Abstract
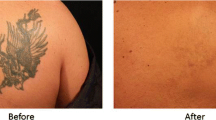
Q-switched lasers have undeniably revolutionized the field of laser dermatology since four decades ago. Just as the first-generation laser emits its photonic signal in a few nanoseconds, the picosecond laser delivers pulse widths of at least ten times shorter. These devices offer a powerful tool for treating a wide range of skin conditions with a minimal downtime for visible improvement. For the current study, a literature research was performed on the dermatological applications of picosecond laser. The literature searched on this topic between 1999 and 2023 accessible through various platforms produce a result of 62 articles. The included studies have discussed the application of picosecond laser technology in tattoo removal, treatment of epidermal and dermal pigmentation, and collagen remodeling. After sifting the data from the articles into tables, the results were discussed in detail. The study shows a lot of evidence towards the efficacy of picosecond laser, yet it draws attention to its downsides.

Similar content being viewed by others
Data availability
The data that support the findings of this study are available on references’ part.
References
Ho D, London R, Zimmerman G, Young D (2002) Laser-tattoo removal—a study of the mechanism and the optimal treatment strategy via computer simulations. Lasers Surg Med 30:389–97
Izikson L, Farinelli W, Sakamoto F, Tannous Z, Anderson RR (2010) Safety and effectiveness of black tattoo clearance in a pig model after a single treatment with a novel 758 nm 500 picosecond laser: a pilot study. Lasers Surg Med 42(7):640–6
Zhou Y, Hamblin MR, Wen X (2023) An update on fractional picosecond laser treatment: histology and clinical applications. Lasers Med Sci 38(1):45
Lyu H, Park J, Lee H, Lee S, Kim Y, Cho SB (2020) In vivo and ex vivo skin reactions after multiple pulses of 1,064-nm, microlens array-type, picosecond laser treatment. Med Lasers 9:142–9
GRADE approach [Internet]. [cité 13 avr 2023]. Disponible sur: https://training.cochrane.org/grade-approach
Bernstein EF, Schomacker KT, Basilavecchio LD, Plugis JM, Bhawalkar JD (2015) A novel dual-wavelength, Nd:YAG, picosecond-domain laser safely and effectively removes multicolor tattoos. Lasers Surg Med sept 47(7):542–548
Friedman DJ (2016) Successful treatment of a red and black professional tattoo in skin type VI with a picosecond dual-wavelength, neodymium-doped yttrium aluminium garnet laser. Dermatol Surg Off Publ Am Soc Dermatol Surg Al 42(9):1121–3
Kauvar ANB, Keaney TC, Alster T (2017) Laser treatment of professional tattoos with a 1064/532-nm dual-wavelength picosecond laser. Dermatol Surg Off Publ Am Soc Dermatol Surg Al 43(12):1434–40
Nguyen HT, Doan EVL, Tran TNA, Vu TTP, Phan HN, Sobanko JF (2021) Safety and efficacy of tattoo removal using a dual-wavelength 1064/532-nm picosecond laser in patients with Fitzpatrick skin type III and IV. Lasers Surg Med sept 53(7):939–945
Alabdulrazzaq H, Brauer JA, Bae YS, Geronemus RG (2015) Clearance of yellow tattoo ink with a novel 532-nm picosecond laser. Lasers Surg Med avr 47(4):285–288
Ross V, Naseef G, Lin G, Kelly M, Michaud N, Flotte TJ et al (1998) Comparison of responses of tattoos to picosecond and nanosecond Q-switched neodymium: YAG lasers. Arch Dermatol févr 134(2):167–171
Herd RM, Alora MB, Smoller B, Arndt KA, Dover JS (1999) A clinical and histologic prospective controlled comparative study of the picosecond titanium:sapphire (795 nm) laser versus the Q-switched alexandrite (752 nm) laser for removing tattoo pigment. J Am Acad Dermatol avr 40(4):603–606
Lorgeou A, Perrillat Y, Gral N, Lagrange S, Lacour JP, Passeron T (2018) Comparison of two picosecond lasers to a nanosecond laser for treating tattoos: a prospective randomized study on 49 patients. J Eur Acad Dermatol Venereol 32(2):265–270
Kato H, Doi K, Kanayama K, Araki J, Nakatsukasa S, Chi D, et al (2020) Combination of dual wavelength picosecond and nanosecond pulse width neodymium-doped yttrium-aluminum-garnet lasers for tattoo removal. Lasers Surg Med 52(6):515‑22.
