Abstract
Purpose
Epidemiological studies on alcohol consumption and the risk of myelodysplastic syndromes (MDS) have been inconclusive. We evaluated the association between alcohol consumption and MDS risk in a Chinese population.
Methods
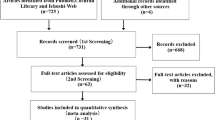
A hospital-based case–control study was conducted between 2012 and 2013 in Hangzhou, China. The analysis included 208 case–control pairs. Diagnosis of MDS was confirmed according to the 2008 World Health Organization classification system. Controls were individually matched to the cases by gender, birth quinquennium, and residential locality. Information on habitual alcohol consumption, diet, and lifestyle was sought from face-to-face interview using a validated questionnaire. Odds ratios (ORs) were calculated using conditional logistic regression.
Results
Fewer cases (36.5 %) were classified as alcohol drinkers compared with the controls (48.6 %). Compared with abstainers, the adjusted OR for alcohol drinkers was 0.41 (95 % CI 0.21–0.80), and significant reduced risks were found for light alcohol consumption (≤12.5 g/day of ethanol) and for wine consumption, adjusted ORs (95 % CIs) being 0.27 (0.12–0.61) and 0.12 (0.02–0.79), respectively. Compared with individuals who consumed neither alcohol nor cigarettes, the reduced risk associated with light alcohol consumption was only statistically significant among non-smokers (OR 0.19, 95 % CI 0.06–0.60).
Conclusions
The findings suggest a favorable role of light alcohol consumption in MDS, particularly among non-smokers.
Similar content being viewed by others
References
Tefferi A, Vardiman JW (2009) Myelodysplastic syndromes. N Engl J Med 361:1872–1885
Rollison DE, Howlader N, Smith MT, Strom SS, Merritt WD, Ries LA et al (2008) Epidemiology of myelodysplastic syndromes and chronic myeloproliferative disorders in the United States, 2001–2004, using data from the NAACCR and SEER programs. Blood 112:45–52
Rodger EJ, Morison IM (2012) Myelodysplastic syndrome in New Zealand and Australia. Intern Med J 42:1235–1242
Chihara D, Ito H, Katanoda K, Shibata A, Matsuda T, Sobue T et al (2014) Incidence of myelodysplastic syndrome in Japan. J Epidemiol 24:469–473
Wang W, Wang H, Wang XQ, Lin GW (2012) First report of incidence of adult myelodysplastic syndrome in China. Ann Hematol 91:1321–1322
Brown LM, Gibson R, Burmeister LF, Schuman LM, Everett GD, Blair A (1992) Alcohol consumption and risk of leukemia, non-Hodgkin’s lymphoma, and multiple myeloma. Leuk Res 16:979–984
Ido M, Nagata C, Kawakami N, Shimizu H, Yoshida Y, Nomura T et al (1996) A case–control study of myelodysplastic syndromes among Japanese men and women. Leuk Res 20:727–731
Nagata C, Shimizu H, Hirashima K, Kakishita E, Fujimura K, Niho Y et al (1999) Hair dye use and occupational exposure to organic solvents as risk factors for myelodysplastic syndrome. Leuk Res 23:57–62
Dalamaga M, Petridou E, Cook FE, Trichopoulos D (2002) Risk factors for myelodysplastic syndromes: a case–control study in Greece. Cancer Causes Control 13:603–608
Strom SS, Gu Y, Gruschkus SK, Pierce SA, Estey EH (2005) Risk factors of myelodysplastic syndromes: a case–control study. Leukemia 19:1912–1918
Pekmezovic T, Suvajdzic Vukovic N, Kisic D, Grgurevic A, Bogdanovic A, Gotic M et al (2006) A case–control study of myelodysplastic syndromes in Belgrade (Serbia Montenegro). Ann Hematol 85:514–519
Lv L, Lin G, Gao X, Wu C, Dai J, Yang Y et al (2011) Case–control study of risk factors of myelodysplastic syndromes according to World Health Organization classification in a Chinese population. Am J Hematol 86:163–169
Ma X, Lim U, Park Y, Mayne ST, Wang R, Hartge P et al (2009) Obesity, lifestyle factors, and risk of myelodysplastic syndromes in a large US cohort. Am J Epidemiol 169:1492–1499
Jin J, Yu M, Hu C, Ye L, Xie L, Chen F et al (2014) Alcohol consumption and risk of myelodysplastic syndromes: a meta-analysis of epidemiological studies. Mol Clin Oncol 2:1115–1120
