Abstract
Objectives
This study assessed the human pulp response after adhesive restoration of cavities by indirect pulp capping with a conventional or a resin-modified glass ionomer cement.
Materials and methods
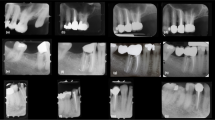
Deep cavities prepared in 26 human premolars were lined with Riva Light Cure (Riva LC), Riva Self Cure (Riva SC), or Dycal, and then restored with composite resin. Four teeth were used as intact control. After time intervals of 7 or 30 days, the teeth were extracted, processed for histological evaluation of the pulp, and the remaining dentin thickness (RDT) between the cavity floor and the pulp was measured.
Results
At 7 days, a slight pulp inflammation associated with discrete tissue disorganization was observed in most of t the teeth lined with Riva LC and Riva SC. Moderate pulp inflammation occurred in one tooth lined with Riva LC. Bacteria were identified in one specimen of the same group that exhibited no pulp damage. At 30 days, slight pulp inflammation and discrete tissue disorganization persisted in two specimens treated with Riva LC, in which a thin layer of tertiary dentin was deposited. Mean RDTs ranged from 383.0 to 447.8 μm.
Conclusions
Riva LC produced more damage to the pulp than Riva SC. However, the initial pulp damage decreased over time and after 30 days both GICs were labeled as biocompatible.
Clinical relevance
In this study conducted with human teeth, the conventional and the resin-modified glass ionomer cements investigated were shown not to cause post-operative sensitivity or persistent pulp damage when applied as liners in very deep cavities, thereby indicating their biocompatibility.




Similar content being viewed by others
References
Soares DG, Zhang Z, Mohamed F, Eyster TW, de Souza Costa CA, Ma PX (2018) Simvastatin and nanofibrous poly(l-lactic acid) scaffolds to promote the odontogenic potential of dental pulp cells in an inflammatory environment. Acta Biomater 1(68):190–203
Luiz de Oliveira da Rosa W, Machado da Silva T, Fernando Demarco F, Piva E, Fernandes da Silva A (2017) Could the application of bioactive molecules improve vital pulp therapy success? A systematic review. J Biomed Mater Res A 105(3):941–956
Hebling J, Giro EM, Costa CA (1999) Human pulp response after an adhesive system application in deep cavities. J Dent 27(8):557–564
de Souza Costa CA, Hebling J, Randall RC (2006) Human pulp response to resin cements used to bond inlay restorations. Dent Mater 22(10):954–962
de Souza Costa CA, Teixeira HM, Lopes do Nascimento AB, Hebling J (2007) Biocompatibility of resin based dental materials applied as liners in deep cavities prepared in human teeth. J Biomed Mater Res B Appl Biomater 81(1):175–184
Costa CA, Ribeiro AP, Giro EM, Randall RC, Hebling J (2011) Pulp response after application of two resin modified glass ionomer cements (RMGICs) in deep cavities of prepared human teeth. Dent Mater 27(7):e158–e170
Rodriguez IA, Ferrara CA, Campos Sanchez F, Alaminos M, Echevarria JU, Campos A (2013) An in vitro biocompatibility study of conventional and resin modified glass ionomer cements. J Adhes Dent 15(6):541–546
de Souza Costa CA, Hebling J, Scheffel DL, Soares DG, Basso FG, Ribeiro AP (2014) Methods to evaluate and strategies to improve the biocompatibility of dental materials and operative techniques. Dent Mater 30(7):769–784
Giraud T, Jeanneau C, Rombouts C, Bakhtiar H, Laurent P, About I (2019) Pulp capping materials modulate the balance between inflammation and regeneration. Dent Mater 35(1):24–35
