Abstract
Background
The consequences of suffering postoperative complications in elderly undergoing spinal surgeries may be different compared to younger patients. The primary objective of this study was to identify the types and frequency of medical complications and mortality rates in patients 80 years of age or older undergoing elective spinal fusion surgeries for degenerative spinal disease.
Methods
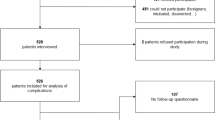
A prospective observational study with a retrospective chart review was performed, which included all consecutive patients ≥80 years old undergoing elective spinal fusion surgeries from May 2012 to August 2015. We identified a total of 95 patients, of which 39 cervical and 56 lumbar surgeries were performed. There were 41 female and 54 male patients with the mean age of 82.8 years (range, 80–91). The perioperative complications were allocated into the following categories: infection, pulmonary, cardiac, gastrointestinal, hematologic, urologic, neurovascular, thromboembolic, and other. Baseline and postoperative clinical outcome scores were compared to evaluate efficacy.
Results
The mean follow-up time was 14.8 months (range, 5 days to 37 months) with an overall mortality rate of 8.4%. The 30-day, 90-day, and 1-year mortality rates were 2.1, 2.1, and 4.2%, respectively. There were 53.9 and 71.4% patients with complications in the cervical and lumbar patient groups, respectively. The presence of general comorbidities and the number of intervertebral levels predicted the occurrence of perioperative complications. Also, longer OR times were associated with a higher number of complications per patient and the occurrence of a UTI. Dysphagia was a significant predictor in developing pneumonia and atelectasis.
Conclusions
The incidence of perioperative medical complications and mortality rates in octogenarians undergoing elective spinal surgeries are quite high. The benefits of having surgery must be weighed against the risks of not only surgical but also adverse medical events. An informed decision-making process should include discussion of potential postoperative morbidity specific to this patient population in order to guide patient’s acceptance of higher risks and expectations postoperatively. It is also important to identify potential complications and adapt preventive measures in order to help minimize them in this patient population.
Similar content being viewed by others
Abbreviations
- ALIF:
-
Anterior lumbar interbody fusion
- ASA:
-
American Society of Anesthesiologists
- EBL:
-
Estimated blood loss
- MCS:
-
Mental component summary
- ODI:
-
Oswestry Disability Index
- OR:
-
Operating room
- PCS:
-
Physical component summary
- SF-36:
-
Short-Form Health Survey
- UTI:
-
Urinary track infection
- VAS:
-
Visual analog scale
References
Balabaud L, Pitel S, Caux I, Dova C, Richard B, Antonietti P, Mazel C (2015) Lumbar spine surgery in patients 80 years of age or older: morbidity and mortality. Eur J Orthop Surg Traumatol 25(Suppl 1):S205–S212. https://doi.org/10.1007/s00590-014-1556-3
Baron EM, Soliman AM, Gaughan JP, Simpson L, Young WF (2003) Dysphagia, hoarseness, and unilateral true vocal fold motion impairment following anterior cervical diskectomy and fusion. Ann Otol Rhinol Laryngol 112:921–926. https://doi.org/10.1177/000348940311201102
Barretto de Carvalho Fernandes MC, Vieira da Costa V, Saraiva RA (2007) Postoperative urinary retention: evaluation of patients using opioids analgesic. Rev Lat Am Enfermagem 15:318–322
Benz RJ, Ibrahim ZG, Afshar P, Garfin SR (2001) Predicting complications in elderly patients undergoing lumbar decompression. Clin Orthop Relat Res 384:116–121
