Abstract
Purpose
To systematically review the published manuscripts on stereopsis after corneal refractive surgery.
Methods
The Web of Science, PubMed, Scopus, ProQuest, Clinical Key, Embase, and Cochrane Library were searched for relevant articles published until August 2020. The fixed- or random-effects models were used to estimate the Weighted mean difference (WMD) or Relative risk (RR) and 95% Confidence interval (CI) for postoperative stereopsis changes and incidence when applicable. Meta-regression was conducted for adjusting the effects of potential confounders.
Results
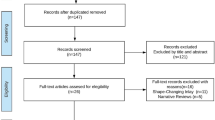
Seven studies (1266 eyes) in adults and ten studies in pediatrics (259 eyes) were included. In adults, stereopsis improved significantly compared to the preoperative state (WMD = − 27.4, 95% CI = − 40.0, − 14.7; I2 = 97.8%; P < 0.001). In pediatrics, proportion of patients with stereoacuity postoperatively was 2.18 times compared to preoperative evaluation. (RR = 2.18, 95% CI = 1.2, 3.9; I2 = 68.6%, P < 0.001).
Conclusions
Stereopsis improves after corneal refractive surgery in adults and pediatrics.



Similar content being viewed by others
References:
Hashmani N, Sharif Hashmani PR, Rajani H, Ahmed J, Kumar J, Kumar A, Jamali M (2017) A comparison of visual outcomes and patient satisfaction between photorefractive keratectomy and femtosecond laser-assisted in situ keratomileusis. Cureus. https://doi.org/10.7759/cureus.1641
Matsuguma S, Negishi K, Kawashima M, Toda I, Ayaki M, Tsubota K (2018) Patients’ satisfaction and subjective happiness after refractive surgery for myopia. Patient Prefer Adherence 12:1901
Tran K and Ryce A 2018 Laser Refractive Surgery for Vision Correction: A Review of Clinical Effectiveness and Cost-effectiveness.
Kezirian GM, Parkhurst GD, Brinton JP, Norden RA (2015) Prevalence of laser vision correction in ophthalmologists who perform refractive surgery. J Cataract Refract Surg 41(9):1826–1832
McAlinden C (2012) Corneal refractive surgery: past to present. Clin Exp Optom 95(4):386–398
Murueta-Goyena A, Canadas P (2018) Visual outcomes and management after corneal refractive surgery: A review. Journal of optometry 11(2):121–129
Gjerdrum B, Gundersen KG, Lundmark PO, Potvin R, Aakre BM (2020) Prevalence of signs and symptoms of dry eye disease 5 to 15 after refractive surgery. Clin Ophthalmol (Auckland, NZ) 14:269
Melki SA, Azar DT (2001) LASIK complications: etiology, management, and prevention. Surv Ophthalmol 46(2):95–116
García-Montero M, Albarrán Diego C, Garzón-Jiménez N, Pérez-Cambrodí RJ, López-Artero E, Ondategui-Parra JC (2019) Binocular vision alterations after refractive and cataract surgery: a review. Acta Ophthalmol 97(2):e145–e155
Cui, D., Chen, J., Meyer, E. and Yang, G., 2019. Anatomy visualizations using stereopsis: current methodologies in developing stereoscopic virtual models in anatomical education. In Biomedical visualisation ( 49–65). Springer, Cham.