Song M, Yu B, Kim S, Hayashi M, Smith C, Sohn S, Kim E, Lim J, Stevenson RG, Kim RH (2017) Clinical and molecular perspectives of reparative dentin formation: lessons learned from pulp capping materials and the emerging roles of calcium. Dent Clin of North Am 61(1):93–110
Prati C, Gandolfi MG (2015) Calcium silicate bioactive cements: biological perspectives and clinical applications. Dent Mater 31(4):351–370
Schwendicke F, Brouwer F, Schwendicke A, Paris S (2016) Different materials for direct pulp capping: systematic review and meta-analysis and trial sequential analysis. Clin Oral Investig 20(6):1121–1132
Frencken JE (2014) The state of the art of ART sealants. Dent Update 41(2):119–120 122-124
Berg JH, Croll TP (2015) Glass ionomer restorative cement systems: an update. Pediatr Dent 37(2):116–124
Mickenautsch S, Yengopal V, Banerjee A (2010) Pulp response to resin modified glass ionomer and calcium hydroxide cements in deep cavities: a quantitative systematic review. Dent Mater 26(8):761–770
Mesquita AJ, Lacerda-Santos R, Pina Godoy G, Nonaka CFW, Alves PM (2017) Morphological and immunohistochemical analysis of the biocompatibility of resin modified cements. Microsc Res Tech 80(5):504–510
Soares DG, Basso FG, Scheffel DL, Giro EM, de Souza Costa CA, Hebling J (2016) Biocompatibility of a restorative resin modified glass ionomer cement applied in very deep cavities prepared in human teeth. Gen Dent 64(4):33–40
Ribeiro DA, Marques ME, Salvadori DM (2006) Genotoxicity and cytotoxicity of glass ionomer cements on Chinese hamster ovary (CHO) cells. J Mater Sci Mater Med 17(6):495–500
Bakopoulou A, Mourelatos D, Tsiftsoglou AS, Giassin NP, Mioglou E, Garefis P (2009) Genotoxic and cytotoxic effects of different types of dental cement on normal cultured human lymphocytes. Mutat Res 31;672(2):103–112
Geurtsen W, Spahl W, Leyhausen G (1998) Residual monomer/additive release and variability in cytotoxicity of light curing glass ionomer cements and compomers. J Dent Res 77(12):2012–2019
Hamid A, Okamoto A, Iwaku M, Hume WR (1998) Component release from light activated glass ionomer and compomer cements. J Oral Rehabil 25(2):94–99
Kanchanavasita W, Anstice HM, Pearson GJ (1997) Water sorption characteristics of resin modified glass ionomer cements. Biomaterials 18(4):343–349
de Mendonca AA, Souza PP, Hebling J, Costa CA (2007) Cytotoxic effects of hard setting cements applied on the odontoblast cell line MDPC-23. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 104(4):e102–e108
Marczuk-Kolada G, Łuczaj-Cepowicz E, Pawińska M, Hołownia A (2017) Evaluation of the cytotoxicity of selected conventional glass ionomer cements on human gingival fibroblasts. Adv Clin Exp Med 26(7):1041–1045
Souza PP, Aranha AM, Hebling J, Giro EM, Costa CA (2006) In vitro cytotoxicity and in vivo biocompatibility of contemporary resin modified glass ionomer cements. Dent Mater 22(9):838–844
Noorani TY, Luddin N, Rahman IA, Masudi SM (2017) In vitro cytotoxicity evaluation of novel nano hydroxyapatite silica incorporated glass ionomer cement. J Clin Diagn Res 11(4):ZC105–ZC109
de Souza Costa CA, Hebling J, Garcia Godoy F, Hanks CT (2003) In vitro cytotoxicity of five glass ionomer cements. Biomaterials 24(21):3853–3858
Gallorini M, Cataldi A, di Giacomo V (2014) HEMA induced cytotoxicity: oxidative stress, genotoxicity and apoptosis. Int Endod J 47(9):813–818
Teti G, Orsini G, Salvatore V, Focaroli S, Mazzotti MC, Ruggeri A, Mattioli Belmonte M, Falconi M (2015) HEMA but not TEGDMA induces autophagy in human gingival fibroblasts. Front Physiol 6:275
Krifka S, Spagnuolo G, Schmalz G, Schweikl H (2013) A review of adaptive mechanisms in cell responses towards oxidative stress caused by dental resin monomers. Biomaterials 34(19):4555–4563
