Abstract
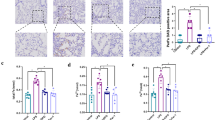
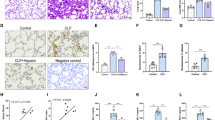
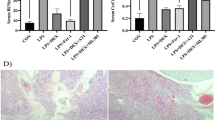
This study investigated the effect of ghrelin on oxidative stress in septic rat lung tissue. Male Sprague-Dawley rats were divided into sham-operation, sepsis, and ghrelin groups. Sepsis was induced by cecal ligation and puncture. Ghrelin was administered intraperitoneally at 3 and 15 h post-operation. Bronchoalveolar lavage was performed to collect alveolar macrophages (AMs). Inducible nitric oxide synthase (iNOS) messenger RNA (mRNA) expression in alveolar macrophages and iNOS protein levels were measured by reverse transcription PCR (RT-PCR) and Western blot. Pulmonary pathology was analyzed and nitrotyrosine expression was examined by immunohistochemistry. Plasma superoxide dismutase (SOD) and lung wet/dry weight were measured. In the sepsis group, iNOS mRNA expression in AMs was 1.33 ± 0.05, 1.44 ± 0.08, and 1.57 ± 0.11 at 6, 12, and 20 h post-surgery, respectively, and were higher compared with the sham-operation group (p < 0.05). No increase was observed at longer time points. iNOS mRNA expression in the sepsis group was lower compared with the ghrelin group (2.27 ± 0.37) (p < 0.05) at 20 h post-surgery. iNOS protein levels in the ghrelin group (0.87 ± 0.03, p < 0.05) were lower than in the sepsis group at 20 h. Ghrelin group pathological scores were lower than in the sepsis group (p < 0.05). Plasma SOD was slightly non-significantly decreased in the ghrelin group. No difference was observed in lung wet/dry weight ratios between sepsis and ghrelin groups. iNOS mRNA expression in AMs was elevated between 6 and 20 h after cecal ligation and puncture (CLP), but did not progress. Ghrelin attenuated pulmonary iNOS protein expression and tended to increase plasma SOD activity. Ghrelin suppressed pulmonary nitrosative stress in septic rats, but did not improve lung wet/dry weight ratios.





Similar content being viewed by others
References
Kooy, N.W., J.A. Royall, Y.Z. Ye, D.R. Kelly, and J.S. Beckman. 1995. Evidence for in vivo peroxynitrite production in human acute lung injury. American Journal of Respiratory and Critical Care Medicine 151(4): 1250–4. doi:10.1164/ajrccm.151.4.7697261.
Chabot, F., J.A. Mitchell, J.M. Gutteridge, and T.W. Evans. 1998. Reactive oxygen species in acute lung injury. European Respiratory Journal 11(3): 745–57.
Kristof, A.S., P. Goldberg, V. Laubach, and S.N. Hussain. 1998. Role of inducible nitric oxide synthase in endotoxin-induced acute lung injury. American Journal of Respiratory and Critical Care Medicine 158(6): 1883–9. doi:10.1164/ajrccm.158.6.9802100.
Zhou, X., and C. Xue. 2010. Ghrelin attenuates acute pancreatitis-induced lung injury and inhibits substance P expression. American Journal of the Medical Sciences 339(1): 49–54. doi:10.1097/MAJ.0b013e3181b9c3d3.
Chen, J., X. Liu, Q. Shu, S. Li, and F. Luo. 2008. Ghrelin attenuates lipopolysaccharide-induced acute lung injury through NO pathway. Medical Science Monitor 14(7): R141–6.
Wu, R., W. Dong, M. Zhou, F. Zhang, C.P. Marini, T.S. Ravikumar, et al. 2007. Ghrelin attenuates sepsis-induced acute lung injury and mortality in rats. American Journal of Respiratory and Critical Care Medicine 176(8): 805–13. doi:10.1164/rccm.200604-511OC.
Kinnula, V.L., and J.D. Crapo. 2003. Superoxide dismutases in the lung and human lung diseases. American Journal of Respiratory and Critical Care Medicine 167(12): 1600–19. doi:10.1164/rccm.200212-1479SO.
Hassett, P., G.F. Curley, M. Contreras, C. Masterson, B.D. Higgins, T. O’Brien, et al. 2011. Overexpression of pulmonary extracellular superoxide dismutase attenuates endotoxin-induced acute lung injury. Intensive Care Medicine 37(10): 1680–7. doi:10.1007/s00134-011-2309-y.
