Abstract
Purpose
Low back pain (LBP) is a major public health problem worldwide. Significant practice variation exists despite guidelines, including strong interventionist focus by some practitioners. Translation of guidelines into pathways as integrated treatment plans is a next step to improve implementation. The goal of the present study was to analyze international examples of LBP pathways in order to identify key interventions as building elements for care pathway for LBP and radicular pain.
Methods
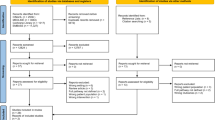
International examples of LBP pathways were searched in literature and grey literature. Authors of pathways were invited to fill a questionnaire and to participate in an in-depth telephone interview. Pathways were quantitatively and qualitatively analyzed, to enable the identification of key interventions to serve as pathway building elements.
Results
Eleven international LBP care pathways were identified. Regional pathways were strongly organized and included significant training efforts for primary care providers and an intermediate level of caregivers in between general practitioners and hospital specialists. Hospital pathways had a focus on multidisciplinary collaboration and stepwise approach trajectories. Key elements common to all pathways included the consecutive screening for red flags, radicular pain and psychosocial risk factors, the emphasis on patient empowerment and self-management, the development of evidence-based consultable protocols, the focus on a multidisciplinary work mode and the monitoring of patient-reported outcome measures.
Conclusion
Essential building elements for the construction of LBP care pathways were identified from a transversal analysis of key interventions in a study of 11 international examples of LBP pathways.



Similar content being viewed by others
Availability of data and material
All data are provided in the Supplementary Materials.
References
Hoy D, Brooks P, Blyth F, Buchbinder R (2010) The epidemiology of low back pain. Best Pract Res Clin Rheumatol 24:769–781
GBD 2017 Disease and Injury Incidence and Prevalence Collaborators (2018) Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392:1789–1858
Hoy D, March L, Brooks P, Blyth F, Woolf A, Bain C et al (2014) The global burden of low back pain: estimates from the Global Burden of Disease 2010 study. Ann Rheum Dis 73:968–974
Olafsson G, Jonsson E, Fritzell P, Hägg O, Borgström F (2017) A health economic lifetime treatment pathway model for low back pain in Sweden. J Med Econ 20:1281–1289
Olafsson G, Jonsson E, Fritzell P, Hägg O, Borgström F (2018) Cost of low back pain: results from a national registry study in Sweden. Eur Spine J 27:2875–2881
Martin BI, Deyo RA, Mirza SK, Turner JA, Comstock BA, Hollingworth W et al (2008) Expenditures and health status among adults with back and neck problems. JAMA 299:656–664
van Zundert J, van Kleef M (2005) Low back pain: from algorithm to cost-effectiveness? Pain Pract 5:179–189
Enthoven P, Skargren E, Oberg B (2004) Clinical course in patients seeking primary care for back or neck pain: a prospective 5-year follow-up of outcome and health care consumption with subgroup analysis. Spine 29:2458–2465
Itz CJ, Geurts JW, van Kleef M, Nelemans P (2013) Clinical course of non-specific low back pain: a systematic review of prospective cohort studies set in primary care. Eur J Pain 17:5–15
Canizares M, Rampersaud YR, Badley EM (2019) Course of back pain in the Canadian population: trajectories, predictors, and outcomes. Arthritis Care Res 71:1660–1670
Deyo RA, Mirza SK, Turner JA, Martin BI (2009) Overtreating chronic back pain: time to back off? J Am Board Fam Med 22:62–68
