Abstract
Objectives
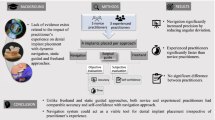
To assess the accuracy of dynamic computer–aided implant surgery (dCAIS) systems when used to place dental implants and to compare its accuracy with static computer–aided implant surgery (sCAIS) systems and freehand implant placement.
Materials and Methods
An electronic search was made to identify all relevant studies reporting on the accuracy of dCAIS systems for dental implant placement. The following PICO question was developed: “In patients or artificial models, is dental implant placement accuracy higher when dCAIS systems are used in comparison with sCAIS systems or with freehand placement? The main outcome variable was angular deviation between the central axes of the planned and final position of the implant. The data were extracted in descriptive tables, and a meta-analysis of single means was performed in order to estimate the deviations for each variable using a random-effects model.
Results
Out of 904 potential articles, the 24 selected assessed 9 different dynamic navigation systems. The mean angular and entry 3D global deviations for clinical studies were 3.68° (95% CI: 3.61 to 3.74; I2 = 99.4%) and 1.03 mm (95% CI: 1.01 to 1.04; I2 = 82.4%), respectively. Lower deviation values were reported in in vitro studies (mean angular deviation of 2.01° (95% CI: 1.95 to 2.07; I2 = 99.1%) and mean entry 3D global deviation of 0.46 mm (95% CI: 0.44 to 0.48 ; I2 = 98.5%). No significant differences were found between the different dCAIS systems. These systems were significantly more accurate than sCAIS systems (mean difference (MD): −0.86°; 95% CI: −1.35 to −0.36) and freehand implant placement (MD: −4.33°; 95% CI: −5.40 to −3.25).
Conclusion
dCAIS systems allow highly accurate implant placement with a mean angular of less than 4°. However, a 2-mm safety margin should be applied, since deviations of more than 1 mm were observed. dCAIS systems increase the implant placement accuracy when compared with freehand implant placement and also seem to slightly decrease the angular deviation in comparison with sCAIS systems.
Clinical Relevance
The use of dCAIS could reduce the rate of complications since it allows a highly accurate implant placement.








Similar content being viewed by others
References
Moraschini V, Poubel LADC, Ferreira VF, Barboza EDSP (2015) Evaluation of survival and success rates of dental implants reported in longitudinal studies with a follow-up period of at least 10 years: a systematic review. Int J Oral Maxillofac Surg 44:377–388. https://doi.org/10.1016/j.ijom.2014.10.023
Chrcanovic BR, Albrektsson T, Wennerberg A (2014) Reasons for failures of oral implants. J Oral Rehabil 41:443–476. https://doi.org/10.1111/joor.12157
Romanos GE, Delgado-Ruiz R, Sculean A (2019) Concepts for prevention of complications in implant therapy. Periodontol 81:7–17. https://doi.org/10.1111/prd.12278
Greenstein G, Cavallaro J, Romanos G, Tarnow D (2008) Clinical recommendations for avoiding and managing surgical complications associated with implant dentistry: a review. J Periodontol 79:1317–1329. https://doi.org/10.1080/17453674.2019.1690339
Hämmerle CHF, Tarnow D (2018) The etiology of hard- and soft-tissue deficiencies at dental implants: A narrative review. J Periodontol 89:291–303. https://doi.org/10.1002/JPER.16-0810
Martin W, Pollini A, Morton D (2014) The influence of restorative procedures on esthetic outcomes in implant dentistry: a systematic review. Int J Oral Maxillofac Implants 29:142–154. https://doi.org/10.11607/jomi.2014suppl.g3.1.