Bernstein EF, Schomacker KT, Shang X, Alessa D, Algzlan H, Paranjape A (2021) The first commercial 730 nm picosecond-domain laser is safe and effective for treating multicolor tattoos. Lasers Surg Med janv 53(1):89–94
Saedi N, Metelitsa A, Petrell K, Arndt KA, Dover JS (2012) Treatment of tattoos with a picosecond alexandrite laser: a prospective trial. Arch Dermatol déc 148(12):1360–1363
Brauer JA, Reddy KK, Anolik R, Weiss ET, Karen JK, Hale EK et al (2012) Successful and rapid treatment of blue and green tattoo pigment with a novel picosecond laser. Arch Dermatol 148(7):820–3
Lee SH, Lee MH, Noh TK, Choi KH, Won CH, Chang SE et al (2016) Successful treatment of tattoos with a picosecond 755-nm alexandrite laser in Asian skin. Ann Dermatol 28(5):673–675
Bernstein EF, Bhawalkar J, Schomacker KT (2018) A novel titanium sapphire picosecond-domain laser safely and effectively removes purple, blue, and green tattoo inks. Lasers Surg Med 50(7):704–10
Vachiramon V, Namasondhi A, Anuntrangsee T, Jurairattanaporn N (2022) Randomized, evaluator-blinded comparative study of a potassium titanyl phosphate (KTP) 532-nm picosecond laser and an alexandrite 755-nm picosecond laser for the treatment of solar lentigines in Asians. J Cosmet Dermatol 21(10):4370–4377
Vachiramon V, Iamsumang W, Triyangkulsri K (2018) Q-switched double frequency Nd:YAG 532-nm nanosecond laser vs. double frequency Nd:YAG 532-nm picosecond laser for the treatment of solar lentigines in Asians. Lasers Med Sci 33(9):1941–7
Kauvar ANB, Sun R, Bhawan J, Singh G, Ugonabo N, Feng H et al (2022) Treatment of facial and non-facial lentigines with a 730 nm picosecond titanium: sapphire laser is safe and effective. Lasers Surg Med janv 54(1):89–97
Lipp MB, Angra K, Wu DC (2021) Safety and efficacy of a novel 730 nm picosecond titanium sapphire laser for the treatment of benign pigmented lesions. Lasers Surg Med avr 53(4):429–434
Mehrabi JN, Friedman O, Al-Niaimi F, Artzi O (2020) Retrospective photographic review of nontattoo indications treated by picosecond laser. J Cosmet Dermatol 19(3):612–621
Negishi K, Akita H, Matsunaga Y (2018) Prospective study of removing solar lentigines in Asians using a novel dual-wavelength and dual-pulse width picosecond laser. Lasers Surg Med 50(8):851–858
Guss L, Goldman MP, Wu DC (2017) Picosecond 532 nm neodymium-doped yttrium aluminium garnet laser for the treatment of solar lentigines in darker skin types: safety and efficacy. Dermatol Surg 43(3):456–9
Chan JCY, Shek SYN, Kono T, Yeung CK, Chan HHL (2016) A retrospective analysis on the management of pigmented lesions using a picosecond 755 nm alexandrite laser in Asians. Lasers Surg Med 48(1):23–9
Lee SJ, Han HS, Hong JK, Park KY, Seo SJ (2020) Successful treatment of pigmentary disorders in Asians with a novel 730-nm picosecond laser. Lasers Surg Med déc 52(10):923–927
Kung KY, Shek SYN, Yeung CK, Chan HHL (2019) Evaluation of the safety and efficacy of the dual wavelength picosecond laser for the treatment of benign pigmented lesions in Asians. Lasers Surg Med janv 51(1):14–22
Chung HJ, McGee JS, Lee SJ (2020) Successful treatment of ephelides in Asian skin using the picosecond 785-nm laser. J Cosmet Dermatol août 19(8):1990–1992
Yang H, Guo L, Jia G, Gong X, Wu Q, Zeng R et al (2021) Treatment of nevus of Ota with 1064 nm picosecond Nd:YAG laser: a retrospective study. Dermatol Ther 34(6):e15152
Loh TY, Wu DC (2021) Novel application of the 730 and 785 nm picosecond titanium sapphire lasers for the treatment of nevus of Ota. Lasers Surg Med 53(9):1141–1145
Artzi O, Mehrabi JN, Koren A, Niv R, Lapidoth M, Levi A (2018) Picosecond 532-nm neodymium-doped yttrium aluminium garnet laser-a novel and promising modality for the treatment of café-au-lait macules. Lasers Med Sci 33(4):693–7
Wu DC (2021) Successful treatment of scalp micropigmentation with 1064 nm picosecond Nd:YAG laser. Lasers Surg Med sept 53(7):935–938
