Abstract
Purpose
To determine risk factors for substantial closed-globe injuries in orbital fractures (SCGI) and to develop the best multivariate model for the prediction of SCGI.
Methods
A retrospective study was performed on patients diagnosed with orbital fractures at Farabi Hospital between 2016 and 2022. Patients with a comprehensive ophthalmologic examination and orbital CT scan were included. Predictive signs or imaging findings for SCGI were identified by logistic regression (LR) analysis. Support vector machine (SVM), random forest regression (RFR), and extreme gradient boosting (XGBoost) were also trained using a fivefold cross-validation method.
Results
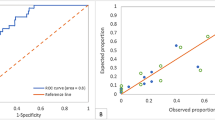
A total of 415 eyes from 403 patients were included. Factors associated with an increased risk of SCGI were reduced uncorrected visual acuity (UCVA), increased difference between UCVA of the traumatic eye from the contralateral eye, older age, male sex, grade of periorbital soft tissue trauma, trauma in the occupational setting, conjunctival hemorrhage, extraocular movement restriction, number of fractured walls, presence of medial wall fracture, size of fracture, intraorbital emphysema and retrobulbar hemorrhage. The area under the curve of the receiver operating characteristic for LR, SVM, RFR, and XGBoost for the prediction of SCGI was 57.2%, 68.8%, 63.7%, and 73.1%, respectively.
Conclusions
Clinical and radiographic findings could be utilized to efficiently predict SCGI. XGBoost outperforms the logistic regression model in the prediction of SCGI and could be incorporated into clinical practice.



Similar content being viewed by others
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Cook T (2002) Ocular and periocular injuries from orbital fractures. J Am Coll Surg 195:831–834
Noh H, Chung JK, Woo KI, Kim Y-D (2021) Occurrence of ocular injury and orbital fracture in orbital blunt trauma patients at tertiary care center emergency room. Graefes Arch Clin Exp Ophthalmol 259:165–171
Lim JW, Yoo JH, Nam KY, Lee SU, Lee SJ (2016) Analysis of ocular complications and blowout fracture in orbital blunt trauma. J Korean Ophthalmol Soc 57:1282–1286
Kreidl KO, Kim DY, Mansour SE (2003) Prevalence of significant intraocular sequelae in blunt orbital trauma. Am J Emerg Med 21:525–528
Andrews BT, Jackson AS, Nazir N, Hromas A, Sokol JA, Thurston TE (2016) Orbit fractures: identifying patient factors indicating high risk for ocular and periocular injury. Laryngoscope 126:S5–S11
Ho TQ, Jupiter D, Tsai JH, Czerwinski M (2017) The incidence of ocular injuries in isolated orbital fractures. Ann Plast Surg 78:59–61
Thurston TE, Jackson AS, Nazir N, Crowe D, Andrews BT (2018) Risk assessment of isolated single-wall orbit fractures and eye injury. J Craniofac Surg 29:943–945
Mellema PA, Dewan MA, Lee MS, Smith SD, Harrison AR (2009) Incidence of ocular injury in visually asymptomatic orbital fractures. Ophthalmic Plast Reconstr Surg 25:306–308
Chow J, Parthasarathi K, Mehanna P, Whist E (2018) Primary assessment of the patient with orbital fractures should include pupillary response and visual acuity changes to detect occult major ocular injuries. J Oral Maxillofac Surg 76:2370–2375
Terrill SB, You H, Eiseman H, Rauser ME (2020) Review of ocular injuries in patients with orbital wall fractures: a 5-year retrospective analysis. Clin Ophthalmol 14:2837–2842
Rossin EJ, Szypko C, Giese I, Hall N, Gardiner MF, Lorch A (2021) Factors associated with increased risk of serious ocular injury in the setting of orbital fracture. JAMA Ophthalmol 139:77–83. https://doi.org/10.1001/jamaophthalmol.2020.5108
Zhong E, Chou TY, Chaleff AJ, Scofield-Kaplan SM, Perzia BM, Naqvi J, Hou W (2022) Orbital fractures and risk factors for ocular injury. Clin Ophthalmol 16:4153–4161
Kuhn F, Morris R, Witherspoon CD, Mester V (2004) The birmingham eye trauma terminology system (BETT). J Fr Ophtalmol 27:206–210. https://doi.org/10.1016/s0181-5512(04)96122-0
Dave TV, Chheda PP, Das AV, Dave VP (2023) Open globe injuries with concurrent orbital fractures-clinical settings and factors predicting outcomesseminars in ophthalmology. Taylor & Francis, pp 1–7
Balla SC, Jha KN, Ramanujam S, Srikanth K, Rajalakshmi AR (2022) Maxillofacial trauma and ocular injuries: reports from a prospective study from Pondicherry, India. Orbit 41:457–463
Ai-Ourainy I, Dutton G, Stassen L, Moos K, Ei-Attar A (1991) The characteristics of midfacial fractures and the association with ocular injury: a prospective study. Br J Oral Maxillofac Surg 29:291–301
