Abstract
Objective
Periarticular osteophyte formation is observed during the repair of damaged joints in rheumatoid arthritis (RA); however, little is known about its clinical and functional roles. This study aimed to determine the influence of periarticular osteophyte formation on the incidence of total knee arthroplasty (TKA) (a surrogate for long-term outcomes of joint destruction) in patients with RA.
Methods
This retrospective longitudinal study included a total of 130 symptomatic (tender and/or swollen) knee joints in 80 patients starting biologics. Cumulative incidences of TKA were compared according to the presence or absence of osteophyte on plain anteroposterior radiograph (osteophyte (±)) and the extent of advanced joint damage as defined by Larsen’s grading system (0–II vs. III–V).
Results
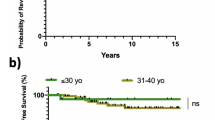
Kaplan-Meier estimates showed a significantly lower cumulative incidence of TKA for the osteophyte (+) group (n = 33) compared with the osteophyte (−) group (n = 31) in the Larsen grades III–V group (38 vs. 74% at 10 years, P = 0.010), whereas no significant difference was observed between the osteophyte (+) (n = 11) and osteophyte (−) (n = 55) groups in the Larsen grades 0–II group (9 vs. 10% at 10 years). Multivariate Cox proportional hazards analysis revealed that older age (hazard ratio (HR), 1.04 per 1 year; 95% confidence interval (CI), 1.01–1.08) and osteophyte formation (HR, 0.39; 95% CI, 0.19–0.79) independently predicted TKA in the Larsen grades III–V group, whereas none of the assessed variables predicted TKA in the Larsen grades 0–II group.
Conclusion
Osteophyte formation reduces the incidence of TKA in patients with RA who have advanced joint damage.
Key Points • Older age and Larsen grade were independent predictors of total knee arthroplasty (TKA) in rheumatoid arthritis (RA) patients. • Periarticular osteophyte formation reduced the incidence of TKA in RA patients with Larsen grades III–V. |



Similar content being viewed by others
References
Harris ED (1990) Rheumatoid arthritis. Pathophysiology and implications for therapy. N Engl J Med 322:1277–1289
Rau R (2006) Is remission in rheumatoid arthritis associated with radiographic healing? Clin Exp Rheumatol 24:S-41–S-44
Cabral AR, Loya BL, Alarcón-Segovia D (1989) Bone remodeling and osteophyte formation after remission of rheumatoid arthritis. J Rheumatol 16:1421–1427
Aschenberg S, Finzel S, Schmidt S, Kraus S, Engelke K, Englbrecht M, Rech J, Schett G (2013) Catabolic and anabolic periarticular bone changes in patients with rheumatoid arthritis: a computed tomography study on the role of age, disease duration and bone markers. Arthritis Res Ther 15:R62
Figueiredo CP, Simon D, Englbrecht M, Haschka J, Kleyer A, Bayat S, Hueber A, Pereira RM, Rech J, Schett G (2016) Quantification and impact of secondary osteoarthritis in patients with anti-citrullinated protein antibody-positive rheumatoid arthritis. Arthritis Rheumatol 68:2114–2121
Kaneko A, Matsushita I, Kanbe K, Arai K, Kuga Y, Abe A, Matsumoto T, Nakagawa N, Nishida K (2013) Development and validation of a new radiographic scoring system to evaluate bone and cartilage destruction and healing of large joints with rheumatoid arthritis: ARASHI (assessment of rheumatoid arthritis by scoring of large joint destruction and healing in radiographic imaging) study. Mod Rheumatol 23:1053–1062
Wolfe F, Zwillich SH (1998) The long-term outcomes of rheumatoid arthritis: a 23-year prospective, longitudinal study of total joint replacement and its predictors in 1,600 patients with rheumatoid arthritis. Arthritis Rheum 41:1072–1082
