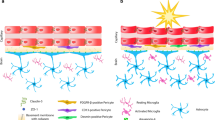
Abstract
Traumatic brain injury (TBI) resulting from explosive-related blast overpressure is a topic at the forefront of neurotrauma research. Compromise of the blood–brain barrier (BBB) and other cerebral blood vessel dysfunction is commonly reported in both experimental and clinical studies on blast injury. This study used a rifle primer-driven shock tube to investigate cerebrovascular injury in rats exposed to low-impulse, pure primary blast at three levels of overpressure (145, 232, and 323 kPa) and with three survival times (acute, 24, and 48 h). BBB disruption was quantified immunohistochemically by measuring immunoglobulin G (IgG) extravasation with image analysis techniques. Pure primary blast generated small lesions scattered throughout the brain. The number and size of lesions increased with peak overpressure level, but no significant difference was seen between survival times. Despite laterally directed blast exposure, equal numbers of lesions were found in each hemisphere of the brain. These observations suggest that cerebrovascular injury due to primary blast is distinct from that associated with conventional TBI.






Similar content being viewed by others
References
Armonda, R. A., R. S. Bell, A. H. Vo, G. Ling, T. J. DeGraba, B. Crandall, J. Ecklund, and W. W. Campbell. Wartime traumatic cerebral vasospasm: recent review of combat casualties. Neurosurgery 59:1215–1225, 2006.
Axelsson, H., H. Hjelmqvist, A. Medin, J. K. Persson, and A. Suneson. Physiological changes in pigs exposed to a blast wave from a detonating high-explosive charge. Mil. Med. 165:119–126, 2000.
Bass, C. R., M. B. Panzer, K. A. Rafaels, G. Wood, J. Shridharani, and B. Capehart. Brain injuries from blast. Ann. Biomed. Eng. 40:185–202, 2012.
Bauman, R. A., G. S. Ling, L. Tong, A. Januszkiewicz, D. Agoston, N. Delanerolle, J. Kim, D. Ritzel, R. Bell, J. M. Ecklund, et al. An introductory characterization of a combat-casualty-care relevant swine model of closed head injury resulting from exposure to explosive blast. J. Neurotrauma 26:841–860, 2009.
Bolander, R., B. Mathie, C. Bir, D. Ritzel, and P. VandeVord. Skull flexure as a contributing factor in the mechanism of injury in the rat when exposed to a shock wave. Ann. Biomed. Eng. 39:2550–2559, 2011.
Bowen, I. G., E. R. Fletcher, D. R. Richmond, F. G. Hirsch, and C. S. White. Biophysical mechanisms and scaling procedures applicable in assessing responses of the thorax energized by air-blast overpressures or by nonpenetrating missiles. Ann. N. Y. Acad. Sci. 152:122–146, 1968.
Cavaglia, M., S. M. Dombrowski, J. Drazba, A. Vasanji, P. M. Bokesch, and D. Janigro. Regional variation in brain capillary density and vascular response to ischemia. Brain Res. 910:81–93, 2001.
Cernak, I., and L. J. Noble-Haeusslein. Traumatic brain injury: an overview of pathobiology with emphasis on military populations. J. Cereb. Blood Flow Metab. 30:255–266, 2010.
Cernak, I., J. Savic, Z. Malicevic, G. Zunic, P. Radosevic, I. Ivanovic, and L. Davidovic. Involvement of the central nervous system in the general response to pulmonary blast injury. J. Trauma 40:100–104, 1996.
Cernak, I., Z. Wang, J. Jiang, X. Bian, and J. Savic. Ultrastructural and functional characteristics of blast injury-induced neurotrauma. J. Trauma 50:695–706, 2001.
Chavko, M., T. Watanabe, S. Adeeb, J. Lankasky, S. T. Ahlers, and R. M. McCarron. Relationship between orientation to a blast and pressure wave propagation inside the rat brain. J. Neurosci. Methods 195:61–66, 2011.
Courtney, M. W., and A. C. Courtney. Note: a table-top blast driven shock tube. Rev. Sci. Instrum. 81:126103, 2010.
Croll, S. D., R. M. Ransohoff, N. Cai, Q. Zhang, F. J. Martin, T. Wei, L. J. Kasselman, J. Kintner, A. J. Murphy, G. D. Yancopoulos, et al. VEGF-mediated inflammation precedes angiogenesis in adult brain. Exp. Neurol. 187:388–402, 2004.
Cullis, I. G. Blast waves and how they interact with structures. J. R. Army Med. Corps 147:16–26, 2001.
Dal Cengio Leonardi, A., N. J. Keane, C. A. Bir, A. G. Ryan, L. Xu, and P. J. VandeVord. Head orientation affects the intracranial pressure response resulting from shock wave loading in the rat. J. Biomech. 45:2595–2602, 2012.