Buser D, Martin W, Belser UC (2004) Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants 19:43–46
Clark D, Barbu H, Lorean A, Mijiritsky E, Levin L (2017) Incidental findings of implant complications on postimplantation CBCTs: a cross-sectional study. Clin Implant Dent Relat Res 19:776–782. https://doi.org/10.1111/cid.12511
Gaêta-Araujo H, Oliveira-Santos N, Mancini AXM, Oliveira ML, Oliveira-Santos C (2020) Retrospective assessment of dental implant-related perforations of relevant anatomical structures and inadequate spacing between implants/teeth using cone-beam computed tomography. Clin Oral Investig 4:3281–3288. https://doi.org/10.1007/s00784-020-03205-8
Jacobs R, Salmon B, Codari M, Hassan B, Bornstein MM (2018) Cone beam computed tomography in implant dentistry: recommendations for clinical use. BMC Oral Health 18:1–16. https://doi.org/10.1186/s12903-018-0523-5
Benavides E, Rios HF, Ganz SD et al (2012) Use of cone beam computed tomography in implant dentistry: the International Congress of Oral Implantologists consensus report. Implant Dent 21:78–86. https://doi.org/10.1097/ID.0b013e31824885b5
Guerrero ME, Jacobs R, Loubele M, Schutyser F, Suetens P, van Steenberghe D (2006) State-of-the-art on cone beam CT imaging for preoperative planning of implant placement. Clin Oral Investig 10:1–7. https://doi.org/10.1007/s00784-005-0031-2
Hammerle CHF, Stone P, Jung RE, Kapos T, Brodala N (2009) Consensus statements and recommended clinical procedures regarding computer-assisted implant dentistry. Int J Oral Maxillofac Implants 24:126–131
Jung RE, Schneider D, Ganeles J et al (2009) Computer technology applications in surgical implant dentistry: a systematic review. Int J Oral Maxillofac Implants 24:92–109
Vercruyssen M, Fortin T, Widmann G, Jacobs R, Quirynen M (2014) Different techniques of static/dynamic guided implant surgery: modalities and indications. Periodontol 66:214–227. https://doi.org/10.1111/prd.12056
Block MS, Emery RW (2016) Static or dynamic navigation for implant placement-choosing the method of guidance. J Oral Maxillofac Surg 74:269–277. https://doi.org/10.1016/j.joms.2015.09.022
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:332–336. https://doi.org/10.1136/bmj.b2535
Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ WV. (2019) Cochrane handbook for systematic reviews of interventions version 6.0 (updated July 2019).
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P (2011) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses.
Higgins JPT, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558
Kang S-H, Lee J-W, Lim S-H, Kim Y-H, Kim M-K (2014) Verification of the usability of a navigation method in dental implant surgery: in vitro comparison with the stereolithographic surgical guide template method. J Craniomaxillofac Surg 42(7):1530–1535. https://doi.org/10.1016/j.jcms.2014.04.025
Jokstad A, Winnett B, Fava J, Powell D, Somogyi-Ganss E (2018) Investigational clinical trial of a prototype optoelectronic computer-aided navigation device for dental implant surgery. Int J Oral Maxillofac Implants 33:679–692. https://doi.org/10.11607/jomi.6351
Chen Y-T, Chiu Y-W, Peng C-Y (2020) Preservation of inferior alveolar nerve using the dynamic dental implant navigation system. J Oral Maxillofac Surg 78:678–679. https://doi.org/10.1016/j.joms.2020.01.007
Panchal N, Mahmood L, Retana A, Emery R (2019) Dynamic navigation for dental implant surgery. Oral Maxillofac Surg Clin North Am 31:539–547. https://doi.org/10.1016/j.coms.2019.08.001
Ruoppoli A, Beltrame C, Tonoli G, Amaroli A, de Angelis N (2019) Accuracy of guided implant surgery: an experimental set-up. Minerva Stomatol 68:61–66. https://doi.org/10.23736/S0026-4970.19.04223-7
Fang Y, An X, Jeong S-M, Choi B-H (2019) Accuracy of computer-guided implant placement in anterior regions. J Prosthet Dent 121:836–842. https://doi.org/10.1016/j.prosdent.2018.07.015
Lin Z, Gao Y (2018) Application and evaluation of real-time navigation system in dental implants surgery. Basic Clin Pharmacol Toxicol 124:32
Younes F, Cosyn J, De Bruyckere T, Cleymaet R, Bouckaert E, Eghbali A (2018) A randomized controlled study on the accuracy of free-handed, pilot-drill guided and fully guided implant surgery in partially edentulous patients. J Clin Periodontol 45:721–732. https://doi.org/10.1111/jcpe.12897
