Abstract
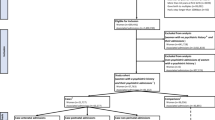
Pregnancy in women suffering from psychotic disorders is becoming more common. However, this psychiatric disorder is linked to the highest risk of early mother and child separation. The aim of this study was to evaluate risk factors associated with these separations. In an observational, naturalist, and multicentric study, 320 women suffering from a psychotic disorder and jointly hospitalized with their child in one of the sixteen mother-baby units (MBUs) in France and Belgium between 2001 and 2010 were assessed for risk factors associated with mother-child separation. Eighty-seven (27.2%) mothers were separated from their infant at discharge from MBUs. Early separation was linked to the placement of the mother herself in an institution in childhood (OR 4.44; CI 95% 1.12–18.69), to the mother being single (OR 3.84; CI 95% 1.38–11.44), to early hospitalization of the baby in neonatology (OR 2.88; CI 95% 1.27–6.59), and to maternal psychiatric decompensation during pregnancy (OR 2.60; CI 95% 1.15–6.20), independently from maternal neglectful behaviors. Low family/social support showed a trend towards association with separation (OR 2.17; CI 95% 0.91–5.42). This study shows that separation is mostly linked to mothers’ environmental and interactive past and current history, to the child’s health, and to maternal mental health decompensation. The identification of these factors is essential to implement antenatal prevention and social programs for these women. Further studies should focus on the long-term development of children of schizophrenic mothers, whether or not they have been placed, in order to help clarifying the impact of the risk factors.
Similar content being viewed by others
References
Buist A, Minto B, Szego K, Samhuel M, Shawyer L, O’Connor L (2004) Mother-baby psychiatric units in Australia—the Victorian experience. Arch Womens Ment Health 7:81–87
Cazas O, Glangeaud-Freudenthal NM (2004) The history of Mother-Baby Units (MBUs) in France and Belgium and of the French version of the Marcé checklist. Arch Womens Ment Health 7:53–58
Gearing RE, Alonzo D, Marinelli C (2012) Maternal schizophrenia: psychosocial treatment for mothers and their children. Clin Schizophr Relat Psychoses 6:27–33
Glangeaud-Freudenthal NM-C (2004) Mother-baby psychiatric units (MBUs): national data collection in France and in Belgium (1999–2000). Arch Womens Ment Health 7:59–64
Glangeaud-Freudenthal NM, Howard LM, Sutter-Dallay AL (2014). Treatment - mother-infant inpatient units. Best Pract Res Clin Obstet Gynaecol 28:147–157
Glangeaud-Freudenthal NM-C, Sutter-Dallay A-L, Thieulin A-C, Dagens V, Zimmermann M-A, Debourg A, Amzallag C, Cazas O, Cammas R, Klopfert ME, Rainelli C, Tielemans P, Mertens C, Maron M, Nezelof S, Poinso F (2013) Predictors of infant foster care in cases of maternal psychiatric disorders. Soc Psychiatry Psychiatr Epidemiol 48:553–561
Gressier F, Guillard V, Cazas O, Falissard B, Glangeaud-Freudenthal NM, Sutter-Dallay AL (2017) Risk factors for suicide attempt in pregnancy and the post-partum period in women with serious mental illnesses. J Psychiatr Res 84:284–291
Hammond J, Lipsedge M (2015) Assessing parenting capacity in psychiatric mother and baby units: a case report and review of literature. Psychiatr Danub 27(Suppl 1):S71–S83
Harlow BL, Vitonis AF, Sparen P, Cnattingius S, Joffe H, Hultman CM (2007) Incidence of hospitalization for postpartum psychotic and bipolar episodes in women with and without prior prepregnancy or prenatal psychiatric hospitalizations. Arch Gen Psychiatry 64:42–48
Hollingsworth LD (2004) Child custody loss among women with persistent severe mental illness. Soc Work Res 28:199–209
Howard LM (2005) Fertility and pregnancy in women with psychotic disorders. Eur J Obstet Gynecol Reprod Biol 119:3–10
Howard LM, Kumar R, Thornicroft G (2001) Psychosocial characteristics and needs of mothers with psychotic disorders. Br J Psychiatry J Ment Sci 178:427–432
Howard L, Shah N, Salmon M, Appleby L (2003) Predictors of social services supervision of babies of mothers with mental illness after admission to a psychiatric mother and baby unit. Soc Psychiatry Psychiatr Epidemiol 38:450–455
Howard LM, Thornicroft G, Salmon M, Appleby L (2004) Predictors of parenting outcome in women with psychotic disorders discharged from mother and baby units. Acta Psychiatr Scand 110:347–355
Jiménez-Morago JM, León E, Román M (2015) Adversity and adjustment in children in institutions, family foster care, and adoption. Span J Psychol 18:E45
Johnson R, Browne K, Hamilton-Giachritsis C (2006) Young children in institutional care at risk of harm. Trauma Violence Abuse 7:34–60
