Abstract
Purpose
The purpose of this study is to compare the opioid requirement and pain intensity after surgeries of mandibular fractures with administration of dexmedetomidine by two approaches of infusion and single bolus.
Methods
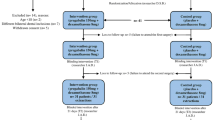
In this double-blind clinical trial, the participants were randomized and matched in terms of age and gender in two groups (infusion and bolus). In both groups, the amount of narcotic used, hemodynamic indices, oxygen saturation, and pain intensity were collected based on the ten-point Visual Analogue Scale (VAS) at 7 time points for 24 h. SPSS version 24 software was used for data analysis. A significance level of less than 5% was considered.
Results
A total of 40 patients were included in the study. There was no significant difference between the two groups in terms of gender, age, ASA class, and duration of surgery (P>0.05). There was no significant difference between the two groups in terms of nausea and vomiting and subsequently receiving anti-nausea medication (P>0.05). The need for opioid consumption after surgery was not different in two groups (P>0.05). Infusion of dexmedetomidine reduced postoperative pain more rapidly than its single bolus dose (P<0.05). However, over time, there was no significant difference between the two groups in terms of changes in oxygen saturation variables (P>0.05). Homodynamic indices including heart rate, systolic blood pressure, and diastolic blood pressure in the bolus group were significantly lower than the infusion group (P<0.05).
Conclusion
Administration of dexmedetomidine in the form of infusion can reduce postoperative pain better than bolus injection, with less probability of hypotension and bradycardia.





Similar content being viewed by others
Data availability
Data available on request from the authors
References
Small C, Laycock H (2020) Acute postoperative pain management. Br J Surg 107(2):e70–e80
Yang MM, Hartley RL, Leung AA, Ronksley PE, Jetté N, Casha S et al (2019) Preoperative predictors of poor acute postoperative pain control: a systematic review and meta-analysis. BMJ open 9(4):e025091
Imani F, Zaman B, De Negri P (2020) Postoperative pain management: role of dexmedetomidine as an adjuvant. Anesth Pain Med 10(6)
Kehlet H (2018) Postoperative pain, analgesia, and recovery—bedfellows that cannot be ignored. Pain 159:S11–SS6
Li J, Yang J-S, Dong B-H, Ye J-M (2019) The effect of dexmedetomidine added to preemptive ropivacaine infiltration on postoperative pain after lumbar fusion surgery: a randomized controlled trial. Spine 44(19):1333–1338
Santos BF, Costa FO, Vasconcelos AM, Cyrino RM, Cota LO (2022) Preemptive effects of ibuprofen and nimesulide on postoperative pain control after open flap periodontal surgeries: a randomized placebo-controlled split-mouth clinical trial. J Periodontol 93(2):300–309
Pereira G-M, Costa F-O (2020) Effect of preemptive analgesia with ibuprofen in the control of postoperative pain in dental implant surgeries: a randomized, triple-blind controlled clinical trial. J Clin Exp Dent 12(1):e71
Hassan B, Al-Khanati NM, Bahhah H (2020) Effect of lingual-based flap design on postoperative pain of impacted mandibular third molar surgery: Split-mouth randomized clinical trial. Med Oral Patol Oral Cir Bucal 25(5):e660
Nejat AH, Eshghpour M, Danaeifar N, Abrishami M, Vahdatinia F, Fekrazad R (2021) Effect of photobiomodulation on the incidence of alveolar osteitis and postoperative pain following mandibular third molar surgery: a double-blind randomized clinical trial. Photochem Photobiol 97(5):1129–1135
Ali HT, Mosleh MI, Shawky M (2018) Variables predictive of the intensity of postoperative pain following mandibular third molar surgery: a prospective study. Minerva Stomatol 67(3):111–116
Lee S (2019) Dexmedetomidine: present and future directions. Korean J Anesthesiol 72(4):323–330
Yuan D, Liu Z, Kaindl J, Maeda S, Zhao J, Sun X et al (2020) Activation of the α2B adrenoceptor by the sedative sympatholytic dexmedetomidine. Nat Chem Biol 16(5):507–512