Dutton J, Watkins A, Henderson J, Burgess FR, Tint NL, Dhillon B, Tatham AJ (2020) Influence of stereopsis on the ability to perform simulated microsurgery. J Cataract Refract Surg 46(4):549–554
Zhao JL, Xiao F, Zhao HX, Dai Y, Zhang YD (2018) Impact of intraocular scatter on stereopsis. Vision Res 153:124–128
Wainman B, Pukas G, Wolak L, Mohanraj S, Lamb J, Norman GR (2020) The critical role of stereopsis in virtual and mixed reality learning environments. Anat Sci Educ 13(3):401–412
O’connor AR, Tidbury LP (2018) Stereopsis: are we assessing it in enough depth? Clin Exp Optom 101(4):485–494
Chen CY, Keeffe JE, Garoufalis P, Islam FM, Dirani M, Couper TA, Taylor HR, Baird PN (2007) Vision-related quality of life comparison for emmetropes, myopes after refractive surgery, and myopes wearing spectacles or contact lenses. J Refract Surg 23(8):752–759
Waring GO (1997) Quality of vision and freedom from optical correction after refractive surgery. J Refract Surg 13(3):213–215
Zarei-Ghanavati S, Gharaee H, Eslampour A, Ehsaei A, Abrishami M (2016) Stereoacuity after photorefractive keratectomy in myopia. J Curr Ophthalmol 28(1):17–20
Sarkar S, Bharadwaj SR, Reddy JC, Vaddavalli PK (2020) Longitudinal changes in optical quality, spatial vision, and depth vision after laser refractive surgery for myopia. Optom Vis Sci 97(5):360–369
Jabbarvand M, Hashemian H, Khodaparast M, Anvari P (2016) Changes in stereopsis after photorefractive keratectomy. J Cataract Refract Surg 42(6):899–903
Karimian F, Ownagh V, Amiri MA, Tabatabaee SM, Dadbin N (2017) Stereoacuity after wavefront-guided photorefractive keratectomy in anisometropia. J Ophthalmic Vis Res 12(3):265
Razmjoo H, Akhlaghi MR, Dehghani AR, Peyman AR, Sari-Mohammadli M, Ghatreh-Samani H (2008) Stereoacuity following LASIK. J Ophthalmic Vis Res 3(1):28
Nucci P, Drack AV (2001) Refractive surgery for unilateral high myopia in children. J Am Assoc Pediatric Ophthalmol Strabismus 5(6):348–351
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188
Egger M, Smith GD, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Singh D, Saxena R, Sinha R, Titiyal JS (2015) Stereoacuity changes after laser in situ keratomileusis. Optom Vis Sci 92(2):196–200
Mravicic I, Bohac M, Lukacevic S, Jagaric K, Maja M, Patel S (2020) The relationship between clinical measures of aniseikonia and stereoacuity before and after LASIK. J Optometry 13(1):59–68
Maden A, Erkin EF, Oner FH (1998) Unilateral refractive keratotomy for anisometropia 14(3):325–330
Autrata R, Rehurek J (2003) Clinical results of excimer laser photorefractive keratectomy for high myopic anisometropia in children: four-year follow-up. J Cataract Refract Surg 29(4):694–702
Autrata R, Rehurek J (2004) Laser-assisted subepithelial keratectomy and photorefractive keratectomy versus conventional treatment of myopic anisometropic amblyopia in children. J Cataract Refract Surg 30(1):74–84
Paysse EA, Coats DK, Hussein MA, Hamill MB, Koch DD (2006) Long-term outcomes of photorefractive keratectomy for anisometropic amblyopia in children. Ophthalmology 113(2):169–176
Astle WF, Rahmat J, Ingram AD, Huang PT (2007) Laser-assisted subepithelial keratectomy for anisometropic amblyopia in children: outcomes at 1 year. J Cataract Refract Surg 33(12):2028–2034
Yin ZQ, Wang H, Yu T, Ren Q, Chen L (2007) Facilitation of amblyopia management by laser in situ keratomileusis in high anisometropic hyperopic and myopic children. J Am Assoc Pediatric Ophthalmol Strabismus 11(6):571–576
