Abstract
Introduction
Stress exposure during a woman’s own childhood and adulthood likely elevate risk of prenatal depression (PND). However, most PND screening tools fail to assess for events prior to conception. This study examined the differential effects of adverse childhood experiences (ACE) and adult life stressors on PND.
Methods
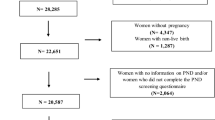
This cross-sectional study was conducted among 199 racially diverse pregnant women, ages 18 to 43, recruited from clinics and ongoing university-based studies between 2012 and 2018. The ACE Scale assessed maternal childhood trauma exposure. Validated scales examining subjective stressors assessed for chronic adult stressors. PND was assessed with the Edinburgh Depression Scale, with the Rini Pregnancy-Related Anxiety Scale as a covariate. Associations were measured using multivariable linear regression modeling. Results were stratified by self-identified Black or white race.
Results
Among 199 participants, mean age was 26.8 years and 67.8% were Black. Controlling for age, race, education, and prenatal anxiety, all participants reporting both childhood trauma and adult stressors were at increased risk for PND (p < 0.0001). PND risk was increased among Black women with childhood stressors (p < 0.01) or three or more adult stressors (p < 0.0001) and among White women following any number of adult stressors (p < 0.001).
Discussion
These findings highlight the importance of cumulative exposure to stress and trauma across the life span as indicators of risk for PND. Black and white participants had differential development of risk, depending on timing and number of exposures. Prenatal depression risk screening during routine prenatal care should include an assessment of current and historical trauma and stressors.
Similar content being viewed by others
Data Availability
Not applicable.
Code Availability
Not applicable.
References
ACOG. (2018). ACOG Committee Opinion No 757: Screening for Perinatal Depression. Obstetrics & Gynecology, 132(5), e208–e212.
Adler, N. E., Epel, E. S., Castellazzo, G., & Ickovics, J. R. (2000). Relationship of subjective and objective social status with psychological and physiological functioning: Preliminary data in healthy white women. Health Psychology, 19(6), 586–592. https://doi.org/10.1037//0278-6133.19.6.586
Ahern, N. R., Kiehl, E. M., Sole, M. L., & Byers, J. (2006). A review of instruments measuring resilience. Issues in Comprehensive Pediatric Nursing, 29(2), 103–125. https://doi.org/10.1080/01460860600677643
Alder, J., Fink, N., Bitzer, J., Hosli, I., & Holzgreve, W. (2007). Depression and anxiety during pregnancy: A risk factor for obstetric, fetal and neonatal outcome? A critical review of the literature. Journal of Maternal-Fetal & Neonatal Medicine, 20(3), 189–209. https://doi.org/10.1080/14767050701209560
Alvarez-Segura, M., Garcia-Esteve, L., Torres, A., Plaza, A., Imaz, M. L., Hermida-Barros, L., San, L., & Burtchen, N. (2014). Are women with a history of abuse more vulnerable to perinatal depressive symptoms? A systematic review. Archives of Women’s Mental Health, 17(5), 343–357. https://doi.org/10.1007/s00737-014-0440-9
Angerud, K., Annerback, E. M., Tyden, T., Boddeti, S., & Kristiansson, P. (2018). Adverse childhood experiences and depressive symptomatology among pregnant women. Acta Obstetricia Et Gynecologica Scandinavica, 97(6), 701–708. https://doi.org/10.1111/aogs.13327
