ, Melo MN, Holthuis JCM (2019) Ceramides bind VDAC2 to trigger mitochondrial apoptosis. Nat Commun 10:1832. https://doi.org/10.1038/s41467-019-09654-4
Nganga R, Oleinik N, Ogretmen B (2018) Chapter one—mechanisms of ceramide-dependent cancer cell death. In: Chalfant CE, Fisher PB (eds) Advances in Cancer Research. Academic Press, Cambridge, pp 1–25
Liu F, Zhang Y, Shi Y, Xiong K, Wang F, Yang J (2022) Ceramide induces pyroptosis through TXNIP/NLRP3/GSDMD pathway in HUVECs. BMC Mol Cell Biol 23:54. https://doi.org/10.1186/s12860-022-00459-w
Restivo I, Attanzio A, Giardina IC, Di Gaudio F, Tesoriere L, Allegra M (2022) Cigarette smoke extract induces p38 MAPK-initiated fas-mediated eryptosis. Int J Mol Sci. https://doi.org/10.3390/ijms232314730
Restivo I, Attanzio A, Tesoriere L, Allegra M, Garcia-Llatas G, Cilla A (2023) A mixture of dietary plant sterols at nutritional relevant serum concentration inhibits extrinsic pathway of eryptosis induced by cigarette smoke extract. Int J Mol Sci 24:1264
Heckmann BL, Tummers B, Green DR (2019) Crashing the computer: apoptosis vs. necroptosis in neuroinflammation. Cell Death Differ 26:41–52. https://doi.org/10.1038/s41418-018-0195-3
Kearney CJ, Martin SJ (2017) An inflammatory perspective on necroptosis. Mol Cell 65:965–973. https://doi.org/10.1016/j.molcel.2017.02.024
Degterev A, Ofengeim D, Yuan J (2019) Targeting RIPK1 for the treatment of human diseases. Proc Natl Acad Sci USA 116:9714–9722. https://doi.org/10.1073/pnas.1901179116
Nakano H, Murai S, Moriwaki K (2022) Regulation of the release of damage-associated molecular patterns from necroptotic cells. Biochem J 479:677–685. https://doi.org/10.1042/bcj20210604
Deng L, Pan X, Wang Y, Wang L, Zhou XE, Li M, Feng Y, Wu Q, Wang B, Huang N (2009) Hemoglobin and its derived peptides may play a role in the antibacterial mechanism of the vagina. Hum Reprod 24:211–218. https://doi.org/10.1093/humrep/den318
Sheshadri P, Abraham J (2012) Antimicrobial properties of hemoglobin. Immunopharmacol Immunotoxicol 34:896–900. https://doi.org/10.3109/08923973.2012.692380
Bissinger R, Bhuyan AAM, Qadri SM, Lang F (2019) Oxidative stress, eryptosis and anemia: a pivotal mechanistic nexus in systemic diseases. FEBS J 286:826–854. https://doi.org/10.1111/febs.14606
Nemkov T, Reisz JA, Xia Y, Zimring JC, D’Alessandro A (2018) Red blood cells as an organ? How deep omics characterization of the most abundant cell in the human body highlights other systemic metabolic functions beyond oxygen transport. Expert Rev Proteomics 15:855–864. https://doi.org/10.1080/14789450.2018.1531710
Funding
Funding was provided by an EHA Ukraine Bridge Funding awarded by the European Hematology Association and Charles University in Prague (Cooperatio).
Author information
Authors and Affiliations
Contributions
AT, OH all authors equally contributed to the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors report there are no competing interests to declare.
Ethical approval
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tkachenko, A., Havranek, O. Erythronecroptosis: an overview of necroptosis or programmed necrosis in red blood cells. Mol Cell Biochem (2024). https://doi.org/10.1007/s11010-024-04948-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11010-024-04948-8