James D, Young A, Kulinskaya E, Knight E, Thompson W, Ollier W, Dixey J, Early Rheumatoid Arthritis Study Group (ERAS) UK (2004) Orthopaedic intervention in early rheumatoid arthritis. Occurrence and predictive factors in an inception cohort of 1064 patients followed for 5 years. Rheumatology (Oxford) 43:369–376
Kapetanovic MC, Lindqvist E, Saxne T, Eberhardt K (2008) Orthopaedic surgery in patients with rheumatoid arthritis over 20 years: prevalence and predictive factors of large joint replacement. Ann Rheum Dis 67:1412–1416
Asai S, Takahashi N, Asai N, Yamashita S, Terabe K, Matsumoto T, Sobue Y, Nishiume T, Suzuki M, Ishiguro N, Kojima T (2019) Characteristics of patients with rheumatoid arthritis undergoing primary total joint replacement: a 14-year trend analysis (2004-2017). Mod Rheumatol:1–7. https://doi.org/10.1080/14397595.2019.1649111
Imagama T, Tanaka H, Tokushige A, Seki K, Sumiura S, Yamamoto M, Nagahiro Y, Taguchi T (2013) Knee joint destruction driven by residual local symptoms after anti-tumor necrosis factor therapy in rheumatoid arthritis. Clin Rheumatol 32:823–828
Aletaha D, Smolen JS (2011) Joint damage in rheumatoid arthritis progresses in remission according to the disease activity score in 28 joints and is driven by residual swollen joints. Arthritis Rheum 63:3702–3711
Kojima T, Kaneko A, Hirano Y, Ishikawa H, Miyake H, Oguchi T, Takagi H, Yabe Y, Kato T, Ito T, Terabe K, Fukaya N, Kanayama Y, Shioura T, Funahashi K, Hayashi M, Kato D, Matsubara H, Fujibayashi T, Kojima M, Ishiguro N, TBC (2012) Study protocol of a multicenter registry of patients with rheumatoid arthritis starting biologic therapy in Japan: Tsurumai Biologics Communication Registry (TBCR) study. Mod Rheumatol 22:339–345
Arnett FC, Edworthy SM, Bloch DA, McShane DJ, Fries JF, Cooper NS, Healey LA, Kaplan SR, Liang MH, Luthra HS (1988) The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum 31:315–324
Larsen A, Dale K, Eek M (1977) Radiographic evaluation of rheumatoid arthritis and related conditions by standard reference films. Acta Radiol Diagn (Stockh) 18:481–491
Guth A, Coste J, Chagnon S, Lacombe P, Paolaggi JB (1995) Reliability of three methods of radiologic assessment in patients with rheumatoid arthritis. Investig Radiol 30:181–185
Altman RD, Gold GE (2007) Atlas of individual radiographic features in osteoarthritis, revised. Osteoarthritis Cartilage 15(Suppl A):A1–A56
Asai S, Takahashi N, Funahashi K, Yoshioka Y, Takemoto T, Terabe K, Asai N, Ishiguro N, Kojima T (2015) Concomitant methotrexate protects against total knee arthroplasty in patients with rheumatoid arthritis treated with tumor necrosis factor inhibitors. J Rheumatol 42:2255–2260
Seki E, Matsushita I, Sugiyama E, Taki H, Shinoda K, Hounoki H, Motomura H, Kimura T (2009) Radiographic progression in weight-bearing joints of patients with rheumatoid arthritis after TNF-blocking therapies. Clin Rheumatol 28:453–460
Nakajima A, Terayama K, Sonobe M, Aoki Y, Takahashi H, Akatsu Y, Taniguchi S, Yamada M, Kubota A, Nakagawa K (2019) Predictive factors for radiographic progression of large joint damage in patients with rheumatoid arthritis treated with biological disease-modifying antirheumatic drugs (bDMARDs): results of 3 to 4 years of follow-up. Mod Rheumatol 29:903–909
van der Kraan PM, van den Berg WB (2007) Osteophytes: relevance and biology. Osteoarthr Cartil 15:237–244
Altman R, Asch E, Bloch D, Bole G, Borenstein D, Brandt K, Christy W, Cooke TD, Greenwald R, Hochberg M (1986) Development of criteria for the classification and reporting of osteoarthritis. Classification of osteoarthritis of the knee. Diagnostic and Therapeutic Criteria Committee of the American Rheumatism Association. Arthritis Rheum 29:1039–1049