Barcelona de Mendoza, V., Harville, E. W., Savage, J., & Giarratano, G. (2018). Experiences of intimate partner and neighborhood violence and their association with mental health in pregnant women. Journal of Interpersonal Violence, 33(6), 938–959. https://doi.org/10.1177/0886260515613346
Barnes, A. J., Anthony, B. J., Karatekin, C., Lingras, K. A., Mercado, R., & Thompson, L. A. (2020). Identifying adverse childhood experiences in pediatrics to prevent chronic health conditions. Pediatric Research, 87(2), 362–370. https://doi.org/10.1038/s41390-019-0613-3
Bouvette-Turcot, A. A., Unternaehrer, E., Gaudreau, H., Lydon, J. E., Steiner, M., Meaney, M. J., & Team, M. R. (2017). The joint contribution of maternal history of early adversity and adulthood depression to socioeconomic status and potential relevance for offspring development. Journal of Affective Disorders, 207, 26–31. https://doi.org/10.1016/j.jad.2016.08.012
Chang, J. J., Tabet, M., Elder, K., Kiel, D. W., & Flick, L. H. (2016). Racial/ethnic differences in the correlates of mental health services use among pregnant women with depressive symptoms. Maternal and Child Health Journal, 20(9), 1911–1922. https://doi.org/10.1007/s10995-016-2005-1
Chung, E. K., Mathew, L., Elo, I. T., Coyne, J. C., & Culhane, J. F. (2008). Depressive symptoms in disadvantaged women receiving prenatal care: The influence of adverse and positive childhood experiences. Ambulatory Pediatrics, 8(2), 109–116. https://doi.org/10.1016/j.ambp.2007.12.003
Cohen, S., Janicki-Deverts, D., & Miller, G. E. (2007). Psychological stress and disease. JAMA, 298(14), 1685–1687. https://doi.org/10.1001/jama.298.14.1685
Cox, J. L., Holden, J. M., & Sagovsky, R. (1987). Detection of postnatal depression: Development of the 10-item edinburgh postnatal depression scale. British Journal of Psychiatry, 150, 782–786.
Cundiff, J. M., Smith, T. W., Uchino, B. N., & Berg, C. A. (2013). Subjective social status: Construct validity and associations with psychosocial vulnerability and self-rated health. International Journal of Behavioral Medicine, 20(1), 148–158. https://doi.org/10.1007/s12529-011-9206-1
Cunningham, T. J., Berkman, L. F., Gortmaker, S. L., Kiefe, C. I., Jacobs, D. R., Jr., Seeman, T. E., & Kawachi, I. (2011). Assessment of differential item functioning in the experiences of discrimination index: The Coronary Artery Risk Development in Young Adults (CARDIA) Study. American Journal of Epidemiology, 174(11), 1266–1274. https://doi.org/10.1093/aje/kwr253
Dong, M., Anda, R. F., Felitti, V. J., Dube, S. R., Williamson, D. F., Thompson, T. J., Loo, C. M., & Giles, W. H. (2004). The interrelatedness of multiple forms of childhood abuse, neglect, and household dysfunction. Child Abuse and Neglect, 28(7), 771–784. https://doi.org/10.1016/j.chiabu.2004.01.008
Dube, S. R., Felitti, V. J., Dong, M., Chapman, D. P., Giles, W. H., & Anda, R. F. (2003). Childhood abuse, neglect, and household dysfunction and the risk of illicit drug use: the adverse childhood experiences study. Pediatrics, 111(3), 564–572.
Esteves, K. C., Jones, C. W., Wade, M., Callerame, K., Smith, A. K., Theall, K. P., & Drury, S. S. (2020). Adverse childhood experiences: Implications for offspring telomere length and psychopathology. American Journal of Psychiatry, 177(1), 47–57. https://doi.org/10.1176/appi.ajp.2019.18030335
Felitti, V. J., Anda, R. F., Nordenberg, D., Williamson, D. F., Spitz, A. M., Edwards, V., Koss, M. P., & Marks, J. S. (1998). Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults: The Adverse Childhood Experiences (ACE) Study. American Journal of Preventive Medicine, 14(4), 245–258.