Boakye M, Patil CG, Santarelli J, Ho C, Tian W, Lad SP (2008) Cervical spondylotic myelopathy: complications and outcomes after spinal fusion. Neurosurgery 62:455–461; discussion 461-452. https://doi.org/10.1227/01.neu.0000316013.97926.4c
Bohl DD, Ahn J, Tabaraee E, Ahn J, Jain A, Grauer JN, Singh K (2015) Urinary tract infection following posterior lumbar fusion procedures: an American College of Surgeons National Surgical Quality Improvement Program Study. Spine (Phila Pa 1976) 40:1785–1791. https://doi.org/10.1097/BRS.0000000000001003
Buerba RA, Giles E, Webb ML, Fu MC, Gvozdyev B, Grauer JN (2014) Increased risk of complications after anterior cervical discectomy and fusion in the elderly: an analysis of 6253 patients in the American College of Surgeons National Surgical Quality Improvement Program database. Spine (Phila Pa 1976) 39:2062–2069. https://doi.org/10.1097/BRS.0000000000000606
Bydon M, Abt NB, De la Garza-Ramos R, Olorundare IO, McGovern K, Sciubba DM, Gokaslan ZL, Bydon A (2015) Impact of age on short-term outcomes after lumbar fusion: an analysis of 1395 patients stratified by decade cohorts. Neurosurgery 77:347–353; discussion 353-344. https://doi.org/10.1227/NEU.0000000000000852
Cabre M, Serra-Prat M, Palomera E, Almirall J, Pallares R, Clave P (2010) Prevalence and prognostic implications of dysphagia in elderly patients with pneumonia. Age Ageing 39:39–45. https://doi.org/10.1093/ageing/afp100
Carreon LY, Puno RM, Dimar JR 2nd, Glassman SD, Johnson JR (2003) Perioperative complications of posterior lumbar decompression and arthrodesis in older adults. J Bone Joint Surg Am 85-A:2089–2092
Cassinelli EH, Eubanks J, Vogt M, Furey C, Yoo J, Bohlman HH (2007) Risk factors for the development of perioperative complications in elderly patients undergoing lumbar decompression and arthrodesis for spinal stenosis: an analysis of 166 patients. Spine (Phila Pa 1976) 32:230–235. https://doi.org/10.1097/01.brs.0000251918.19508.b3
Chang MS, Chang YH, Revella J, Crandall DG (2014) Revision spinal fusion in patients older than 75: is it worth the risks? Spine (Phila Pa 1976) 39:E35–E39. https://doi.org/10.1097/BRS.0000000000000067
Chen TY, Anderson DJ, Chopra T, Choi Y, Schmader KE, Kaye KS (2010) Poor functional status is an independent predictor of surgical site infections due to methicillin-resistant Staphylococcus aureus in older adults. J Am Geriatr Soc 58:527–532. https://doi.org/10.1111/j.1532-5415.2010.02719.x
Chikuda H, Yasunaga H, Horiguchi H, Takeshita K, Sugita S, Taketomi S, Fushimi K, Tanaka S (2013) Impact of age and comorbidity burden on mortality and major complications in older adults undergoing orthopaedic surgery: an analysis using the Japanese diagnosis procedure combination database. BMC Musculoskelet Disord 14:173. https://doi.org/10.1186/1471-2474-14-173
Cloyd JM, Acosta FL Jr, Cloyd C, Ames CP (2010) Effects of age on perioperative complications of extensive multilevel thoracolumbar spinal fusion surgery. J Neurosurg Spine 12:402–408. https://doi.org/10.3171/2009.10.SPINE08741
Creditor MC (1993) Hazards of hospitalization of the elderly. Ann Intern Med 118:219–223
Deiner S, Westlake B, Dutton RP (2014) Patterns of surgical care and complications in elderly adults. J Am Geriatr Soc 62:829–835. https://doi.org/10.1111/jgs.12794
Deyo RA, Hickam D, Duckart JP, Piedra M (2013) Complications after surgery for lumbar stenosis in a veteran population. Spine (Phila Pa 1976) 38:1695–1702. https://doi.org/10.1097/BRS.0b013e31829f65c1
Dunne JR, Malone D, Tracy JK, Gannon C, Napolitano LM (2002) Perioperative anemia: an independent risk factor for infection, mortality, and resource utilization in surgery. J Surg Res 102:237–244. https://doi.org/10.1006/jsre.2001.6330