Stanislawski L, Daniau X, Lautic A, Goldberg M (1999) Factors responsible for pulp cell cytotoxicity induced by resin modified glass ionomer cements. J Biomed Mater Res 48(3):277–288
Schmalz G, Krifka S, Schweikl H (2011) Toll like receptors, LPS, and dental monomers. Adv Dent Res 23(3):302–306
Bolling AK, Samuelsen JT, Morisbak E, Ansteinsson V, Becher R, Dahl JE, Mathisen GH (2013) Dental monomers inhibit LPS induced cytokine release from the macrophage cell line RAW264.7. Toxicol Lett 216(23):130–138
Di Nicolo R, Shintome LK, Myaki SI, Nagayassu MP (2007) Bond strength of resin modified glass ionomer cement to primary dentin after cutting with different bur types and dentin conditioning. J Appl Oral Sci 15(5):459–464
About I, Murray PE, Franquin JC, Remusat M, Smith AJ (2001) The effect of cavity restoration variables on odontoblast cell numbers and dental repair. J Dent 29(2):109–117
Hashimoto M, Ito S, Tay FR, Svizero NR, Sano H, Kaga M, Pashley DH (2004) Fluid movement across the resin dentin interface during and after bonding. J Dent Res 83(11):843–848
Yoshikawa T, Hirasawa M, Tosaki S, Hirota K (1994) Concentration of HEMA eluted from light cured glass ionomers. J Dent Res 73:133
Volk J, Ziemann C, Leyhausen G, Geurtsen W (2009) Non irradiated campherquinone induces DNA damage in human gingival fibroblasts. Dent Mater 25(12):1556–1563
Volk J, Leyhausen G, Wessels M, Geurtsen W (2014) Reduced glutathione prevents camphorquinone induced apoptosis in human oral keratinocytes. Dent Mater 30(2):215–226
Savas S, Botsali MS, Kucukyilmaz E, Sari T (2014) Evaluation of temperature changes in the pulp chamber during polymerization of light cured pulp capping materials by using a VALO LED light curing unit at different curing distances. Dent Mater Journal 33(6):764–769
Zach L, Cohen G (1965) Pulp response to externally applied heat. Oral Surg Oral Med Oral Pathol 19:515–530
Lizarelli RF, Moriyama LT, Bagnato VS (2006) Temperature response in the pulp chamber of primary human teeth exposed to Nd:YAG laser using a picosecond pulsed regime. Photomed Laser Surg 24(5):610–615
Santis LR, Silva TM, Haddad BA, Goncalves LL, Goncalves SE (2017) Influence of dentin thickness on intrapulpal temperature under simulated pulpal pressure during Nd:YAG laser irradiation. Lasers Med Sci 32(1):161–167
Kim S (1990) Neurovascular interactions in the dental pulp in health and inflammation. J Endod 16(2):48–53
Aranha AM, Giro EM, Souza PP, Hebling J, de Souza Costa CA (2006) Effect of curing regime on the cytotoxicity of resin-modified glass-ionomer lining cements applied to an odontoblast-cell line. Dent Mater 22(9):864–869
Acknowledgments
The authors would like to thank Mr. Jose Antonio Sampaio Zuanon, technician of the Laboratory of Pathology, Department of Physiology and Pathology, Univ Estadual Paulista—Unesp, Araraquara School of Dentistry, SP, Brazil, for all technical support provided in this in vivo study.
Funding
This study was partially supported by the National Council for Scientific and Technological Development—CNPq (grant # 307696/2014-6 and # 408721/2018-9) and SDI Limited, Bayswater, Victoria, Australia.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Research Ethics Committee of the University of Araraquara, Araraquara, Sao Paulo, Brazil, Protocol # 645.
Informed consent
Formal consent was provided by the donors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ribeiro, A.P.D., Sacono, N.T., Soares, D.G. et al. Human pulp response to conventional and resin-modified glass ionomer cements applied in very deep cavities. Clin Oral Invest 24, 1739–1748 (2020). https://doi.org/10.1007/s00784-019-03035-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-03035-3