Astle WF, Fawcett SL, Huang PT, Alewenah O, Ingram A (2008) Long-term outcomes of photorefractive keratectomy and laser-assisted subepithelial keratectomy in children. J Cataract Refract Surg 34(3):411–416
Magli A, Iovine A, Gagliardi V, Fimiani F, Nucci P (2008) Photorefractive keratectomy for myopic anisometropia: a retrospective study on 18 children. Eur J Ophthalmol 18(5):716–722
Lin XM, Yan XH, Zheng WANG, Bin YANG, Chen QW, Su JA, Ye XL (2009) Long-term efficacy of excimer laserin situkeratomileusis in the management of children with high anisometropic amblyopia. Chin Med J 122(7):813–817
Ghanem AA, Moad AI, Nematallah EH, El-Adawy IT, Anwar GM (2010) Laser in situ keratomileusis for treated myopic anisometropic amblyopia in children. Saudi J Ophthalmol 24(1):3–8
Ghanem AA, Nematallah EH, El-Adawy IT, Anwar GM (2010) Facilitation of amblyopia management by laser in situ keratomileusis in children with myopic anisometropia. Curr Eye Res 35(4):281–286
Zhang J, Yu KM (2017) Femtosecond laser corneal refractive surgery for the correction of high myopic anisometropic amblyopia in juveniles. Int J Ophthalmol 10(11):1678
Astle WF, Huang PT, Ereifej I, Paszuk A (2010) Laser-assisted subepithelial keratectomy for bilateral hyperopia and hyperopic anisometropic amblyopia in children: one-year outcomes. J Cataract Refract Surg 36(2):260–267
Eissa S, Eldin NB (2018) ICL versus SMILE in management of anisometropic myopic amblyopia in children. Can J Ophthalmol 53(6):560–567
Yang JW, Huang TY, Yang KJ, Lee JS, Ku WC, Yeung L, Wu PH, Lin YF, Sun CC (2012) The effects of hyperopic and astigmatic ametropia on stereoacuity by Titmus stereo test. Taiwan J Ophthalmol 2(1):22–24
Yang JW, Huang TY, Lee JS, Yeung L, Lin YF, Sun CC (2013) Correlation between myopic ametropia and stereoacuity in school-aged children in Taiwan. Jpn J Ophthalmol 57(3):316–319
Adler FH, Moses RA (1965) Physiology of the eye: clinical application. Mosby, Berkeley, CA, USA, pp 528–535
Liu S, Zhang P, Wu X, Hu S, Tan X (2003) Clinical analysis of binocular anisei konia after laser in situ keratomileusis on myopic patients. Yan Ke Xue Bao 19(2):107–109
Wilson HR (2017) Binocular contrast, stereopsis, and rivalry: toward a dynamical synthesis. Vision Res 140:89–95
Zhao L, Wu H (2019) The difference in stereoacuity testing: contour-based and random dot-based graphs at far and near distances. Ann Transl Med 7(9):193–198
Fawcett SL (2005) An evaluation of the agreement between contour-based circles and random dot-based near stereoacuity tests. J Am Assoc Pediatric Ophthalmol Strabismus 9(6):572–578
Sekundo W, Gertnere J, Bertelmann T, Solomatin I (2014) One-year refractive results, contrast sensitivity, high-order aberrations and complications after myopic small-incision lenticule extraction (ReLEx SMILE). Graefes Arch Clin Exp Ophthalmol 252(5):837–843
Sutton G, Lawless M, Hodge C (2014) Laser in situ keratomileusis in 2012: a review. Clin Exp Optom 97(1):18–29
Daoud YJ, Hutchinson A, Wallace DK, Song J, Kim T (2009) Refractive surgery in children: treatment options, outcomes, and controversies. Am J Ophthalmol 147(4):573–582
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest regarding the publication of this paper.
Ethics approval
Ethics approval for this report was obtained from the Ethics Committee of Isfahan University of Medical Sciences, Isfahan, Iran.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Peyman, A., Pourazizi, M., Akhlaghi, M. et al. Stereopsis after corneal refractive surgeries: a systematic review and meta-analysis. Int Ophthalmol 42, 2273–2288 (2022). https://doi.org/10.1007/s10792-021-02201-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-02201-5