Koes BW, van Tulder M, Lin CW, Macedo LG, McAuley J, Maher C (2010) An updated overview of clinical guidelines for the management of non-specific low back pain in primary care. Eur Spine J 19:2075–2094
Dubois M (2013) PhD dissertation. Causes and prevention of long-term disability due to low back pain. KULeuven, Leuven
Vinck I, Vijverman A, Vollebregt E, Broeckx N, Wouters K, Piët M, Bacic N, Vlayen J, Thiry N, Neyt M (2018) Responsible use of high-risk medical devices: the example of 3D printed medical devices. Health Technology Assessment. Belgian Healthcare Knowledge Center Report 297A
Scott NA, Moga C, Harstall C (2010) Managing low back pain in the primary care setting: the know-do gap. Pain Res Manag 15:392–400
Vanhaecht KDWK, Sermeus W (2007) The impact of clinical pathways on the organisation of care processes. ACCO, Leuven
Van Wambeke P, Desomer A, Ailliet L, Berquin A, Demoulin C et al (2017) Low back pain and radicular pain: assessment and management. Belgian Healthcare Knowledge Center report 287A
Fourney DR, Dettori JR, Hall H, Hartl R, McGirt MJ, Daubs MD (2011) A systematic review of clinical pathways for lower back pain and introduction of the Saskatchewan Spine pathway. Spine 36(21 Suppl):S164–S171
Dierckx de Casterlé B, Gastmans C, Bryon E, Denier Y (2012) Quagol: a quide for quantitative data analysis. Int J Nurs Stud 49:360–371
Kindrachuk DR, Fourney DR (2014) Spine surgery referrals redirected through a multidisciplinary care pathway: effects of nonsurgeon triage including MRI utilization. J Neurosurg Spine 20:87–92
Wilgenbusch CS, Wu AS, Fourney DR (2014) Triage of spine surgery referrals through a multidisciplinary care pathway: a value-based comparison with conventional referral processes. Spine 39(22 Suppl 1):S129–S135
Harris SA, Rampersaud YR (2016) The importance of identifying and modifying unemployment predictor variables in the evolution of a novel model of care for low back pain in the general population. Spine J 16:16–22
Paskowski I, Schneider M, Stevans J, Ventura JM, Justice BD (2011) A hospital-based standardized spine care pathway: report of a multidisciplinary, evidence-based process. J Manip Physiol Ther 34:98–106
Arnold PM, Burton DC, Khan TW, Dixon KA, Asher MA, Varghese G (2013) Establishment of a university academic spine center: from concept to reality. J Med Pract Manag 28:220–224
Klein BJ, Radecki RT, Foris MP, Feil EI, Hickey ME (2000) Bridging the gap between science and practice in managing low back pain. Spine 25:738–740
Murray MM (2011) Reflections on the development of nurse-led back pain triage clinics in the UK. Int J Orthop Trauma Nurs 15:113–120
de Goumoens P, Genevay S, Tessitore E, Zaarour M, Duff JM, Faundez A et al (2014) Inter-hospital CHUV-HUG medical consensus of back pain management. Its application in care pathways within CHUV of Lausanne. Rev Med Suisse 10:970–973
Bramberg EB, Klinga C, Jensen I, Busch H, Bergstrom G, Brommels M et al (2015) Implementation of evidence-based rehabilitation for non-specific back pain and common mental health problems: a process evaluation of a nationwide initiative. BMC Health Serv Res 15:79
van Hooff ML, Spruit M, O’Dowd JK, van Lankveld W, Fairbank JC, van Limbeek J (2014) Predictive factors for successful clinical outcome 1 year after an intensive combined physical and psychological programme for chronic low back pain. Eur Spine J 23:102–112
Low back pain: The early management of persistent non-specific low back pain. NICE clinical guideline 88, guidance.nice.org.uk/cg88 (2009)
van Tulder M, Becker A, Bekkering T, Breen A, Gil del Real MT et al (2006) Chapter 3: European guidelines for the management of acute nonspecific low back pain in primary care. Eur Spine J 15(Suppl):S169–S191
Hill JC, Dunn KM, Lewis M, Mullis R, Main CJ, Foster NE et al (2008) A primary care back pain screening tool: identifying patient subgroups for initial treatment. Arthritis Rheum 59:632–641
