Abstract
Background
When unintentional pancreatic duct access occurs during difficult biliary cannulation, the double guidewire (DGW) or transpancreatic sphincterotomy (TPS) may be utilized. DGW can be easily switched to TPS due to the existing guidewire in the pancreatic duct. However, the efficacy of TPS after DGW, named sequential DGW-TPS technique, versus primary TPS has not been assessed.
Aims
Our aim was to compare the benefits and adverse events of sequential DGW-TPS technique and primary TPS.
Methods
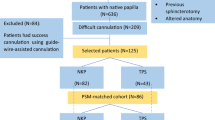
We performed a comparative retrospective cohort study that enrolled a total of 117 patients with native papillae. The patients were divided into one of 2 groups according to the primary bile duct access technique (sequential DGW-TPS or primary TPS), both with pancreatic stenting.
Results
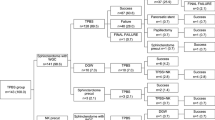
Between November 2017 and May 2023, a total of 84 patients were grouped into sequential DGW-TPS and 33 into primary TPS. The overall post-ERCP pancreatitis (PEP) rate was 4.3% in the entire cohort, with no statistical differences were observed between the groups in terms of PEP rates (P = 0.927), PEP severity (P = 1.000), first biliary cannulation success (P = 0.621), overall cannulation success (P = 1.000), hyperamylasemia incidence (P = 0.241), elevated amylase levels (P = 0.881), and postoperative hospital stay (P = 0.185). Furthermore, these results remained consistent in multivariable regression analysis.
Conclusions
The sequential DGW-TPS technique showed a comparable safety and biliary cannulation success rate to primary TPS in difficult biliary cannulation. Given the potential long-term complications associated with TPS, DGW should be first if inadvertent pancreatic access occurs, with TPS serving as second only if DGW fails.
Graphical Abstract
A retrospective cohort study was conducted to compare the safety and efficacy of the 33 sequential DGW-TPS and 84 primary TPS techniques. No significant differences were found in PEP, cannulation success, or other AEs. Multivariable regression analysis reaffirmed these findings. The sequential DGW-TPS technique showed a comparable safety and efficacy to primary TPS, supporting its use if inadvertent pancreatic access occurs.


Similar content being viewed by others
Abbreviations
- ERCP:
-
Endoscopic retrograde cholangiopancreatography
- PEP:
-
Post-ERCP pancreatitis
- AEs:
-
Adverse events
- PD:
-
Pancreatic duct
- DGW:
-
Double guidewire
- TPS:
-
Transpancreatic sphincterotomy
- SDTT:
-
Sequential DGW-TPS technique
- PTPS:
-
Primary transpancreatic sphincterotomy
- CBD:
-
Common bile duct
- GI:
-
Gastrointestinal
- OR:
-
Odds ratio
- CI:
-
Confidence interval
- RCT:
-
Randomized controlled trial
References
Laquiere A, Privat J, Jacques J et al. Early double-guidewire versus repeated single-guidewire technique to facilitate selective bile duct cannulation: a randomized controlled trial. Endoscopy 2022;54:120–127. https://doi.org/10.1055/a-1395-7485.
Thiruvengadam NR, Forde KA, Ma GK et al. Rectal indomethacin reduces pancreatitis in high- and low-risk patients undergoing endoscopic retrograde cholangiopancreatography. Gastroenterology 2016;151:288–297. https://doi.org/10.1053/j.gastro.2016.04.048.
Berry R, Han JY, Tabibian JH. Difficult biliary cannulation: Historical perspective, practical updates, and guide for the endoscopist. World J Gastrointest Endosc 2019;11:5–21. https://doi.org/10.4253/wjge.v11.i1.5.
Jang SI, Kim DU, Cho JH et al. Primary needle-knife fistulotomy versus conventional cannulation method in a high-risk cohort of post-endoscopic retrograde cholangiopancreatography pancreatitis. Am J Gastroenterol 2020;115:616–624. https://doi.org/10.14309/ajg.0000000000000480.
Op DWM, Schirra J, Schulz C et al. Biliary cannulation in endoscopic retrograde cholangiography: how to tackle the difficult papilla. Dig Dis 2022;40:85–96. https://doi.org/10.1159/000515692.
Testoni PA, Mariani A, Aabakken L et al. Papillary cannulation and sphincterotomy techniques at ERCP: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline. Endoscopy. 2016;48:657–683. https://doi.org/10.1055/s-0042-108641.
Huang L, Yu QS, Zhang Q et al. Comparison between double-guidewire technique and transpancreatic sphincterotomy technique for difficult biliary cannulation. Dig Endosc. 2015;27:381–387. https://doi.org/10.1111/den.12387.
Laquiere A, Desilets E, Belle A et al. Double guidewire endoscopic technique, a major evolution in endoscopic retrograde cholangiopancreatography: results of a retrospective study with historical controls comparing two therapeutic sequential strategies. Dig Endosc. 2017;29:182–189. https://doi.org/10.1111/den.12740.
Pin F, Conti BM, Crino SF et al. Double guide-wire technique versus transpancreatic biliary sphincterotomy for difficult biliary cannulation: Real life experience from a referral center. Dig Liver Dis. 2022;54:1548–1553. https://doi.org/10.1016/j.dld.2022.07.011.