Eismont FJ, Norton RP, Hirsch BP (2014) Surgical management of lumbar degenerative spondylolisthesis. J Am Acad Orthop Surg 22:203–213. https://doi.org/10.5435/JAAOS-22-04-203
Fineberg SJ, Ahmadinia K, Patel AA, Oglesby M, Singh K (2013) Incidence and mortality of cardiac events in lumbar spine surgery. Spine (Phila Pa 1976) 38:1422–1429. https://doi.org/10.1097/BRS.0b013e3182986d71
Fineberg SJ, Oglesby M, Patel AA, Singh K (2013) Incidence, risk factors, and mortality associated with aspiration in cervical spine surgery. Spine 38:E1189–E1195. https://doi.org/10.1097/BRS.0b013e31829cc19b
Frazier SC (2005) Health outcomes and polypharmacy in elderly individuals: an integrated literature review. J Gerontol Nurs 31:4–11
Galiano K, Obwegeser AA, Gabl MV, Bauer R, Twerdy K (2005) Long-term outcome of laminectomy for spinal stenosis in octogenarians. Spine (Phila Pa 1976) 30:332–335
Glassman SD, Carreon LY, Dimar JR, Campbell MJ, Puno RM, Johnson JR (2007) Clinical outcomes in older patients after posterolateral lumbar fusion. Spine J 7:547–551. https://doi.org/10.1016/j.spinee.2006.11.003
Hamel MB, Henderson WG, Khuri SF, Daley J (2005) Surgical outcomes for patients aged 80 and older: morbidity and mortality from major noncardiac surgery. J Am Geriatr Soc 53:424–429. https://doi.org/10.1111/j.1532-5415.2005.53159.x
Hayashi K, Matsumura A, Konishi S, Kato M, Namikawa T, Nakamura H (2016) Clinical outcomes of posterior lumbar Interbody fusion for patients 80 years of age and older with lumbar degenerative disease: minimum 2 years’ follow-up. Glob Spine J 6:665–672. https://doi.org/10.1055/s-0036-1578806
Jakola AS, Sorlie A, Gulati S, Nygaard OP, Lydersen S, Solberg T (2010) Clinical outcomes and safety assessment in elderly patients undergoing decompressive laminectomy for lumbar spinal stenosis: a prospective study. BMC Surg 10:34. https://doi.org/10.1186/1471-2482-10-34
Kalanithi PS, Patil CG, Boakye M (2009) National complication rates and disposition after posterior lumbar fusion for acquired spondylolisthesis. Spine (Phila Pa 1976) 34:1963–1969. https://doi.org/10.1097/BRS.0b013e3181ae2243
Li G, Patil CG, Lad SP, Ho C, Tian W, Boakye M (2008) Effects of age and comorbidities on complication rates and adverse outcomes after lumbar laminectomy in elderly patients. Spine (Phila Pa 1976) 33:1250–1255. https://doi.org/10.1097/BRS.0b013e3181714a44
Loeb MB, Becker M, Eady A, Walker-Dilks C (2003) Interventions to prevent aspiration pneumonia in older adults: a systematic review. J Am Geriatr Soc 51:1018–1022
Manku K, Bacchetti P, Leung JM (2003) Prognostic significance of postoperative in-hospital complications in elderly patients. I. Long-term survival. Anesth Analg 96:583–589 table of contents
Merani S, Payne J, Padwal RS, Hudson D, Widder SL, Khadaroo RG (2014) Predictors of in-hospital mortality and complications in very elderly patients undergoing emergency surgery. World J Emerg Surg 9:43. https://doi.org/10.1186/1749-7922-9-43
Nagashima H, Dokai T, Hashiguchi H, Ishii H, Kameyama Y, Katae Y, Morio Y, Morishita T, Murata M, Nanjo Y, Takahashi T, Tanida A, Tanishima S, Yamane K, Teshima R (2011) Clinical features and surgical outcomes of cervical spondylotic myelopathy in patients aged 80 years or older: a multi-center retrospective study. Eur Spine J 20:240–246. https://doi.org/10.1007/s00586-010-1672-7
Nanjo Y, Nagashima H, Dokai T, Hamamoto Y, Hashiguchi H, Ishii H, Kameyama Y, Morio Y, Murata M, Tanida A, Tanishima S, Teshima R (2013) Clinical features and surgical outcomes of lumbar spinal stenosis in patients aged 80 years or older: a multi-center retrospective study. Arch Orthop Trauma Surg 133:1243–1248. https://doi.org/10.1007/s00402-013-1808-4
