Abstract
Purpose
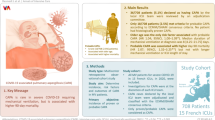
We conducted a monocentric retrospective study using the latest definitions to compare the demographic, clinical, and biological characteristics of influenza-associated pulmonary aspergillosis (IAPA) and COVID-19-associated pulmonary aspergillosis (CAPA).
Methods
The study retrospectively enrolled 180 patients, including 70 influenza/IPA patients (with positive influenza A/B and Aspergillus) and 110 COVID-19/IPA patients (with positive SARS-CoV-2 and Aspergillus). Among them, 42 (60%) and 30 (27.3%) patients fulfilled the definitions of IAPA and CAPA, respectively.
Results
The CAPA patients had significantly higher in-hospital mortality (13/31, 41.9%) than IAPA patients (8/42, 19%) with a P-value of 0.033. Kaplan–Meier survival curve also showed significantly higher 30-day mortality for CAPA patients (P = 0.025). Additionally, the CAPA patients were older, though insignificantly, than IAPA patients (70 (60–80) vs. 62 (52–72), P = 0.075). A lower percentage of chronic pulmonary disease (12.9 vs. 40.5%, P = 0.01) but higher corticosteroids use 7 days before and after ICU admission (22.6% vs. 0%, P = 0.002) were found in CAPA patients. Notably, there were no significant differences in the percentage of ICU admission or ICU mortality between the two groups. In addition, the time from observation to Aspergillus diagnosis was significantly longer in CAPA patients than in IAPA patients (7 (2–13) vs. 0 (0–4.5), P = 0.048).
Conclusion
Patients infected with SARS-CoV-2 and Aspergillus during the concentrated outbreak of COVID-19 in China had generally higher in-hospital mortality but a lower percentage of chronic pulmonary disease than those infected with influenza and Aspergillus. For influenza-infected patients who require hospitalization, close attention should be paid to the risk of invasive aspergillosis upfront.



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are not publicly available due to individual privacy but are available from the corresponding author on reasonable request.
References
Donnelly JP, Chen SC, Kauffman CA, Steinbach WJ, Baddley JW, Verweij PE, Clancy CJ, Wingard JR, Lockhart SR, Groll AH, Sorrell TC, Bassetti M, Akan H, Alexander BD, Andes D, Azoulay E, Bialek R, Bradsher RW, Bretagne S, Calandra T, Caliendo AM, Castagnola E, Cruciani M, Cuenca-Estrella M, Decker CF, Desai SR, Fisher B, Harrison T, Heussel CP, Jensen HE, Kibbler CC, Kontoyiannis DP, Kullberg BJ, Lagrou K, Lamoth F, Lehrnbecher T, Loeffler J, Lortholary O, Maertens J, Marchetti O, Marr KA, Masur H, Meis JF, Morrisey CO, Nucci M, Ostrosky-Zeichner L, Pagano L, Patterson TF, Perfect JR, Racil Z, Roilides E, Ruhnke M, Prokop CS, Shoham S, Slavin MA, Stevens DA, Thompson GR, Vazquez JA, Viscoli C, Walsh TJ, Warris A, Wheat LJ, White PL, Zaoutis TE, Pappas PG (2020) Revision and Update of the Consensus Definitions of Invasive Fungal Disease From the European Organization for Research and Treatment of Cancer and the Mycoses Study Group Education and Research Consortium. Clin Infect Dis 71(6):1367–1376
Feys S, Almyroudi MP, Braspenning R, Lagrou K, Spriet I, Dimopoulos G, Wauters J (2021) A visual and comprehensive review on COVID-19-associated pulmonary aspergillosis (CAPA). J Fungi (Basel) 7(12):1067
Schauwvlieghe A, Rijnders BJA, Philips N, Verwijs R, Vanderbeke L, Van Tienen C, Lagrou K, Verweij PE, Van de Veerdonk FL, Gommers D, Spronk P, Bergmans D, Hoedemaekers A, Andrinopoulou ER, van den Berg C, Juffermans NP, Hodiamont CJ, Vonk AG, Depuydt P, Boelens J, Wauters J, Dutch-Belgian Mycosis study g (2018) Invasive aspergillosis in patients admitted to the intensive care unit with severe influenza: a retrospective cohort study. Lancet Respir Med 6(10):782–792