He D, Blomquist PH, Ellis E III (2007) Association between ocular injuries and internal orbital fractures. J Oral Maxillofac Surg 65:713–720
Rockafellow A, Busby E, WuDunn D, Grover S, Salman SO (2021) Evidence-based protocol for ophthalmology consult for orbital fractures. J Oral Maxillofac Surg 79:1507–1513. https://doi.org/10.1016/j.joms.2021.02.026
Layton CJ (2014) Factors associated with significant ocular injury in conservatively treated orbital fractures. J Ophthalmol 2014
Dutton G, Al-Qurainy I, Stassen L, Titterington D, Moos K, El-Attar A (1992) Ophthalmic consequences of mid-facial trauma. Eye 6:86–89
Richani K, Do T, Merritt HA, Pfeiffer ML, Chuang AZ, Phillips ME (2019) Screening criteria for detecting severe ocular injuries in the setting of orbital fractures. Ophthalmic Plast Reconstr Surg 35:609
Rossin EJ, Szypko C, Giese I, Hall N, Gardiner MF, Lorch A (2021) Factors associated with increased risk of serious ocular injury in the setting of orbital fracture. JAMA Ophthalmol 139:77–83
Santamaria J, Mehta A, Reed D, Blegen H, Bishop B, Davies B (2019) Orbital roof fractures as an indicator for concomitant ocular injury. Graefes Arch Clin Exp Ophthalmol 257:2541–2545
Kuhn F, Morris R, Witherspoon CD, Heimann K, Jeffers JB, Treister G (1996) A standardized classification of ocular trauma. Graefes Arch Clin Exp Ophthalmol 234:399–403
Lange C, Feltgen N, Junker B, Schulze-Bonsel K, Bach M (2009) Resolving the clinical acuity categories “hand motion” and “counting fingers” using the Freiburg visual acuity test (FrACT). Graefes Arch Clin Exp Ophthalmol 247:137–142. https://doi.org/10.1007/s00417-008-0926-0
Klein B, Karlson T, Rose J (1993) An anatomic index for the severity of ocular injuries. Eur J Ophthalmol 3:57–60
Moon H, Kim Y, Wi J, Chi M (2016) Morphological characteristics and clinical manifestations of orbital emphysema caused by isolated medial orbital wall fractures. Eye 30:582–587
Anton N, Doroftei B, Curteanu S, Catãlin L, Ilie OD, Târcoveanu F, Bogdănici CM (2022) Comprehensive review on the use of artificial intelligence in ophthalmology and future research directions. Diagnostics. https://doi.org/10.3390/diagnostics13010100
Wang S, Li F, Jin S, Zhang Y, Yang N, Zhao J (2023) Biomechanics of open-globe injury: a review. Biomed Eng Online 22:53. https://doi.org/10.1186/s12938-023-01117-8
Lee BW, Samarawickrama C (2023) Closed globe and adnexal eye injuries: Epidemiology, clinical and surgical outcomes, and an economic cost analysis. Clin Exp Ophthalmol
Mitchell R, Frank E (2017) Accelerating the XGBoost algorithm using GPU computing. PeerJ Comput Sci 3:e127
Vaid A, Chan L, Chaudhary K, Jaladanki SK, Paranjpe I, Russak A, Kia A, Timsina P, Levin MA, He JC (2021) Predictive approaches for acute dialysis requirement and death in COVID-19. Clin J Am Soc Nephrol 16:1158
Yoo TK, Ryu IH, Choi H, Kim JK, Lee IS, Kim JS, Lee G, Rim TH (2020) Explainable machine learning approach as a tool to understand factors used to select the refractive surgery technique on the expert level. Transl Vis Sci Technol 9:8–8
Acknowledgements
The authors would like to thank the Farabi Eye Hospital staff for their kind assistance during this study.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
BS, RF, MTR, MR, and FS contributed to the design of the study. FS and HF reviewed medical records. FS evaluated CT scans. MTR and RF interpreted the data. MY performed statistical analyses. FH developed machine learning models. FS wrote the original draft of the paper. MR and BS revised the manuscript and supervised the study. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This study was conducted under approval from institutional review boards at the Tehran University of Medical Sciences (IR.TUMS.FARABIH.REC.1401.028). This study was performed according to the principles of the Declaration of Helsinki.
Consent to participate
As this study was a retrospective study without direct contact with the subjects, the Ethics Committee of Tehran University of Medical Sciences waived the requirement for informed consent.
Consent for publication
As this study was a retrospective study without direct contact with the subjects, the Ethics Committee of Tehran University of Medical Sciences waived the requirement for informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Salari, F., Rafizadeh, S.M., Fakhredin, H. et al. Prediction of substantial closed-globe injuries in orbital wall fractures. Int Ophthalmol 44, 219 (2024). https://doi.org/10.1007/s10792-024-03113-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10792-024-03113-w