Cassetta M, Bellardini M (2017) How much does experience in guided implant surgery play a role in accuracy? A randomized controlled pilot study. Int J Oral Maxillofac Surg 46:922–930. https://doi.org/10.1016/j.ijom.2017.03.010
Block MS, Emery RW, Lank K, Ryan J (2017) Implant placement accuracy using dynamic navigation. Int J Oral Maxillofac Implants 32:92–99. https://doi.org/10.11607/jomi.5004
Horwitz J, Machtei EE, Zigdon-Giladi H (2017) Clinical accuracy of a novel open-lattice-frame implant positioning system: a case series. Quintessence Int 48:33–39. https://doi.org/10.3290/j.qi.a37134
Simon Z (2015) Computer-guided implant surgery: placing the perfect implant. J Calif Dent Assoc 43:126–129
Dreiseidler T, Neugebauer J, Ritter L et al (2009) Accuracy of a newly developed integrated system for dental implant planning. Clin Oral Implants Res 20:1191–1199. https://doi.org/10.1111/j.1600-0501.2009.01764.x
Orentlicher G, Horowitz A, Goldwaser B, Abboud M (2017) Ten myths of guided implant surgery. Compend Contin Educ Dent 38:552–557
Casap N, Laviv A, Wexler A (2011) Computerized navigation for immediate loading of dental implants with a prefabricated metal frame: a feasibility study. J Oral Maxillofac Surg 69:512–519. https://doi.org/10.1016/j.joms.2010.10.031
Casap N, Nadel S, Tarazi E, Weiss EI (2011) Evaluation of a navigation system for dental implantation as a tool to train novice dental practitioners. J Oral Maxillofac Surg 69:2548–2556. https://doi.org/10.1016/j.joms.2011.04.026
Ganeles J, Mandelaris GA, Rosenfeld AL, Rose LF (2011) Image guidance for implants improves accuracy and predictability. Compend Contin Educ Dent 32:52–55
Turkyilmaz I (2011) Implant dentistry - a rapidly evolving practice. InTech, London
Rossi R, Morales RS, Frascaria M, Benzi R, Squadrito N (2010) Planning implants in the esthetic zone using a new implant 3D navigation system. Eur J Esthet Dent 5:172–188
Scheyer ET, Mandelaris GA, McGuire MK, AlTakriti MA, Stefanelli LV (2020) Implant placement under dynamic navigation using trace registration: case presentations. Int J Periodontics Restorative Dent 40:e241–e248
Zhan Y, Wang M, ChengX LY, Shi X, Liu F (2020) Evaluation of a dynamic navigation system for training students in dental implant placement. J Dent Educ. In press. https://doi.org/10.1002/jdd.12399
Cecchetti F, Di Girolamo M, Mazza D, Ippolito G, Baggi L (2020) Computer-guided implant surgery: analysis of dynamic navigation systems and digital accuracy. J Biol Regul Homeost Agents 34:9–17
Stefanelli LV, DeGroot BS, Lipton DI, Mandelaris GA (2019) Accuracy of a dynamic dental implant navigation system in a private practice. Int J Oral Maxillofac Implants 34:205–213. https://doi.org/10.11607/jomi.6966
Stefanelli LV, Mandelaris GA, DeGroot BS, Gambarini G, De Angelis F, Di Carlo S (2020) Accuracy of a novel trace-registration method for dynamic navigation surgery. Int J Periodontics Restor Dent 40:427–435. https://doi.org/10.1111/clr.13563
Aydemir CA, Arisan V (2020) Accuracy of dental implant placement via dynamic navigation or the freehand method: a split-mouth randomized controlled clinical trial. Clin Oral Implants Res 31:255–263. https://doi.org/10.1111/clr.13563
Pellegrino G, Taraschi V, Andrea Z, Ferri A, Marchetti C (2019) Dynamic navigation: a prospective clinical trial to evaluate the accuracy of implant placement. Int J Comput Dent 22:139–147
Kaewsiri D, Panmekiate S, Subbalekha K, Mattheos N, Pimkhaokham A (2019) The accuracy of static vs. dynamic computer-assisted implant surgery in single tooth space: a randomized controlled trial. Clin Oral Implants Res 30:505–514. https://doi.org/10.1111/clr.13435
Block MS, Emery RW, Cullum DR, Sheikh A (2017) Implant placement is more asccurate using dynamic navigation. J Oral Maxillofac Surg 75:1377–1386. https://doi.org/10.1016/j.joms.2017.02.026
Sun TM, Lee HE, Lan TH (2020) Comparing accuracy of implant installation with a navigation system (NS), a laboratory guide (LG), NS with LG, and freehand drilling. Int J Environ Res Public Health 17:2107. https://doi.org/10.3390/ijerph17062107
Stefanelli LV, Mandelaris GA, Franchina A et al (2020) Accuracy evaluation of 14 maxillary full arch implant treatments performed with Da Vinci bridge: a case series. Materials (Basel) 13:2806. https://doi.org/10.3390/ma13122806