DeWitt, D. S., and D. S. Prough. Blast-induced brain injury and posttraumatic hypotension and hypoxemia. J. Neurotrauma 26:877–887, 2009.
Elsayed, N. M. Toxicology of blast overpressure. Toxicology 121:1–15, 1997.
Garman, R. H., L. W. Jenkins, R. C. Switzer, R. A. Bauman, L. C. Tong, P. V. Swauger, S. A. Parks, D. V. Ritzel, C. E. Dixon, R. S. B. Clark, et al. Blast exposure in rats with body shielding is characterized primarily by diffuse axonal injury. J. Neurotrauma 28:947–959, 2011.
Goldstein, L. E., A. M. Fisher, C. A. Tagge, X.-L. Zhang, L. Velisek, J. A. Sullivan, C. Upreti, J. M. Kracht, M. Ericsson, M. W. Wojnarowicz, et al. Chronic traumatic encephalopathy in blast-exposed military veterans and a blast neurotrauma mouse model. Sci. Transl. Med. 4:134ra160, 2012.
Graham, D. I. Neuropathology of head injury. In: Neurotrauma, edited by R. K. Nrayan, J. E. Wilberger, and J. T. Povlishock. New York: McGraw-Hill, 1996, pp. 43–59.
Klatzo, I. Blood–brain barrier and ischaemic brain oedema. Z. Kardiol. 76:67–69, 1987.
Long, J. B., T. L. Bentley, K. A. Wessner, C. Cerone, S. Sweeney, and R. A. Bauman. Blast overpressure in rats: recreating a battlefield injury in the laboratory. J. Neurotrauma 26:827–840, 2009.
Lossinsky, A. S., and R. R. Shivers. Structural pathways for macromolecular and cellular transport across the blood–brain barrier during inflammatory conditions. Rev. Histol. Histopathol. 19:535–564, 2004.
Moss, W. C., M. J. King, and E. G. Blackman. Skull flexure from blast waves: a mechanism for brain injury with implications for helmet design. Phys. Rev. Lett. 103:108702, 2009.
Mouritz, A. P. Ballistic impact and explosive blast resistance of stitched composites. Compos. B Eng. 32:431–439, 2001.
Ohtake, M., S. Morino, T. Kaidoh, and T. Inoue. Three-dimensional structural changes in cerebral microvessels after transient focal cerebral ischemia in rats: scanning electron microscopic study of corrosion casts. Neuropathology 24:219–227, 2004.
Paxinos, G., and C. Watson. The rat brain in stereotaxic coordinates (4th ed.). San Diego: Academic Press, 1998.
Rafaels, K. A., C. R. Bass, M. B. Panzer, R. S. Salzar, W. A. Woods, S. H. Feldman, T. Walilko, R. W. Kent, B. P. Capehart, J. B. Foster, et al. Brain injury risk from primary blast. J. Trauma. Acute. Care. Surg. 73:895–901, 2012.
Readnower, R. D., M. Chavko, S. Adeeb, M. D. Conroy, J. R. Pauly, R. M. McCarron, and P. G. Sullivan. Increase in blood–brain barrier permeability, oxidative stress, and activated microglia in a rat model of blast-induced traumatic brain injury. J. Neurosci. Res. 88:3530–3539, 2010.
Reneer, D. V. Blast-induced brain injury influence of shockwave components. Lexington, KY: University of Kentucky, 2012.
Saljo, A., F. Arrhen, H. Bolouri, M. Mayorga, and A. Hamberger. Neuropathology and pressure in the pig brain resulting from low-impulse noise exposure. J. Neurotrauma 25:1397–1406, 2008.
Svetlov, S. I., V. Prima, O. Glushakova, A. Svetlov, D. R. Kirk, H. Gutierrez, V. L. Serebruany, K. C. Curley, K. K. Wang, and R. L. Hayes. Neuro-glial and systemic mechanisms of pathological responses in rat models of primary blast overpressure compared to “composite” blast. Front. Neurol. 3:15, 2012.
White, C. S. The scope of blast and shock biology and problem areas in relating physical and biological parameters. Ann. N. Y. Acad. Sci. 152:89–102, 1968.
Acknowledgments
Funding for this research was provided by the Department of Defense (W81XWH-08-1-0295). The authors would like to acknowledge Jordan Walker and Louise Butler for assistance with tissue processing, imaging, and data analysis.
Conflict of interest
No conflicting financial interests exist.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Stefan M Duma oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Yeoh, S., Bell, E.D. & Monson, K.L. Distribution of Blood–Brain Barrier Disruption in Primary Blast Injury. Ann Biomed Eng 41, 2206–2214 (2013). https://doi.org/10.1007/s10439-013-0805-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-013-0805-7