van Hooff ML, van Loon J, van Limbeek J, de Kleuver M (2014) The Nijmegen decision tool for chronic low back pain. Development of a clinical decision tool for secondary or tertiary spine care specialists. PLoS One 9:e104226
American Academy of Orthopaedic Surgeons and North American Spine Society (1996) Clinical guideline on low back pain—phase 1
Hall H, McIntosh G, Boyle C (2009) Effectiveness of a low back pain classification system. Spine 9:648657
Zarrabian M, Bidos A, Fanti C, Young B, Drew B, Puskas D et al (2017) Improving spine surgical access, appropriateness and efficiency in metropolitan, urban and rural settings. Can J Surg 60:342–348
Kim JS, Dong JZ, Brener S, Coyte PC, Rampersaud YR (2011) Cost-effectiveness analysis of a reduction in diagnostic imaging in degenerative spinal disorders. Healthc Policy 7:e105–e121
Rampersaud YR, Bidos A, Schultz S, Fanti C, Young B, Drew B, Puskas D, Henry D (2016) Ontario’s Inter-professional Spine Assessment and Education Clinics (ISAEC): patient, provider and system impact of an integrated model of care for the management of low back pain. Can J Surg 59(3 Suppl 2):S39
Buchbinder R, van Tulder M, Oberg B, Costa LM, Woolf A, Schoene M et al (2018) Low back pain: a call for action. Lancet 391:2384–2388
Davis MA (2012) Where the United States spends its Spine Dollars. expenditure on different ambulatory services for the management of back and neck conditions. Spine 37:1693–1701
Maetzl A, Li L (2002) The economic burden of low back pain: a review of studies published between 1996 and 2001. Best Pract Res Clin Rheumatol 16:23–30
Whitehurst DGT, Bryan S, Lewis M, Hill J, Hay EM (2012) Exploring the cost-utility of stratified primary care management for low back pain compared with current best practice within risk-defined subgroups. Ann Rheum Dis 71:1796–1802
Lin CWC, Haas M, Maher CG, Machado LAC, van Tulder MW (2011) Cost-effectiveness of general practice care for low back pain: a systematic review. Eur Spine J 20:1012–1023
Jonckheer P, Desomer A, Depreitere B, Berquin A, Bruneau M et al (2017) Low back pain and radicular pain: development of a clinical pathway. Belgian Healthcare Knowledge Center Report 295A
Depreitere B, Jonckheer P, Desomer A, Van Wambeke P (2020) The pivotal role for the multidisciplinary approach at all phases and at all levels in the national pathway for the management of low back pain and radicular pain in Belgium. Eur J Phys Rehabil Med 56:228–236
Magel J, Hansen P, Meier W, Cohee K, Thackery A, Hiush M, Firtz JM (2018) Implementation of an alternative pathway for patients seeking care for low back pain: a prospective observational cohort study. Phys Ther 98:1000–1009
Cancelliere C, Donovan J, Stochkendahl MJ, Biscardi M, Ammendolia C, Myburgh C et al (2016) Factors affecting return to work after injury or illness: best evidence synthesis of systematic reviews. Chiropr Man Therap 24:32
Acknowledgments
We wish to thank dr. John Lee (London, UK), Dr. Charles Greenough (North East England, UK), Mrs. Susan Murphy (Waterford, Ireland), Mr. Andrew Bidos (Ontario, Canada), Mrs. Terry Blackmore (Sasketchewan, Canada), Dr. Ian Paskowski and James Berghelli (Plymouth, USA) and Dr. Susanne Schwarzkopf (Nuremberg, Germany) for their enthusiast help in providing insight into their low back pain pathways.
Funding
This Project was funded by the Belgian Healthcare Knowledge Center (KCE).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Coeckelberghs, E., Verbeke, H., Desomer, A. et al. International comparative study of low back pain care pathways and analysis of key interventions. Eur Spine J 30, 1043–1052 (2021). https://doi.org/10.1007/s00586-020-06675-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06675-2