Hamid RN, Yang RG, Munavalli GS (2021) Treatment of imipramine-induced hyperpigmentation with quality-switched ruby and picosecond lasers. JAAD Case Rep 17:12–17
Wong CSM, Chan MWM, Shek SYN, Yeung CK, Chan HHL (2021) Fractional 1064 nm picosecond laser in treatment of melasma and skin rejuvenation in Asians, a prospective study. Lasers Surg Med 53(8):1032–1042
Chalermchai T, Rummaneethorn P (2018) Effects of a fractional picosecond 1,064 nm laser for the treatment of dermal and mixed type melasma. J Cosmet Laser Ther Off Publ Eur Soc Laser Dermatol 20(3):134–9
Hai L, Phuong B, Ha L, Lam V, Van B, Al-Niaimi F (2021) Dual toning method with the combination of picosecond and microsecond Nd:YAG in refractory melasma unresponsive to picosecond alone. J Cutan Aesthetic Surg 14(1):101–6
Levi A, Amitai DB, Mimouni D, Leshem YA, Arzi O, Lapidoth M (2018) Picosecond 532-nm neodymium-doped yttrium aluminum garnet laser—a promising modality for the management of verrucous epidermal nevi. Lasers Med Sci 33(3):597–601
Koren A, Niv R, Cohen S, Artzi O (2019) A 1064-nm neodymium-doped yttrium aluminum garnet picosecond laser for the treatment of hyperpigmented scars. Dermatol Surg Off Publ Am Soc Dermatol Surg Al 45(5):725–9
Al-Niaimi F (2020) Localized argyria from silver nasal piercing unresponsive to Q-switched laser successfully treated with a 1064 picoseconds laser. J Cosmet Dermatol 19(6):1535–1536
Méndez Baca I, Al-Niaimi F, Colina C, Anuzita A (2019) A case of ochronosis successfully treated with the picosecond laser. J Cosmet Dermatol 18(5):1322–1325
Lee HJ, Lee S, Yoon S, Lee J, Kim Y, Choi EH (2018) Postinflammatory hyperpigmentation successfully treated with 1,064-nm picosecond-domain neodymium:yttrium-aluminum-garnet laser. Med Lasers 7:52–4
Leight-Dunn H, Hadi A, Patel F, Yao CJ, Tu YM, Chapas A (2022) The effect of a dual-wavelength 532 nm and 1064 nm picosecond-domain laser with a fractionated holographic optic on photoaging and patient age perception: a pilot study. J Cosmet Dermatol janv 21(1):320–326
Zhang M, Huang Y, Wu Q, Lin T, Gong X, Chen H et al (2021) Comparison of 1064-nm and dual-wavelength (532/1064-nm) picosecond-domain Nd:YAG lasers in the treatment of facial photoaging: a randomized controlled split-face study. Lasers Surg Med 53(9):1158–1165
Kirsanova L, Araviiskaia E, Rybakova M, Sokolovsky E, Bogantenkov A, Al-Niaimi F (2020) Histological characterization of age-related skin changes following the use of picosecond laser: low vs high energy. Dermatol Ther 33(4):e13635
Feng H, Wu Y, Jiang M, Luo X, Yan S, Lu Z (2021) The efficacy and safety of fractional 1064 nm Nd:YAG picosecond laser combined with intense pulsed light in the treatment of atrophic acne scar: a split-face study. Lasers Surg Med 53(10):1356–1363
Shi Y, Jiang W, Li W, Zhang W, Zou Y (2021) Comparison of fractionated frequency-doubled 1,064/532 nm picosecond Nd:YAG lasers and non-ablative fractional 1,540 nm Er: glass in the treatment of facial atrophic scars: a randomized, split-face, double-blind trial. Ann Transl Med mai 9(10):862
Yang CS, Huang YL, Cheng CY, Hu S, Chang SL, Lee MC (2020) A prospective study of fractionated dual-wavelength picosecond laser in treating acne scar. Lasers Surg Med 52(8):735–742
Bernstein EF, Schomacker KT, Basilavecchio LD, Plugis JM, Bhawalkar JD (2017) Treatment of acne scarring with a novel fractionated, dual-wavelength, picosecond-domain laser incorporating a novel holographic beam-splitter. Lasers Surg Med 49(9):796–802
Yeh YT, Peng JH, Peng P (2020) Histology of ex vivo skin after treatment with fractionated picosecond Nd:YAG laser in high and low-energy settings. J Cosmet Laser Ther Off Publ Eur Soc Laser Dermatol 22(1):43–47
Choi YJ, Kim JY, Nam JH, Lee GY, Kim WS (2019) Clinical outcome of 1064-nm picosecond neodymium-doped yttrium aluminium garnet laser for the treatment of hypertrophic scars. J Cosmet Laser Ther Off Publ Eur Soc Laser Dermatol 21(2):91–98