Taccone FS, Van den Abeele AM, Bulpa P, Misset B, Meersseman W, Cardoso T, Paiva JA, Blasco-Navalpotro M, De Laere E, Dimopoulos G, Rello J, Vogelaers D, Blot SI, Asp ICUSI (2015) Epidemiology of invasive aspergillosis in critically ill patients: clinical presentation, underlying conditions, and outcomes. Crit Care 19(1):7
Verweij PE, Rijnders BJA, Bruggemann RJM, Azoulay E, Bassetti M, Blot S, Calandra T, Clancy CJ, Cornely OA, Chiller T, Depuydt P, Giacobbe DR, Janssen NAF, Kullberg BJ, Lagrou K, Lass-Florl C, Lewis RE, Liu PW, Lortholary O, Maertens J, Martin-Loeches I, Nguyen MH, Patterson TF, Rogers TR, Schouten JA, Spriet I, Vanderbeke L, Wauters J, van de Veerdonk FL (2020) Review of influenza-associated pulmonary aspergillosis in ICU patients and proposal for a case definition: an expert opinion. Intensive Care Med 46(8):1524–1535
Loughlin L, Hellyer TP, White PL, McAuley DF, Conway Morris A, Posso RB, Richardson MD, Denning DW, Simpson AJ, McMullan R (2020) Pulmonary aspergillosis in patients with suspected ventilator-associated pneumonia in UK ICUs. Am J Respir Crit Care Med 202(8):1125–1132
Sharma A, Mishra T, Kumar N, Soubani AO (2020) Influenza-associated aspergillosis: nationwide trends, predictors and outcomes from 2005 to 2014. Chest 158(5):1857–1866
Huang L, Zhai T, Hua L, Zhan Q (2020) Early identification of patients with severe influenza-associated aspergillosis (IAA) in the intensive care unit–an IAA prediction score system (Asper-PreSS). J Infect 81(4):639–646
van de Veerdonk FL, Kolwijck E, Lestrade PP, Hodiamont CJ, Rijnders BJ, van Paassen J, Haas PJ, Oliveira Dos Santos C, Kampinga GA, Bergmans DC, van Dijk K, de Haan AF, van Dissel J, van der Hoeven HG, Verweij PE (2017) Influenza-associated aspergillosis in critically ill patients. Am J Respir Crit Care Med 196(4):524–527
Wauters J, Baar I, Meersseman P, Meersseman W, Dams K, De Paep R, Lagrou K, Wilmer A, Jorens P, Hermans G (2012) Invasive pulmonary aspergillosis is a frequent complication of critically ill H1N1 patients: a retrospective study. Intensive Care Med 38(11):1761–1768
Chong WH, Neu KP (2021) Incidence, diagnosis and outcomes of COVID-19-associated pulmonary aspergillosis (CAPA): a systematic review. J Hosp Infect 113:115–129
Chong WH, Saha BK, Neu KP (2022) Comparing the clinical characteristics and outcomes of COVID-19-associate pulmonary aspergillosis (CAPA): a systematic review and meta-analysis. Infection 50(1):43–56
Muthuri SG, Venkatesan S, Myles PR, Leonardi-Bee J, Al Khuwaitir TS, Al Mamun A, Anovadiya AP, Azziz-Baumgartner E, Baez C, Bassetti M, Beovic B, Bertisch B, Bonmarin I, Booy R, Borja-Aburto VH, Burgmann H, Cao B, Carratala J, Denholm JT, Dominguez SR, Duarte PA, Dubnov-Raz G, Echavarria M, Fanella S, Gao Z, Gerardin P, Giannella M, Gubbels S, Herberg J, Iglesias AL, Hoger PH, Hu X, Islam QT, Jimenez MF, Kandeel A, Keijzers G, Khalili H, Knight M, Kudo K, Kusznierz G, Kuzman I, Kwan AM, Amine IL, Langenegger E, Lankarani KB, Leo YS, Linko R, Liu P, Madanat F, Mayo-Montero E, McGeer A, Memish Z, Metan G, Mickiene A, Mikic D, Mohn KG, Moradi A, Nymadawa P, Oliva ME, Ozkan M, Parekh D, Paul M, Polack FP, Rath BA, Rodriguez AH, Sarrouf EB, Seale AC, Sertogullarindan B, Siqueira MM, Skret-Magierlo J, Stephan F, Talarek E, Tang JW, To KK, Torres A, Torun SH, Tran D, Uyeki TM, Van Zwol A, Vaudry W, Vidmar T, Yokota RT, Zarogoulidis P, Investigators PC, Nguyen-Van-Tam JS (2014) Effectiveness of neuraminidase inhibitors in reducing mortality in patients admitted to hospital with influenza A H1N1pdm09 virus infection: a meta-analysis of individual participant data. Lancet Respir Med 2(5):395–404
