Abstract
Objectives
Assessing the impact of interdisciplinary training programs is highly desirable and needed. However, there are currently no established methods to prospectively assess long-term outcomes of trainees compared to individuals who did not receive training. Our objective was to test the feasibility of a longitudinal, prospective cohort design to evaluate training outcomes, and to use this method to evaluate Leadership Education in Neurodevelopmental Disabilities and Related Disorders (LEND) training outcomes.
Methods
LEND trainees were matched to comparison peers and followed annually for up to five years using a pre-existing outcomes survey. We assessed study feasibility using recruitment and retention data over five years. We then looked at preliminary efficacy of LEND training in LEND trainees compared to comparison peers using the pre-existing outcomes survey.
Results
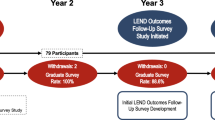
Overall, 68.3% of eligible trainees participated in the Outcomes Study across five years, and 66.0% were matched to comparison peers. On average, 84.4% of LEND trainees and 79.9% of comparison peers completed the outcomes survey annually. Attrition was low at 0.9% for LEND trainees and 2.6% for comparison peers over five years. LEND training demonstrated preliminary efficacy in promoting leadership development: LEND trainees began their careers engaged in more leadership activities than comparison peers, and the rate of growth in their participation in leadership activities was greater.
Conclusions
The design used to assess outcomes is a feasible approach that can be widely used to assess training program outcomes. Analyses suggest that LEND training is efficacious in increasing involvement in leadership activities over time after graduation.



Similar content being viewed by others
Availability of Data and Code
De-identified data and code for analyses are available upon request from the first author.
References
Association of University Centers on Disabilities (2011). About LEND. Retrieved from: https://www.aucd.org/template/page.cfm?id=473
Brosco, J. P., Pulgaron, E., Vanderbilt, D. L., Macias, M., Mathew, M. S., & Blum, N. J. (2018). The Interprofessional/Family-Centered-Care Observation Rubric (I-FOR): Results of a multicenter study of a new measure of educational outcomes. Maternal and Child Health Journal, 22(10), 1384–1392
Devon, E. P., Tenney-Soeiro, R., Ronan, J., & Balmer, D. F. (2019). A pediatric pre-intern boot camp: Program development and evaluation informed by a conceptual framework. Academic Pediatrics, 19(2), 165–169
Efstathiou, N., & Walker, W. M. (2014). Interprofessional, simulation-based training in end of life care communication: a pilot study. Journal of Interprofessional Care, 28(1), 68–70
Fisher, R. J. (1993). Social desirability bias and the validity of indirect questioning. Journal of Consumer Research, 20(2), 303–315
Humphreys, B. P., Kurtz, A. J., Portrie, C., Couse, L. J., & Hajnaghizadeh, F. (2018). Advancing leadership skills: A multiyear examination of LEND trainee self-efficacy Growth. Maternal and Child Health Journal, 22(10), 1377–1383
Ioachimescu, O. C., Wickwire, E. M., Harrington, J., Kristo, D., Arnedt, J. T., Ramar, K. … Paruthi, S. (2014). A dozen years of American Academy of Sleep Medicine (AASM) International Mini-Fellowship: Program evaluation and future directions. Journal of Clinical Sleep Medicine, 10(3), 331–334
Kavanagh, L., Menser, M., Pooler, J., Mathis, S., & Ramos, L. R. (2015). The MCH training program: Developing MCH leaders that are equipped for the changing health care landscape. Maternal and Child Health Journal, 19(2), 257–264
Leyva, V. L., Breshears, E. M., & Ringstad, R. (2014). Assessing the efficacy of LGBT cultural competency training for aging services providers in California’s Central Valley. Journal of Gerontological Social Work, 57(2–4), 335–348
Margolis, L. H., Rosenberg, A., Umble, K., & Chewning, L. (2013). Effects of interdisciplinary training on MCH professionals, organizations and systems. Maternal and Child Health Journal, 17(5), 949–958
McDougal, J. A., Lapidus, J., Albanese, M., & Redding, G. (2003). Interdisciplinary leadership training outcomes of maternal and child health-funded pediatric pulmonary centers. Maternal and Child Health Journal, 7(4), 253–260
Rosenberg, A., Margolis, L. H., Umble, K., & Chewning, L. (2015). Fostering intentional interdisciplinary leadership in developmental disabilities: The North Carolina LEND experience. Maternal and Child Health Journal, 19(2), 290–299
Slort, W., Blankenstein, A. H., Schweitzer, B. P., Knol, D. L., van der Horst, H. E., Aaronson, N. K., & Deliens, L. (2014). Effectiveness of the palliative care ‘Availability, Current issues and Anticipation’(ACA) communication training programme for general practitioners on patient outcomes: a controlled trial. Palliative Medicine, 28(8), 1036–1045
Symons, A. B., McGuigan, D., & Akl, E. A. (2009). A curriculum to teach medical students to care for people with disabilities: Development and initial implementation. BMC Medical Education, 9(1), 1–7
Szilassy, E., Carpenter, J., Patsios, D., & Hackett, S. (2013). Outcomes of short course interprofessional training in domestic violence and child protection. Violence Against Women, 19(11), 1370–1383
Wong, M. D., Guerrero, L., Sallam, T., Frank, J. S., Fogelman, A. M., & Demer, L. L. (2016). Outcomes of a novel training program for physician-scientists: Integrating graduate degree training with specialty fellowship. Journal of Graduate Medical Education, 8(1), 85–90
Acknowledgements
We would like to thank Miya Asato, MD (Director, LEND Center of the University of Pittsburgh) and Amy Wentmore for their support of this research.
Funding
This study was supported in part by grants from the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) Leadership Education in Neurodevelopmental and Related Disabilities Training Grants to the University of Wisconsin-Madison (T73MC00044), The Ohio State University (T73MC24481), and the University of Pittsburgh (T73MC00036); the Interdisciplinary Technical Assistance Center on Autism and Developmental Disabilities; the Eunice Kennedy Shriver National Institute of Child Health and Human Development (U54HD090256); and the National Center for Advancing Translational Sciences (UL1TR002373; KL2TR002374; KL2TR000428). The contents are those of the authors and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, of the U.S. Government.
Author information
Authors and Affiliations
Contributions
Dr. Bishop conceptualized and designed the study, drafted study manuals, cleaned and obtained data, carried out analyses, drafted the manuscript, and reviewed and revised the manuscript. Dr. Noll conceptualized and obtained initial funding for the broader Outcomes Study and served as the Pittsburgh site PI prior to retirement. Drs. Harris, Rabidoux, and Laughlin served as site PIs and participated in reviewing and revising the manuscript. Ms. McLean participated in reviewing and revising the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Ethics
This study was approved by institutional review boards at the University of Pittsburgh, The Ohio State University, and the University of Wisconsin-Madison. All participants provided informed consent.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bishop, L., Harris, A.B., Rabidoux, P.C. et al. A model to evaluate interprofessional training effectiveness: feasibility and five-year outcomes of a multi-site prospective cohort study. Matern Child Health J 26, 1622–1631 (2022). https://doi.org/10.1007/s10995-022-03421-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-022-03421-6