Flanagan, T., Alabaster, A., McCaw, B., Stoller, N., Watson, C., & Young-Wolff, K. C. (2018). Feasibility and acceptability of screening for adverse childhood experiences in prenatal care. Journal of Women’s Health (2002), 27(7), 903–911. https://doi.org/10.1089/jwh.2017.6649
Ghimire, U., Papabathini, S. S., Kawuki, J., Obore, N., & Musa, T. H. (2021). Depression during pregnancy and the risk of low birth weight, preterm birth and intrauterine growth restriction- an updated meta-analysis. Early Human Development, 152, 105243. https://doi.org/10.1016/j.earlhumdev.2020.105243
Giurgescu, C., Zenk, S. N., Templin, T. N., Engeland, C. G., Dancy, B. L., Park, C. G., Kavanaugh, K., Dieber, W., & Misra, D. P. (2015). The impact of neighborhood environment, social support, and avoidance coping on depressive symptoms of pregnant african-american women. Women’s Health Issues, 25(3), 294–302. https://doi.org/10.1016/j.whi.2015.02.001
Glowa, P. T., Olson, A. L., & Johnson, D. J. (2016). Screening for adverse childhood experiences in a family medicine setting: A feasibility study. Journal of the American Board of Family Medicine, 29(3), 303–307. https://doi.org/10.3122/jabfm.2016.03.150310
Gray, S. A. O., Jones, C. W., Theall, K. P., Glackin, E., & Drury, S. S. (2017). Thinking across generations: Unique contributions of maternal early life and prenatal stress to infant physiology. Journal of the American Academy of Child and Adolescent Psychiatry, 56(11), 922–929. https://doi.org/10.1016/j.jaac.2017.09.001
Hahn, C. K., Gilmore, A. K., Aguayo, R. O., & Rheingold, A. A. (2018). Perinatal intimate partner violence. Obstetrics and Gynecology Clinics of North America, 45(3), 535–547. https://doi.org/10.1016/j.ogc.2018.04.008
Hilmert, C. J., Schetter, C. D., Dominguez, T. P., Abdou, C., Hobel, C. J., Glynn, L., & Sandman, C. (2008). Stress and blood pressure during pregnancy: Racial differences and associations with birthweight. Psychosomatic Medicine, 70(1), 57–64. https://doi.org/10.1097/PSY.0b013e31815c6d96
Holzman, C., Eyster, J., Tiedje, L. B., Roman, L. A., Seagull, E., & Rahbar, M. H. (2006). A life course perspective on depressive symptoms in mid-pregnancy. Maternal and Child Health Journal, 10(2), 127–138. https://doi.org/10.1007/s10995-005-0044-0
Jaffee, K. D., Liu, G. C., Canty-Mitchell, J., Qi, R. A., Austin, J., & Swigonski, N. (2005). Race, urban community stressors, and behavioral and emotional problems of children with special health care needs. Psychiatric Services (washington, DC), 56(1), 63–69. https://doi.org/10.1176/appi.ps.56.1.63
Kerker, B. D., Storfer-Isser, A., Szilagyi, M., Stein, R. E., Garner, A. S., O’Connor, K. G., Hoagwood, K. E., & Horwitz, S. M. (2016). Do pediatricians ask about adverse childhood experiences in pediatric primary care? Academic Pediatric, 16(2), 154–160. https://doi.org/10.1016/j.acap.2015.08.002
Krieger, N., Smith, K., Naishadham, D., Hartman, C., & Barbeau, E. M. (2005). Experiences of discrimination: Validity and reliability of a self-report measure for population health research on racism and health. Social Science and Medicine, 61(7), 1576–1596. https://doi.org/10.1016/j.socscimed.2005.03.006
Lewis, T. T., Williams, D. R., Tamene, M., & Clark, C. R. (2014). Self-Reported experiences of discrimination and cardiovascular disease. Current Cardiovascular Risk Reports, 8(1), 365. https://doi.org/10.1007/s12170-013-0365-2
Madewell, A. N., Ponce-Garcia, E., & Martin, S. E. (2016). Data replicating the factor structure and reliability of commonly used measures of resilience: The Connor-Davidson Resilience Scale, Resilience Scale, and Scale of Protective Factors. Data in Brief, 8, 1387–1390. https://doi.org/10.1016/j.dib.2016.08.001
Matthey, S., Valenti, B., Souter, K., & Ross-Hamid, C. (2013). Comparison of four self-report measures and a generic mood question to screen for anxiety during pregnancy in English-speaking women. Journal of Affective Disorders, 148(2), 347–351.
