Abstract
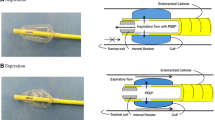
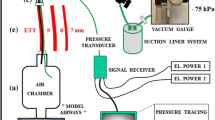
The endotracheal tubes (ETTs) used for children have a smaller inner diameter. Accordingly, the resistance across ETT (RETT) is higher. Theoretically, shortening the ETTs can decrease total airway resistance (Rtotal), because Rtotal is sum of RETT and patient’s airway resistance. However, the effectiveness of ETT shortening for mechanical ventilation in the clinical setting has not been reported. We assessed the effectiveness of shortening a cuffed ETT for decreasing Rtotal, and increasing tidal volume (TV), and estimated the RETT/Rtotal ratio in children. In anesthetized children in a constant pressure-controlled ventilation setting, Rtotal and TV were measured with a pneumotachometer before and after shortening a cuffed ETT. In a laboratory experiment, the pressure gradient across the original length, shortened length, and the slip joint alone of the ETT were measured. We then determined the RETT/Rtotal ratio using the above results. The clinical study included 22 children. The median ETT percent shortening was 21.7%. Median Rtotal was decreased from 26 to 24 cmH2O/L/s, and median TV was increased by 6% after ETT shortening. The laboratory experiment showed that ETT length and the pressure gradient across ETT are linearly related under a certain flow rate, and approximately 40% of the pressure gradient across the ETT at its original length was generated by the slip joint. Median RETT/Rtotal ratio were calculated as 0.69. The effectiveness of ETT shortening on Rtotal and TV was very limited, because the resistance of the slip joint was very large.





Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Miyake F, Suga R, Akiyama T, Namba F. An in vitro evaluation of the influence of neonatal endotracheal tube diameter and length on the work of breathing. Paediatr Anaesth. 2018;28:458–62. https://doi.org/10.1111/pan.13366.
Manczur T, Greenough A, Nicholson GP, Rafferty GF. Resistance of pediatric and neonatal endotracheal tubes: Influence of flow rate, size, and shape. Crit Care Med. 2000;28:1595–8. https://doi.org/10.1097/00003246-200005000-00056.
Ivanov VA. Reduction of endotracheal tube connector dead space improves ventilation: a bench test on a model lung simulating an extremely low birth weight neonate. Respir Care. 2016;61:155–61. https://doi.org/10.4187/respcare.04076.
Fine GF, Borland LM. The future of the cuffed endotracheal tube. Paediatr Anaesth. 2004;14:38–42. https://doi.org/10.1046/j.1460-9592.2003.01203.x.
Elayaperumal A, Venkataraju A. Cut tracheal tube and GlideRite® Rigid Stylet. Br J Anaesth. 2014;113:517–8. https://doi.org/10.1093/bja/aeu279.
Marr R, Lax P. Tracheal tubes can be cut safely when in situ. Anaesthesia. 2011;66:753. https://doi.org/10.1111/j.1365-2044.2011.06831.x.
Fitzpatrick G. Tracheal tubes can be cut safely when in situ. Anaesthesia. 2011;66:1059–60. https://doi.org/10.1111/j.1365-2044.2011.06953_2.x.
Hughes C, Popat M. Tracheal tubes can be cut safely when in situ. Anaesthesia. 2011;66:1059. https://doi.org/10.1111/j.1365-2044.2011.06953_1.x.
Mahajan R, Nazir RSF. More on cutting tracheal tubes in situ. Anaesthesia. 2012;67:192. https://doi.org/10.1111/j.1365-2044.2011.07038_1.x.
Jarreau PH, Louis B, Dassieu G, Desfrere L, Blanchard PW, Moriette G, et al. Estimation of inspiratory pressure drop in neonatal and pediatric endotracheal tubes. J Appl Physiol. 1999;87:36–46. https://doi.org/10.1152/jappl.1999.87.1.36.
Guttmann J, Kessler V, Mols G, Hentschel R, Haberthür C, Geiger K. Continuous calculation of intratracheal pressure in the presence of pediatric endotracheal tubes. Crit Care Med. 2000;28:1018–26. https://doi.org/10.1097/00003246-200004000-00018.