Liu P, Zhang M, Jin J, Holman D (2015) Tea consumption reduces the risk of de novo myelodysplastic syndromes. Leuk Res 39:164–169
Zhang M, Holman CD (2011) Low-to-moderate alcohol intake and breast cancer risk in Chinese women. Br J Cancer 105:1089–1095
Ji BT, Chow WH, Yang G, McLaughlin JK, Zheng W, Shu XO et al (1998) Dietary habits and stomach cancer in Shanghai, China. Int J Cancer 76:659–664
Thompson FE, Byers T (1994) Dietary assessment resource manual. J Nutr 124:2245S–2317S
Hankin JH, Wilkens LR, Kolonel LN, Yoshizawa CN (1991) Validation of a quantitative diet history method in Hawaii. Am J Epidemiol 133:616–628
Australian Bureau of Statistics (1997). National Health Survey Summary of Results (1995). ABS Catalogue No. 4364.0. Australian Bureau of Statistics, Canberra. http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/4364.01995
Jian L, Binns CW, Lee AH (2006) Validity of a food-frequency questionnaire for elderly men in southeast China. Public Health Nutr 9:928–933
Zhang M, Binns CW, Lee AH (2005) A quantitative food frequency questionnaire for women in southeast China: development and reproducibility. Asia Pac J Public Health 17:29–35
Shu XO, Yang G, Jin F, Liu D, Kushi L, Wen W et al (2004) Validity and reproducibility of the food frequency questionnaire used in the Shanghai Women’s Health Study. Eur J Clin Nutr 58:17–23
National Institute of Nutrition and Food Safety, Chinese Center for Disease Control and Prevention (2009) China food composition, book 1, 2nd edn. Peking University Medical Press, Beijing
Fedirko V, Tramacere I, Bagnardi V, Rota M, Scotti L, Islami F et al (2011) Alcohol drinking and colorectal cancer risk: an overall and dose–response meta-analysis of published studies. Ann Oncol 22:1958–1972
Breslow NE, Day NE (1980) Statistical methods in cancer research, vol 1: the analysis of case–control studies. IARC scientific publications no. 32. International Agency for Research on Cancer, Lyon
Rothman KJ, Greenland S, Lash TL (2008) Modern epidemiology, 3rd edn. Lippincott Williams & Wilkins, Philadelphia
Du Y, Fryzek J, Sekeres MA, Taioli E (2010) Smoking and alcohol intake as risk factors for myelodysplastic syndromes (MDS). Leuk Res 34:1–5
Ma X, Park Y, Mayne ST, Wang R, Sinha R, Hollenbeck AR et al (2010) Diet, lifestyle, and acute myeloid leukemia in the NIH-AARP cohort. Am J Epidemiol 171:312–322
Romeo J, Warnberg J, Nova E, Diaz LE, Gomez-Martinez S, Marcos A (2007) Moderate alcohol consumption and the immune system: a review. Br J Nutr 98:S111–S115
Smith C, Gasparetto M, Jordan C, Pollyea DA, Vasiliou V (2015) The effects of alcohol and aldehyde dehydrogenases on disorders of hematopoiesis. Adv Exp Med Biol 815:349–359
Tsan MF, White JE, Maheshwari JG, Chikkappa G (2002) Anti-leukemia effect of resveratrol. Leuk Lymphoma 43:983–987
Edenberg HJ (2007) The genetics of alcohol metabolism: role of alcohol dehydrogenase and aldehyde dehydrogenase variants. Alcohol Res Health 30:5–13
Tong H, Hu C, Yin X, Yu M, Yang J, Jin J (2013) A meta-analysis of the relationship between cigarette smoking and incidence of myelodysplastic syndromes. PLoS One 8:e67537
Li L, Zhang M, Holman D (2011) Population versus hospital controls for case–control studies on cancers in Chinese hospitals. BMC Med Res Methodol 11:167
Acknowledgments
The authors are grateful to the participants who participated in this study. We thank Dr. Hong-Yan Tong, Dr. Li-Hong Cao, and other staff from the First Affiliated Hospital of Zhejiang University for their kind assistance with fieldwork. Ping Liu was supported by the Scholarship for International Research Fees and the University Postgraduate Award of The University of Western Australia.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Liu, P., Holman, C.D.J., Jin, J. et al. Alcohol consumption and risk of myelodysplastic syndromes: a case–control study. Cancer Causes Control 27, 209–216 (2016). https://doi.org/10.1007/s10552-015-0698-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-015-0698-x