Stefanelli LV, Mandelaris GA, Franchina A et al (2020) Accuracy of dynamic navigation system workflow for implant supported full arch prosthesis : a case series. Int J Environ Res Public Health 17:5038. https://doi.org/10.3390/ijerph17145038
Yimarj P, Subbalekha K, Dhanesuan K, Siriwatana K, Mattheos N, Pimkhaokham A (2020) Comparison of the accuracy of implant position for two-implants supported fixed dental prosthesis using static and dynamic computer-assisted implant surgery: a randomized controlled clinical trial. Clin Implant Dent Relat Res. In press. https://doi.org/10.1111/cid.12949
Pellegrino G, Bellini P, Cavallini PF et al (2020) Dynamic navigation in dental implantology : The influence of surgical experience on implant placement accuracy and operating time . an in vitro study. Int J Environ Res Public Health 17:2153. https://doi.org/10.3390/ijerph17062153
Jorba-García A, Figueiredo R, González-Barnadas A, Camps-Font O, Valmaseda-Castellón E (2019) Accuracy and the role of experience in dynamic computer guided dental implant surgery: an in-vitro study. Med Oral Patol Oral Cir Bucal 24:76–83. https://doi.org/10.4317/medoral.22785
Somogyi-Ganss E, Holmes HI, Jokstad A (2015) Accuracy of a novel prototype dynamic computer-assisted surgery system. Clin Oral Implants Res 26:882–890. https://doi.org/10.1111/clr.12414
Widmann G, Keiler M, Zangerl A et al (2010) Computer-assisted surgery in the edentulous jaw based on 3 fixed intraoral reference points. J Oral Maxillofac Surg 68(5):1140–1147. https://doi.org/10.1016/j.joms.2009.10.008
Golob Deeb J, Frantar A, Deeb GR, Carrico CK, Rener-Sitar K (2020) In vitro comparison of time and accuracy of implant placement using trephine and conventional drilling techniques under dynamic navigation. J Oral Implantol. https://doi.org/10.1563/aaid-joi-D-19-00125
Sun T-M, Lee H-E, Lan T-H (2019) The influence of dental experience on a dental implant navigation system. BMC Oral Health 19:222. https://doi.org/10.1186/s12903-019-0914-2
Mediavilla Guzman A, Riad Deglow E, Zubizarreta-Macho A, Agustin-Panadero R, Hernandez Montero S (2019) Accuracy of computer-aided dynamic navigation compared to computer-aided static navigation for dental implant placement: an in vitro study. J Clin Med 8:2123. https://doi.org/10.3390/jcm8122123
Golob Deeb J, Bencharit S, Carrico CK et al (2019) Exploring training dental implant placement using computer-guided implant navigation system for predoctoral students: a pilot study. Eur J Dent Educ 23:415–423. https://doi.org/10.1111/eje.12447
Jiang W, Ma L, Zhang B et al (2018) Evaluation of the 3D augmented reality-guided intraoperative positioning of dental implants in edentulous mandibular models. Int J Oral Maxillofac Implants 33:1219–1228. https://doi.org/10.11607/jomi.6638
Sun T-M, Lan T-H, Pan C-Y, Lee H-E (2018) Dental implant navigation system guide the surgery future. Kaohsiung J Med Sci 34:56–64. https://doi.org/10.1016/j.kjms.2017.08.011
Chen C-K, Yuh D-Y, Huang R-Y, Fu E, Tsai C-F, Chiang C-Y (2018) Accuracy of implant placement with a navigation system, a laboratory guide, and freehand drilling. Int J Oral Maxillofac Implants 33:1213–1218. https://doi.org/10.11607/jomi.6585
Emery RW, Merritt SA, Lank K, Gibbs JD (2016) Accuracy of dynamic navigation for dental implant placement-model-based evaluation. J Oral Implantol 42:399–405. https://doi.org/10.1563/aaid-joi-D-16-00025
Kim SG, Lee WJ, Lee SS et al (2015) An advanced navigational surgery system for dental implants completed in a single visit: an in vitro study. J Craniomaxillofac Surg 43:117–125. https://doi.org/10.1016/j.jcms.2014.10.022
Zhou M, Zhou H, Li SY, Zhu YB, Geng YM (2020) Comparison of the accuracy of dental implant placement using static and dynamic computer-assisted systems: an in vitro study. J Stomatol Oral Maxillofac Surg 8:S2468-7855(20)30293-7. https://doi.org/10.1016/j.jormas.2020.11.008
Tahmaseb A, Wu V, Wismeijer D, Coucke W, Evans C (2018) The accuracy of static computer-aided implant surgery: a systematic review and meta-analysis. Clin Oral Implants Res 29:416–435. https://doi.org/10.1111/clr.13346
Bover-Ramos F, Vina-Almunia J, Cervera-Ballester J, Penarrocha-Diago M, Garcia-Mira B (2018) Accuracy of implant placement with computer-guided surgery: a systematic review and meta-analysis comparing cadaver, clinical, and in vitro studies. Int J Oral Maxillofac Implants 33:101–115. https://doi.org/10.11607/jomi.5556