Yen, C.C., Y.W. Lai, H.L. Chen, C.W. Lai, C.Y. Lin, W. Chen, et al. 2011. Aerosolized human extracellular superoxide dismutase prevents hyperoxia-induced lung injury. PLoS One 6(10): e26870. doi:10.1371/journal.pone.0026870.
Pacher, P., J.S. Beckman, and L. Liaudet. 2007. Nitric oxide and peroxynitrite in health and disease. Physiological Reviews 87(1): 315–424. doi:10.1152/physrev.00029.2006.
Kwan, R.O., E. Cureton, K. Dozier, B. Curran, J. Sadjadi, and G.P. Victorino. 2010. Ghrelin decreases microvascular leak during inflammation. Journal of Trauma 68(5): 1186–91. doi:10.1097/TA.0b013e3181bb9878.
Rittirsch, D., M.S. Huber-Lang, M.A. Flierl, and P.A. Ward. 2009. Immunodesign of experimental sepsis by cecal ligation and puncture. Nature Protocols 4(1): 31–6. doi:10.1038/nprot.2008.214.
Ware, L.B., and M.A. Matthay. 2001. Alveolar fluid clearance is impaired in the majority of patients with acute lung injury and the acute respiratory distress syndrome. American Journal of Respiratory and Critical Care Medicine 163(6): 1376–83. doi:10.1164/ajrccm.163.6.2004035.
Buras, J.A., B. Holzmann, and M. Sitkovsky. 2005. Animal models of sepsis: setting the stage. Nature Reviews Drug Discovery 4(10): 854–65. doi:10.1038/nrd1854.
Wu, R., M. Zhou, X. Cui, H.H. Simms, and P. Wang. 2003. Ghrelin clearance is reduced at the late stage of polymicrobial sepsis. International Journal of Molecular Medicine 12(5): 777–81.
Lu, M.C., T.A. Liu, M.R. Lee, L. Lin, and W.C. Chang. 2002. Apoptosis contributes to the decrement in numbers of alveolar macrophages from rats with polymicrobial sepsis. Journal of Microbiology, Immunology, and Infection 35(2): 71–7.
Sudar, E., B. Dobutovic, S. Soskic, V. Mandusic, Z. Zakula, M. Misirkic, et al. 2011. Regulation of inducible nitric oxide synthase activity/expression in rat hearts from ghrelin-treated rats. Journal of Physiology and Biochemistry 67(2): 195–204. doi:10.1007/s13105-010-0063-1.
Bonni, A., A. Brunet, A.E. West, S.R. Datta, M.A. Takasu, and M.E. Greenberg. 1999. Cell survival promoted by the Ras-MAPK signaling pathway by transcription-dependent and -independent mechanisms. Science 286(5443): 1358–62.
Granado, M., J.A. Chowen, C. Garcia-Caceres, A. Delgado-Rubin, V. Barrios, E. Castillero, et al. 2009. Ghrelin treatment protects lactotrophs from apoptosis in the pituitary of diabetic rats. Molecular and Cellular Endocrinology 309(1–2): 67–75. doi:10.1016/j.mce.2009.06.006.
Rezaeian, F., R. Wettstein, C. Scheuer, K. Baumker, A. Bachle, B. Vollmar, et al. 2012. Ghrelin protects musculocutaneous tissue from ischemic necrosis by improving microvascular perfusion. American Journal of Physiology. Heart and Circulatory Physiology 302(3): H603–10. doi:10.1152/ajpheart.00390.2010.
Acknowledgments
Mian Zeng, guarantor of the entire manuscript, conceived the study, participated in its design, and drafted the manuscript. Wanmei He carried out operation on animals, samples detection, and drafted the manuscript. Lijun Li helped to translate the manuscript. Bin Li participated in the collection of samples. Liang Luo and Weiling Chen participated in the blood sample collection. Xubin Huang and Kaipan Guan performed the statistical analysis. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Mian Zeng and Wanmei He are first co-authors.
Rights and permissions
About this article
Cite this article
Zeng, M., He, W., Li, L. et al. Ghrelin Attenuates Sepsis-Associated Acute Lung Injury Oxidative Stress in Rats. Inflammation 38, 683–690 (2015). https://doi.org/10.1007/s10753-014-9977-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-014-9977-z