Chong WH, Saha BK, Tan CK (2022) Clinical characteristics and outcomes of influenza-associated pulmonary aspergillosis among critically ill patients: a systematic review and meta-analysis. J Hosp Infect 120:98–109
Alanio A, Delliere S, Fodil S, Bretagne S, Megarbane B (2020) Prevalence of putative invasive pulmonary aspergillosis in critically ill patients with COVID-19. Lancet Respir Med 8(6):e48–e49
Arastehfar A, Carvalho A, van de Veerdonk FL, Jenks JD, Koehler P, Krause R, Cornely OA, Perlin DS, Lass-Florl C, Hoenigl M (2020) COVID-19 associated pulmonary aspergillosis (CAPA)-from immunology to treatment. J Fungi (Basel) 6(2):91
Henry BM, Aggarwal G, Wong J, Benoit S, Vikse J, Plebani M, Lippi G (2020) Lactate dehydrogenase levels predict coronavirus disease 2019 (COVID-19) severity and mortality: a pooled analysis. Am J Emerg Med 38(9):1722–1726
Janssen NAF, Nyga R, Vanderbeke L, Jacobs C, Ergun M, Buil JB, van Dijk K, Altenburg J, Bouman CSC, van der Spoel HI, Rijnders BJA, Dunbar A, Schouten JA, Lagrou K, Bourgeois M, Reynders M, van Regenmortel N, Rutsaert L, Lormans P, Feys S, Debavaye Y, Tamion F, Costa D, Maizel J, Dupont H, Chouaki T, Nseir S, Sendid B, Bruggemann RJM, van de Veerdonk FL, Wauters J, Verweij PE (2021) Multinational observational cohort study of COVID-19-associated pulmonary aspergillosis(1). Emerg Infect Dis 27(11):2892–2898
Bartoletti M, Pascale R, Cricca M, Rinaldi M, Maccaro A, Bussini L, Fornaro G, Tonetti T, Pizzilli G, Francalanci E, Giuntoli L, Rubin A, Moroni A, Ambretti S, Trapani F, Vatamanu O, Ranieri VM, Castelli A, Baiocchi M, Lewis R, Giannella M, Viale P, Group PS (2021) Epidemiology of invasive pulmonary aspergillosis among intubated patients with COVID-19: a prospective study. Clin Infect Dis 73(11):e3606–e3614
Xu J, Yang X, Lv Z, Zhou T, Liu H, Zou X, Cao F, Zhang L, Liu B, Chen W, Yu Y, Shu H, Yuan S, Hu M, Huang C, Shang Y (2021) Risk factors for invasive aspergillosis in patients admitted to the intensive care unit with coronavirus disease 2019: a multicenter retrospective study. Front Med (Lausanne) 8:753659
Koehler P, Bassetti M, Chakrabarti A, Chen SCA, Colombo AL, Hoenigl M, Klimko N, Lass-Florl C, Oladele RO, Vinh DC, Zhu LP, Boll B, Bruggemann R, Gangneux JP, Perfect JR, Patterson TF, Persigehl T, Meis JF, Ostrosky-Zeichner L, White PL, Verweij PE, Cornely OA, European Confederation of Medical M, International Society for Human Animal M, Asia Fungal Working G, Group ILIW, Group IPAMW, European Society for Clinical M, Infectious Diseases Fungal Infection Study G, Patients ESGfIiCI, Interregional Association of Clinical M, Antimicrobial C, Medical Mycology Society of N, Medical Mycology Society of China Medicine Education A, Infectious Diseases Working Party of the German Society for H, Medical O, Association of Medical M, Infectious Disease C (2021) Defining and managing COVID-19-associated pulmonary aspergillosis: the 2020 ECMM/ISHAM consensus criteria for research and clinical guidance. Lancet Infect Dis 21(6):e149–e162
van Arkel ALE, Rijpstra TA, Belderbos HNA, van Wijngaarden P, Verweij PE, Bentvelsen RG (2020) COVID-19-associated pulmonary aspergillosis. Am J Respir Crit Care Med 202(1):132–135