Nie H, Hao J, Peng C, Ou Y, Quan Z, An H (2013) Clinical outcomes of discectomy in octogenarian patients with lumbar disc herniation. J Spinal Disord Tech 26:74–78. https://doi.org/10.1097/BSD.0b013e318236b92d
Oldridge NB, Yuan Z, Stoll JE, Rimm AR (1994) Lumbar spine surgery and mortality among Medicare beneficiaries, 1986. Am J Public Health 84:1292–1298
Puvanesarajah V, Jain A, Shimer AL, Li X, Singla A, Shen F, Hassanzadeh H (2016) Complications and mortality following 1 to 2 level lumbar fusion surgery in patients above 80 years of age. Spine (Phila Pa 1976). https://doi.org/10.1097/BRS.0000000000001759
Raffo CS, Lauerman WC (2006) Predicting morbidity and mortality of lumbar spine arthrodesis in patients in their ninth decade. Spine (Phila Pa 1976) 31:99–103
Rihn JA, Hilibrand AS, Zhao W, Lurie JD, Vaccaro AR, Albert TJ, Weinstein J (2015) Effectiveness of surgery for lumbar stenosis and degenerative spondylolisthesis in the octogenarian population: analysis of the spine patient outcomes research trial (SPORT) data. J Bone Joint Surg Am 97:177–185. https://doi.org/10.2106/JBJS.N.00313
Rodgers WB, Gerber EJ, Rodgers JA (2010) Lumbar fusion in octogenarians: the promise of minimally invasive surgery. Spine (Phila Pa 1976) 35:S355–S360. https://doi.org/10.1097/BRS.0b013e3182023796
Shabat S, Arinzon Z, Folman Y, Leitner J, David R, Pevzner E, Gepstein R, Pekarsky I, Shuval I (2008) Long-term outcome of decompressive surgery for lumbar spinal stenosis in octogenarians. Eur Spine J 17:193–198. https://doi.org/10.1007/s00586-007-0514-8
Shen Y, Silverstein JC, Roth S (2009) In-hospital complications and mortality after elective spinal fusion surgery in the united states: a study of the nationwide inpatient sample from 2001 to 2005. J Neurosurg Anesthesiol 21:21–30. https://doi.org/10.1097/ANA.0b013e31818b47e9
Sura L, Madhavan A, Carnaby G, Crary MA (2012) Dysphagia in the elderly: management and nutritional considerations. Clin Interv Aging 7:287–298. https://doi.org/10.2147/CIA.S23404
Vitaz TW, Raque GH, Shields CB, Glassman SD (1999) Surgical treatment of lumbar spinal stenosis in patients older than 75 years of age. J Neurosurg 91:181–185
Wang MC, Chan L, Maiman DJ, Kreuter W, Deyo RA (2007) Complications and mortality associated with cervical spine surgery for degenerative disease in the United States. Spine (Phila Pa 1976) 32:342–347. https://doi.org/10.1097/01.brs.0000254120.25411.ae
Wang MY, Green BA, Shah S, Vanni S, Levi AD (2003) Complications associated with lumbar stenosis surgery in patients older than 75 years of age. Neurosurg Focus 14:e7
Wang MY, Widi G, Levi AD (2015) The safety profile of lumbar spinal surgery in elderly patients 85 years and older. Neurosurg Focus 39:E3. https://doi.org/10.3171/2015.7.FOCUS15180
Yoshihara H, Yoneoka D (2014) Trends in the incidence and in-hospital outcomes of elective major orthopaedic surgery in patients eighty years of age and older in the United States from 2000 to 2009. J Bone Joint Surg Am 96:1185–1191. https://doi.org/10.2106/JBJS.M.01126
Young EY, Ahmadinia K, Bajwa N, Ahn NU (2013) Does chronic warfarin cause increased blood loss and transfusion during lumbar spinal surgery? Spine J 13:1253–1258. https://doi.org/10.1016/j.spinee.2013.05.052
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
Formal consent was not required.
Rights and permissions
About this article
Cite this article
Rajpal, S., Lee Nelson, E., Villavicencio, A.T. et al. Medical complications and mortality in octogenarians undergoing elective spinal fusion surgeries. Acta Neurochir 160, 171–179 (2018). https://doi.org/10.1007/s00701-017-3384-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-017-3384-9