Meijer, J. L., Beijers, C., van Pampus, M. G., Verbeek, T., Stolk, R. P., Milgrom, J., Bockting, C. L., & Burger, H. (2014). Predictive accuracy of Edinburgh postnatal depression scale assessment during pregnancy for the risk of developing postpartum depressive symptoms: A prospective cohort study. BJOG, 121(13), 1604–1610. https://doi.org/10.1111/1471-0528.12759
Mestad, R., Lane, S. D., Hall, M., Smith, C. J., Carter, D. B., Rubinstein, R. A., Keefe, R. H., & Jones-Moore, C. (2016). Prenatal depression: Screening and referral for women who are low income during antenatal care. Soc Work Public Health, 31(6), 557–564. https://doi.org/10.1080/19371918.2016.1160344
Mukherjee, S., Trepka, M. J., Pierre-Victor, D., Bahelah, R., & Avent, T. (2016). Racial/ethnic disparities in antenatal depression in the united states: A systematic review. Maternal and Child Health Journal, 20(9), 1780–1797. https://doi.org/10.1007/s10995-016-1989-x
Murray, D., & Cox, J. L. (1990). Screening for depression during pregnancy with the Edinburgh Depression Scale (EDDS). Journal of Reproductive and Infant Psychology, 8(2), 99–107.
Navaratne, P., Foo, X. Y., & Kumar, S. (2016). Impact of a high Edinburgh Postnatal Depression Scale score on obstetric and perinatal outcomes. Science and Reports, 6, 33544. https://doi.org/10.1038/srep33544
Okah, F. A., Oshodi, A., Liu, Y., & Cai, J. (2014). Community violence and pregnancy health behaviors and outcomes. Southern Medical Journal, 107(8), 513–517. https://doi.org/10.14423/SMJ.0000000000000143
Pantell, M. S., Prather, A. A., Downing, J. M., Gordon, N. P., & Adler, N. E. (2019). Association of social and behavioral risk factors with earlier onset of adult hypertension and diabetes. JAMA Network Open, 2(5), e193933. https://doi.org/10.1001/jamanetworkopen.2019.3933
Racine, N., Zumwalt, K., McDonald, S., Tough, S., & Madigan, S. (2020). Perinatal depression: The role of maternal adverse childhood experiences and social support. Journal of Affective Disorders, 263, 576–581. https://doi.org/10.1016/j.jad.2019.11.030
Ribeiro, A. I., Amaro, J., Lisi, C., & Fraga, S. (2018). Neighborhood socioeconomic deprivation and allostatic load: A scoping review. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph15061092
Rini, C. K., Dunkel-Schetter, C., Wadhwa, P. D., & Sandman, C. A. (1999). Psychological adaptation and birth outcomes: the role of personal resources, stress, and sociocultural context in pregnancy. Health Psychology, 18(4), 333–345.
Robertson-Blackmore, E., Putnam, F. W., Rubinow, D. R., Matthieu, M., Hunn, J. E., Putnam, K. T., Moynihan, J. A., & O’Connor, T. G. (2013). Antecedent trauma exposure and risk of depression in the perinatal period. Journal of Clinical Psychiatry, 74(10), e942-948. https://doi.org/10.4088/JCP.13m08364
Rosenthal, L., & Lobel, M. (2011). Explaining racial disparities in adverse birth outcomes: Unique sources of stress for Black American women. Social Science and Medicine, 72(6), 977–983. https://doi.org/10.1016/j.socscimed.2011.01.013
Sanders-Phillips, K. (1996). The ecology of urban violence: its relationship to health promotion behaviors in low-income black and Latino communities. American Journal of Health Promotion, 10(4), 308–317.