Sundaram S, Jagtap N. Transpancreatic biliary sphincterotomy: justified or overkill? Endoscopy. 2021;53:985. https://doi.org/10.1055/a-1408-3258.
Sugiyama H, Tsuyuguchi T, Sakai Y et al. Transpancreatic precut papillotomy versus double-guidewire technique in difficult biliary cannulation: prospective randomized study. Endoscopy. 2018;50:33–39. https://doi.org/10.1055/s-0043-118000.
Kylanpaa L, Koskensalo V, Saarela A et al. Transpancreatic biliary sphincterotomy versus double guidewire in difficult biliary cannulation: a randomized controlled trial. Endoscopy. 2021;53:1011–1019. https://doi.org/10.1055/a-1327-2025.
Facciorusso A, Ramai D, Gkolfakis P et al. Comparative efficacy of different methods for difficult biliary cannulation in ERCP: systematic review and network meta-analysis. Gastrointest Endosc. 2022;95:60–71. https://doi.org/10.1016/j.gie.2021.09.010.
Kylanpaa L, Koskensalo V, Udd M et al. Reply to Sundaram and Jagtap. Endoscopy. 2021;53:986. https://doi.org/10.1055/a-1408-3754.
Shi QQ, Ning XY, Zhan LL et al. Placement of prophylactic pancreatic stents to prevent post-endoscopic retrograde cholangiopancreatography pancreatitis in high-risk patients: a meta-analysis. World J Gastroenterol. 2014;20:7040–7048. https://doi.org/10.3748/wjg.v20.i22.7040.
Choudhary A, Bechtold ML, Arif M et al. Pancreatic stents for prophylaxis against post-ERCP pancreatitis: a meta-analysis and systematic review. Gastrointest Endosc. 2011;73:275–282. https://doi.org/10.1016/j.gie.2010.10.039.
Jowell PS, Baillie J, Branch MS et al. Quantitative assessment of procedural competence. A prospective study of training in endoscopic retrograde cholangiopancreatography. Ann Intern Med. 1996;125:983–989. https://doi.org/10.7326/0003-4819-125-12-199612150-00009.
IAP, Working Group. IAP/APA evidence-based guidelines for the management of acute pancreatitis. Pancreatology. 2013;13:1–15. https://doi.org/10.1016/j.pan.2013.07.063.
Cotton PB, Eisen GM, Aabakken L et al. A lexicon for endoscopic adverse events: report of an ASGE workshop. Gastrointest Endosc. 2010;71:446–454. https://doi.org/10.1016/j.gie.2009.10.027.
Zou XP, Leung JW, Li YH et al. Comparison of sequential pancreatic duct guidewire placement technique and needle knife precut sphincterotomy for difficult biliary cannulation. J Dig Dis. 2015;16:741–746. https://doi.org/10.1111/1751-2980.12300.
Kim CW, Chang JH, Kim TH et al. Sequential double-guidewire technique and transpancreatic precut sphincterotomy for difficult biliary cannulation. Saudi J Gastroenterol. 2015;21:18–24. https://doi.org/10.4103/1319-3767.151212.
Elmunzer BJ. Reducing the risk of post-endoscopic retrograde cholangiopancreatography pancreatitis. Dig Endosc. 2017;29:749–757. https://doi.org/10.1111/den.12908.
Akshintala VS, Kanthasamy K, Bhullar FA et al. Incidence, severity, and mortality of post-ERCP pancreatitis: an updated systematic review and meta-analysis of 145 randomized controlled trials. Gastrointest Endosc. 2023;98:1–6. https://doi.org/10.1016/j.gie.2023.03.023.
Goff JS. Common bile duct pre-cut sphincterotomy: transpancreatic sphincter approach. Gastrointest Endosc. 1995;41:502–505. https://doi.org/10.1016/s0016-5107(05)80011-2.
Buscaglia JM, Kalloo AN. Pancreatic sphincterotomy: technique, indications, and complications. World J Gastroenterol. 2007;13:4064–4071. https://doi.org/10.3748/wjg.v13.i30.4064.
Kozarek R. Flail, flay, or fail: needle-knife versus transpancreatic sphincterotomy to access the difficult-to-cannulate bile duct during ERCP. Endoscopy. 2017;49:842–843. https://doi.org/10.1055/s-0043-117045.
Acknowledgments
None.
Author information
Authors and Affiliations
Contributions
RH, QM, and JB conceived and designed the study. SL, YF, CZ, XC, QH, JW, and JH acquired the data. SW analyzed and interpreted the data. SW drafted and edited the manuscript. YL, ZX, and XL critically reviewed the manuscript for important intellectual content. BQB did the statistical analysis. The authors alone are responsible for the content and the writing of the paper.
Corresponding author
Ethics declarations
Competing interests
We declare no competing interests.
Ethics approval
The research protocol has been approved by the Hospital Research Ethics Committee (No. Quick-PJ 2023–09-14).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, S., Bai, B., Liu, S. et al. Transpancreatic Sphincterotomy After Double Guidewire Technique Was Noninferior to Primary Transpancreatic Sphincterotomy in Difficult Biliary Cannulation. Dig Dis Sci (2024). https://doi.org/10.1007/s10620-024-08319-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10620-024-08319-7