Wang F, Bornstein MM, Hung K et al (2018) Application of real-time surgical navigation for zygomatic implant insertion in patients with severely atrophic maxilla. J Oral Maxillofac Surg 76:80–87. https://doi.org/10.1016/j.joms.2017.08.021
Feine J, Abou-Ayash S, Al Mardini M et al (2018) Group 3 ITI consensus report: patient-reported outcome measures associated with implant dentistry. Clin Oral Implants Res 29:270–275. https://doi.org/10.1111/clr.13299
Joda T, Derksen W, Wittneben JG, Kuehl S (2018) Static computer-aided implant surgery (s-CAIS) analysing patient-reported outcome measures (PROMs), economics and surgical complications: a systematic review. Clin Oral Implants Res 29:359–373. https://doi.org/10.1111/clr.13136
Pellegrino G, Mangano C, Mangano R, Ferri A, Taraschi V, Marchetti C (2019) Augmented reality for dental implantology: a pilot clinical report of two cases. BMC Oral Health 19:158. https://doi.org/10.1186/s12903-019-0853-y
Ma L, Jiang W, Zhang B et al (2019) Augmented reality surgical navigation with accurate CBCT-patient registration for dental implant placement. Med Biol Eng Comput 57:47–57. https://doi.org/10.1007/s11517-018-1861-9
Rawal S, Tillery DEJ, Brewer P (2020) Robotic-assisted prosthetically driven planning and immediate placement of a dental implant. Compend Contin Educ Dent 41:26–30
Acknowledgements
The authors wish to thank Mary Georgina Hardinge for her English language editing assistance.
Funding
The research was not supported by any source of funding.
Author information
Authors and Affiliations
Contributions
Adrià Jorba-García and Albert González-Barnadas: Conception of the review; literature search and data acquisition; article drafting; approval of the final version of the manuscript and agreement to be accountable for all aspects of the work.
Octavi Camps-Font: Conception of the review; analysis and interpretation of the data; critical review of the article; approval of the final version of the manuscript and agreement to be accountable for all aspects of the work.
Rui Figueiredo and Eduard Valmaseda-Castellón: Conception of the review; interpretation of the data; critical review of the article; approval of the final version of the manuscript and agreement to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Ethics approval
This article does not report on any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Conflict of interest
The authors have no direct financial or other interests in the products or information mentioned in this paper. Adrià Jorba-Garcia and Albert González-Barnadas declare no conflicts of interest. Dr. Octavi Camps-Font reports grants from Avinent (Santpedor, Spain) and has participated as a sub-investigator in clinical trials sponsored by Mundipharma (Cambridge, UK) and Menarini Richerche (Florence, Italy).
Dr. Rui Figueiredo reports grants, personal fees, and non-financial support from MozoGrau (Valladolid, Spain) and from Avinent (Santpedor, Spain) and personal fees from BioHorizons Iberica (Madrid, Spain), Inibsa Dental (Lliçà de Vall, Spain), Dentsply implants Iberia (Barcelona, Spain), and ADIN Implants (Afula, Israel) outside the submitted work. Dr. Figueiredo has also participated as a principal investigator in a randomized clinical trial sponsored by Mundipharma (Cambridge, UK) and in another clinical trial as a sub-investigator for Menarini Richerche (Florence, Italy). Dr. Eduard Valmaseda-Castellón reports personal fees and non-financial support from MozoGrau (Valladolid, Spain) and from Avinent (Santpedor, Spain) and personal fees from BioHorizons Iberica (Madrid, Spain), Inibsa Dental (Lliçà de Vall, Spain), and Dentsply implants Iberia (Barcelona, Spain) outside the submitted work. In addition, Dr. Valmaseda-Castellón has also participated as a sub-investigator in a randomized clinical trial sponsored by Mundipharma (Cambridge, UK).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOC 65.5 kb)
Rights and permissions
About this article
Cite this article
Jorba-García, A., González-Barnadas, A., Camps-Font, O. et al. Accuracy assessment of dynamic computer–aided implant placement: a systematic review and meta-analysis. Clin Oral Invest 25, 2479–2494 (2021). https://doi.org/10.1007/s00784-021-03833-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-03833-8