Abstract
Purpose
To assess the effect of hydroxypropyl methylcellulose (HPMC) 2% to prevent dry eye during phacoemulsification in senile and diabetic patients.
Methods
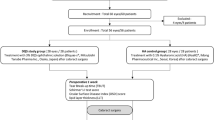
This prospective interventional case series comprised 60 eyes (44 patients) with age-related cataract scheduled for standardized phacoemulsification surgery. The patients were assigned to receive either balanced saline solution (BSS, 30 eyes) or HPMC 2% (30 eyes) during surgery. Preoperative and postoperative examinations (1, 3, 7 and 30 days) included measurements of automatic noninvasive tear film breakup time (NITBUT), fluorescein staining, Schirmer I test, tear meniscus height, depth and area and subjective symptoms. Intraoperative application frequency was also assessed.
Results
The mean age of patients was 68.7 ± 2.3 years. The application frequency of BSS during surgery was significantly reduced in HPMC group (P = 0.001). The incidence of dry eye syndrome (DES) was significantly reduced in HPMC group in both senile and diabetic patients. Scores of subjective symptoms were significantly higher in the BSS group in 1 day (P = 0.003) and 3 days (P = 0.043) postoperatively. The first and average NITBUT were significantly higher in HPMC group in 1 day and 3 days after surgery, respectively (P = 0.012 and P = 0.024, respectively). NITBUT values did not significantly change postoperatively in the HPMC group (P > 0.05), while they were significantly lower postoperatively in the BSS group.
Conclusions
Application of HPMC 2% during phacoemulsification reduced the incidence of DES and improved patients’ satisfaction in both senile and diabetic cataract patients. It was also effective in maintaining corneal hydration and was able to significantly reduce the application frequency intraoperatively.



Similar content being viewed by others
References
Li XM, Hu L, Hu J, Wang W (2007) Investigation of dry eye disease and analysis of the pathogenic factors in patients after cataract surgery. Cornea 26(9 Suppl 1):S16–S20. doi:10.1097/ICO.0b013e31812f67ca
Han KE, Yoon SC, Ahn JM, Nam SM, Stulting RD, Kim EK et al (2014) Evaluation of dry eye and meibomian gland dysfunction after cataract surgery. Am J Ophthalmol 157(6):1144 e1–1150 e1. doi:10.1016/j.ajo.2014.02.036
Kasetsuwan N, Satitpitakul V, Changul T, Jariyakosol S (2013) Incidence and pattern of dry eye after cataract surgery. PLoS ONE 8(11):e78657. doi:10.1371/journal.pone.0078657
Ram J, Gupta A, Brar G, Kaushik S, Gupta A (2002) Outcomes of phacoemulsification in patients with dry eye. J Cataract Refract Surg 28(8):1386–1389
Cho YK, Kim MS (2009) Dry eye after cataract surgery and associated intraoperative risk factors. Korean J Ophthalmol KJO 23(2):65–73. doi:10.3341/kjo.2009.23.2.65
Yu Y, Hua H, Wu M, Yu Y, Yu W, Lai K et al (2015) Evaluation of dry eye after femtosecond laser-assisted cataract surgery. J Cataract Refract Surg 41(12):2614–2623. doi:10.1016/j.jcrs.2015.06.036
Cetinkaya S, Mestan E, Acir NO, Cetinkaya YF, Dadaci Z, Yener HI (2015) The course of dry eye after phacoemulsification surgery. BMC Ophthalmol 15:68. doi:10.1186/s12886-015-0058-3
Sanchez MA, Arriola-Villalobos P, Torralbo-Jimenez P, Giron N, de la Heras B, Herrero Vanrell R et al (2010) The effect of preservative-free HP-Guar on dry eye after phacoemulsification: a flow cytometric study. Eye 24(8):1331–1337. doi:10.1038/eye.2010.24
Oh T, Jung Y, Chang D, Kim J, Kim H (2012) Changes in the tear film and ocular surface after cataract surgery. Jpn J Ophthalmol 56(2):113–118. doi:10.1007/s10384-012-0117-8
Khanal S, Tomlinson A, Esakowitz L, Bhatt P, Jones D, Nabili S et al (2008) Changes in corneal sensitivity and tear physiology after phacoemulsification. Ophthalmic physiol opt 28(2):127–134. doi:10.1111/j.1475-1313.2008.00539.x
Bron AJ, Tomlinson A, Foulks GN, Pepose JS, Baudouin C, Geerling G et al (2014) Rethinking dry eye disease: a perspective on clinical implications. Ocul Surf 12(2 Suppl):S1–S31. doi:10.1016/j.jtos.2014.02.002
Dogru M, Katakami C, Inoue M (2001) Tear function and ocular surface changes in noninsulin-dependent diabetes mellitus. Ophthalmology 108(3):586–592
Yoon KC, Im SK, Seo MS (2004) Changes of tear film and ocular surface in diabetes mellitus. Korean J Ophthalmol KJO 18(2):168–174
Alves Mde C, Carvalheira JB, Modulo CM, Rocha EM (2008) Tear film and ocular surface changes in diabetes mellitus. Arq Bras Oftalmol 71(6 Suppl):96–103
Jiang D, Xiao X, Fu T, Mashaghi A, Liu Q, Hong J (2016) Transient tear film dysfunction after cataract surgery in diabetic patients. PLoS ONE 11(1):e0146752. doi:10.1371/journal.pone.0146752
Liu X, Gu YS, Xu YS (2008) Changes of tear film and tear secretion after phacoemulsification in diabetic patients. J Zhejiang Univ Sci B 9(4):324–328. doi:10.1631/jzus.B0710359
Goebbels M (2000) Tear secretion and tear film function in insulin dependent diabetics. Br J Ophthalmol 84(1):19–21