Serati, M., Redaelli, M., Buoli, M., & Altamura, A. C. (2016). Perinatal Major depression biomarkers: A systematic review. Journal of Affective Disorders, 193, 391–404. https://doi.org/10.1016/j.jad.2016.01.027
Sherin, K. M., Sinacore, J. M., Li, X. Q., Zitter, R. E., & Shakil, A. (1998). HITS: a short domestic violence screening tool for use in a family practice setting. Family Medicine, 30(7), 508–512.
Simon, C. D., Adam, E. K., Holl, J. L., Wolfe, K. A., Grobman, W. A., & Borders, A. E. (2016). Prenatal stress and the cortisol awakening response in African-American and caucasian women in the third trimester of pregnancy. Maternal and Child Health Journal, 20(10), 2142–2149. https://doi.org/10.1007/s10995-016-2060-7
Suglia, S. F., Staudenmayer, J., Cohen, S., Enlow, M. B., Rich-Edwards, J. W., & Wright, R. J. (2010). Cumulative Stress and cortisol disruption among black and hispanic pregnant women in an urban cohort. Psychological Trauma: Theory, Research, Practice and Policy, 2(4), 326–334. https://doi.org/10.1037/a0018953
Van den Bergh, B. R. H., van den Heuvel, M. I., Lahti, M., Braeken, M., de Rooij, S. R., Entringer, S., Hoyer, D., Roseboom, T., Raikkonen, K., King, S., & Schwab, M. (2017). Prenatal developmental origins of behavior and mental health: The influence of maternal stress in pregnancy. Neuroscience and Biobehavioral Reviews. https://doi.org/10.1016/j.neubiorev.2017.07.003
Verner, G., Epel, E., Lahti-Pulkkinen, M., Kajantie, E., Buss, C., Lin, J., Blackburn, E., Raikkonen, K., Wadhwa, P. D., & Entringer, S. (2021). Maternal psychological resilience during pregnancy and newborn telomere length: A prospective study. American Journal of Psychiatry, 178(2), 183–192. https://doi.org/10.1176/appi.ajp.2020.19101003
Wajid, A., van Zanten, S. V., Mughal, M. K., Biringer, A., Austin, M. P., Vermeyden, L., & Kingston, D. (2019). Adversity in childhood and depression in pregnancy. Archives of Women’s Mental Health. https://doi.org/10.1007/s00737-019-00966-4
Wallace, M., Harville, E., Theall, K., Webber, L., Chen, W., & Berenson, G. (2013). Preconception biomarkers of allostatic load and racial disparities in adverse birth outcomes: The Bogalusa Heart Study. Paediatric and Perinatal Epidemiology, 27(6), 587–597. https://doi.org/10.1111/ppe.12091
Weinreb, L., Savageau, J. A., Candib, L. M., Reed, G. W., Fletcher, K. E., & Hargraves, J. L. (2010). Screening for childhood trauma in adult primary care patients: A cross-sectional survey. Primary Care Companion to the Journal of Clinical Psychiatry. https://doi.org/10.4088/PCC.10m00950blu
Acknowledgements
The authors would like to acknowledge key staff members, Kyle Esteves, Christopher Jones, and Marni Jacobs, for their dedication to the study implementation. We would also like to thank all of the families who volunteered for their selfless contributions to the Infant Development Study.
Funding
This research was supported by the National Institutes of Health (NIH) R01MH101533.
Author information
Authors and Affiliations
Contributions
Dr. KT and Dr. SD conceptualized, designed, and provided oversight for the study and analyses. Material preparation, data collection, and data anlysis was performed by CJ. The draft preparation, review, and editing was led by Dr. MGE with contributions from all authors. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest relevant to this article to disclose.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Consent to Publish
Not applicable.
Ethical Approval
Tulane University Institutional Review Board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Evans, M.G., Theall, K.P., Jackson, C. et al. Racial Differences in the Risk of Prenatal Depression Among Women Experiencing Childhood and Adult Stressors. Matern Child Health J 26, 614–622 (2022). https://doi.org/10.1007/s10995-021-03322-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-021-03322-0