Guttmann J, Eberhard L, Fabry B, Bertschmann W, Wolff G. Continuous calculation of intratracheal pressure in tracheally intubated patients. Anesthesiology. 1993;79:503–13. https://doi.org/10.1097/00000542-199309000-00014.
Spaeth J, Steinmann D, Kaltofen H, Guttmann J, Schumann S. The pressure drop across the endotracheal tube in mechanically ventilated pediatric patients. Paediatr Anaesth. 2015;25:413–20. https://doi.org/10.1111/pan.12595.
Berry A, Brimacombe J, Keller C, Verghese C. Pulmonary airway resistance with the endotracheal tube versus laryngeal mask airway in paralyzed anesthetized adult patients. Anesthesiology. 1999;90:395–7. https://doi.org/10.1097/00000542-199902000-00011.
Board PDP. Cutting tracheal tubes in situ. Anaesthesia. 2011;66:319. https://doi.org/10.1111/j.1365-2044.2011.06663.x.
Takahashi K, Toyama H, Funahashi Y, Kawana S, Ejima Y, Kikuchi K, et al. Influence of respiratory gas density on tidal volume during mechanical ventilation: a laboratory investigation and observational study in children. Tohoku J Exp Med. 2022;256:271–81. https://doi.org/10.1620/tjem.2022.j003.
Weiss M, Dullenkopf A, Gysin C, Dillier CM, Gerber AC. Shortcomings of cuffed paediatric tracheal tubes. Br J Anaesth. 2004;92:78–88. https://doi.org/10.1093/bja/aeh023.
Tareerath M, Mangmeesri P. Accuracy of age-based formula to predict the size and depth of cuffed oral preformed endotracheal tubes in children undergoing tonsillectomy. Ear, Nose Throat J. 2021. https://doi.org/10.1177/0145561320980511.
Daoud EG, Katigbak R, Ottochian M. Accuracy of the ventilator automated displayed respiratory mechanics in passive and active breathing conditions: a bench study. Respir Care. 2019;64:1555–60. https://doi.org/10.4187/RESPCARE.06422.
Toyama H, Endo Y, Ejima Y, Matsubara M, Kurosawa S. Comparison of actual tidal volume in neonatal lung model volume control ventilation using three ventilators. Anaesth Intensive Care. 2011;39:599–606. https://doi.org/10.1177/0310057x1003800401.
Kanaya A, Satoh D, Kurosawa S. Higher fraction of inspired oxygen in anesthesia induction does not affect functional residual capacity reduction after intubation: a comparative study of higher and lower oxygen concentration. J Anesth. 2013;27:385–9. https://doi.org/10.1007/s00540-012-1547-7.
Brown ES. Resistance factors in pediatric endotracheal tubes and connectors. Anesth Analg. 1971;50:355–60. https://doi.org/10.1213/00000539-197105000-00017.
Takasugi Y, Futagawa K, Kazuhara K, Morishita S, Okuda T. Roles of endotracheal tubes and slip joints in respiratory pressure loss: a laboratory study. J Anesth. 2016;30:789–95. https://doi.org/10.1007/s00540-016-2210-5.
Uchiyama A, Yoshida T, Yamanaka H, Fujino Y. Estimation of tracheal pressure and imposed expiratory work of breathing by the endotracheal tube, heat and moisture exchanger, and ventilator during mechanical ventilation. Respir Care. 2013;58:1157–69. https://doi.org/10.4187/respcare.01698.
Beydon N. Interrupter resistance: what’s feasible? Paediatr Respir Rev. 2006;7:S5-7. https://doi.org/10.1016/j.prrv.2006.04.022.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation and data collection and analysis were performed by KT, HT, RK, and NY. Data analysis were performed by KT, HT, YE, KK, and TI. The study was supervised by MY. The first draft of the manuscript was written by KT and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Tohoku University Graduate School of Medicine (Date; November 16, 2020/No; 2020-1-727).
Consent to participate
Written informed consent was obtained from the parents of all participants.
Consent to publish
Consent to publish has been received from the parents of all participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Takahashi, K., Toyama, H., Kubo, R. et al. Effectiveness of substantial shortening of the endotracheal tube for decreasing airway resistance and increasing tidal volume during pressure-controlled ventilation in pediatric patients: a prospective observational study. J Clin Monit Comput 37, 1513–1519 (2023). https://doi.org/10.1007/s10877-023-01038-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-023-01038-w