Wu DC, Jones IT, Boen M, Al-Haddad M, Goldman MP (2021) A randomized, split-face, double-blind comparison trial between fractionated frequency-doubled 1064/532 nm picosecond Nd:YAG laser and fractionated 1927 nm thulium fiber laser for facial photorejuvenation. Lasers Surg Med 53(2):204–211
Gold MH (2019) Dual wavelength treatment protocol with a picosecond laser for the reduction of facial wrinkles. J Cosmet Laser Ther 21(3):147–51
Ross EV, Tidwell WJ, Guss L, Sutton AV (2022) Study of a 532/1064 fractional picosecond laser for facial rejuvenation. Dermatol Surg Off Publ Am Soc Dermatol Surg Al 48(1):109–13
Bernstein EF, Schomacker KT, Paranjape AS, Bhawalkar JD (2017) Treatment of photoaging with a dual-wavelength, 532 nm and 1,064 nm picosecond-domain laser producing a fractionated treatment beam using a holographic optic. J Drugs Dermatol JDD 16(11):1077–82
Using normal and high pulse coverage with picosecond laser treatment of wrinkles and acne scarring: long term clinical observations - Dierickx - 2018 - Lasers in Surgery and Medicine - Wiley Online Library [Internet]. [cité 1 mars 2023]. Disponible sur: https://onlinelibrary.wiley.com/doi/10.1002/lsm.22763
Jia X, Zheng L, Fang L, Zhang L, Wu Y, Yang Y et al (2023) Evaluation of the safety and efficacy of a fractional picosecond 1064 nm laser for post-acne erythema in adult Chinese patients. Skin Res Technol 29(1):e13274
Kim JH, Choe S, Kim TG (2020) Post-acne erythema successfully treated with 595-nm picosecond-domain neodymium:yttrium-aluminum-garnet laser. Med Lasers 9:84–7
Haimovic A, Brauer JA, Cindy Bae YS, Geronemus RG (2016) Safety of a picosecond laser with diffractive lens array (DLA) in the treatment of Fitzpatrick skin types IV to VI: a retrospective review. J Am Acad Dermatol mai 74(5):931–936
Treatment of abdominal striae distensae in Fitzpatrick skin types IV to V using a 1064‐nm picosecond laser with a fractionated microlens array. [cité 7 avr 2023]; Disponible sur: https://onlinelibrary.wiley.com/doi/10.1002/lsm.23471
Qu Y, Feng X, Liang J, Liu J, Gao D (2021) The picosecond laser effects on tattoo removal and metabolic pathways. Clin Cosmet Investig Dermatol 14:1343–1350
Tanghetti MdE, Jennings J (2018) A comparative study with a 755 nm picosecond alexandrite laser with a diffractive lens array and a 532 nm/1064 nm Nd:YAG with a holographic optic. Lasers Surg Med janv 50(1):37–44
Chung HJ, Lee HC, Park J, Childs J, Hong J, Kim H et al (2019) Pattern analysis of 532- and 1064-nm microlens array-type, picosecond-domain laser-induced tissue reactions in ex vivo human skin. Lasers Med Sci août 34(6):1207–1215
Chang YS, Yang TH, Li CN. Histology changes of in vivo human skin after treatment with fractional 1064 nm Nd:YAG picosecond laser in different energy settings. Lasers Med Sci. 1 avr 2022;37(3):2087‑92.
Pinto F, Große-Büning S, Karsai S, Weiß C, Bäumler W, Hammes S et al (2017) Neodymium-doped yttrium aluminium garnet (Nd:YAG) 1064-nm picosecond laser vs. Nd:YAG 1064-nm nanosecond laser in tattoo removal: a randomized controlled single-blind clinical trial. Br J Dermatol 176(2):457–64
Zhang M, Huang Y, Lin T, Wu Q (2018) Comparison of treatment with an alexandrite picosecond laser and Nd:YAG nanosecond laser for removing blue-black Chinese eyeliner tattoos. J Cosmet Laser Ther Off Publ Eur Soc Laser Dermatol 20(7–8):415–418
Author information
Authors and Affiliations
Contributions
DH had the concept for the writing with assistance from HC, CM, and SM. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
The authors declare human ethical approval was not needed for this article.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Haykal, D., Cartier, H., Maire, C. et al. Picosecond lasers in cosmetic dermatology: where are we now? An overview of types and indications. Lasers Med Sci 39, 8 (2024). https://doi.org/10.1007/s10103-023-03945-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10103-023-03945-5