Alizargar J, Etemadi M, Kaviani N, Wu SFV, Jafarzadeh K, Ranjbarian P, Hsieh NC (2021) Injection of lidocaine alone versus lidocaine plus dexmedetomidine in impacted third molar extraction surgery, a double-blind randomized control trial for postoperative pain evaluation. Pain Res Manag
Phillips BT, Wang ED, Rodman AJ, Watterson PA, Smith KL, Finical SJ et al (2012) Anesthesia duration as a marker for surgical complications in office-based plastic surgery. Ann Plast Surg 69(4):408–411
Loeffelbein DJ, Julinek A, Wolff K-D, Kochs E, Haller B, Haseneder R (2016) Perioperative risk factors for postoperative pulmonary complications after major oral and maxillofacial surgery with microvascular reconstruction: a retrospective analysis of 648 cases. Journal of Cranio-Maxillofacial Surgery 44(8):952–957
Davoudi A, Movahedian Attar B, Shadmehr E (2017) Risks and benefits of pre-operative dexmedetomidine in oral and maxillofacial surgeries: a systematic review. Expert Opin Drug Saf 16(6):711–720
Giovannitti JA Jr, Thoms SM, Crawford JJ (2015) Alpha-2 adrenergic receptor agonists: a review of current clinical applications. Anesth Prog 62(1):31–38
Gu X, Tan X, Chen J, Wang J, Lu Y, Zhang L (2020) The clinical effect of dexmedetomidine combined with parecoxib sodium on sedation, antianxiety and prevention of intubation stress in patients undergoing functional endoscopic sinus surgery: a randomised controlled trial. BMC anesthesiol 20(1):1–8
Mishra N, Birmiwal KG, Pani N, Raut S, Sharma G, Rath KC (2016) Sedation in oral and maxillofacial day care surgery: a comparative study between intravenous dexmedetomidine and midazolam. Natl J Maxillofac Surg 7(2):178
Yamane A, Higuchi H, Tomoyasu Y, Ishii-Maruhama M, Maeda S, Miyawaki T (2015) Effect of dexmedetomidine injected into the oral mucosa in combination with lidocaine on local anesthetic potency in humans: a crossover double-blind study. J Oral Maxillofac Surg 73(4):616–621
Ge D-J, Qi B, Tang G, Li J-Y (2016) Intraoperative dexmedetomidine promotes postoperative analgesia and recovery in patients after abdominal hysterectomy: a double-blind, randomized clinical trial. Sci Rep 6(1):1–7
Choi JJ, Kim K, Park HY, Chang YJ, Lee KC, Kim KY et al (2021) CONSORT the effect of a bolus dose of dexmedetomidine on postoperative pain, agitation, and quality of recovery after laparoscopic cholecystectomy. Medicine 100(3)
Bielka K, Kuchyn I, Babych V, Martycshenko K, Inozemtsev O (2018) Dexmedetomidine infusion as an analgesic adjuvant during laparoscopic сholecystectomy: a randomized controlled study. BMC Anesthesiol 18(1):1–6
Khare A, Sharma SP, Deganwa ML, Sharma M, Gill N (2017) Effects of dexmedetomidine on intraoperative hemodynamics and propofol requirement in patients undergoing laparoscopic cholecystectomy. Anesth Essays Res 11(4):1040
Peng K, Jin X-h, Liu S-l, Ji F-h (2015) Effect of intraoperative dexmedetomidine on post-craniotomy pain. Clin Ther 37(5):1114–1121 e1
Song J, Ji Q, Sun Q, Gao T, Liu K, Li L (2016) The opioid-sparing effect of intraoperative dexmedetomidine infusion after craniotomy. J Neurosurg Anesthesiol 28(1):14–20
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation was performed by Saeed Nezafati, Loghman Ebrahimi, and Abbas Ali Dehghani. Data collection and analysis were done by Reza Khorshidi Khiavi, Ali Mortazavi, and Saeed Nezafati. Loghman Ebrahimi wrote the first draft of the manuscript, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This research has been approved by the ethics committee of Tabriz University of Medical Sciences (IR.TBZMED.REC.1401.308).
Consent to participate
Informed consent to participate in the study was obtained from all patients before the procedures.
Consent for publication
All the authors of this manuscript declare their consent for publication in “Oral and Maxillofacial Surgery.”
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nezafati, S., Dehghani, A.A., Khiavi, R.K. et al. Opioid requirement and pain intensity after mandibular surgeries with dexmedetomidine administration in two ways: intraoperative infusion versus bolus injection. Oral Maxillofac Surg (2023). https://doi.org/10.1007/s10006-023-01169-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10006-023-01169-z