Abstract
Purpose
Reports of mesh infections following open tension-free inguinal hernioplasty are gradually increasing. Recent research has focused on identifying and managing mesh infections. However, studies examining the long-term outcomes and quality of life following mesh removal for late-onset infections are few. This study aimed to analyze the short and long-term outcomes after maximal removal of the implanted mesh in patients with late-onset mesh infection after open tension-free inguinal hernioplasty.
Methods
Data of 105 patients who developed late-onset mesh infection after open tension-free inguinal hernioplasty and were admitted to our hospital from January 2014 to January 2019 were retrospectively analyzed. Patients were followed up by telephone or outpatient consultation for 3 years, focusing on hernia recurrence and mesh infection recurrence. Quality of life was assessed preoperatively and postoperatively using our developed scale; postoperative inguinal area pain was assessed using the visual analog score, and postoperative anxiety was assessed using the anxiety self-assessment scale.
Results
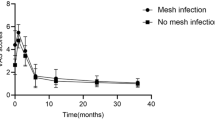
Of the 105 patients who experienced late-onset mesh infection following open inguinal hernioplasty, 100 underwent mesh plug repair. The mean follow-up time was 58 months, and 10.5% (95/105) of the patients were lost to follow-up. Recurrence of infection was observed in 28.6% of patients (2/7) who underwent partial mesh removal and in 3.4% of patients (3/88) who underwent complete mesh removal. One inguinal hernia recurred 12 months after mesh removal (1.0% recurrence rate). In the third year following surgery as compared to the preoperative period, there were significant improvements in quality of life.
Conclusions
Hernia plugs may not be a good choice in tension-free inguinal hernia repair in view of the risk of late infections and fistulas. Remove all mesh at the time of the first operation for mesh infection. Hernia recurrence after late-onset infected mesh removal following open inguinal tension-free hernioplasty is rare. The post-operative quality of life, pain, and anxiety are gradually steadily improving.



Similar content being viewed by others
References
Lichtenstein IL et al (1989) The tension-free hernioplasty. Am J Surg 157(2):188–193
Delikoukos S et al (2007) Late-onset deep mesh infection after inguinal hernia repair. Hernia 11(1):15–17
Pérez-Köhler B, Bayon Y, Bellón JM (2016) Mesh infection and hernia repair: a review. Surg Infect 17(2):124–137
Rehman S et al (2012) Recurrence of inguinal herniae following removal of infected prosthetic meshes: a review of the literature. Hernia 16(2):123–126
Kao AM et al (2018) Prevention and treatment strategies for mesh infection in abdominal wall reconstruction. Plast Reconstr Surg 142:149S-155S
Levy S et al (2018) Comparison of complete versus partial mesh removal for the treatment of chronic mesh infection after abdominal wall hernia repair. Hernia 22(5):773–779
Mann DV et al (1998) Late-onset deep prosthetic infection following mesh repair of inguinal hernia. Am J Surg 176(1):12–14
Kong W et al (2015) Early-versus late-onset prosthetic mesh infection: more than time alone. Indian J Surg 77(Suppl 3):1154–1158
Hays RD, Sherbourne CD, Mazel RM (1993) The RAND 36-item health survey 1.0. Health Econ 2(3):217–227
Skevington SM et al (2021) Enhancing the multi-dimensional assessment of quality of life: introducing the WHOQOL-Combi. Qual Life Res 30(3):891–903
Thompson AJ, Turner AJ (2020) A comparison of the EQ-5D-3L and EQ-5D-5L. Pharmacoeconomics 38(6):575–591
HerniaSurge Group (2018) International guidelines for groin hernia management. Hernia 22(1):1–165
McCarthy MJ et al (2005) Visual analog scales for assessing surgical pain. J Am Coll Surg 201(2):245–252
Zung WW (1965) A self-rating depression scale. Arch Gen Psychiatry 12:63–70
Tamura T, Ohata Y, Katsumoto F (2019) Mesh removal and reconstruction with posterior components separation technique for delayed mesh infection developed 10 years after abdominal incisional hernia repair: a rare case report. Surg Case Rep 5(1):140
Fawole AS, Chaparala RP, Ambrose NS (2006) Fate of the inguinal hernia following removal of infected prosthetic mesh. Hernia 10(1):58–61
Jin C, Shen Y, Chen J (2020) Laparoscopic evaluation and management of 47 patients with late-onset mesh infection after inguinal hernioplasty. Hernia 24(2):381–385
Klinge U, Klosterhalfen B (2012) Modified classification of surgical meshes for hernia repair based on the analyses of 1,000 explanted meshes. Hernia 16(3):251–258
Agrawal A, Avill R (2006) Mesh migration following repair of inguinal hernia: a case report and review of literature. Hernia 10(1):79–82
Amid PK (2003) The Lichtenstein repair in 2002: an overview of causes of recurrence after Lichtenstein tension-free hernioplasty. Hernia 7(1):13–16
Brown C, O’Hare R, Stephenson BM (2022) Avoiding migration at open mesh plug inguinal hernioplasty. Heliyon 8(5):e09320
D’Amore L et al (2012) Mesh plug repair: can we reduce the risk of plug erosion into the sigmoid colon? Hernia 16(4):495–496
Li J, Cheng T (2019) Mesh erosion into urinary bladder, rare condition but important to know. Hernia 23(4):709–716
Trabucco EE (1993) The office hernioplasty and the Trabucco repair. Ann Ital Chir 64(2):127–149
Robbins AW, Rutkow IM (1993) The mesh-plug hernioplasty. Surg Clin North Am 73(3):501–512
Bueno-Lledo J et al (2017) Partial versus complete removal of the infected mesh after abdominal wall hernia repair. Am J Surg 214(1):47–52
Gachabayov M et al (2020) Recurrence of infection and hernia following partial versus complete removal of infected hernia mesh: a systematic review and cohort meta-analysis. Hernia 24(3):433–439
Sabbagh C et al (2012) Partial removal of infected parietal meshes is a safe procedure. Hernia 16(4):445–449
Chung L, Tse GH, O’Dwyer PJ (2014) Outcome of patients with chronic mesh infection following abdominal wall hernia repair. Hernia 18(5):701–704
Yang H et al (2020) Study of mesh infection management following inguinal hernioplasty with an analysis of risk factors: a 10-year experience. Hernia 24(2):301–305
Arnaud JP et al (1977) Critical evaluation of prosthetic materials in repair of abdominal wall hernias: new criteria of tolerance and resistance. Am J Surg 133(3):338–345
Akyol C et al (2013) Outcome of the patients with chronic mesh infection following open inguinal hernia repair. J Korean Surg Soc 84(5):287
Sanders DL et al (2014) Randomized clinical trial comparing self-gripping mesh with suture fixation of lightweight polypropylene mesh in open inguinal hernia repair. Br J Surg 101(11):1373–1382
Funding
None.
Author information
Authors and Affiliations
Contributions
ZZ and HC: conceived the study and drafted the manuscript. WH and CD: identified and screened clinical data of patients eligible for late-onset mesh infection. ZZ and HC: extracted data independently and consulted with WH when controversial issues were raised. XL: revised and directed the study. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Ethical approval was agreed by the ethical committee of the institution.
Human and animal rights
The study including human participants has been performed in accordance with the ethical standards of the Declaration of Helsinki and its later amendments.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhi, Z., Cui, H., Han, W. et al. What is the outcome of late-onset infected mesh removal after open tension-free inguinal hernioplasty: 3-year follow-up. Hernia 27, 935–942 (2023). https://doi.org/10.1007/s10029-022-02684-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-022-02684-w