Kinds MB, Marijnissen AC, Vincken KL, Viergever MA, Drossaers-Bakker KW, Bijlsma JW, Bierma-Zeinstra SM, Welsing PM, Lafeber FP (2012) Evaluation of separate quantitative radiographic features adds to the prediction of incident radiographic osteoarthritis in individuals with recent onset of knee pain: 5-year follow-up in the CHECK cohort. Osteoarthr Cartil 20:548–556
Katsuragi J, Sasho T, Yamaguchi S, Sato Y, Watanabe A, Akagi R, Muramatsu Y, Mukoyama S, Akatsu Y, Fukawa T, Endo J, Hoshi H, Yamamoto Y, Sasaki T, Takahashi K (2015) Hidden osteophyte formation on plain X-ray is the predictive factor for development of knee osteoarthritis after 48 months--data from the osteoarthritis initiative. Osteoarthr Cartil 23:383–390
Liu L, Ishijima M, Kaneko H, Sadatsuki R, Hada S, Kinoshita M, Aoki T, Futami I, Yusup A, Arita H, Shiozawa J, Takazawa Y, Ikeda H, Kaneko K (2017) The MRI-detected osteophyte score is a predictor for undergoing joint replacement in patients with end-stage knee osteoarthritis. Mod Rheumatol 27:332–338
Monsees B, Destouet JM, Murphy WA, Resnick D (1985) Pressure erosions of bone in rheumatoid arthritis: a subject review. Radiology 155:53–59
Nell VP, Machold KP, Stamm TA, Eberl G, Heinzl H, Uffmann M, Smolen JS, Steiner G (2005) Autoantibody profiling as early diagnostic and prognostic tool for rheumatoid arthritis. Ann Rheum Dis 64:1731–1736
Smolen JS, Van Der Heijde DM, St Clair EW, Emery P, Bathon JM, Keystone E, Maini RN, Kalden JR, Schiff M, Baker D, Han C, Han J, Bala M, Group A-CSoPRIftToRAoEOAS (2006) Predictors of joint damage in patients with early rheumatoid arthritis treated with high-dose methotrexate with or without concomitant infliximab: results from the ASPIRE trial. Arthritis Rheum 54:702–710
Courvoisier N, Dougados M, Cantagrel A, Goupille P, Meyer O, Sibilia J, Daures JP, Combe B (2008) Prognostic factors of 10-year radiographic outcome in early rheumatoid arthritis: a prospective study. Arthritis Res Ther 10:R106
Vastesaeger N, Xu S, Aletaha D, St Clair EW, Smolen JS (2009) A pilot risk model for the prediction of rapid radiographic progression in rheumatoid arthritis. Rheumatology (Oxford) 48:1114–1121
Kuper HH, van Leeuwen MA, van Riel PL, Prevoo ML, Houtman PM, Lolkema WF, van Rijswijk MH (1997) Radiographic damage in large joints in early rheumatoid arthritis: relationship with radiographic damage in hands and feet, disease activity, and physical disability. Br J Rheumatol 36:855–860
Drossaers-Bakker KW, Kroon HM, Zwinderman AH, Breedveld FC, Hazes JM (2000) Radiographic damage of large joints in long-term rheumatoid arthritis and its relation to function. Rheumatology (Oxford) 39:998–1003
Smolen JS, Landewé R, Bijlsma J, Burmester G, Chatzidionysiou K, Dougados M, Nam J, Ramiro S, Voshaar M, van Vollenhoven R, Aletaha D, Aringer M, Boers M, Buckley CD, Buttgereit F, Bykerk V, Cardiel M, Combe B, Cutolo M, van Eijk-Hustings Y, Emery P, Finckh A, Gabay C, Gomez-Reino J, Gossec L, Gottenberg JE, Hazes JMW, Huizinga T, Jani M, Karateev D, Kouloumas M, Kvien T, Li Z, Mariette X, McInnes I, Mysler E, Nash P, Pavelka K, Poór G, Richez C, van Riel P, Rubbert-Roth A, Saag K, da Silva J, Stamm T, Takeuchi T, Westhovens R, de Wit M, van der Heijde D (2017) EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs: 2016 update. Ann Rheum Dis 76:960–977
Singh JA, Saag KG, Bridges SL, Akl EA, Bannuru RR, Sullivan MC, Vaysbrot E, McNaughton C, Osani M, Shmerling RH, Curtis JR, Furst DE, Parks D, Kavanaugh A, O’Dell J, King C, Leong A, Matteson EL, Schousboe JT, Drevlow B, Ginsberg S, Grober J, St Clair EW, Tindall E, Miller AS, McAlindon T (2016) 2015 American College of Rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol 68:1–26