Kumar R, Marks M, Platz C, Yoshida K (1995) Clinical survey of a psychiatric mother and baby unit: characteristics of 100 consecutive admissions. J Affect Disord 33:11–22
Lagan M, Knights K, Barton J, Boyce PM (2009) Advocacy for mothers with psychiatric illness: a clinical perspective. Int J Ment Health Nurs 18(1):53–61
Park JM, Solomon P, Mandell DS (2006) Involvement in the child welfare system among mothers with serious mental illness. Psychiatr Serv Wash DC 57:493–497
Parnas J, Teasdale TW, Schulsinger H (1985) Institutional rearing and diagnostic outcome in children of schizophrenic mothers. A prospective high-risk study. Arch Gen Psychiatry 42:762–769
Parnas J, Cannon TD, Jacobsen B, Schulsinger H, Schulsinger F, Mednick SA (1993) Lifetime DSM-III-R diagnostic outcomes in the offspring of schizophrenic mothers. Results from the Copenhagen High-Risk Study. Arch Gen Psychiatry 50(9):707–714
Plant K, Byrne L, Barkla J, McLean D, Hearle J, McGrath J (2014) Parents with psychosis: a pilot study examining self-report measures related to family functioning. Aust E-J Adv Ment Health 1:38–48
Poinso F, Gay MP, Glangeaud-Freudenthal NMC, Rufo M (2002) Care in a mother-baby psychiatric unit: analysis of separation at discharge. Arch Womens Ment Health 5:49–58
Salmon M, Abel K, Cordingley L, Friedman T, Appleby L (2003) Clinical and parenting skills outcomes following joint mother-baby psychiatric admission. Aust N Z J Psychiatry 37:556–562
Salmon MP, Abel K, Webb R, Warburton AL, Appleby L (2004) A national audit of joint mother and baby admissions to UK psychiatric hospitals: an overview of findings. Arch Womens Ment Health 7:65–70
Seeman MV (2012) Intervention to prevent child custody loss in mothers with schizophrenia. Schizophr Res Treat 2012:796763
Seeman MV (2013) Clinical interventions for women with schizophrenia: pregnancy. Acta Psychiatr Scand 127:12–22
Simkiss DE, Spencer NJ, Stallard N, Thorogood M (2012) Health service use in families where children enter public care: a nested case control study using the General Practice Research Database. BMC Health Serv Res 12:65
Vittinghoff E, McCulloch CE (2007) Relaxing the rule of ten events per variable in logistic and cox regression. Am J Epidemiol 165:710–718
Walker EF, Cudeck R, Mednick SA, Schulsinger F (1981) Effects of parental absence and institutionalization on the development of clinical symptoms in high-risk children. Acta Psychiatr Scand 63:95–109
Wan MW, Salmon MP, Riordan DM, Appleby L, Webb R, Abel KM (2007) What predicts poor mother-infant interaction in schizophrenia? Psychol Med 37:537–546
Whitmore J, Heron J, Wainscott G (2011) Predictors of parenting concern in a mother and baby unit over a 10-year period. Int J Soc Psychiatr 57:455–461
WHO (n.d.) | Schizophrenia http://www.who.int/mediacentre/factsheets/fs397/fr/
Winokur M, Holtan A, Batchelder KE (2014) Kinship care for the safety, permanency, and well-being of children removed from the home for maltreatment. Cochrane Database Syst Rev 1:CD006546
Acknowledgments
The authors thank members of MBUs: Bordeaux, Montesson, Strasbourg, Le Vesinet, Créteil, Villejuif, Paris, Brussels, Limoges, Ottiginies, Marseille, Gent, Lille, Besançon, Albi, Brumath, who contributed to data collection and the women who participated in the study.
We also thank the Francophone Marcé Society.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All women provided informed consent for their inclusion in the database. The study was performed in accordance with the ethics standards of the French National Data Protection Authority (CNIL). The CNIL approved the study.
Conflict of interest
Regarding potential conflicts of interest, all of them were indirect:
Agathe Cès, Nine Glangeaud-Freudenthal, and Anne-Laure Sutter-Dallay report no financial relationships with commercial interests.
Bruno Falissard has been a consultant and expert or has given talks for E. Lilly, BMS, Servier, Sanofi, GlaxoSmithKline, HRA, Roche, Boeringer Ingelheim, Bayer, Almirall, Allergan, Stallergene, Genzyme, Pierre Fabre, Astra Zeneca, Novartis, Janssen, Astellas, Biotronik, Daiichi-Sankyo, Gilead, MSD, Lundbeck.
Florence Gressier has given talks for Lundbeck and Servier and received a grant from Servier for a postdoctoral degree (2011–2012).
Rights and permissions
About this article
Cite this article
Cès, A., Falissard, B., Glangeaud-Freudenthal, N.M.C. et al. Pregnancy in women with psychotic disorders: risk factors associated with mother-baby separation. Arch Womens Ment Health 21, 699–706 (2018). https://doi.org/10.1007/s00737-018-0848-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-018-0848-8