Schwartz IS, Friedman DZP, Zapernick L, Dingle TC, Lee N, Sligl W, Zelyas N, Smith SW (2020) High rates of influenza-associated invasive pulmonary aspergillosis may not be universal: a retrospective cohort study from Alberta Canada. Clin Infect Dis 71(7):1760–1763
Peral J, Estella Á, Nuvials X, Rodríguez A, Seijas I, Soriano C, Suberviola B, Zaragoza R (2023) Managing the next wave of influenza and/or SARS-CoV-2 in the ICU—practical recommendations from an expert group for CAPA/IAPA patients. J Fungi 9(3):312
Wu C-J, Cia C-T, Wang H-C, Chen C-W, Lin W-C, Lee J-C, Chen P-S, Hsieh C-C, Li W-T, Su P-L, Liao X-M, Hsieh M-I, Choi P-C, Ko W-C (2022) Clinical and microbiological characteristics of culture-positive, influenza-associated pulmonary aspergillosis: a single-center study in Southern Taiwan, 2016–2019. J Fungi 8(1):49
Reizine F, Pinceaux K, Lederlin M, Autier B, Guegan H, Gacouin A, Luque-Paz D, Boglione-Kerrien C, Bacle A, Le Dare B, Launey Y, Lesouhaitier M, Painvin B, Camus C, Mansour A, Robert-Gangneux F, Belaz S, Le Tulzo Y, Tadie JM, Maamar A, Gangneux JP (2021) Influenza- and COVID-19-associated pulmonary aspergillosis: are the pictures different? J Fungi (Basel) 7(5):388
Piroth L, Cottenet J, Mariet AS, Bonniaud P, Blot M, Tubert-Bitter P, Quantin C (2021) Comparison of the characteristics, morbidity, and mortality of COVID-19 and seasonal influenza: a nationwide, population-based retrospective cohort study. Lancet Respir Med 9(3):251–259
Shadrivova O, Gusev D, Vashukova M, Lobzin D, Gusarov V, Zamyatin M, Zavrazhnov A, Mitichkin M, Borzova Y, Kozlova O, Desyatik E, Burygina E, Ignatyeva S, Oganesyan E, Vasilyeva N, Klimko N, Working G (2021) COVID-19-associated pulmonary aspergillosis in Russia. J Fungi (Basel) 7(12):1059
Lamoth F (2022) Invasive aspergillosis in coronavirus disease 2019: a practical approach for clinicians. Curr Opin Infect Dis 35(2):163–169
Erami M, Hashemi SJ, Raiesi O, Fattahi M, Getso MI, Momen-Heravi M, Daie Ghazvini R, Khodavaisy S, Parviz S, Mehri N, Babaei M (2023) COVID-19-associated pulmonary aspergillosis (CAPA) in Iranian patients admitted with severe COVID-19 pneumonia. Infection 51(1):223–230
Rana M, Khan S, Pervez M, Fatimi S (2020) Giant pneumatocele secondary to Aspergillus nidulans in autosomal dominant hyper-Ige syndrome child. Chest 157(6):A33
Bastos RW, Valero C, Silva LP, Schoen T, Drott M, Brauer V, Silva-Rocha R, Lind A, Steenwyk JL, Rokas A, Rodrigues F, Resendiz-Sharpe A, Lagrou K, Marcet-Houben M, Gabaldon T, McDonnell E, Reid I, Tsang A, Oakley BR, Loures FV, Almeida F, Huttenlocher A, Keller NP, Ries LNA, Goldman GH (2020) Functional characterization of clinical isolates of the opportunistic fungal pathogen Aspergillus nidulans. mSphere 5(2):e00153-00120
Funding
This work was founded by the Chinese Academy of Medical Sciences (CAMS) Innovation Fund for Medical Sciences (CIFMS 2021-I2M-1-048).
Author information
Authors and Affiliations
Contributions
BC and BL contributed to the study conception and design. Material preparation, data collection, and analysis were performed by JZ, XZ, and DP. The first draft of the manuscript was written by JZ. JZ, XZ, BL, and BC commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval
The study was performed in line with the principles of the Ethics Committee of China-Japan Friendship Hospital (2022-KY-052).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhao, J., Zhuo, X., Pu, D. et al. Comparison of influenza- and COVID-19-associated pulmonary aspergillosis in China. Eur J Clin Microbiol Infect Dis 43, 683–692 (2024). https://doi.org/10.1007/s10096-024-04772-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-024-04772-4