Leon L, Abasolo L, Carmona L, Rodriguez-Rodriguez L, Lamas JR, Hernandez-Garcia C, Jover JA, Group eS (2013) Orthopedic surgery in rheumatoid arthritis in the era of biologic therapy. J Rheumatol 40:1850–1855
Hassett G, Hart DJ, Doyle DV, March L, Spector TD (2006) The relation between progressive osteoarthritis of the knee and long term progression of osteoarthritis of the hand, hip, and lumbar spine. Ann Rheum Dis 65:623–628
Nakada I, Nakamura I, Juji T, Ito K, Matsumoto T (2015) Correlation between knee and hindfoot alignment in patients with rheumatoid arthritis: the effects of subtalar joint destruction. Mod Rheumatol 25:689–693
Eckstein F, Kwoh CK, Boudreau RM, Wang Z, Hannon MJ, Cotofana S, Hudelmaier MI, Wirth W, Guermazi A, Nevitt MC, John MR, Hunter DJ, Investigators O (2013) Quantitative MRI measures of cartilage predict knee replacement: a case-control study from the osteoarthritis initiative. Ann Rheum Dis 72:707–714
Jämsen E, Huhtala H, Puolakka T, Moilanen T (2009) Risk factors for infection after knee arthroplasty. A register-based analysis of 43,149 cases. J Bone Joint Surg Am 91:38–47
Himanen AK, Belt EA, Lehto MU, Hämäläinen MM (2007) A comparison of survival of moulded monoblock and modular tibial components of 751 AGC total knee replacements in the treatment of rheumatoid arthritis. J Bone Joint Surg Br 89:609–614
Availability of data and materials
The datasets generated during and/or analyzed in the current study are available from the corresponding author on reasonable request.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
SA designed the study, conducted statistical analyses, and drafted the manuscript. All authors contributed to interpretation of data, manuscript preparation, and manuscript review; approved the draft for publication; and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
SA has received speakers’ fees from AbbVie, Astellas, Bristol-Myers Squibb, Chugai, Daiichi-Sankyo, Eisai, Janssen, Takeda, and UCB Japan. NT has received speakers’ fees from AbbVie, Asahi Kasei, Astellas, Bristol-Myers Squibb, Chugai, Daiichi-Sankyo, Eisai, Eli Lilly, Janssen, Mitsubishi Tanabe, Ono, Pfizer, Takeda, and UCB Japan. YS has received speakers’ fees from Astellas, Bristol-Myers Squibb, and Ono. MS has received speakers’ fees from Bristol-Myers Squibb. NI has received grant/research support, consulting fees, and/or speakers’ fees from AbbVie, Asahi Kasei, Astellas, Bristol-Myers Squibb, Chugai, Daiichi-Sankyo, Eisai, Eli Lilly, Kaken, Mitsubishi Tanabe, Ono, Otsuka, Pfizer, Taisho Toyama, Takeda, and Zimmer Biomet. TK has received grant/research support and/or speakers’ fees from AbbVie, Astellas, Bristol-Myers Squibb, Chugai, Daiichi-Sankyo, Eli Lilly, Janssen, Mitsubishi Tanabe, Novartis, Pfizer, and Takeda. The other authors declare no conflicts of interest.
Ethics approval
This study was approved by the Ethics Committee of Nagoya University Graduate School of Medicine (2019-0230) and complied with the principles set forth in the Declaration of Helsinki.
Consent to participate and for publication
Informed consent was obtained by an opt-out procedure.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Asai, S., Takahashi, N., Terabe, K. et al. Periarticular osteophyte formation protects against total knee arthroplasty in rheumatoid arthritis patients with advanced joint damage. Clin Rheumatol 39, 3331–3339 (2020). https://doi.org/10.1007/s10067-020-05140-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05140-1