Chen YA, Hirnschall N, Findl O (2011) Comparison of corneal wetting properties of viscous eye lubricant and balanced salt solution to maintain optical clarity during cataract surgery. J Cataract Refract Surg 37(10):1806–1808. doi:10.1016/j.jcrs.2011.07.001
Dick HB, Augustin AJ, Pfeiffer N (2000) Osmolality of various viscoelastic substances: comparative study. J Cataract Refract Surg 26(8):1242–1246
Kiss B, Findl O, Menapace R, Petternel V, Wirtitsch M, Lorang T et al (2003) Corneal endothelial cell protection with a dispersive viscoelastic material and an irrigating solution during phacoemulsification: low-cost versus expensive combination. J Cataract Refract Surg 29(4):733–740
Yao K, Bao Y, Ye J, Lu Y, Bi H, Tang X et al (2015) Efficacy of 1% carboxymethylcellulose sodium for treating dry eye after phacoemulsification: results from a multicenter, open-label, randomized, controlled study. BMC ophthalmol 15:28. doi:10.1186/s12886-015-0005-3
Prinz A, Fennes C, Buehl W, Findl O (2012) Efficacy of ophthalmic viscosurgical devices in maintaining corneal epithelial hydration and clarity: in vitro assessment. J Cataract Refract Surg 38(12):2154–2159. doi:10.1016/j.jcrs.2012.06.054
Chylack LT Jr, Wolfe JK, Singer DM, Leske MC, Bullimore MA, Bailey IL et al (1993) The lens opacities classification system III. The longitudinal study of cataract study group. Arch Ophthalmol 111(6):831–836
Peng CH, Liu JH, Woung LC, Lin TJ, Chiou SH, Tseng PC et al (2012) MicroRNAs and cataracts: correlation among let-7 expression, age and the severity of lens opacity. Br J Ophthalmol 96(5):747–751. doi:10.1136/bjophthalmol-2011-300585
Schiffman RM, Christianson MD, Jacobsen G, Hirsch JD, Reis BL (2000) Reliability and validity of the ocular surface disease index. Arch Ophthalmol 118(5):615–621
Arita R, Itoh K, Maeda S, Maeda K, Furuta A, Fukuoka S et al (2009) Proposed diagnostic criteria for obstructive meibomian gland dysfunction. Ophthalmology 116(11):2058 e1–2063 e1. doi:10.1016/j.ophtha.2009.04.037
Arriola-Villalobos P, Fernandez-Vigo JI, Diaz-Valle D, Peraza-Nieves JE, Fernandez-Perez C, Benitez-Del-Castillo JM (2015) Assessment of lower tear meniscus measurements obtained with Keratograph and agreement with Fourier-domain optical-coherence tomography. Br J Ophthalmol 99(8):1120–1125. doi:10.1136/bjophthalmol-2014-306453
Serin D, Karsloglu S, Kyan A, Alagoz G (2007) A simple approach to the repeatability of the Schirmer test without anesthesia: eyes open or closed? Cornea 26(8):903–906. doi:10.1097/ICO.0b013e3180950083
DEWS (2007) The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 5(2):75–92
Arshinoff SA, Khoury E (1997) HsS versus a balanced salt solution as a corneal wetting agent during routine cataract extraction and lens implantation. J Cataract Refract Surg 23(8):1221–1225
Gayton JL (2009) Etiology, prevalence, and treatment of dry eye disease. Clin Ophthalmol 3:405–412
Kohlhaas M (1998) Corneal sensation after cataract and refractive surgery. J Cataract Refract Surg 24(10):1399–1409
Liu NN, Liu L, Li J, Sun YZ (2014) Prevalence of and risk factors for dry eye symptom in mainland china: a systematic review and meta-analysis. J Ophthalmol 2014:748654. doi:10.1155/2014/748654
Misra SL, Patel DV, McGhee CN, Pradhan M, Kilfoyle D, Braatvedt GD et al (2014) Peripheral neuropathy and tear film dysfunction in type 1 diabetes mellitus. J Diabetes Res 2014:848659. doi:10.1155/2014/848659
Lv H, Li A, Zhang X, Xu M, Qiao Y, Zhang J et al (2014) Meta-analysis and review on the changes of tear function and corneal sensitivity in diabetic patients. Acta Ophthalmol 92(2):e96–e104. doi:10.1111/aos.12063
Najafi L, Malek M, Valojerdi AE, Aghili R, Khamseh ME, Fallah AE et al (2013) Dry eye and its correlation to diabetes microvascular complications in people with type 2 diabetes mellitus. J Diabetes Complicat 27(5):459–462. doi:10.1016/j.jdiacomp.2013.04.006
Kanellopoulos AJ, Asimellis G (2014) Corneal epithelial remodeling following cataract surgery: three-dimensional investigation with anterior-segment optical coherence tomography. J Refract Surg 30(5):348–353. doi:10.3928/1081597X-20140416-04
Acknowledgements
This study was funded by National Natural Science Foundation of China (Grant No. 81371002).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
No author has a financial or proprietary interest in any material or method mentioned.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee of Eye and ENT Hospital of Fudan University and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Yusufu, M., Liu, X., Zheng, T. et al. Hydroxypropyl methylcellulose 2% for dry eye prevention during phacoemulsification in senile and diabetic patients. Int Ophthalmol 38, 1261–1273 (2018). https://doi.org/10.1007/s10792-017-0590-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-017-0590-7