Abstract
Background
The standard of care for treatment of localized muscle-invasive bladder cancer (MIBC) is radical cystectomy (RC). The patient’s condition may affect management of MIBC, especially for elderly patients with more comorbid conditions and lower performance status. We retrospectively evaluated the association between clinicopathological data and outcomes for patients with bladder cancer (BCa) treated by RC. We particularly focused on elderly patients (age ≥75 years) with BCa.
Methods
We enrolled 254 patients with BCa who underwent RC and urinary diversion with or without pelvic lymph node dissection. We assessed perioperative complications and clinicopathological data affecting overall survival (OS) after RC.
Results
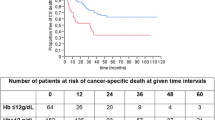
The incidence of complications was 34.3 %, and that of severe complications (Grade 3–5) was 16.5 %. The elderly group experienced more severe complications (P = 0.042). Median follow-up was 43.0 months (range 1.0–155.6). Five-year OS after RC was 62.7 %. OS after RC was no different for patients aged ≥75 and <75 years (P = 0.983). Multivariate analysis revealed that Eastern Cooperative Oncology Group performance status (ECOG PS) and hemoglobin (Hb) concentration were associated with all-cause mortality. Hb concentration of <12.6 g/dl was an independent predictor of a poor prognosis among elderly patients after RC for BCa. ECOG PS >1 tended to affect OS after RC in this group.
Conclusion
ECOG PS and preoperative Hb concentration were useful for prediction of clinical outcome after RC for elderly patients. This information may aid decision-making in the treatment of elderly patients with MIBC.


Similar content being viewed by others
References
Siegel R, Naishadham D, Jemal A (2012) Cancer statistics, 2012. CA Cancer J Clin 62:10–29
Prout GR Jr, Wesley MN, Yancik R et al (2005) Age and comorbidity impact surgical therapy in older bladder carcinoma patients: a population-based study. Cancer 104:1638–1647
Yuge K, Kikuchi E, Matsumoto K et al (2011) Could patient age influence tumor recurrence rate in non-muscle-invasive bladder cancer patients treated with BCG immunotherapy? Jpn J Clin Oncol 41:565–570
Rodel C, Grabenbauer GG, Kuhn R et al (2002) Combined-modality treatment and selective organ preservation in invasive bladder cancer: long-term results. J Clin Oncol 20:3061–3071
Evers PD, Logan JE, Sills V et al (2014) Karnofsky performance status predicts overall survival, cancer-specific survival, and progression-free survival following radical cystectomy for urothelial carcinoma. World J Urol 32:385–391
Charlson ME, Pompei P, Ales KL et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Koppie TM, Serio AM, Vickers AJ et al (2008) Age-adjusted Charlson comorbidity score is associated with treatment decisions and clinical outcomes for patients undergoing radical cystectomy for bladder cancer. Cancer 112:2384–2392
Clavien PA, Barkun J, De Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Clavien PA, Sanabria JR, Strasberg SM (1992) Proposed classification of complications of surgery with examples of utility in cholecystectomy. Surgery 111:518–526
Martinez-Velilla N, Cambra-Contin K, Ibanez-Beroiz B (2014) Comorbidity and prognostic indices do not improve the 5-year mortality prediction of components of comprehensive geriatric assessment in hospitalized elderly patients. BMC Geriatr 14:64
Takada N, Abe T, Shinohara N et al (2012) Peri-operative morbidity and mortality related to radical cystectomy: a multi-institutional retrospective study in Japan. BJU Int 110:E756–E764
Shabsigh A, Korets R, Vora KC et al (2009) Defining early morbidity of radical cystectomy for patients with bladder cancer using a standardized reporting methodology. Eur Urol 55:164–174
Eisenberg MS, Boorjian SA, Cheville JC et al (2013) The SPARC score: a multifactorial outcome prediction model for patients undergoing radical cystectomy for bladder cancer. J Urol 190:2005–2010
Ficarra V, Dalpiaz O, Alrabi N et al (2005) Correlation between clinical and pathological staging in a series of radical cystectomies for bladder carcinoma. BJU Int 95:786–790
Djaladat H, Bruins HM, Miranda G et al (2014) The association of preoperative serum albumin level and American Society of Anesthesiologists (ASA) score on early complications and survival of patients undergoing radical cystectomy for urothelial bladder cancer. BJU Int 113:887–893
Boorjian SA, Kim SP, Tollefson MK et al (2013) Comparative performance of comorbidity indices for estimating perioperative and 5-year all cause mortality following radical cystectomy for bladder cancer 190:55–60
Gondo T, Nakashima J, Ohno Y et al (2012) Prognostic value of neutrophil-to-lymphocyte ratio and establishment of novel preoperative risk stratification model in bladder cancer patients treated with radical cystectomy. Urology 79:1085–1091
Sejima T, Morizane S, Yao A et al (2014) Prognostic impact of preoperative hematological disorders and a risk stratification model in bladder cancer patients treated with radical cystectomy. Int J Urol 21:52–57
Willems JM, Vlasveld T, Den Elzen WP et al (2013) Performance of Cockcroft-Gault, MDRD, and CKD-EPI in estimating prevalence of renal function and predicting survival in the oldest old. BMC Geriatr 13:113
Ploussard G, Shariat SF, Dragomir A et al (2014) Conditional survival after radical cystectomy for bladder cancer: evidence for a patient changing risk profile over time. Eur Urol 66:361–370
Karl A, Carroll PR, Gschwend JE et al (2009) The impact of lymphadenectomy and lymph node metastasis on the outcomes of radical cystectomy for bladder cancer. Eur Urol 55:826–835
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Consortia
Corresponding author
About this article
Cite this article
Hara, T., Matsuyama, H., Kamiryo, Y. et al. Use of preoperative performance status and hemoglobin concentration to predict overall survival for patients aged ≥75 years after radical cystectomy for treatment of bladder cancer. Int J Clin Oncol 21, 139–147 (2016). https://doi.org/10.1007/s10147-015-0857-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-015-0857-9